Achieving excellence in pharmaceutical care: a strategy for Scotland
Strategy aiming to transform the role of pharmacy across all areas of pharmacy practice, increase capacity, and offer the best person-centred care.
3. Improving NHS Pharmaceutical Care
Context
Don Berwick, President Emeritus and Senior Fellow of the Institute for Healthcare Improvement ( IHI), promotes seeking excellence through the eyes of the people we serve. Achieving excellence in pharmaceutical care consists of a number of components, but at its core is playing to the strengths of pharmacists, pharmacy technicians and other pharmacy support staff. Unlocking this capacity in an incremental and structured way is the fundamental objective of the priorities set out in this strategy. The National Clinical Strategy [4] sets out a high level vision to guide how services will develop over the next 10-15 years, with strong primary and community health services planned around individuals and their communities, opening access to care and enhancing the quality of care, improving outcomes and ensuring we have sustainable services for all.
In primary care we need to build capacity and provide a more broadly based mix of professionals based around GP practices which will be increasingly working in clusters and working closely with social care and voluntary agencies. In secondary care we must consider the potential for developing fewer inpatient sites that will provide more highly specialised services, linked into local hospitals providing a comprehensive range of outpatient, diagnostic and day case surgery.
The community pharmacy network located at the heart of our communities, pharmacists and pharmacy technicians working in, and with, general practice and the specialist roles pharmacists and technicians bring to our hospital care are already making a significant impact on delivering improved health and social care services. In addition, the specific contribution the entire pharmacy team can bring to improving the overall care in remote and rural communities and settings such as care homes or care at home is not only where further capacity can be unlocked, but importantly maximises the opportunities to embed the safer use of medicines at every point of healthcare.
Care is increasingly provided by multidisciplinary teams, including GPs and consultants, nurses, allied healthcare professionals, pharmacists, pharmacy technicians, social workers, social care staff, the voluntary sector and other specialists working together. This means that each member of the team needs to be aware of their own specific role(s) as well as how to play to each other's strengths and skills. An increasing focus on improving the quality of care and achieving better health outcomes for the population, and in particular for people with multiple and complex long term conditions, requires improved pathways of care based on integrated, multidisciplinary team-based care which is preventative, anticipatory and proactive in nature. It also requires improved access to data and information through a more coordinated approach to appropriate data sharing, and ensuring that the right digital culture, skills, processes, tools and systems are in place.
The pharmacy team has a unique and specialist knowledge of medicine and there is a need to ensure services are structured so that when a member of the public or healthcare professional and/or social care organisation needs a medicine or advice and information about medicines the appropriate member of the pharmacy team is positioned to lead on ensuring this provision. Other team members will fulfill other roles but this clarity of function will improve multidisciplinary working and outcomes for people and practitioners alike.
Health and Social Care Delivery Plan [5]
The Health and Social Care Delivery Plan sets out clear actions and milestones to create modern, sustainable health and social care services within a single delivery framework. There is a firm emphasis on the integration of health and social care, an even greater shift of the balance of care from hospital to community setting, necessitating whole system redesign across acute and primary care, with multidisciplinary team working and service delivery driven by frontline practitioners, particularly in primary care.
Primary care transformation
The transformation of primary care establishes the planning and delivery of services through a multidisciplinary, community-based approach, centred around clusters of GP practices working collaboratively. There is an acknowledged need to increase resources in primary and community care to support this approach, including better use of the skills of pharmacists and pharmacy technicians, to ensure that care is person-centred, peer-led and values-based, so that people can be treated close to home, or in a homely setting, where it is safe to do so. Pulling Together [6] , Sir Lewis Ritchie's review of out-of-hours services describes plans to transform out-of-hours urgent care and envisages extended roles for pharmacists in delivery of primary care out-of-hours, focusing on the need for multidisciplinary teams to work together to provide care.
Realistic Medicine [7]
The Chief Medical Officer's report, Realistic Medicine, gives a clear direction on how we should now be approaching healthcare provision and the transformational change that NHS pharmaceutical care provision needs to undergo to allow the pharmacy profession to play its full part.
