Better Cancer Care, An Action Plan
Better Cancer Care, An Action Plan outlines the way forward for cancer services, which are required to support all those in Scotland who find themselves living with and beyond cancer.
SECTION THREE: EARLY DETECTION OF CANCER
The earlier a cancer is diagnosed, the better the chance there is of a complete cure. The Scottish Government is committed to an evidence-based approach to screening, based upon the advice of the UK National Screening Committee and supports national screening programmes for cervical, breast and bowel cancers. The Scottish National Advisory Group on Breast and Cervical screening ( NAG) assesses emerging evidence from research and provides advice on possible changes to these programmes. Advice on bowel screening is provided by the Scottish Bowel Screening Programme Board.
Scottish Cervical Screening Programme
The Scottish Cervical Screening Programme was introduced in 1988 with the aim of reducing the incidence of invasive cancer of the cervix. Cervical screening is offered to eligible women aged 20-60 every three years and women with an abnormal result are invited for follow up as appropriate. The incidence of cervical cancer decreased by 47.7% between 1986 and 2005. Just over 400,000 tests were completed during 2006/07, with 3.5% of tests showing an abnormal result.
The introduction of Liquid Based Cytology as the method for preparing samples for laboratory examination has helped to reduce the percentage of test results that are deemed unsatisfactory from 8.8% in 2003/04 to 2.4% in 2007. This has reduced the unnecessary anxiety associated with an unsatisfactory result and the need for women to have their test repeated. The Scottish Cervical Call/Recall System ( SCCRS) was introduced in May 2007 to improve 'call/recall' arrangements. The purpose of this electronic system is to allow standardised call and recall, online updating of information and speedy reporting of results in line with the national NHS Quality Improvement Scotland ( NHSQIS) Standards for Cervical Screening, which require 80% of women to receive results within four weeks of their test. The data generated by this system will enable the quality of the national programme to be assessed against NHSQIS standards and will allow NHS Boards to consider further action that might be necessary to meet these standards at a local level.
Over the past five years there has been a gradual fall in uptake for cervical screening especially in the 20-24 age group (Figure 8). As such, there is an urgent need to ensure that young women, whether they have been immunised or not, still attend for cervical screening. The publicity generated by the HPV Immunisation Programme will reinforce the importance of the screening programme.
Figure 8: Comparative uptake for cervical screening by age group - for 2001/02 and 2006/07
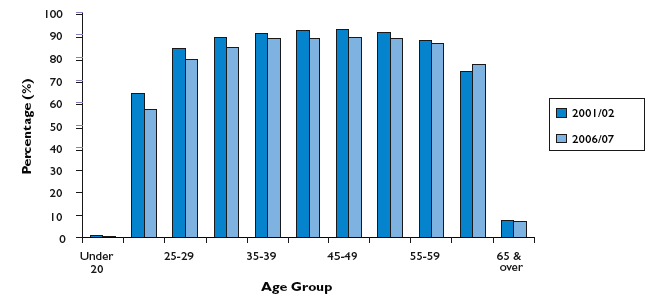
This graph shows the percentage of women who have attended for cervical screening within the last 5.5 years by age group.
Excludes Lothian data, based on adjusted Community Health Index (excluding medically ineligible women).
Data Source: ISD
Example of Good Practice in Scotland
Community Health Educators: Addressing Cervical Screening Uptake Among Vulnerable Groups In Lanarkshire, Scotland
Women in the most deprived areas and from certain ethnic minority communities tend to be less likely to take part in cervical screening. NHS Lanarkshire is addressing cervical screening uptake among its vulnerable groups, by exploring factors affecting participation, using a combination of qualitative and quantitative techniques. The research exercise found that community health educators (trained 'lay' members of the community, who deliver education) have been successful in promoting awareness, knowledge and uptake in cervical screening in ethnic minority communities, making a potentially sensitive topic more accessible to these communities. There were clearly defined areas found which could be packaged into a resource to support professionals.
'Test of Cure'
'Test of cure' is a different follow-up pathway for managing patients who have been treated for high-grade cervical disease ( CIN2+). There is evidence to suggest that the use of HPV testing, in conjunction with cytology, will identify at an early stage those who are likely to show residual or recurrent disease after treatment. This will reduce the number of cervical smears required in those women who are HPV negative and have cytology results within normal limits. A sub group of the NAG considered the implications of this evidence for the Scottish Cervical Screening Programme, concluding that the intervention should be further explored in terms of service and organisational impact, cost and the options for service delivery appraised. The Scottish Government has agreed to fund a project to take this work forward.
