Better Cancer Care, An Action Plan
Better Cancer Care, An Action Plan outlines the way forward for cancer services, which are required to support all those in Scotland who find themselves living with and beyond cancer.
SECTION NINE: DELIVERY
Better Cancer Care
Better Cancer Care maps out the key priorities and actions for tackling cancer in Scotland. By necessity it is a broad plan which requires the involvement of NHSScotland and the people who work within it, other parts of the Scottish public sector, the voluntary sector and of course, patients, carers and others who are affected directly by cancer. If this plan is to achieve the outcomes and deliver the benefits it seeks, it needs to be underpinned by a strong and determined focus on delivery, supported by structures and processes that direct the attention of all stakeholders on delivering outcomes and minimising the risks to delivery across Scotland.
Scottish Cancer Taskforce
The implementation of this plan will be overseen by a new Scottish Cancer Taskforce, chaired by the Deputy Chief Medical Officer. This will replace the Scottish Cancer Group and provide a focal point for the actions in this plan, provide support and advice to NHS Boards and the RCAGs and ensure that patients, NHS staff, the Royal Colleges and the voluntary sector continue to have a strong voice in advising the Scottish Government and NHS Boards on cancer issues.
"There should be better engagement between professionals and users. Patient and carer experience should be central to planning. There should be workshops with the Scottish Government to agree quality indicators and cancer targets." Better Cancer Care Consultation Respondent |
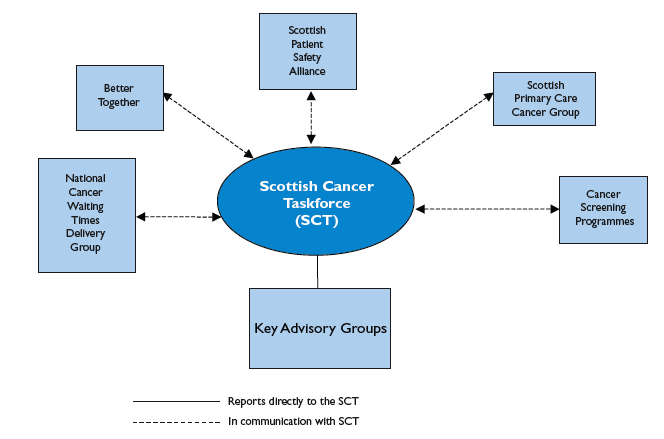
The first task of the new group will be to review the rest of the cancer 'delivery landscape' (Figure 18) and to identify ways in which the current network of advisory, planning and delivery groups can be streamlined in order to ensure that they are best able to support the effective and efficient implementation of this plan. In particular, this review will need to demonstrate how the delivery and subsequent development of the actions in this plan will continue to be informed by patients and the public more generally and be fully integrated within the planning processes and priorities of NHSScotland at board, regional and national level.
Subject to the conclusions of this initial review, it is envisaged that the key, ongoing tasks of the new Scottish Cancer Taskforce will be to:
- Agree an annual work programme with key advisory groups to ensure that actions are delivered and that the Scottish Government and NHS Boards have access to the latest advice and expertise
- The future work programme for quality improvement in cancer services will reflect the six dimensions of quality
- Work with Patient Safety Alliance, Better Together and the National Cancer Waiting Times Delivery Group to improve the patient experience, ensure the highest standards of patient safety and advise on waiting times issues
- Ensure that the plan is implemented in a way that supports NHSScotland's commitment to equality and diversity
- Provide guidance on taking forward the national audits set out in this plan
- Identify and advise the Scottish Government on the implications and opportunities arising from NHS Board and regional workforce and service delivery plans, including the identification of priority education and training needs
- Provide advice to eHealth and Telehealth teams within Scottish Government and NHS Boards to support the design and implementation of solutions which enhance services for patients and clinicians.
Figure 18: Links to Scottish Cancer Taskforce
Clinical Leadership
There was much debate during the Better Cancer Care consultation process about the need for clinical leadership to deliver this plan. The appointment of the Deputy Chief Medical Officer as Chair of the Scottish Cancer Taskforce provides the opportunity of providing such leadership at the very heart of Scottish Government. The Taskforce will also include the three regional clinical leads for cancer, together with the Chair of the Scottish Primary Care Cancer Group who, with the Deputy Chief Medical Officer, will further enhance clinical leadership by developing a national component to their respective roles and in particular:
- Advise the Scottish Government about key clinical issues and ensuring that work in such areas is coordinated appropriately at a national level
- Work with Directors of Nursing and Allied Health Professional leads to ensure that all NHS professional groups' views are appropriately represented at a national level
- Facilitate the ongoing involvement of regional and local lead clinicians in developing and delivering the broad programme of quality improvement envisaged by this plan
- Represent the views of local and regional clinicians at a national level to deliver the quality programme outlined in this plan.