Self-management and medicines
Pharmacists and their teams are well placed to support people to self-manage their care which is a core component of providing person-centred pharmaceutical care. We know from existing evidence that personalised care planning leads to improvements in both health outcomes and a person's capability to self-manage their condition compared to routine care. An important aspect of this includes the need to be responsive to people's health literacy needs as described in Making it Easy [8] , our health literacy action plan. In addition, the impact is greater when it is embedded into routine care. Pharmacists, working across all care settings, are ideally positioned to take on an increased clinical role in delivering clinical care and ensuring informed decision making and medicines safety approaches are integral to the pharmaceutical care they provide. This needs to be further strengthened by access to and sharing of electronic health information and data. This will help ensure that pharmaceutical care is genuinely designed around the needs and wishes of each individual person, making the right decisions together with them at the right time: from 'what is the matter with you?' to 'what matters to you?'
"Our focus is on achieving excellence in NHS pharmaceutical care provision to ensure safe, effective and person-centred care."
Person-centred pharmaceutical care
The evolving focus of pharmacy practice to ensure that people have an understanding of what to expect from their medication requires an acknowledgement that people and their carers rightly wish to be active partners in treatment options. This involves balancing a person's preferences and expectations alongside the provision of evidence-based interventions. For truly shared decision-making there needs to be a shift towards participative care meaning that there is an acceptance by professionals of a situation where people may choose something different from what has been traditionally offered. This shared approach to personalised pharmaceutical care can be challenging, but one where collaborative practice is beneficial.
In Realising Realistic Medicine [9] Sir Muir Gray refers to the 'point of optimality' as being one of the most important concepts in healthcare. It shows how benefits to people increase rapidly with investment of resources, but then level out, even though investment increases, whereas harm rises in a straight line. In other words, the more we do the more harm we cause because the procedures we carry out have risks. Pharmacists, with their expertise in medicines, have a critical role in identifying medicines with limited or no value or that have a higher risk benefit ratio and by working in collaboration with other clinicians can reduce the burden of harm in relation to medicines at multiple points in the care pathway.
The pharmacy profession has a key role in empowering people and the carers who support them to make best use of the services on offer, enabling people to take an increased role in making decisions about their medicines and care. The success of this is also dependent on informed and engaged individuals and carers developing new relationships with care providers. People want to know what services are available: where to access them, how to use them, being clear about how their pharmacist can support them and being aware of the supported self-management approaches they can use to manage their illnesses and conditions, including self-referral to other services, such as physiotherapy, rather than only the GP.
Working in partnership with NHS Boards, HSCPs and partners including the Scottish Health Council and the Health and Social Care Alliance, we have been involving people and carers to build an understanding of their experience of pharmacy and how this can help to inform the design of NHS pharmaceutical care provision. We will continue to work in partnership with them to develop a mutual understanding of how best to achieve shared clinical decision making and person-centred pharmaceutical care.
The work, started initially through Prescription for Excellence, and now being taken forward through the priorities highlighted in this strategy, aligns what we are doing in pharmacy with recent policy developments outlined in the Health and Social Care Delivery Plan, the National Clinical Strategy, Pulling Together, the Modern Outpatient Collaborative [10] , Realistic Medicine, the Mental Health Strategy [11] and the six essential actions to improve unscheduled care. It is helping us better understand what is required for the integration of pharmacy and pharmaceutical care into a person's experience of health and social care.
Our focus is on ensuring safe, effective and person-centred pharmaceutical care, and safer use of medicines is a core component of health and social care services in all settings. These settings include care homes and those requiring more care at home. We need to understand the enablers to deliver this which includes identifying the clinical capability and capacity required within the pharmacy workforce, the resources needed to improve IT system interoperability and leverage digital technologies and data and modernising our planning and delivery systems for securing NHS pharmaceutical care services.
Inherent to improving service provision within particular care settings is improving the transitions between settings. This means considering how to make best use of the pharmacy resources in order to improve how we deliver services, and that people, irrespective of where they are, have access to and receive the pharmaceutical care that they require. The commitments set out in the rest of this chapter tend towards describing pharmacy services within existing structural boundaries however we recognise the need for ongoing flexibility as new ways of working are embedded as part of the transformational change across our health system required to meet people's health and social care needs and preferences.
Community pharmacy
Commitment 1:
Increasing access to community pharmacy as the first port of call for managing self-limiting illnesses and supporting self-management of stable long term conditions, in-hours and out-of-hours.
