Patient pathways - basic building blocks methodology: guidance
Guidance on the use of the Basic Building Blocks methodology which is a systematic approach to the demand and capacity analysis of existing patient pathways.
3. Emergency Department Profiling
The Emergency Department is often a common staging post, appearing as the 1 st point of contact for many emergency pathway patients.
As an identified staging post within your basic footprint and pathways you then need to understand the profile of the unscheduled flow though this unit.
There are 4 key areas of analysis for an Emergency Department ( ED).
a) Current performance
b) Demand
c) Length of stay
d) Occupancy profiling
a) Understanding Current Performance
Emergency Access Standard
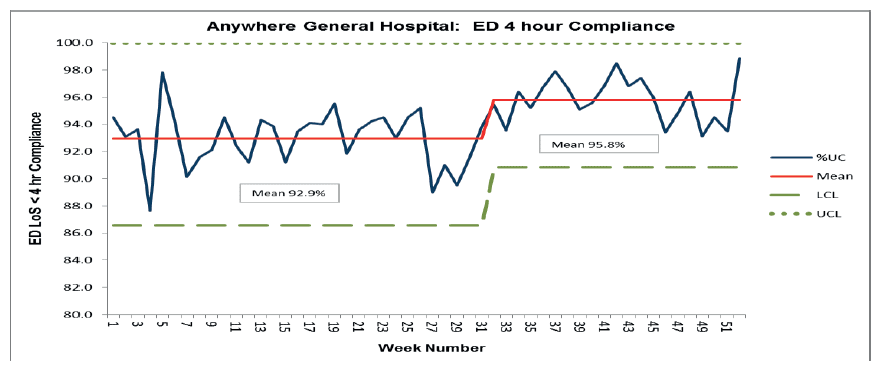
Weekly monitoring of performance against the Emergency Access Standard for ED should be undertaken routinely. Using statistical process control allows identification of standard variation as opposed to special cause variation. Upper and lower control limits should be re-calculated once a known change to the system has taken place and sufficient data points have been recorded. Recalculation of the Upper Control Limit ( UCL) and Lower Control Limit ( LCL) is important as this will indicate the current level of variation in the system. Reduced variation will equate to improved flow.
For further information on Statistical Process Control please see: http://www.qihub.scot.nhs.uk/knowledge-centre/quality-improvement-tools/statistical-process-control.aspx
Operational and Improvement Managers can use this type of chart to track and monitor improvements and changes to the system, with increasing variation or spikes or dips in performance being examined to determine cause.
Fig 4.
Performance by Flow and Day of Week
Analysing Emergency Department data by flow group and day of week is useful to identify the flow group/s with lower performance and average daily performance against the Emergency Access Standard.
For flow group definitions please see: http://www.ndc.scot.nhs.uk/Dictionary-A-Z/Definitions/index.asp?Search=P&ID=385&Title=Patient%20Flow
Examples of useful analysis are provided in Fig 5.
Fig 5.
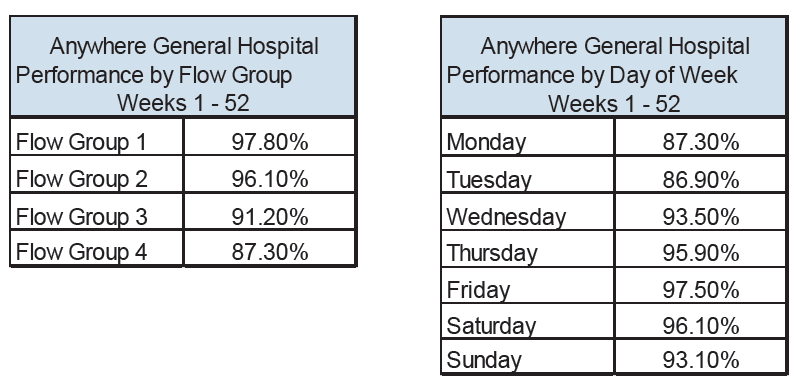
In this example admitted flow groups (3&4) are the lowest performing. Further analysis of the recorded 'reason for breach' codes by flow groups should be undertaken to ascertain the key reasons for patients staying in excess of 4 hours.
