Better Cancer Care, An Action Plan
Better Cancer Care, An Action Plan outlines the way forward for cancer services, which are required to support all those in Scotland who find themselves living with and beyond cancer.
SECTION TWO: PREVENTION
Lifestyle factors such as smoking, poor diet, physical inactivity, the proportion and distribution of fat in the body and alcohol consumption are all important modifiable factors that contribute to an increased risk of getting cancer. Changing behaviours can affect the risks associated with more than one cancer as well as other diseases (such as heart disease and diabetes). Responses during Better Cancer Care consultation indicated that not all people believe cancer can be preventable.
"I don't really believe you can do much [to prevent cancer] and apart from good diet etc. to prevent cancer it has no respect for anyone, if cancer wants to strike any individual nothing will alter that. You have just to hope and pray you will not be the next victim." Better Cancer Care Consultation Respondent |
Recent European studies have suggested that addressing these lifestyle factors, coupled with improving life circumstances, can be effective in preventing cancer in the future. It is estimated that over half of all cancers might be avoided through such actions, which is often referred to as 'the preventable fraction'.
Tobacco
The evidence linking tobacco use to cancer is irrefutable, with smoking being strongly associated with cancers of the oral cavity, pharynx, larynx, oesophagus, pancreas, kidneys and bladder, as well as lung cancer. In 2004, among men, 40% of all cancer deaths and 91% of lung cancer deaths were attributable to smoking, while for women, the equivalent figures were 29% and 88%, respectively. Smoking also works together with other risk factors such as alcohol to multiply the risks of cancers of the oral cavity, pharynx, larynx and oesophagus. In the UK, an estimated 90% of lung cancer cases are due to smoking and there is clear evidence that stopping smoking is the single most important action that current smokers can take to reduce their risk of cancer.
Example of Good Practice in Scotland
It is recognised good practice that dentists opportunistically screen for oral cancer/precancerous conditions when examining patients, given that they are trained for and obviously well placed, to check mouths for such abnormalities. The number of adults registered with dental practices decreases after the age of 44, meaning that dentists have less access to those groups of patients who are at a higher risk of developing oral cancers (including older males who smoke and drink).
Significant progress has been made in recent years in shifting cultural attitudes to smoking, including through the introduction of a ban on smoking in public places in March 2006 and legislation to raise the age of sales for tobacco from 16 to 18 in October 2007. Whilst it is too early to assess the long-term effects of such changes, there are some extremely positive signs with, for example, one year after the legislation, an 89% reduction in exposure to second-hand smoke among bar workers (based on measurements of salivary nicotine, a marker of exposure to tobacco smoke).
The Scottish Government is determined to see a further reduction in smoking levels and is committing £42 million over the next three years (2008/09 to 2010/11) to support the wide-ranging programme of actions arising from A Breath of Fresh Air for Scotland including increased emphasis on preventing people from becoming smokers in the first place. Scotland's Future is Smoke-free: A Smoking Prevention Action Plan, published in May 2008, sets out an ambitious programme of measures designed specifically to discourage children and young people from starting to smoke and becoming regular smokers by reducing the attractiveness, affordability and availability of cigarettes and other tobacco products. Measures within this action plan include further legislative controls on the sale and display of tobacco products.
Example of Good Practice in Scotland
NHS Lothian has developed an innovative two-year pilot smoking cessation service, targeting patients with cancer, their families and their carers who are motivated to give up smoking following their diagnosis. Based on robust, international evidence, the pilot has clearly defined aims and objectives and if successful, could be replicated elsewhere in Scotland.
Diet and Obesity
Since the publication of Cancer in Scotland: Action for Change 2001, the evidence linking obesity and excess body fat to cancer has become much stronger. Avoiding excess body fat, modifying diets and increasing the consumption of fruit and vegetables are important factors to consider in any approach to cancer prevention.
Obesity is associated with a number of serious chronic diseases including certain cancers (breast, large bowel and kidney). Building on the continued delivery of the Scottish Diet Action Plan and Physical Activity Strategy, the Scottish Government has committed £56 million for initiatives dedicated to tackling obesity in Healthy Eating, Active Living: An Action Plan to Improve Diet, Increase Physical Activity and Tackle Obesity, published in June 2008. Actions are aimed at supporting people to make healthier choices in what they eat, to build more physical activity into their everyday lives and to maintain or achieve a healthy weight.