Regional Cancer Networks and Managed Clinical Networks ( MCNs)
MCNs facilitate clinical collaboration across Scotland and are a key feature of the more mutual NHS described in Better Health, Better Care. They have strengthened significantly over the past seven years and enabled professionals to share effective clinical practice and develop consistent treatment protocols. NHS Boards collaborate in planning cancer services under the auspices of three regional cancer networks ( NoSCAN in the north of Scotland, SCAN in the south east and WoSCAN in the west). These networks offer the opportunity to take shared planning decisions and enable individual NHS Boards to maximise the effectiveness of their investment in cancer services. The regional cancer networks will continue to report their progress on their respective websites and through the publication of annual reports.
The National Delivery Plan for Specialist Children's Services in Scotland - a Draft for Consultation stated children's cancer services in Scotland should be planned on a national basis through the National Managed Clinical Network, and delivered according to the levels of care described in Option Appraisal for Children's Cancer Services in Scotland, 2008. This National Managed Clinical Network should operate on a permissive basis that facilitates the delivery of local 'shared care', the development of care pathways and progression of measures targeted at supporting the progressive improvement in patient outcomes. The service pattern for Scotland will be developed in accordance with the guidance set out in the National Delivery Plan for Children and Young People's Specialist Services in Scotland which will be published later in 2008.
Workforce Planning
Effective workforce planning is required in order to quantify the numbers, skills and levels of expertise of staff currently within NHSScotland and enable NHS Boards both individually and collectively to prepare for changes in the services they offer and the ongoing need to replace those staff lost through retirement or from leaving the service. Better Health, Better Care: Planning Tomorrow's Workforce Today set out a number of key actions that must be undertaken at NHS Board, regional and national levels to ensure that the workforce in NHSScotland has the capacity and capability to meet current and future demand for health services. As a key clinical priority, it is vital that such approaches recognise both the future demand for cancer services and the skills and new roles that will be required to meet such demand.
The Career Framework and its links with the Knowledge and Skills Framework for NHS Staff offer opportunities to ensure close integration with the processes of service planning at NHS Board, regional and national level. Work is underway within NES and Skills for Health to support this process by providing tools that will assist in the identification of competences needed for the delivery of cancer services, for example, ward-based and outpatient services, chemotherapy and radiotherapy services. These tools will allow planners to model multidisciplinary staff teams and plan for an improved skill mix which will deliver quality care. This will allow the development of competence-based job roles and will provide an approach to quantifying the number and type of new roles needed. It is acknowledged that this must be supported by continued investment in education and training.
To support workforce development, NES has developed a capability framework for cancer care. The framework, which will be published in late 2008, can be used by staff at different levels to identify learning needs, for self assessment and planning personal development, for team development and as a guide to developing education and training.
A coherent and strategic approach needs to be taken to workforce planning, development, education and training. NES, in conjunction with workforce planners and the service will have a critical role to play in taking this forward. Education and training are essential in meeting workforce development needs. NES will continue to work closely with the three RCAGs to identify their workforce education and development needs and support RCAGs in devising educational solutions to meet these needs in collaboration with the Scottish Cancer Taskforce.
"The role of the surgical team members need to evolve; extended roles for nurses would allow surgeons more time. There should be national planning of surgical services and conglomerations of expertise to ensure best results." Better Cancer Care Consultation Respondent |
A key priority for workforce planning will be to ensure that plans for the surgical workforce include, not only the need for surgical consultants and trainee surgeons, but also those for the wider multidisciplinary team, including nursing and allied health professionals ( AHP) staff in wards and theatres, pharmacy, healthcare scientists and facilities staff. Action is also required to promote and ensure the development of new roles such as healthcare support workers and assistant practitioners, along with effective educational programmes that will enable NHS Boards to meet the objective of delivering safe and effective chemotherapy services closer to the patient's home. The NESWorkforce Education and Training Framework for the Safe Use of Cytotoxic Medicines (2007) promotes the safe use of cytotoxic medicines and supports implementation of national guidelines, particularly HDL (2005) 29 and HDL (2004) 30 Safe Administration of Intrathecal Cytotoxic Chemotherapy. It is equally applicable to primary and secondary care settings and staff working with adults and children. It provides the foundation for a consistent approach to education and training across Scotland. The Scottish Government is committed to the utilisation of this framework for the benefits it brings to patient care.