It is useful to monitor flow group performance on a weekly basis, particularly during period of improvement work or re-design. Operational and Improvement Managers can use this data to identify the specific flow groups or individual days of the week where performance is lower. Further analysis of these identified days or flow groups can then be undertaken to understand the cause, is it due to patient numbers, staffing levels, changes of practice?
Using the Performance Toolkit will give this information by time of the day and day of the week. This analysis is useful when comparing one week to another to identify where trends emerge and show indications of where further analysis is required using the above method and support information for improvement of waits delays and bottlenecks.
Performance Toolkit https://performancetoolkit.blob.core.windows.net/doc/toolkithelp.html
Other Useful Measures of Emergency Department Flow
Consider the other data items that are currently collected by your site and how these are used for performance or improvement purposes.
Key Quality indicators for the ED include journey point measures such as:
- time to 1 st assessment
- time to 1 st assessment by triage category
- time to cubicle etc.
These internal ED indicators are key to the review of the flow of patients within the Emergency Department.
Tables and charts generated to show the 'effect' on flow within patient journeys across each staging post. The example provided in Fig 6. is the 'Saturday' chart of a suite of analysis prepared to examine the average time to first assessment within the Emergency Department by hour by day of the week. In this chart a clear spike in average time to 1 st assessment on the Saturday evening is identified. This profile would warrant further analysis of the underlying data and combined with operational knowledge will identify and understand what has caused this increase. Common causes may be due to volume of patients, increased acuity of patients, changes in medical and nurse staffing levels, or a combination of reasons.
Fig 6.
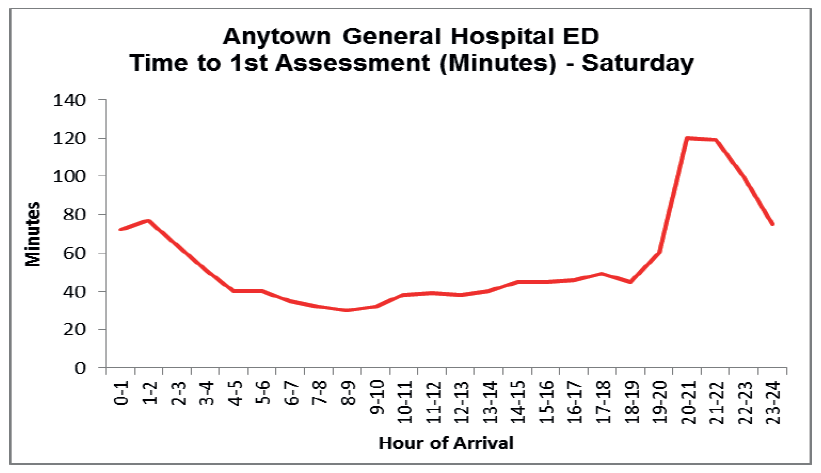
The aim of this detailed analysis is to understand what causes delay to most patients most of the time.
b) Emergency Department Demand Profiling
Understanding the profile of demand is key to managing on a day to day basis. Such information will feed into daily Hospital Safety Huddles and contribute to determining daily prediction of attendance and admission. It supports the planning of services and resources.
The profiling chart in Fig 7. displays box plots which summarise the key statistics relating to Emergency Department attendances numbers per weekday, based on a 12 month dataset. By using a boxplots to display this information average numbers are determined but also includes more detailed information about the range of attendances per day. This includes minimum and maximum numbers recorded and the 85 th percentile average number of attendances.
Daily Profiling
Hospital: Anytown General Hospital
Analysis:
ED Attendances by
Day (Apr 14 - Mar 15)
Fig 7.
