Alcohol Framework 2018
Updated framework setting out our national prevention aims on alcohol.
Section 1 - Introduction
Updating the 2009 Framework for Action
1. Scotland’s 2009 alcohol strategy, the Framework for Action[1], is well established. Many of our original actions have been completed, with others continuing and evolving. We have taken, and will continue to take, an evidence-based approach to our alcohol strategy. This updated Framework retains three central themes, which are well accepted and understood:
- Reducing consumption
- Positive attitudes, positive choices
- Supporting families and communities
2. This document sets out our national prevention aims on alcohol: the activities that will reduce consumption and minimise alcohol-related harm arising in the first place. This is consistent with Public Health Priorities for Scotland[2] where one of the priorities is a “Scotland where we reduce the use of and harm from alcohol, tobacco and other drugs.” An overarching strategy for prevention and treatment of alcohol and drugs, setting out our support for individuals, for families and for communities, will follow.
Scotland’s alcohol policy on the world stage
3. With the introduction of minimum unit pricing on 1 May 2018, Scotland has truly become a world-leader on alcohol policy. We will continue to share our experiences within Europe and internationally. In 2015, Scotland hosted the Global Alcohol Policy Alliance Conference[3]; the only European country asked to host the conference. In 2016, Scotland was awarded the inaugural European Reducing Alcohol Harm[4] Award at the 7th European Alcohol Policy Conference (EAPC) in Slovenia, and we are delighted to be hosting the 8th EAPC[5] in November 2018, in Edinburgh. The United Nations (UN) recognised the Scottish Government’s contribution towards tackling non-communicable diseases with a UN Interagency Task Force Award[6] for its work on minimum unit pricing in 2018.
A balanced approach
4. The Scottish Government’s focus is on preventing and reducing alcohol-related harm. Tackling higher-risk alcohol use forms a significant part of reducing alcohol-related harm. We define higher-risk alcohol use as drinking above the lower-risk maximum amounts advised in the UK Chief Medical Officers’ (CMOs) guidelines[7]. This means that higher-risk is a broad range which covers those who drink marginally above the guidelines to those who drink significantly above them. The guidelines were revised across the whole of the UK in 2016 after a thorough evidence review, because that is the best way to minimise risk of harm for the people of Scotland. A summary of the guidelines is provided at Annex A. They recommend a maximum of 14 units of alcohol per week for both women and men to keep health risks low, preferably spread over three or more days, with no drinking at all during pregnancy.
Lower-risk drinking guidelines for men and women

5. We will continue to work with a wide range of stakeholders to reduce alcohol-related harms, including Health and Social Care Partnerships, Alcohol and Drug Partnerships, other local partners and the third sector. We will also work jointly with industry, where that is appropriate. Where we do so, we will set the bar high and collaborate only on projects which can impact meaningfully on reducing alcohol harms. The Scottish Government will not work with the alcohol industry on health policy development, on health messaging campaigns or on provision of education in schools and beyond the school setting. Our approach to joint work with the industry will be based on the principles of the World Health Organization (WHO) Global Strategy to reduce the harmful use of alcohol, which recognises industry’s role as developers, producers, distributors, marketers and sellers of alcohol products[8].
A ‘whole population’ approach
6. We continue to take a whole population approach which aims to reduce alcohol consumption and the risk of alcohol-related harms across a population, because Scotland’s consumption remains too high. In 2017, Scots bought enough alcohol (10.2 litres of pure alcohol) for everyone aged over 16 to drink 19.6 units of alcohol every week[9]. This is equivalent to 40 bottles of vodka, or around 100 bottles of wine, per adult each year. This is 40% more than the lower-risk CMO drinking guidelines of 14 units. Sales data provide information on how much we are drinking in totality whereas the Scottish Health Survey is useful for providing information on our pattern of drinking. The latest Survey (2017[10]) shows that 24% of adults drank above the lower-risk guidelines, which is down from 34% in 2003; and the proportion of adults saying they did not drink alcohol increased from 11% in 2003 to 17% in 2017. These figures are encouraging, however, as self-reported survey estimates of consumption are typically lower than estimates based on sales data, it is the sales data that provide a more accurate picture of how much we are drinking as a nation.
7. Alongside a whole population approach, we continue to progress interventions targeted at those at most risk, such as Alcohol Brief Interventions and a suite of treatment options. Our approach is aligned with WHO[11] and Organization for Economic Co-operation and Development (OECD)[12] strategies to tackle the harmful use of alcohol. Prevention measures are key, and we follow the WHO approach of placing the three prevention ‘A’s front and centre: Affordability, Availability and Attractiveness.