Use of Computer Technology to Assess Cervical Cytology Slides
Automated imager systems, a new technology currently being used in the USA, detects abnormal cells and directs the cytology screener to the appropriate fields of view on a slide, rather than the screener looking at all the fields of view. This technology may change the way that laboratory testing in Scotland is delivered for the cervical screening programme in the future. Its implications are being considered by a review group, established to provide advice on the future requirements of the Scottish Cervical Cytology Laboratory Service. As part of this process, a feasibility study has been commissioned on the use of an automated imager system for the Scottish Cervical Screening Programme.
Scottish Bowel Screening Programme
In 2005, colorectal cancer accounted for 14.5% of all cancer in men and 11.3% in women. There have been significant improvements in survival for cancers of the colon and the rectum. Around 55% of patients diagnosed between 2000 and 2004 are now surviving at least five years after diagnosis, compared to around 35% of those diagnosed between 1980 and 1984.
The Scottish arm of a UK colorectal cancer screening pilot commenced in April 2000 in NHS Tayside, NHS Fife and NHS Grampian and was completed in May 2007. Following a successful evaluation of the pilot, it was agreed to roll out a population-based bowel screening programme from June 2007 with the pilot NHS Boards implementing the screening programme first and other Scottish NHS Boards phasing it in over the next two years, up to December 2009. All men and women aged between 50 and 74 years are being invited to participate in the programme through completion of a faecal occult blood test ( FOBt) at home every two years. Data from the three rounds of the pilot (2000-2007) are set out in Table 4. When implementation is complete, more than 700,000 people in Scotland will be issued with home test kits every year and it is estimated that the programme may prevent 150 premature deaths per year.
Table 4. Bowel screening pilot (men and women aged 50-69) summary data
Round 1 Apr 2000 - Dec 2002 |
Round 2 Dec 2002 - Apr 2005 |
Round 3 May 2005 - Jun 2007 |
|
|---|---|---|---|
Number completing screening process |
167,415 |
164,077 |
175,853 |
Number of positive results |
3,464 |
3,123 |
2,044 |
% of positive results |
2.1% |
1.9% |
1.2% |
Number having colonoscopy |
2,961 |
2,795 |
1,661 |
Numbers of cancers found |
354 |
197 |
124 |
Cancers detected in those who tested FOBt positive |
12% |
7% |
7% |
Data Source: ISD
NHSQIS has published a range of standards relating to the Scottish Bowel Screening Programme. These include a national target for the Scottish Bowel Screening Programme that 60% of those invited to participate respond and complete a test.
"More needs to be done to make men go for this screening as they often wait until it is too late." Better Cancer Care Consultation Respondent |
During the pilot phase, uptake stood at only 54.4% (Figure 9) so more needs to be done to encourage uptake. Uptake in men is particularly challenging being around 8-10% lower than that amongst women. Furthermore, a particular focus will be required in Scotland's less affluent communities, given that uptake in the least deprived quintile was 50% higher than in the most deprived quintile (Figure 10).
Figure 9: Percentage uptake of screening by gender and round
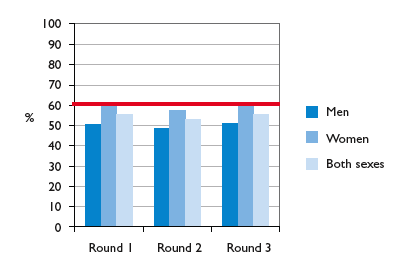
Data Source: ISD
Figure 10: Percentage uptake of screening by Scottish Index of Multiple Deprivation Quintile
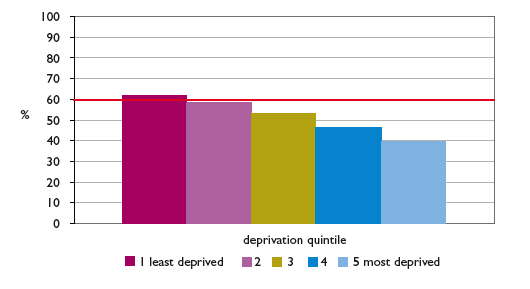
Data Source: ISD
Scottish Breast Screening Programme
Breast screening in Scotland had its twentieth anniversary in 2008. Women aged 50-70 are invited for breast screening every three years by GP practice. Screening can also be requested by women over 70. In 2006/07 over 166,000 women of all ages were screened in the programme. Over 8,400 women were recalled for further investigations, leading to the diagnosis of 1,395 cases of cancer. Figures show that 76.5% of women aged 50-64 resident in Scotland have been screened at least once in the previous three years.