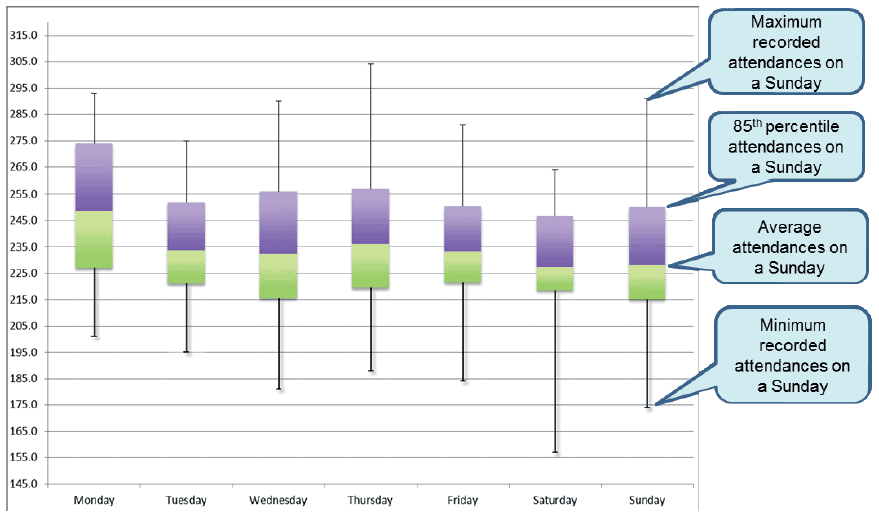
Fig 8.
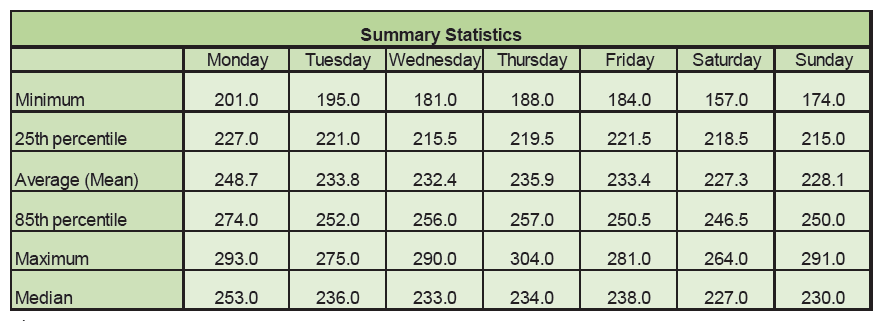
Understanding the Summary Statistics (Fig 7&8.)
85th percentile: For effective capacity planning it is recommended that the upper quartile used is 85%. i.e. You plan capacity to meet demand 85% of the time. In this example the 85 th percentile value on a Sunday is 250 attendances. This means that clinicians and managers can have confidence that on 85% of Sunday's there will be 250 or less Emergency Department attendances.
Average (mean): This statistic is often the most frequently used and as a result is well understood. It is useful to understand average demand levels throughout the week however basing capacity planning on these values should be done with caution, as you are in effect planning capacity to meet demand only 50% of the time. It can however be useful when looking at underlying trends over periods of time. Very often changes in attendance levels or monitoring of system re-design is done by looking at changes to the average attendance levels over a time period.
Maximum and Minimum: Simply the maximum and minimum values recorded throughout the data period for the day. This is useful to understand the full range of the daily attendances and can be further reviewed by using the underlying dataset to identify exact dates of these occurrences. Very often these will be a result of 'special cause' variation, for example post public holidays, specific events. It is always worthwhile to identify these days and examine underlying causes. This can often aid future 'surge' planning.
Using the Summary Statistics
Using a chart, such as the boxplot, can be useful to understand trends and changes in attendance numbers over time. These charts can be produced on a monthly or quarterly basis, and the outputs reviewed to identify changes in patterns, or volume. This type of chart is a good method of keeping track of inter-week variation in attendance levels, as it allows the quick identification of the 'highest' attendance days, not only providing the average numbers, but the range of attendances for that given day of the week. This type of information is very useful when reviewing available capacity, including medical and nurse staffing levels
Emergency Department Arrival Patterns
Analysis of arrival patterns per hour are essential within the Emergency Department to support effective capacity planning. Capacity includes cubicle space, equipment and staffing resource. In the charts below (Fig 9&10.) the average weekday arrival pattern is compared to the weekend. One noticeable difference is the higher attendance levels from 10.00 pm - midnight at the weekend.
Fig 9.