"It is important to include nutrition education as well as physical activity in the curriculum of children." Better Cancer Care Consultation Respondent |
It is essential that the focus on good nutrition begins at the earliest stages of a child's life. Scottish Government funding has been made available to ensure that maternal and infant nutrition is given a high priority, through a range of interventions. These include the encouragement to breastfeed, as there is strong evidence to suggest that breastfeeding protects the mother against both pre-menopausal and post-menopausal breast cancer and some evidence to suggest breastfeeding protects against ovarian cancer.
Hungry for Success is a programme which focuses on helping pupils make informed choices with their diet both within and outside of school. The Schools (Health Promotion and Nutrition) (Scotland) Act 2007 builds upon and reinforces Hungry for Success and health-promoting schools' policies. The Scottish Government has agreed with local government to extend free school meal entitlement to more families living in poverty. Starting in August 2009, entitlement for free school meals will be extended to all primary and secondary school pupils whose parents or carers are in receipt of both maximum child tax credit and maximum working tax credit, subject to the necessary legislation being passed. In addition, school meals will be provided to all primary 1-3 pupils from August 2010 (subject to the necessary legislation being passed by the Scottish Parliament), with the agreement of the Scottish Government and local government.
Cancer Risk and Lifestyle
- 71% of people did not know of the connection between cancer and body weight
- 64% of obese and overweight people were unaware that regular exercise could reduce cancer risk
- 48% of obese and overweight people did not believe that eating healthily could help reduce cancer risk.
Cancer Research UK (2006)
Physical Activity
"There is a need to address the perception that a healthy lifestyle is expensive." Better Cancer Care Consultation Respondent |
Evidence suggests that physical activity can protect against a number of cancers, including colon and breast cancer. The minimum recommended levels of physical activity are 30 minutes per day on most days of the week for adults and one hour per day on most days of the week for children and young people. However, the most recent estimates of the Scottish population found that only 33% of women and 44% of men currently meet the recommended daily amount of physical activity. The Scottish Government is committed to achieving the goal of 50% of adults and 80% of children meeting the minimum recommended levels of physical activity by 2022. To do this, individuals must be supported to take a greater responsibility for their health by encouraging them and providing them with more opportunities to become more active. Working in partnership with a range of local and national organisations, access to physical activity will be increased in:
- Schools - through programmes such as Active Schools and Y-Dance, and the Schools (Health Promotion and Nutrition) Act 2007
- Communities - through programmes such as Paths to Health, Jog Scotland and Girls on the Move
- Homes - through initiatives such as Play@Home
- Workplaces - through initiatives such as the Institute of Leisure and Amenity Management Healthy Living Award and the support provided to local businesses by the Fitness Industry Association.
Alcohol
There is now a substantial body of evidence which links alcohol to cancer. Indeed Cancer Research UK suggests that alcohol causes about 6% of cancer deaths in the UK. As little as three units a day can increase the risk of cancer of the oral cavity, pharynx, larynx, oesophagus, breast and large bowel. Primary liver cancer can also be a consequence of chronic liver disease, mortality rates of which in Scotland are one of the fastest growing in the world. Current advice suggests that men should consume no more than 3-4 units a day and no more than 21 units a week and for women to consume no more than 2-3 units a day and no more than 14 units a week. This advice suggests that people should also have at least two alcohol-free days a week.
The Scottish Government's consultation on new proposals to tackle alcohol misuse closed in September 2008 and will be used to inform a long-term strategic approach to tackling alcohol misuse in Scotland.
Example of Good Practice in Scotland
NHS Greater Glasgow & Clyde has developed a formal partnership with Glasgow City Council to manage and develop integrated alcohol and drug treatment services. The Addiction Services Partnership provides rapid access holistic care from health and social care professionals to individuals who have alcohol problems and who are at high risk of developing severe health problems including many alcohol associated cancers.
The Partnership has a range of services, including direct access to Community Addiction Teams, Community Alcohol Support Services, and it leads the implementation of screening and brief intervention programmes aimed at early detection of hazardous and problematic alcohol use. Nurse-led, supported detoxification programmes are available, aimed at helping patients reduce and/or cease their alcohol intake. A wide-ranging action plan is in place to assist acute services to better identify and manage individuals who have been admitted with alcohol problems.
Socio-economic Inequalities
Risk factors are known to vary by socio-economic status with, for example, higher rates of smoking amongst people living in deprived areas (Figure 7).