Currently, two x-ray views are taken at the first screening appointment and one view at all later screening appointments. This will change to two x-ray views being taken of each breast, but from different angles, at all appointments. Forecasts show that this will lead to an additional 275 cancers being detected through the screening programme. This change to appointments should be fully implemented across Scotland by April 2010 and £13.4 million has been set aside to achieve this. Work on pathways and role redesign, in order to support the implementation of two views, will be taken forward by the Scottish Government's Improvement and Support Team in partnership with Scottish Breast Screening Programme.
NHSQIS published a status report in December 2006 on the Scottish Breast Screening Programme and reported that "the programme achieves high clinical standards, not as a one-off, but consistently, year after year". The report made five recommendations:
- Monitor and report performance of radiologists and other film readers
- Reduce the number of women recalled for assessment after their first screening appointment
- Meet the targets for issuing results
- Each Scottish Breast Screening service needs to assess and manage the risks associated with breast screening, so that they can assure the clinical governance committee of their host NHS Board that risks are minimised
- NHSScotland has to use the experience gained from breast screening to improve breast cancer services generally.
The Scottish Breast Screening Programme has been tasked with addressing these issues and to continue working with the Scottish Government and NHS Boards to ensure the appropriate level of staffing and training needs of the workforce are met. In addition, there may be a need to redesign services to better meet the needs of women attending the screening units.
The Scottish Breast Screening Programme is currently undertaking early planning for the introduction of digital mammography where digital images, rather than film images, will be used. Digital images have advantages over film records as they can be viewed, used and stored on a computer. Although this technology is unlikely to be introduced systematically before 2011, it offers the screening service far greater flexibility because images can be read at a different location. A recent study compared the double reading of mammograms ( i.e. two radiology consultants examining the mammogram films) with a single reading and a computer assisted programme; the results showed a similar performance in both groups. The NAG will be asked to look at these results and advise on the possible use of this technology in the Scottish Breast Screening Programme.
Tackling Inequalities
"Travelling communities have structured, family networks. To access the younger generations, the matriarch (grandmothers usually) need to be targeted." Better Cancer Care Fair for All - Ethnic Minorities Roadshow Participant |
NHS Boards have a responsibility for ensuring the quality and performance of care for the patients within their Board area and also for encouraging uptake of screening in their local population. Screening services need to be accessible to all. This includes disabled people (whatever their impairment) and would, for example, include people with learning disabilities, amongst whom there are much lower rates of screening for cervical and breast cancer. It is also known that attendance at screening varies by gender, age and socio-economic group. Such issues are being addressed, for example, for bowel screening. It is the NHS Boards' responsibility to develop protocols for gypsies/travellers and homeless people, in line with the terms of the Scottish Bowel Screening manual.
A study conducted in NHS Greater Glasgow & Clyde found that the uptake of cervical screening by women with learning disabilities was markedly lower (at 13.5%) than for all women in this NHS Board area (74% overall). Some women with learning disabilities are more disadvantaged than others and the reasons for poor uptake are likely to be related to the multiple barriers to access experienced by this group. Marital status, living circumstances, pregnancy history, contraceptive usage, smoking and the level of learning disability were all significantly associated with uptake rate.
Example of Good Practice in Scotland
Breast Screening
To ensure that the service is as accessible as possible, mobile breast screening units are used for approximately 80% of appointments. These units can be parked in areas such as Community Centres and GP surgeries and are (manual) wheelchair accessible. The units are also used to ensure women in long-stay institutions, such as state hospitals, can access screening.