Actions
Minor Ailment Service
Chronic Medication Service
Public Health Service
Serial prescribing & dispensing
Independent prescribing & advanced clinical skills
Community pharmacy already plays an important role in the provision of NHS pharmaceutical care, providing highly accessible services for people both in-hours and out-of-hours. We want more people to use their community pharmacy as a first port of call, not only for the treatment of self-limiting illnesses and medicine-related matters, but for the on-going self-management support for people with long term conditions. Enhancing these services also expands the clinical role of community pharmacists. In addition to this, Pulling Together identifies the need for community pharmacy to play its part in the proposed Urgent Care Resource hubs which will be multidisciplinary and will involve a range of healthcare providers. This may be through working directly in hubs on a sessional basis, or alternatively, supporting these hubs through the services they provide in their community pharmacies via referrals to and from the hubs. Appropriate two-way sharing of information is also required to allow and support this.
Good progress is being made towards delivering the pharmacy recommendations from Pulling Together, including funding in 2017 to roll out the 'Pharmacy First' initiative based on work originally started in NHS Forth Valley. This enables community pharmacists to treat some additional self-limiting conditions such as uncomplicated urinary tract infections and impetigo. This is improving access for people requiring assessment and treatment, reducing pressure on GP practices and out-of-hours services and maximising the skills of pharmacists.
Action:
We will target resources to expand the number of community pharmacists undertaking independent prescribing and advanced clinical skills training. This includes exploring how resources to cover back-fill for the residential training and period of learning in practice can be provided in order to build clinical capacity to deliver an extended MAS and enhanced CMS.
Minor Ailment Service
The Minor Ailment Service ( MAS) was introduced in 2006 and has allowed specific groups of people to access treatment for self-limiting illnesses such as fungal infections, allergies, skin conditions and infestations on the NHS without the need for an appointment with a GP. Through exploring opportunities to expand the MAS in Inverclyde we are looking to extend eligibility to more people and expand the range of conditions that can be treated. This is in line with the recommendations in Pulling Together and builds on the Pharmacy First initiative.
An extended MAS has the potential to improve access to treatment for a range of uncomplicated illnesses normally requiring a prescription. It more fully utilises the clinical skills of pharmacists and reduces demand on GP practices, out-of-hours and Emergency Department workload. This, in turn, helps address capacity issues across the wider primary care team in-hours and out-of-hours. Many community pharmacies are open at times considered to be out-of-hours by other parts of the service, in the evening and at weekends and this is a strength for the whole primary care team. It also serves to re-emphasise community pharmacy as the first port of call for healthcare advice and support, using their accessibility and 'walk-in' mode of delivery to its full advantage both in-hours and when GP practices are closed. As part of this work we are testing improved communications between pharmacies and GP practices in order to inform how we best underpin this going forward using appropriate work-flowed electronic processes. This will include details of what treatment has been provided.
Inverclyde extended MAS pilot
During 2017, an extended MAS is being piloted in Inverclyde as part of the Inverclyde New Ways of Working Programme. The pilot involves extending MAS eligibility to all individuals registered with a GP practice in Inverclyde. It also expands the range of conditions that can be treated by use of Patient Group Directions ( PGDs) in the first instance to cover conditions such as impetigo, uncomplicated urinary tract infections in women, shingles, bridging contraception and exacerbations of Chronic Obstructive Pulmonary Disease ( COPD) for patients with self-management plans.
The Inverclyde extended MAS pilot is focusing on utilising the clinical skills of the pharmacist, and any future expansion of the service will benefit from as many community pharmacists as possible undertaking independent prescribing and advanced clinical skills training to allow them to extend the conditions they can treat and prescribe a wider range of medicines without relying on the use of PGDs. Again, this is also aligned with recommendations within Pulling Together. The Inverclyde pilot is due to report early in 2018.
Action:
We will use the evaluation of the Inverclyde extended MAS pilot to inform any future enhancements to the national Minor Ailment Service.
"People tend to default to going to their GP for advice about medicines and are not fully aware of the expertise and services offered by their community pharmacist."
Chronic Medication Service
We are also strengthening and refreshing the Chronic Medication Service ( CMS) in order to improve how it enables community pharmacists to provide personalised care for people with stable long term conditions . As experts in medicines and their use, pharmacists play a crucial role in supporting people to use their medicines to achieve the best clinical outcomes, as part of an ongoing partnership with them to manage their healthcare. Based on feedback from people using the service we will also change the name of the service to reflect a more positive person-centred image.
