Coronavirus (COVID-19) Phase 2: supporting evidence for moving to Phase 2 of Scotland's route map
This publication provides an assessment of the evidence to help inform the decision to move to Phase 2 of Scotland's route map.
WHO criterion 3: Outbreak risks are minimized in high vulnerability settings
WHO criterion 3: Outbreak risks are minimized in high vulnerability settings, such as long-term care facilities (i.e. nursing homes, rehabilitative and mental health centres) and congregate settings.
Long term care facilities can be high risk for severe Covid outbreaks due to their congregate nature and often vulnerable populations. Minimizing risks within these settings has been a core component of our response.
Hospital Acquired Infections (HAI)
Scotland is the only UK country that has identified HAI clusters where they are not expected, that is within non-COVID areas. Where we suspect that Covid-19 was contracted after admission to hospital (rather than in the community), those cases are also reported in our figures. UK COVID-19 Infection, Prevention and Control (IPC) guidance has been widely implemented within NHS Boards and supplemented with various webinars, aide memoires and posters to support IPC practice for frontline stakeholders.
This cluster data is reported to SG on a daily basis. The reporting system on Antimicrobial Resistance and Healthcare Acquired Infection (ARHAI) asks that Boards report point prevalence data around active clusters on a daily basis – this include patient numbers (suspected/confirmed), staff numbers, control measures and investigations and number of death. This data is self-reported and therefore unvalidated. A validation exercise using the agreed UK/ECDC definitions is currently underway between HPS and NHS Boards to ascertain how many of these cases are HAI and how many are community associated.
Children's Services
We have established a children's residential care group which brings together children's homes, secure care and residential schools. This group is considering what environmental, care and staffing changes need to be put in place and how they respond to Test and Protect policy. The group is supported by SG officials and relevant staff from the Chief Social Work Adviser (CSWA), Chief Nursing Officer (CNO) and Health Protection Scotland (HPS) and will report to the Care Homes Oversight Board.
Prisons
New powers have been put in place through the Coronavirus (Scotland) Act 2020 for the early release of a specific class of prisoners held in Scottish prisons. A controlled early release scheme was then undertaken in order to provide the Scottish Prison Service with additional operational capacity. This allowed for a greater use of single cell occupancy, keeping prison staff and the people in their care safe. A total of 348 people have been released from prison in the course of this scheme.
Operational measures taken by prison and health staff in Scotland have been effective in reducing the spread of COVID-19 across the prison estate. As at week ending 9 June, there were no confirmed positive cases of COVID-19 in Scottish prisons and just 10 individuals self-isolating across 5 establishments.
Care homes
Since the beginning of March, we have taken regular and firm action to support care homes across Scotland and protect the wellbeing of those who work and live there.
Clinical and practical guidance for care homes was first published on 13 March and has been kept updated, most recently on 15 May, to reflect developing circumstances. We have established a Care Homes Clinical and Professional Advisory Group led by the Chief Medical Officer (CMO) and CNO to provide up-to-date advice on the response to COVID-19 in the care home sector.
We have tasked Directors of Public Health with providing enhanced clinical leadership to care homes. To supplement this, we have asked all Health Boards and local authorities to establish multidisciplinary clinical and professional oversight teams – including Medical Directors, Nurse Directors and Chief Social Work Officers – to provide scrutiny of care home provision in their areas.
A Care Homes Rapid Action Group has been established, with representatives from across the sector to receive regular updates and activate local action where it is required. As well as providing advice and oversight, we have ensured care homes have the means, resources, and capacity to implement the guidance.
Personal Protective Equipment (PPE)
From the outset, we have helped care homes access PPE in spite of the immense pressure that global supply chains are under. Since 19 March, a dedicated helpline has delivered emergency PPE directly to social care providers. We have also established local PPE hubs, allowing care homes to collect 'preventative' equipment or have it delivered onwards to them. Hubs' stocks have grown over time to meet increased demand. To date, more than 53 million items of PPE for social care, including care homes, have been distributed from the national stock to over 1,000 locations across Scotland.
Funding
We have confirmed an initial £50 million allocated to health boards to route to integration authorities to strengthen resilience. We have also assured local authorities that additional costs arising from COVID-19 will be met by the Scottish Government, aligned to local plans already in place.
Workforce
Steps have been taken to bolster and support the social care workforce, through a mix of new recruits, returnees or redeployment. The Scottish Social Services Council recruitment portal went live on 29 March. And, as of 2 June, 253 individuals have been matched into roles. This complements extensive work on the ground to deploy local health and social care staff to support care homes at this time.
Testing
Reflecting increasing capacity, we have progressively expanded the availability of testing for both residents and staff, establishing a sick pay fund for those care workers who test positive and go off work. Since 21 April Covid-19 patients discharged from hospital to a care home should be given 2 negative tests before discharge; and other new admissions to care homes should be tested and isolated for 14 days.