Figure 7: Prevalence of smoking by area deprivation, Scotland 2005-06
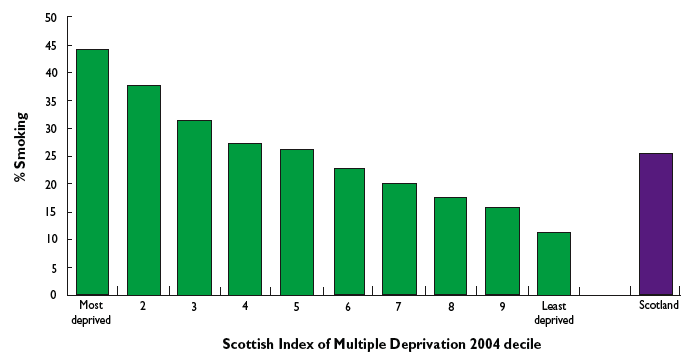
Data Source: Scottish Government
Equally Well made a series of recommendations to address health inequalities and indentified new Scottish Government funding of £15 million to reduce inequalities in the incidence of cancer and risk factors, such as smoking, as a priority. It encourages NHS Boards to play a leadership role in promoting good relations within communities, recognising the impact of discrimination and disadvantages on health, and the importance that social care pathways play for cancer patients. Community Health Partnerships should consider the potential for community pharmacies to reduce inequalities in health, by targeting services towards people living in the most deprived areas.
"Deprivation is an area where community pharmacies could have a key role." Better Cancer Care Consultation Respondent |
NHS Boards are creating hospital environments which create good health for patients, staff and visitors. The Health Promoting Health Service concept is that " every healthcare contact is a health improvement opportunity". In March 2008, guidance was issued on health promotion action to be taken in acute care settings ( CEL (2008) 14 Health Promoting Health Service; Action in Acute Care Settings). NHS Boards have been asked to implement specific health-promoting actions on smoking, alcohol, breastfeeding, diet and health and health at work, to support health improvement in acute care settings. Each action offers significant potential to improve health (including reducing the incidence of cancer) and to reduce health inequalities. Convenient locations, such as community pharmacies (for smoking cessation), will be used to encourage uptake.
Human Papilloma Virus ( HPV)
Infection with the Human Papilloma Virus is a risk factor for cervical cancer and is mainly transmitted through intimate skin to skin contact during sexual activity. Two HPV vaccines have been developed which will help to protect teenage girls from developing cervical cancer later in life by protecting against the two HPV types that cause 70% of cervical cancers.
The Scottish Government has set aside £64 million over the next three years to implement an immunisation programme across the country. The routine immunisation programme for girls aged 12-13 began in September 2008. In total, around 210,000 girls will be offered HPV immunisation between 2008 and 2010. The 'catch-up' programme for girls aged between 13 and 17 years began in September 2008, and will be offered to girls over a period of three years.
This represents a significant step forward in improving Scotland's health and reducing cervical cancer. HPV immunisation will be delivered largely through schools. Girls who have left school will be contacted by their local NHS Board and offered immunisation. Even with this immunisation programme it remains vital that all women from the age of 20 continue to attend their cervical screening appointments, including those who have received the immunisation, as the vaccine protects against only 70% of virus strains that cause cervical cancer cases. Further information on HPV and the immunisation programme in Scotland is available on www.fightcervicalcancer.org.uk/

Excessive Exposure to Ultraviolet Radiation
The incidence of skin cancers in Scotland has increased significantly and malignant melanoma of the skin is now the ninth most common cancer in men and the seventh most common in women.
The primary recognised risk factor for melanoma of the skin is exposure to sun, especially but not exclusively, in childhood and adolescence. In addition, sunbed use provides a form of intense exposure to ultraviolet light. Just one session a month will double the average individual's annual dose of ultraviolet radiation, which is linked to increasing risk of cancer. Medical evidence on the use of sunbeds is increasing, with links to premature skin ageing, skin cancer, eye damage, photodermatosis and photosensitivity.