The registration of people for CMS continues to increase, as does the number of people with pharmaceutical care plans. However, we know that there is much more to do. We are currently piloting the development of a pharmaceutical care bundle approach, which is a set of evidence-based interventions that when used together can significantly improve clinical outcomes. We are also working to enhance the Pharmacy Care Record ( PCR) to introduce an annual pharmacist-led medication review traditionally carried out by a person's GP. Introducing a formalised medication review will help identify people who will benefit from a more detailed pharmaceutical care plan in a more systematic way than present. It also plays to the skills and strengths of pharmacists in that there is good evidence that community pharmacy based medication reviews can reduce the risk of drug-related problems and improve the appropriateness of prescribing. In addition, a number of community pharmacists are providing additional initiatives such as condition specific clinics to support people with long term conditions.
Community pharmacist-led clinics
A community pharmacist Parkinson's clinic in NHS Tayside offers more frequent contact with people between Parkinson's annual review clinics. People attending typically have polypharmacy issues and the pharmacist reviews their pharmaceutical care needs and agrees an action plan, with a follow-up home visit carried out by a pharmacy technician. The pharmacist liaises with the person's GP practice to feed back on any care issues requiring their input.
Long term condition management
Another important improvement we wish to make to CMS is enhancing pharmacists' interventions by building on the current focus on consultation, medication review, care planning and education to include more monitoring and prescribing. This builds on the work currently being undertaken by community pharmacists providing pharmacist prescribing clinics. By playing to pharmacists' core skills, this improvement will develop the current service where community pharmacists are limited to making recommendations to GPs about changes to medicines.
It will also help embed and mainstream community pharmacist-led prescribing clinics. This means that over time community pharmacists will be enabled to play a greater role in managing people with long term conditions, by prescribing, monitoring and adjusting medicines, working alongside pharmacists in GP practices, GPs and other members of the multidisciplinary team. Work has also commenced towards widening secure sharing of electronic information and data, where this is appropriate, to underpin best care and to facilitate informed decision making and optimal communications with other health and social care services.
In support of this enhancement to CMS we will make improvements to the PCR to improve the measurement and sharing of outcome data. This will allow us to better quantify the benefits from pharmacist interventions and their contribution to improving health outcomes as part of the multidisciplinary team.
Action:
We will further develop the Chronic Medication Service to incorporate a more formalised role for community pharmacists in managing people with long term conditions by building in medication review, prescribing, monitoring and dose titration. We will enhance the Pharmacy Care Record in order to record and share outcome data to improve health outcomes and benefit person-centred care.
Serial prescribing and dispensing
The serial prescribing and dispensing element of CMS has the potential to reduce workload for both GP practices and community pharmacies. However the rate of uptake of serial prescriptions remains low meaning that benefits for people with stable long term conditions, GP practices and pharmacies are not being attained. In the main this is because it requires a front-loaded investment of time to identify and transfer people from a repeat to a serial prescription. Using a quality improvement approach we are currently undertaking tests of change to explore different processes that will increase the use of serial prescriptions and help us to realise the full potential of the service. An action plan has been developed to support the embedding of serial prescribing and dispensing into every day practice and there are clear links with how it can reduce GP practice workload and help deliver on a range of GP practice sustainability commitments. There are also opportunities to align with aspects of Realistic Medicine with regards reducing harm, variation and waste, supporting person-centred care and shared decision making.
Action:
We will encourage HSCP to maximise the use of serial prescribing and dispensing to benefit people, utilise community pharmacy more effectively and ease the workload on GPs. We will support engagement between GP practices and community pharmacies and provide enablers to embed serial prescribing and dispensing into normal working practice.
Public Health Service
Community pharmacists are highly accessible primary care practitioners and provide a unique opportunity to improve signposting and access to information and services. This includes the most vulnerable in our communities such as people with mental health problems, homeless people and substance misusers, all of whom might have difficulty in accessing mainstream healthcare. The Public Health Service ( PHS) element of the contract has made a significant contribution to areas such as smoking cessation and access to emergency hormonal contraception, demonstrating measurable impact at both individual and population level. We will continue to build on this and enhance the valuable public health role of community pharmacists as well as other members of the pharmacy team. The newly formed GP cluster groups provide an opportunity to further define local public health priorities. One of the early priorities we will take forward is a review of the existing sexual health service which allows community pharmacists to provide emergency hormonal contraception. Following on from recent guidelines we will consider the introduction of bridging contraception with the possibility of including long acting contraception at a later stage.