8. Building on the ‘three As’, in September 2018, WHO launched its new SAFER initiative[13], which is backed by a range of partners including the United Nations. SAFER is a package of five evidence-based, high impact strategies which WHO recommends governments should prioritise to tackle alcohol-related harm.
Strengthen restrictions on alcohol availability.
Advance and enforce drink driving countermeasures.
Facilitate access to screening, brief interventions, and treatment.
Enforce bans or comprehensive restrictions on alcohol advertising, sponsorship, and promotion.
Raise prices on alcohol through excise taxes and pricing policies.
The Scottish Government fully endorses the new SAFER initiative, and will work to support and promote this approach within Europe and worldwide.
A well-connected approach
9. It is crucial that government understands people’s motivations for drinking. The same is true for all public and private sector actors who seek to influence alcohol behaviours. We also need to recognise that some cultural norms around drinking have become so deeply embedded that they cannot be turned around through short-term action. Two consistent threads run through this document: (i) our actions must reduce health inequalities; and (ii) our actions must protect children and young people. The evidence on the effects of alcohol on the developing adolescent brain is strong[14], and we now know that brain development continues until the mid-twenties so we need to be mindful of this when developing policies to protect young people.
10. Where we strive to change behaviours, we need to enable positive and sustainable changes in the conditions that can drive behaviours in the first place. It is vital to recognise and address the wider, social determinants of health in policies across government. To maximise the impacts of our updated alcohol strategies, we must connect into the policies and programmes that are tackling some of the fundamental issues of our times. This includes, but is not limited to, enabling and supporting positive mental health; reducing poverty and tackling inequalities at source; providing good quality housing and ending homelessness; enabling the best starts in life for our children, including recognising the impact of adverse childhood experiences; improving the life circumstances of children, young people and families at risk; improving social connectedness, community cohesion and safety and evolving our justice system to improve outcomes for individuals, families and communities. NHS Health Scotland’s work illustrates the importance of ‘place’ to health[15].
Scotland’s progress
11. We have already:
- changed the way alcohol is marketed with the introduction of the quantity discount ban, associated with a 2.6% reduction in consumption[16];
- banned irresponsible promotions, so consumers are not encouraged to drink more than they intended;
- introduced restrictions on where alcohol and associated marketing can be displayed by retailers to curb impulse purchases;
- rolled out a nationwide programme of alcohol brief interventions, delivering over 834,000 since 2008/09;
- worked to protect our children and young people from alcohol-related harm through the introduction of a mandatory age verification policy, such as Challenge 25, to make it harder for young people to obtain alcohol;
- continued work to equip our young people to make better decisions through improved substance use education and access to positive alternative activities;
- worked to make our communities safer through a range of initiatives to tackle alcohol-related violence and crime and to encourage safer drinking environments;
- legislated to crack down on those who supply to under-18s: the Air Weapons and Licensing (Scotland) Act 2015[17] (the 2015 Act) made it an offence to supply alcohol to under-18s in a public place, giving police the power to address the problem of groups of underage people drinking in public;
- further protected young people through the 2015 Act, which broadened the ‘protecting children from harm’ licensing objective to include young persons aged 16 and 17, rather than just those under 16, allowing Licensing Boards to more appropriately consider the range of issues involving children and young persons; and
- made our roads safer with the introduction of a lower drink drive limit, bringing Scotland into line with the majority of other European countries.
12. Most recently, we have introduced minimum unit pricing for alcohol on 1 May 2018, which will save lives and reduce hospital admissions. In 2017, 47% of alcohol sold in the off-trade was sold at less than 50 pence (Figure 1). Minimum unit pricing is a structural pricing intervention in the alcohol sales market.