Radiotherapy requires a mix of skills from a range of staff, including clinical oncologists, therapeutic radiographers, medical physicists, healthcare scientists, nurses, radiotherapy assistants, helpers and administrative and clerical staff. A priority for workforce planning is to redesign the radiotherapy workforce through a focus on skills and competence (rather than job titles) in order to address staff shortages and recruitment difficulties in some areas.
Implementation of the Society and College of Radiographers 4-tier career progression framework has progressed over the last few years but has not been consistent across Scotland. This is particularly disappointing, as centres that have implemented it have demonstrated the model can reduce waiting times for patients, aid recruitment and retention of staff and increase capacity. Maximising the potential of the 4-tier model should be progressed by NHS Boards, with continued support from NES and other partners.
eHealth
Clinical care requires a variety of sophisticated data capture, information storage and communication processes. Communication, in particular, is a key challenge, given the wide range of contributors to care and the number of different organisations involved. IT related support for these processes, which has come to be known as 'eHealth', has in the past, involved a mixture of manual and various eHealth support systems across NHS Board areas.
Greater consistency has now been achieved, for example, with an ever increasing proportion of GP referrals now being made electronically via the ' SCI Gateway' IT system and each NHS Board's ' SCI Store' is increasingly being used for accessing test results. The national Picture Archive Communication System ( PACS) is also being rolled out, which supports the transfer of digital x-rays between sites.
The national eHealth strategy published in June 2008 is focused on continuing this work and supporting the roll-out of systems locally when proven. Examples include the widely publicised Emergency Care Summary uploaded electronically from GP records, available to NHS 24, Out of Hours and accident and emergency services; and the associated development of a national Palliative Care Summary of essential palliative care information derived from GP systems, which contain explicit patient consent relating to such matters. In addition to major investments in hospital-focused patient management systems, the strategy also supports the greater use of video conferencing to enhance the ability of clinicians to work together, so they may effectively plan treatment for patients and improve information for patients and their carers.
"Specialists can provide support in a variety of ways, including visits, telephone advice, video-conferencing and out-patient clinics. It is also important to maximise the opportunities offered by new technologies, for example using cell-phone technology to monitor symptoms and provide self help information." Better Cancer Care Consultation Respondent |
Telehealth
Telehealth, where deployed effectively, can improve the patient's experience of care by reducing the need for travel to major cities and hospitals to receive their care and treatment. It offers a range of options remotely via phones, (including mobile phones) and broadband, often involving video-conferencing. The Scottish Centre for Telehealth is supporting NHS Boards to pilot the use of telehealth to help redesign and improve patients' access to healthcare, no matter where they live.
Example of Good Practice
In May 2006, the Scottish Government supported the project team at the Scottish Centre for Telehealth by funding a pilot to test the 'proof of concept' in the use of tele-endoscopy. This used remote diagnostic technology to facilitate the examination of an airway for patients with symptoms of head and neck cancer. The pilot delivered a remote diagnostic service from Aberdeen to Shetland, following which, the clinics are now part of routine service delivery, with high levels of patient satisfaction being reported. In May 2008, this pilot was extended to deliver a remote diagnostic service from Raigmore to Stornoway and a local Speech and Language Therapist has been trained to perform endoscopy and facilitate the clinics. The final phase will see the delivery of a Head and Neck review appointment service to a local Community Hospital in Aberdeenshire.
The economic evaluation of the above project by Health Economic Research Unit ( HERU) at the University of Aberdeen will be assessed by the Scottish Cancer Taskforce to ascertain wider roll out of the model of care. It is likely roll out of the model will be be recommended if it is shown to be safe and effective, demonstrates better use of equipment and improved clinical outcomes for patients and reduces the number of patients who have to travel to major cities for specialist investigations.
We will:
- Form a new Scottish Cancer Taskforce to replace the existing Scottish Cancer Group
- Agree an annual work programme with key advisory groups to ensure that the actions set out in this plan are addressed and that the Scottish Government and NHS Boards have access to the latest advice and expertise
- Review the current network of groups that provide advice and guidance on cancer issues to ensure that this network is fit for purpose in supporting the delivery of this plan
- Provide national clinical leadership from the Deputy Chief Medical Officer, who will chair the Taskforce together with the three cancer lead clinicians from each Regional network and the Chair of the Scottish Primary Care Cancer Group
- Bring together the RCAGs, voluntary sector, NES, Directors of Workforce Planning and other stakeholders to address current and future workforce challenges
- Maximise the potential of the 4-tier model within radiotherapy with continued support from NES and other partners
- Support NES and NHS Boards to utilise the capability framework for cancer care
- Continue to involve and work with the eHealth programme, the networks and NHS Boards in the development of IT tools
- Assess the outcomes of eHealth and telehealth projects, which may improve service delivery and clinical outcomes for cancer patients.