Action:
We will work at a national level to expand the public health role in community pharmacy with evidence-based interventions that add value. We will direct NHS Boards and HSCPs to consider opportunities to utilise community pharmacy to help meet local needs.
Community Pharmacy gluten-free food service
Work to co-design a Coeliac Disease Clinical Pathway has resulted in a community pharmacy Gluten-Free Food Service being embedded in the pathway. The pathway ensures people are supported to self-manage their gluten-free diet using the community pharmacy rather than the GP practice for access to the products they require. The service includes an annual Coeliac Disease health check provided by the community pharmacist.
GP practice-based pharmacy
Commitment 2:
Access to GP practice based pharmacy
Integrating pharmacists with advanced clinical skills and pharmacy technicians in GP practices to improve pharmaceutical care and contribute to the multidisciplinary team.
Through the Primary Care Fund, NHS Boards are being supported to build capacity around pharmacists with advanced clinical skills, or those undertaking this training, and pharmacy technicians in GP practices. These pharmacists and technicians are working directly with GP practices to free up GP time to spend with people with more complex care needs. Boards are targeting resources towards priority areas at a local level based on patient need, including areas with a greater proportion of elderly people, deprived areas, and people with multiple morbidities who receive a significant number of prescriptions and who have been identified as being more at risk of hospital admission or readmission.
The primary role of these practice-based pharmacists is to deal with the many medicine-related problems and issues that arise in every GP practice on a day-to-day basis and to support people in the management of their long term conditions. The support they provide covers, but is not limited to, improving medication management systems, including: formulary compliance, hospital outpatient requests, and repeat prescribing management. They also provide polypharmacy and medication reviews, including high risk medicines, and take on the management of people with more complex, multiple conditions where they are taking decisions with the individual on the use of their medication and monitoring and adjusting treatment prescriptions where appropriate. By taking on this role these pharmacists are improving clinical outcomes for people, reducing workload for GPs and other members of the multidisciplinary team, freeing capacity for them to focus on those with undifferentiated illness or other complex health needs.
There is also an important role for GP practice-based pharmacists, at the interfaces of the profession, working closely with hospital pharmacists, community pharmacists and care homes to ensure seamless care and reduce potential medication related problems and errors. There are good examples of how they are also working closely with community pharmacists to review people's medicines, particularly those who have complex conditions or who take medicines with a higher element of associated risk. They can also ensure that, for people who are admitted and discharged from hospital, any medication changes are reconciled and updated. An evaluation of the GP practice-based pharmacists programme has been commissioned to capture the learning and inform any models for future practice developments.
Pharmacist-led medication review
A Dundee GP practice introduced pharmacist-led medicine reviews working in multidisciplinary teams for frail and elderly people. One person taking multiple medicines had problems with recurrent falls, urinary tract infections and anxiety. A review of their medication and blood tests led to a change in medication and dosage. This was coupled with frequent visits from the locality nurse and fortnightly follow-up calls from the pharmacist. At the end of the interventions the person has seen vast improvements in blood pressure, is less prone to falls and has seen an improvement in their overall health, including their continence.
With community pharmacists taking on an increasing role in supporting people with stable long term conditions through CMS, GP practice-based pharmacists' focus will clearly be on people with more complex needs who may benefit from a more comprehensive polypharmacy review. They can also ensure that any pharmaceutical care issues raised as part of CMS by community pharmacists are considered as part of an integrated pharmaceutical care pathway. This integrated way of working, as illustrated in Figure one, is supplemented with hospital pharmacists focusing on areas such as in-patient care, outpatient clinics and specialist services, some of which, like Teach and Treat clinics, may occur in primary care.