Figure 1: Price distribution (%) of pure alcohol sold off-trade in Scotland, 2017[18]
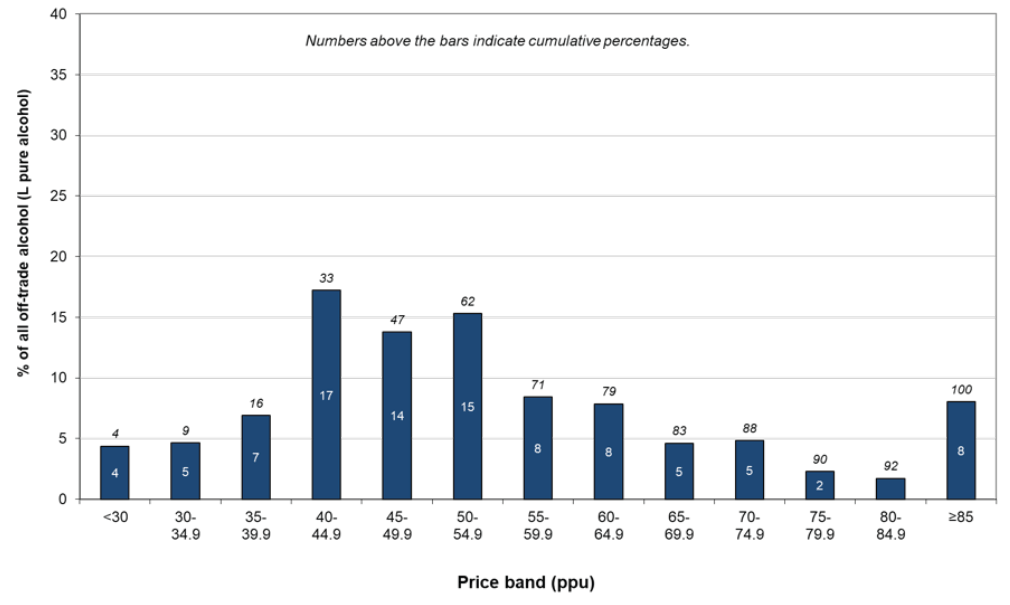
13. Modelling by the University of Sheffield[19] estimates that the new minimum price of 50p per unit from 1 May 2018 is estimated to result in 58 fewer alcohol-related deaths and 1,299 fewer alcohol-related hospital admissions in the first year. That accumulates to 392 fewer alcohol-related deaths and 8,254 fewer alcohol-related hospital admissions over the first five years. For some illnesses that are associated with drinking alcohol, it will take a long time to see the full benefit of drinking less. It may take 20 years for all the benefits of the policy to be realised. After 20 years, it is estimated there could be 121 fewer deaths and 2,042 fewer hospital admissions each year. That accumulates to 2,036 fewer alcohol-related deaths and 38,859 fewer alcohol-related hospital admissions over the 20 years.
The present picture
Sales
14. After a fall between 2009 and 2013, alcohol sales in Scotland have remained broadly stable up to 2017[20]. This more than likely reflects the economic climate over that period. The shift from purchasing alcohol in pubs, clubs and restaurants (on-trade) to supermarkets and shops (off-trade) has been dramatic – off-trade sales have seen a 42% increase since 1994. Of all alcohol sold in Scotland in 2017, 73% was sold through the off-trade. This means that we have gone from drinking in a social, regulated environment in pubs and clubs to now drinking in a largely isolated, non-regulated environment at home. Since the 1980s, we have seen substantially increased alcohol consumption in Scotland and, consequently, high levels of alcohol-related harm.
Harms
15. Alcohol-related hospital admissions have reduced 20% since 2007/08, but are still over four times higher than in the early 1980s (Figure 2). Overall, mortality rates have fallen 30% from a 2003 peak, but are still over twice as high as in 1981 (Figure 3). We also recognise that, within a whole population approach, some groups are affected more than others: those in the most deprived areas are impacted more than those in the least deprived[21]; adult drinkers aged 45 to 64 reported the highest mean weekly consumption in 2016[22]. Although men overall drink almost twice as much as women, there is more stigma attached to women drinking[23]. The LGBTI community experiences significant health inequalities around higher-risk alcohol use[24]. And we need to remember that harms are not experienced solely by the drinker, but also by family and friends, communities and employers[25].