The Scottish Government is committed to improving public awareness about exposure to the sun and in recent years has supported the UK SunSmart campaign which highlights the importance of early detection, avoiding burning from sun exposure and the potential dangers of sunbeds. The Public Health etc (Scotland) Act 2008 includes measures for controls on the use of sunbeds (which will come into force in 2009), as follows:
- A ban on operators from allowing the use of sunbeds by under 18s in commercial premises
- A ban on the sale or hire of sunbeds to under 18s
- A ban on the use of unsupervised or coin-operated sunbeds
- A requirement that sunbed operators give customers information on the health risks associated with sunbed use.
Occupational Exposure
Some cancers are linked to occupation; for example, exposure to asbestos in the workplace (such as the workplace for pipe fitters) is linked to the development, sometimes many years later, of mesothelioma (cancer of the lining of the lung).
Interim research from Imperial College London suggests that occupational exposures are responsible for around 4.9% of current deaths from mesothelioma, lung, bladder, nose and nasal cavity cancers, non-melanoma skin cancers and leukaemia combined. However, the researchers consider this to underestimate the true figure and further studies are being undertaken.
Occupational health and safety is a reserved matter, with responsibility for enforcement of occupational hygiene standards and control of occupational hazards residing with the Health and Safety Executive; these standards are enforced UK-wide. The Scottish Government will work with statutory agencies to further reduce occupational exposure of its population. Work is also taking place to estimate the burden of other cancers linked to occupation and potential occupational cancers due to more recent exposures. The work is scheduled for completion in November 2009 and the Scottish Government will take its advice into consideration after publication.
"The environments where people live and work should promote, not undermine, good health." Better Cancer Care Consultation Respondent |
Wider Environmental Issues
When considering the wider environment, the hazardous toxins of principal concern as known or probable carcinogens are radon gas from the ground, secondary tobacco smoke and diesel exhaust emissions. These toxins are all associated with an increased risk of lung cancer. The Air Quality Standards (Scotland) Regulations 2007 set quality standards for air pollutants of principal public health concern, including those primarily linked to traffic, and established the mechanisms whereby air quality can be monitored and maintained against these standards. The UK Health Protection Agency is currently completing a detailed mapping exercise to establish the levels of radon in Scottish homes and once published, the Scottish Government will consider these findings and, where appropriate, act on them.
A potential for exposure to cancer-causing agents in food is well recognised. The Food Standards Agency is tasked with ensuring that the chemicals present in food do not compromise health and safety.
The Strategic Framework for Environment and Health initiative reflects a conviction within the Scottish Government that a smarter and more strategic approach is required, so that often quite subtle environmental influences on health can be addressed. Better understanding of the relationship between environment and health can promote a further reduction in health inequalities in Scotland. The Scottish Government is committed to funding research aimed at evaluating and improving the environment, including a research project which will develop tools and techniques to marshal and interpret evidence supportive of the new approach to policy on environment and health in Scotland.
Research into Cancer Prevention
The National Cancer Research Institute Strategic Analysis Report ( 2002) highlighted that only 2% of the total cancer research funding by National Cancer Research Institute partners was spent on cancer prevention research. This led to the establishment of the National Prevention Research Initiative aimed at improving health and preventing not only cancer but conditions such as cardiovascular disease, diabetes, obesity, stroke and dementia. This is supported by a wide range of government and voluntary sector funders. A total of £10.5 million has been spent so far, with ten of the 40 awards made being led by Scottish researchers. A further £12 million has been made available to support large research projects on behaviours associated with significant risks to health, such as poor diet, physical inactivity, smoking and alcohol consumption and on the environmental factors that influence those behaviours. This expenditure compares favourably to other parts of the UK.
We will:
- Continue to implement a wide-ranging and ambitious programme of action to reduce smoking levels in Scotland
- Expand entitlement to free school meals as part of a comprehensive approach to improve diet and tackle obesity
- Work with local and national partners to continue to expand access to physical activity
- Consider the findings of the national consultation on alcohol and publish an action plan for Scotland on tackling alcohol misuse
- Support NHS Boards to implement the recommendations of Equally Well, the report from the Ministerial Taskforce on Tackling Health Inequalities
- Consider the potential ways in which community pharmacies can reduce inequalities in health, for example, by targeting services to address the health disadvantages of those groups of people living in the most deprived areas
- Continue to roll out the HPV Immunisation Programme
- Improve public awareness about the risks of exposure to the sun through awareness-raising campaigns and the implementation of controls on the use of sunbeds
- Consider Health and Safety Executive advice expected in November 2009 on occupational links to cancer
- Support a comprehensive programme of cancer prevention research.