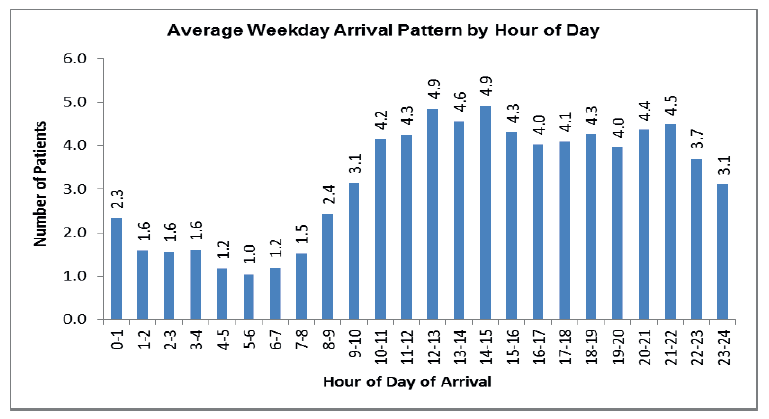
Fig 10.
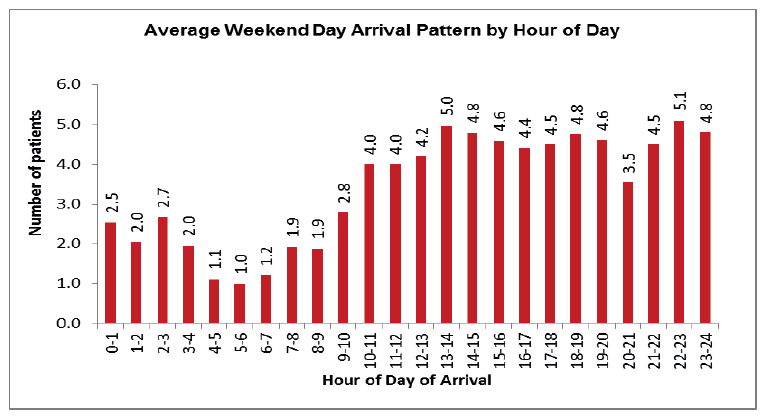
In addition to weekday and weekend arrival profiling, individual daily arrival patterns can be useful. Understanding the total Emergency Department attendances anticipated per day and the arrival pattern supports resource planning. This information, supplemented by analysis on patient acuity, usually done via triage category, can inform decision making regarding the required medical and nurse staffing resource required to meet the anticipated demand at key points in the week.
Emergency Department Average Arrivals versus Departures Profiling
Ideally to maintain balance, the number of arrivals would match the number of departures, per hour. Redressing the balance is crucial to improvement across the whole system and is supported by work across the other Essential Actions, such as EA3 - Daily Dynamic Discharge.
In the graphs below (Fig 11.), a full year of data (for weekdays, Monday to Friday) has been analysed, with the average numbers of arrivals versus the average number of departures per hour displayed.
Fig 11.
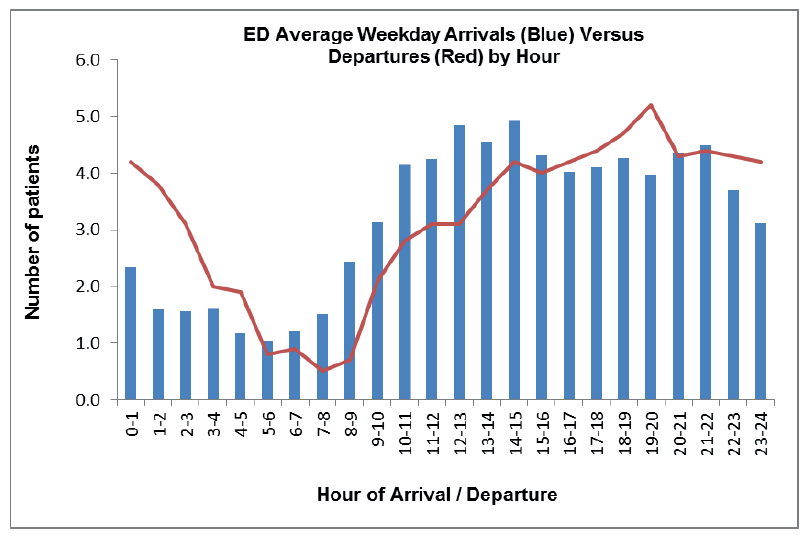
The resulting pattern of arrival numbers versus departures for this Emergency Department is quite common. Through the night the number of arrivals reduces whilst the departure rate is higher as the department slowly starts manage demand and either admit, discharge or transfer patients. From 7 am the average hourly arrivals start to increase, with the number of arrivals exceeding departures until late afternoon. As a result the occupancy of the department will rise significantly during this time period.
