Patient pathways - basic building blocks methodology: guidance
Guidance on the use of the Basic Building Blocks methodology which is a systematic approach to the demand and capacity analysis of existing patient pathways.
5. Whole System 'Ought to Be' Numbers
With a complex system it can be difficult to ascertain what the 'ought to be' numbers should be for the different component parts to optimise flow. One simple technique that can be used is to split the hospital system into 3 component parts, the front door ( ED), inpatient receiving / assessment areas and downstream wards.
This analysis describes the whole hospital by using two x nine number grids.
The metrics of 'how many', 'how long' and 'how full' are calculated for each area of the hospital, for 2 specific cohorts, the top 25% of days in terms of performance against the 4 hour Emergency Access Standard and for the lowest performing 25% of days against the 4 hour Emergency Access Standard. The results for Anytown General Hospital are shown in the grids below (Fig 29).
Anytown General Hospital
91 Lower Quartile days and 91 upper Quartile
days
Fig 29.
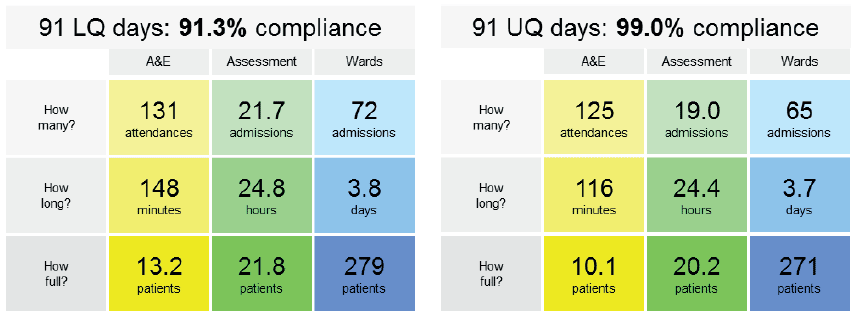
These two grids (Fig 29) provide key flow metrics associated with each area of the hospital at 99% compliance for the 'ought to be numbers' and alternatively when EAS compliance is lower at 91.3%.
When there is good compliance with EAS the number of ED attendances at Anytown General Hospital are slightly lower and the average length of stay is 32 minutes lower resulting in a lower occupancy. The GP assessment and admissions ward and the downstream wards follow a similar pattern with slightly lower admission numbers, similar length of stays, and a slightly reduced occupancy. Small differences in each component part of the system combine to have a significant impact on the Emergency Access Standard performance.
These grids confirm the importance of optimising flow at each stage of the hospital system by demonstrating even a slight increase in occupancy or length of stay downstream can impact on the whole system.
Contact
Email: Unscheduled Care Team