Figure 2: Alcohol-related hospitalisation rates, Scotland, 1981-2016/17[26]
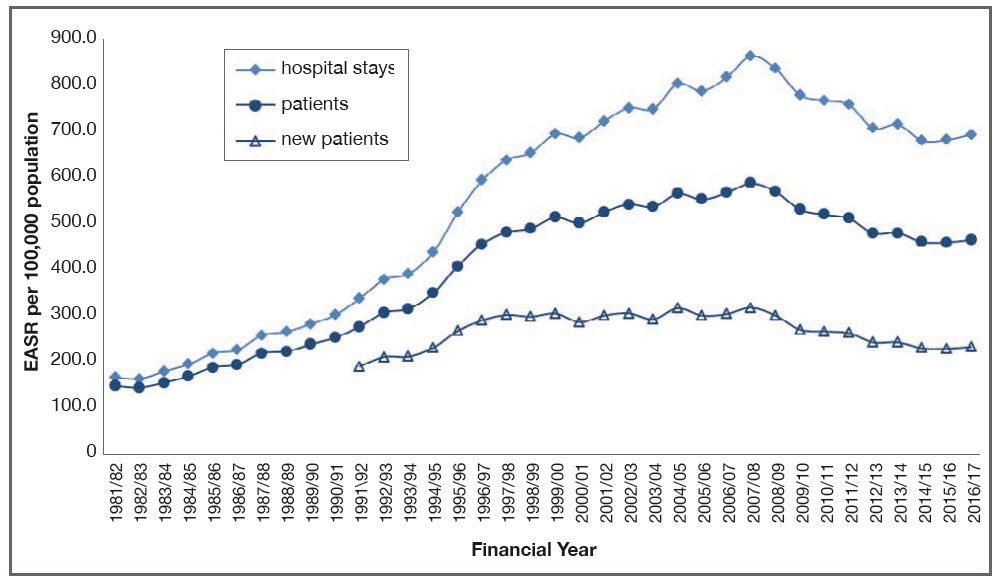
Figure 3: Alcohol-specific death rates overall and by gender in Scotland 1981-2017[27, 28]
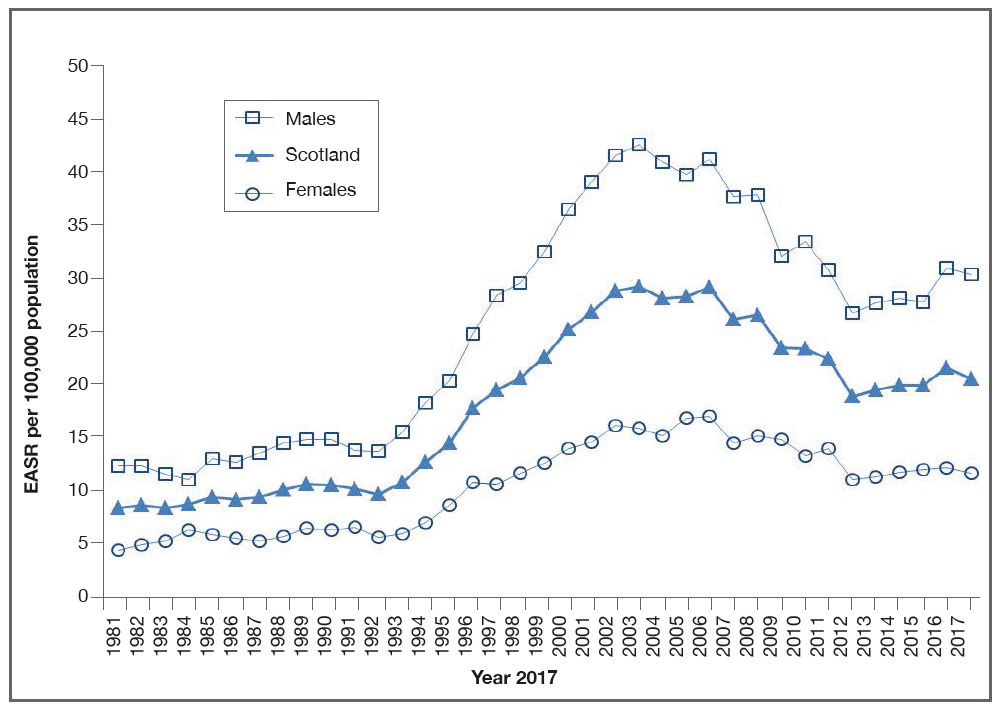
16. Our Framework is having an impact, as demonstrated by the MESAS Final Report 2016[29]. There are some encouraging trends, particularly regarding young people with the proportion of 13 and 15 year olds who drank alcohol in the last week being at its lowest since 1990[30]. And the introduction of minimum unit pricing will see a step change in saving lives and preventing hospital admissions. However, Scotland requires a sustained focus on alcohol harm reduction. The present population-level harms, of 22 deaths[31] and 697 hospital admissions[32] on average per week due to higher-risk alcohol use, are simply too high.
17. So, too, is the economic cost. Alcohol misuse costs Scotland far too much in financial terms – in 2010, this was found to be a staggering £3.6 billion each year, using 2007 data[33]. To put this into perspective, that’s an average of £900 for every adult. The total includes estimated annual costs to the NHS of some £140 million - £400 million each year. We are presently updating these data; however, with the enduring levels of harm we experience as a nation, this is likely to continue to point towards a very substantial national burden.
International comparisons
18. Scotland has high rates of alcohol-related harm in international terms[34], as does the UK. In 2016, the latest year for which comparable figures are available, total alcohol consumption in the UK (11.4L) was more than 16% above the European regional average (9.8L[35]). Even though only half the world’s population drinks alcohol, it is the world’s third leading cause of ill health and premature death[36]. Prevalence of Chronic Liver Disease and cirrhosis (closely associated with heavy alcohol consumption) remains high by comparison with other European countries. Where data are available, Scotland, along with Hungary and Finland, had the highest Chronic Liver Disease mortality rates in 2014[37]. Although they have decreased since peaking in 2003, rates remains 20-40% higher than in Austria, Germany and Poland; over twice that experienced in Spain and Sweden; and almost six times that of Norway. Closer to home, per adult sales were 14% higher in Scotland than in England and Wales in 2017[38].
Contact
Email: Alison Ferguson