When reviewing these graphs, it is important to look for interesting changes in departure or arrival rates, and explore the potential reasons for these. For example in the graph (Fig 11.) shown you will note that throughout the year, on weekdays, the departure rate spikes up between 1900-2000 hours. Recognising where anomalies present leads to further investigation of cause and effect.
One possible explanation may be nursing shift handover time, with a 'push' to ensure those patients ready for discharge or admission are completed before handover. Some improvement activities on completing todays work in hours has proven beneficial in improving this balance profile
It may also be beneficial to create these charts by day of the week, often this can reveal subtle intra week variations which may be attributable to capacity (in terms of physical space or staffing levels), on specific days and times.
Emergency Department Admission and Discharge Rates
Weekly emergency department admission and discharge rates should be prepared to provide a baseline of current system outcomes. These statistics should then be continuously monitored utilising Statistical Process Control ( SPC) charts (Fig 12&13). These charts should be routinely updated and monitored to pick up any developing trends.
Fig 12.
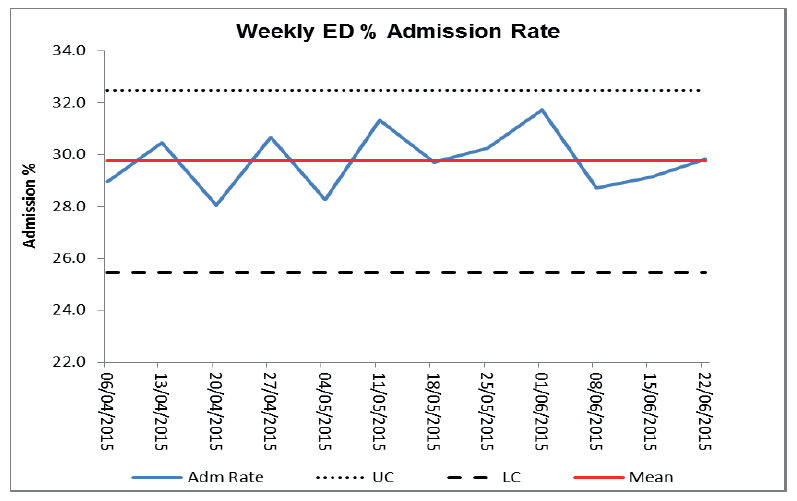
Fig 13.
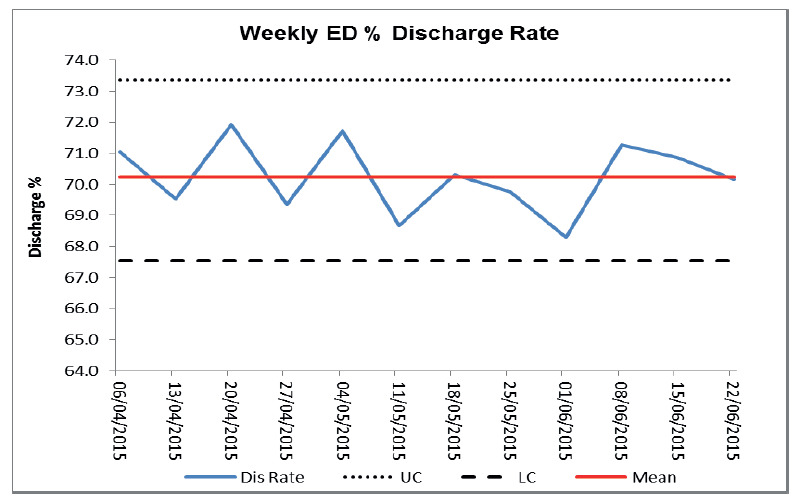
Admission and discharge rates should be reviewed on a day of week basis to identify variations. If as specific day is identified as having a high admission rate it is worthy of further examination to establish cause, such as staffing resource levels on specific days. Similar consideration should be given to weekly average admission numbers, again where increases are noted further investigation of cause should be undertaken to determine cause and identify if internal factors or an external factors, such as increasing incidence of influenza within the community or bad weather with snow and ice etc. This is information for improvement and can identify relevant test of change to minimise variation and reduce resultant delays.