The Scottish Government is addressing the health inequalities that can be seen between Scotland's least deprived and most deprived communities through its support of the Keep Well programme. Aimed at 45-64 year olds in the 15% most deprived communities of Scotland, the programme engages with those who typically do not make full use of the health services available to them, inviting them to attend a health check at their local GP practice or a suitable alternative venue. Whilst this programme focuses in particular on assessing the risk of cardiovascular disease, there are similarities in terms of the risk factors for cancer and the Keep Well programme offers a unique opportunity to tackle cancer inequalities.
At present, it is difficult to identify differences in access to screening services amongst different ethnic groups because ethnicity is not routinely documented in medical records. It is planned to expand incentives to improve ethnicity recording in GP records through the General Medical Services contract in Scotland. A Chief Scientist Office-funded project is underway to study ethnic variation in health, health service utilisation and health outcomes in Scotland. This project uses record linkage between Scotland's health databases and the 2001 census data, creating a retrospective cohort study of about 5 million people. These findings will provide valuable data that NHSScotland can use to address the needs of ethnic minority groups, demonstrating compliance with legislation and NHS policy.
Screening for Prostate Cancer
The prostate specific antigen ( PSA) test is one of a range of investigations which may be undertaken to confirm a diagnosis of prostate cancer. At present, the UK National Screening Committee recommends that a national screening programme for prostate cancer using the current PSA test would not be beneficial and could cause unnecessary harm because some men would be offered treatment they may not require. In addition, recent published evidence from the USA advises against PSA screening. Current PSA testing cannot differentiate between men whose prostate cancer will grow rapidly and aggressively and those in whom it will remain localised to the prostate for the rest of their lives. PSA levels may also be raised in a number of conditions unrelated to cancer.
Although there are no current plans for a national screening programme, the PSA test is readily accessible via GPs. Due to issues surrounding sensitivity and specificity, as well as those regarding treatment and possible side-effects (current treatments for prostate cancer can have serious side-effects, including impotence and incontinence), there is a requirement for GPs to fully explain all of these issues to enable men to make an informed choice before proceeding to have a PSA test. The UK National Screening Committee will continue to review all new evidence on this topic as it becomes available.
Screening for Lung Cancer
The Health Technology Assessment ( HTA) programme has requested feasibility studies in lung cancer screening. The aim is to identify the potential cost effectiveness of a screening programme in high-risk individuals, probably using spiral computed technology ( CT) imaging. Clearly there is considerable benefit to patients if lung cancer can be detected much earlier and at a point when surgery is a treatment option. If the early feasibility work is encouraging, it is expected that this will lead to a large trial run across the UK. Should such trials go ahead patients from across Scotland will be encouraged to participate.
We will:
- Provide advice through the National Advisory Group to NHS Boards on further national, regional and local actions that can be taken to increase the uptake of cervical screening services, particularly amongst younger women
- Carry out a programme of research and attitudinal surveys through NHS Health Scotland into the reasons for non-uptake of cervical cancer screening in order to inform this advice
- Fund a pilot for the 'test of cure' treatment pathway to determine how this programme may be integrated with the Scottish Cervical Screening Programme in both a clinically and cost effective way
- Take advantage of the opportunity provided by the HPV immunisation programme to reinforce messages about the continuing importance of cervical screening
- Consider and respond to the recommendations of the Cervical Cytology Laboratory Review Group on the future laboratory requirements of the cervical screening programme when it provides its advice in 2009
- Ensure that the Scottish Bowel Screening Programme is rolled out across Scotland by the end of 2009
- Consider actions that might be taken within primary care to improve uptake of the Scottish Bowel Screening Programme
- Look at means to encourage relevant individuals' participation in Scottish Bowel Screening Programme , for example, by exploring the use of Keep Well projects for inclusion of Scottish Bowel Screening Programme information
- Monitor compliance with the NHSQIS standards for the Scottish Bowel Screening Programme
- Implement two x-ray views at each breast screening round by April 2010. There may need to be redesign of roles and services to achieve this
- Support screening services to examine the processes involved in the breast screening pathway and explore opportunities for improvement
- Consider any developments in technology or screening tests that may improve the screening programmes
- Complete the Chief Scientist Office-funded study which seeks to address the information gap relating to ethnicity and medical recording
- Work with the Chief Scientist Office to examine opportunities to support Scottish researchers and patients participating in lung cancer research trials.