Since 1 May enhanced outbreak investigations have been taking place in all care homes where there are confirmed cases of COVID-19 with all residents and staff offered testing, whether they are symptomatic or not. Where staff may still be working between homes run by the same operator, testing will also take place in any linked homes following an outbreak in one. There is also sample testing in care homes where there are no cases.
From 25 May we have begun to offer care home staff testing, regardless of whether they have symptoms or if there is an ongoing outbreak in their care home. This is being done on a weekly basis. The Cabinet Secretary for Health and Sport wrote to NHS Boards to direct them to implement this with immediate effect and all boards now have plans in place to implement this action.
We are working with Health Boards and Local Authorities to support them in delivering this increased testing regime, including through the establishment of a process for deploying mobile testing units and enabling care homes and Health and Social Care Partnerships to access the UK Government Social Care Testing Portal which is now available.
Emergency legislation
We have brought in new legislative powers to ensure the swiftest intervention if care home residents are being put at risk. The Coronavirus (Scotland) (No. 2) Act 2020 contains powers allowing direct ministerial interventions in the ownership, management and operation of care homes and care home services. These powers can be used where there is an anticipated risk to residents' health, and allow the highest risk cases to be addressed urgently. These additional measures reflect our commitment to working with all stakeholders to take action, adapt and improve the system as new information comes to light.
Data
Data from both Public Health Scotland and Health Boards on testing in care homes shows that over the week commencing 8th June:
- 477 care home staff tests were carried out through NHS labs, bringing the total to 22,544.
- At least 7,920 individual care home staff were tested. This includes staff tested via the NHS Care Portal who are not captured in number of NHS lab tests above.[1]
- 2,342 care home resident tests were carried out, bringing the total through NHS labs to 17,394. This includes tests on care home residents in hospital.[2]
- At least 1,776 individual residents in care homes were tested, based on data reported by NHS Boards[1].
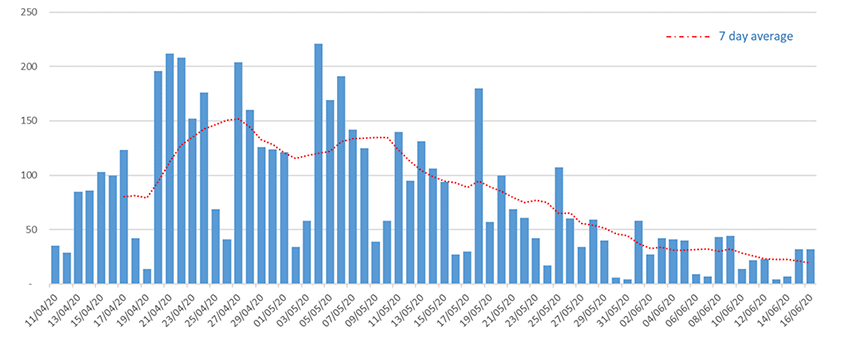
Source: Care Inspectorate
NRS figures for care home deaths
National Records of Scotland are the official source of Covid-19 deaths. The most recent publication on 17 June shows a steady decrease in the weekly number of deaths in care homes, falling from a peak of 340 at the end of April to 35 deaths from 8 – 14 June.
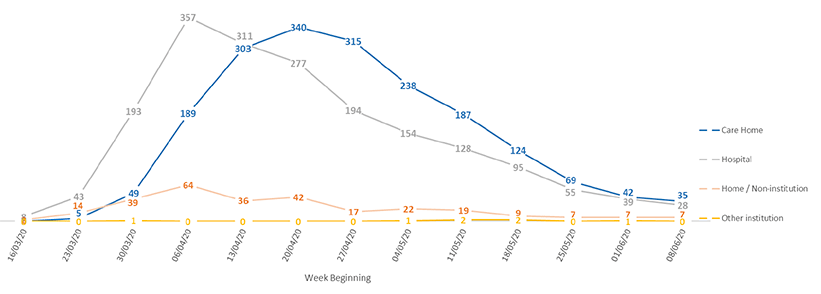
Source: National Records of Scotland
As at 17 June 351 (33%) adult care homes had a current case of suspected COVID-19. This number relates to care homes who have notified the Care Inspectorate of at least one suspected case of COVID-19, and have not subsequently notified they no longer have any cases.
Cases of infection in hospitals, prisons and care homes have consistently declined since late April.
Robust monitoring and reporting mechanisms, together with enhanced funding, provision of PPE and bolstering of the workforce in care settings will ensure that any new cases are quickly identified and isolated and the risk of future outbreaks is minimised.
Application of robust testing measures will ensure that infections are not being moved around the care system, and that staff are routinely tested to ensure their health and wellbeing.
We will take further action to address nosocomial infection in healthcare settings that is comprehensive and system wide and that delivers sustainably and at pace; and ensure for care homes full compliance with the testing policy in place. We will strengthen information on other residential settings including adult mental health, learning disability and forensic services. We are putting in place comprehensive and location-specific measures across the mental health inpatient estate to minimise the risk of infection. Patient safety is an absolute priority in mental health inpatient settings
Contact
Email: covidexitstrategy@gov.scot