c) Emergency Department Average Length of Stay
Length of Stay is an important metric to monitor within an Emergency Department. An increasing length of stay often drives increasing occupancy levels and capacity pressures within the department. There are a number of ways to monitor length of stay. The aim of monitoring is to allow the identification of increased variation, or longer lengths of stay. Length of stay by week (to identify any trends), and by day (to identify inter-week variations), and also by flow group are useful metrics.
The simple chart below (Fig 14) graphs the average length of stay by week, over a 12 week period and shows the weekly variation.
Fig 14.
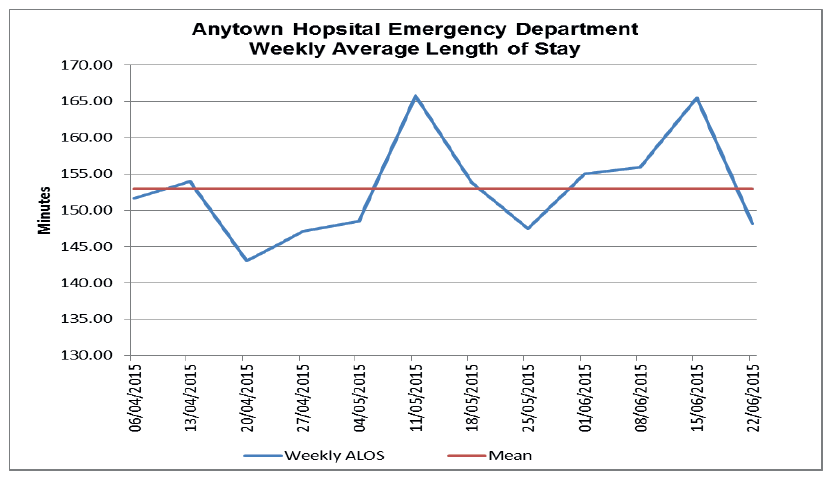
Day of the Week
Further analysis of the same dataset allows you to 'drill down' to identify length of stay variations by day of week, and then flow group.
The chart below (Fig 15) provides the average length of stay by day of the week, from the 12 weeks dataset. It is evident that for 6 of the 7 days the average length of stay is in the range of 153-158 minutes however on a Wednesday length of stay is significantly lower at 138 minutes on average. This variation is worthy of further investigation to understand if this is due to external factors such as reduced attendances which is out with control or improved internal factors such as increased staffing, availability of diagnostics, which if in place would support improvements across the other days of the week.
Fig 15.
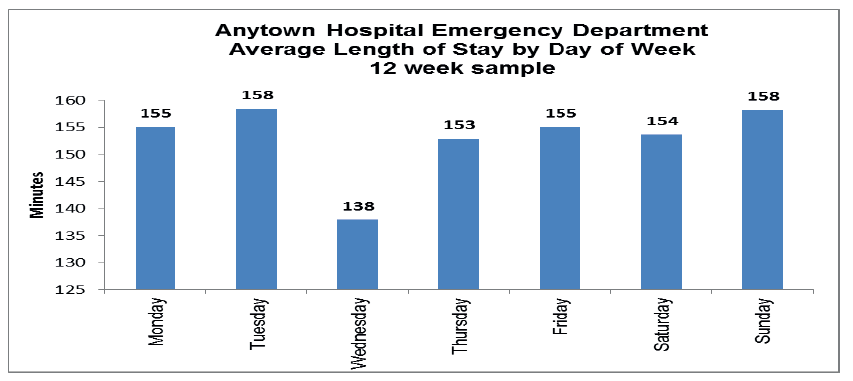
The following table (Fig 16.) provides the average length of stay by flow group. The variation in ED length of stay on these 4 cohorts of patients is evident showing Flow 3 patients have on average the highest length of stay at 230.14 minutes. This type of information is useful in understanding what cohorts of patients are driving the overall average length of stay within the Emergency Department.