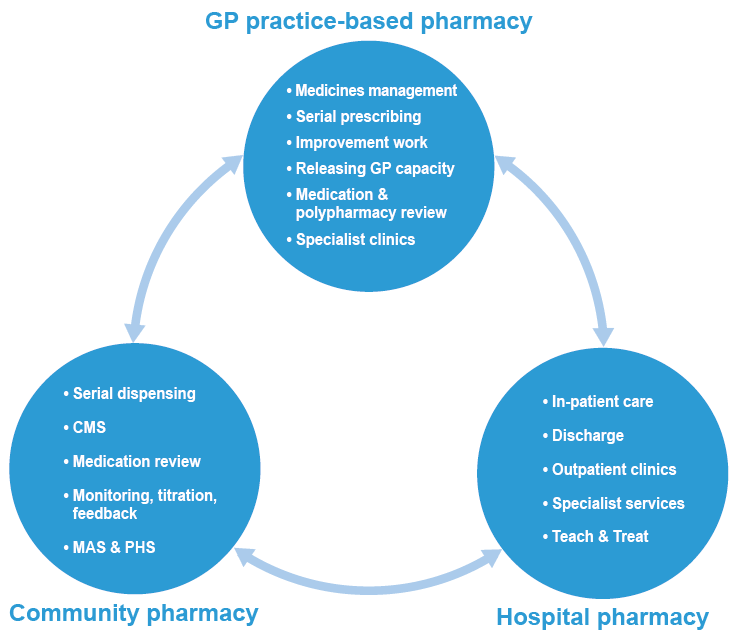
Figure one - Integrated pharmaceutical care
We are committed to ensuring that every GP practice has access to a pharmacist with advanced clinical skills by 2021 as outlined in the Health and Social Care Delivery Plan. It is important to recognise that there will not always be a uniform approach to the support for all GP practices. How they utilise pharmacists' and pharmacy technicians' skills will be dependent on the needs of the local population, the GP practice and the skills of the pharmacy team.
The aim is to match the GP practice needs and the pharmacy support more closely as we go forward, taking into account that some practices will want and be able to deliver more complex care and consultation arrangements around polypharmacy and long term conditions management. Some will do this by utilising the skills of pharmacists prescribers while others will focus more on medication management-related safe systems-based approaches which can be managed by a pharmacy technician.
It may also be that a GP practice and pharmacist start out with routine interventions which develop over time to deliver more complex pharmaceutical care. Some of the approaches being tested include sessional input from local community pharmacists who can follow-up aspects of pharmaceutical care with people in the community pharmacy.
Community pharmacy sessional input
A community pharmacist working three days a week in a pharmacy and the other two days with three local GP practices is seen as a key member of the multidisciplinary healthcare team as well as being more clinically involved in providing care. This sessional role has also benefited the other local community pharmacies who receive peer feedback which helps them understand what is important to the local GPs and why certain activities are being done, ensuring everyone is working together for a common goal.
'As a result of my work in GP practices, I enjoy my time in the community pharmacy even more. I am very focused on the pharmaceutical care of my patients and feel more confident in my clinical knowledge and carrying out polypharmacy reviews. Having worked with GP colleagues and as part of the multi disciplinary team, I find that I am making more significant interventions, I am comfortable in suggesting that people actually stop taking certain medication and I can resolve issues more easily. Feedback from the practices I work with is they find it really useful that I'm still community pharmacy based as I can advise them on things like stock supply issues and community pharmacy services such as the Minor Ailment Service and they can refer any hard-to-reach people to me as I'm much more likely to see them when they are picking up their prescriptions in the pharmacy.'
Community pharmacist
NHS Greater Glasgow & Clyde
We will use the evaluation from the pharmacists in GP practice pilots to carry out an options appraisal to help us understand in more details the impact of each of the models on service delivery, roles and responsibilities and outcomes and impact. We are keen to ensure pharmacists working across all settings, including community pharmacy, are drawn into this work in order build and maintain capacity and to make the best use of all pharmacists with advanced clinical skills.
Action:
We will deliver the commitment to ensure every GP practice in Scotland has access to a pharmacist with advanced clinical skills.
"There is an important role for GP practice-based pharmacists, at the interfaces of the profession, working closely with hospital pharmacists, community pharmacists and care homes to ensure seamless care and reduce potential medication related problems and errors."
Hospital pharmacy
Commitment 3:
Actions
Transformation requirements
Discharge process
Quality improvement & performance measures
Modern Outpatient Programme
Creating the conditions to transform hospital pharmacy services to deliver world leading pharmaceutical care.
