Realising Realistic Medicine: Chief Medical Officer for Scotland annual report 2015-2016 appendix
Case studies of applying the personalised, patient-centred Realistic Medicine approach across Scotland.
NHS Lanarkshire
Initial thoughts
Realistic Medicine has been used to stimulate discussion at forums across NHS Lanarkshire. Work streams inspired by this have resulted in work starting in acute, community and primary care services. These work streams are important in achieving some tangible outcomes aligned with Realistic Medicine, but it is equally important to bring about culture change so that supporting actions become embedded in normal practice.
What have we done so far?
A 'Virtual Intelligence Group' has been established to support the commissioning of the evidence related to Realistic. The group has been tasked with scoping current key areas of work dovetailing this with other work that is being developed across Lanarkshire such as the trialling of an Ethical Peer Group, roll out of Hospital Anticipatory Care Planning and development of a Prescribing Quality & Efficiency Programme. A template has been developed for 'Realistic Medicine' projects to capture the vision and outcomes.
Key assessment criteria are:
1. Realistic Medicine Domains
2. Croydon Guiding List
3. NHS Lanarkshire Guiding Parameters
Support from Public Health, NSS and project management has been essential.
While proposed projects to improve pathways are accepted via the template, a proposal to reduce or stop an intervention must by investigated by the Board. Some work undertaken has confirmed that current pathways are working well, which is helpful to be aware of. In other areas pathways have been improved, such as improving shared decision making at the pre-assessment stage in a nurse-led group setting for people considering tonsillar surgery.
The recently published Healthcare Strategy 'Achieving Excellence' references 'Realistic Medicine' a number of times. Within the primary care section the need for a new clinical paradigm that adopts the least invasive or disruptive processes as a first step is highlighted.
HACP
is also essential.
HACP
has been introduced for patients with long term conditions who are
on an
end-of-life trajectory. It is designed to make interventions
appropriate given the patient's wishes, to ensure that futile and
harmful treatments are avoided, and to prompt early use of
palliative treatments. The approach is structured and
person-centred and the overall aim is to avoid bad deaths and
facilitate good ones.
This work has now progressed to implementation across the clinical areas of the Acute Division.
What next?
The next steps for the VIG include further development of the commissioning template, collecting additional evidence and developing a benefits matrix and performance metrics. Reports will be fed back from each hospital site.
In the area of HACP, the team is now visiting sites across NHS Lanarkshire speaking with clinicians to discuss barriers and challenges to HACP. An educational video has been developed and a Learn-Pro module will be up and running in early 2017 focusing on this area. Reference material will also be available on the intranet with agreed documentation being held alongside other complementary advance directives.
Final thoughts
NHS Lanarkshire are committed to the direction of travel set out in Realistic Medicine and have used its publication as a catalyst for change in how we deliver healthcare to our population.
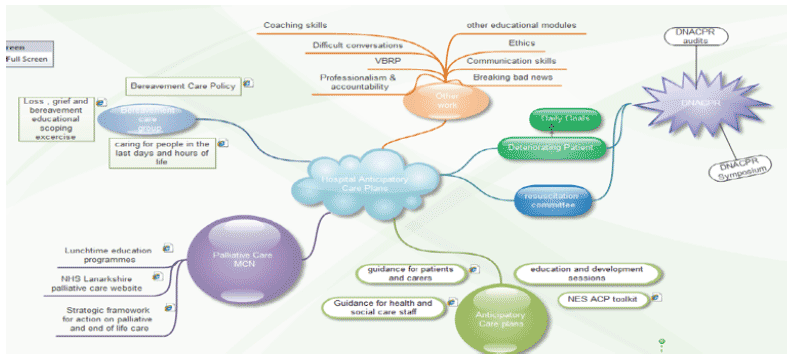
NHS Lanarkshire Hospital Anticipatory Care Plan flow chart (Board Paper, March 2016).
Contact
Email: Catherine Calderwood