Fig 16.
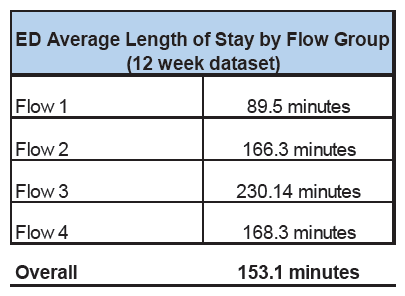
Reducing average length of stay within ED will improve patient flow, decrease occupancy and alleviate the pressure of over-crowding. The data should be used to provide the current baseline metrics but also to identify variation between days or patient cohorts, to identify opportunities for improvement.
d) Emergency Department Occupancy
The occupancy of the unit per hour, per day is important. Many of the other factors we analyse such as attendance numbers and length of stay are the variables which create the occupancy level. A unit's "fullness" significantly impacts on its ability to meet the demand placed on it. High / over occupancy leads to backlogs, poor flow and reduced quality of care for patients. An analysis of occupancy of an Emergency Department over a one week period is shown below. The following table (Fig 17) provides analysis that can and should be generated for longer periods to identify patterns and trends.
Fig 17.
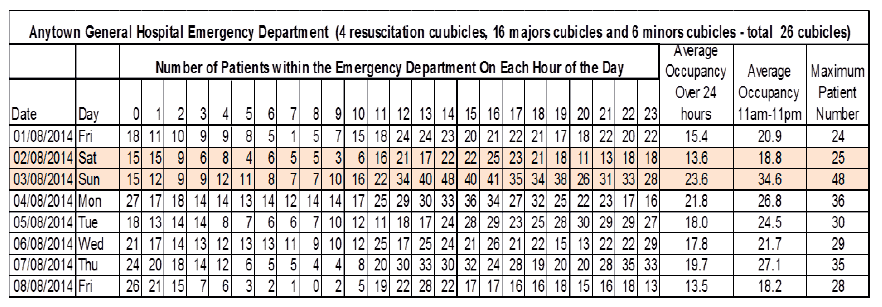
Using the Occupancy Table
The occupancy table provides a raw count of the number of patients within the department per hour of the day. In the 7 day sample provided (Fig 17) the pattern of occupancy across the days and hours within this Emergency Department becomes clear. It is busy at midnight, clearing overnight resulting in generally low numbers at 08.00 am. From 08.00 am occupancy starts to rise, continuing throughout the afternoon and into the evening.
The data within the table can be used to analyse specific days for example in Fig 17 it is evident it is evident that the department remained busy throughout the early hours of Monday. By using occupancy analysis, over a longer time period, it is possible to compare the profile for a number of Mondays. This will confirm if the trend identified on this individual Monday was unusual or is the Sunday nightshift into Monday morning always busy.
The occupancy numbers generated are the 'effect' of patient's numbers and length of stay. High attendances or increasing length of stay will all contribute to increasing occupancy. Although high levels of occupancy usually exhibit a high correlation with lower performance against the 4 hour Emergency Access Standard, the numbers themselves do not fully describe the pressure or 'busy-ness' of a department. Other factors can significantly impact occupancy levels, such as patient acuity.
Where periods of high occupancy have been identified, to establish the cause it is important to review other data for the same time period, such as patient numbers by triage category by hour, and staffing profiles etc. This will ensure that all the contributing factors are considered and will create a fuller picture of the 'pressure' within the Emergency Department. This information will help focus improvement by identifying the peak 'pressure' times within the department.
The occupancy template used to generate these figures has been distributed to Board's Data Analysts, following a workshop in December 2015. This tool can be used, not only to generate the initial baseline of occupancy levels in the Emergency Department, but is useful for monitoring the impact on improvement work over a period of time.
Contact
Email: Unscheduled Care Team