The hospital pharmacy team plays an invaluable role in delivering clinical services, working closely with doctors, nursing staff and others to ensure the appropriate medicines are prescribed and dispensed and that clinical outcomes are monitored to ensure best use and to avoid harm and unwarranted variation. They also have an important contribution in supporting the Realistic Medicine agenda working in collaboration with their clinical teams at multiple points in the healthcare system including pre-admission, admission, prescribing, monitoring and discharge. This is with a particular focus on where there is evidence of admissions due to adverse reactions to medicines, or people who require more pharmacist input such as the frail elderly and those with multiple and complex conditions, in order to address any concerns about inappropriate polypharmacy.
Seven-day services
Most hospital pharmacy departments already deliver a seven-day medicine supply service. However, currently there are gaps in terms of the availability of clinical pharmacy services across weekends. Addressing this in an equitable way and matching demand to flow will require consideration and action on a number of factors. In particular it can be argued that even during weekdays the pharmacy resource has to be targeted through a triage model focusing on high risk and complex cases in response to the available pharmacy workforce.
Traditionally the pharmacy workforce tends to target people at admission and discharge; however, as part of this commitment to promote excellence in hospital pharmacy practice we will develop a plan to support the delivery of safe, effective and productive working across seven days. This needs to take into account how the whole hospital pharmacy team adapt their working patterns and prioritise direct frontline care. It also needs to take account of the challenges presented through urgent unscheduled care, as well as scheduled care. This requires thoughtful consideration to exactly what clinical activities need to be prioritised on both weekdays and at weekends and what role remote consultations and mobile working could play in ensuring adequate pharmacy coverage. It will also need to link to wider hospital pharmacy plans to deliver seven-day services with other teams such as Allied Health Professions ( AHPs) and laboratory services. This will require closer planning, integration and co-ordination of pharmacy services across all care settings at national, regional and local level, to ensure the best use of the available skill mix, expertise and digital tools.
Balancing flow and demand of people through the system against a finite hospital pharmacy workforce is challenging. Going forward it will be important to gain a better understanding of the appropriate skill mix of pharmacists and pharmacy technicians required. Ideally we want a combination of clinical pharmacist prescribers, and pharmacy technicians within clinical teams in a similar way to primary care, with roles underpinned by advanced practice frameworks for both pharmacists and pharmacy technicians. It is important to recognise the work of other pharmacy staff and to maximise the contribution of all grades of staff to the delivery of pharmaceutical care.
Part of the solution involves the effective application of digital solutions and Technology Enabled Care ( TEC) to support more productive ways of working through the implementation of Hospital Electronic Prescribing and Medicines Administration ( HEPMA) and the use of automation. These can enable pharmacy staff to be available on the ward assisting people to achieve the best outcomes from their medicines. In addition, improved clinical decision support tools and providing more remote Home and Mobile Health Monitoring [12] ( HMHM) and review will also deliver opportunities to improve self-management and provide step-down care in a person's own home or homely setting.
Action:
We will commission work to transform the delivery of hospital pharmaceutical services and pharmaceutical care during weekdays and at weekends.
Hospital discharge
Another key area for focus is ensuring a seamless transition for people not only on admission but also at discharge. There are well-documented challenges with regards delays at discharge. A number of solutions have been tested including: not providing discharge medication if people have sufficient medicine supplies at home; the use of NHS hospital prescriptions for those for whom discharge is simple and who are able to access a community pharmacy for their medication; the use of 'take home' pre-labeled packs of medication in the case of simple analgesics and antibiotics; and the use of people's own medicines on the ward. However, there are often other factors that can impact such as discharge sign-off being tied to a consultant ward round. It is also important to acknowledge the workload challenges and multiplicity of priorities for Foundation Year Doctors who have a critical role in the discharge process. There is a need to work with them to identify and deliver solutions. HEPMA brings advantages in that it allows all of a person's medication to be pre-populated into the electronic discharge letter thereby improving the discharge process. A further improvement to explore is whether providing people with an electronic copy of the discharge letter could improve the discharge process and timelines.
In addition, hospital discharge can be a difficult time to support people with adherence to new medication regimens. There is a role for pharmacists and pharmacy technicians in supporting this transition by taking on a greater part in managing care prior to and during discharge and with empowerment and authority to intervene to change prescriptions if necessary. There is also a need to consider the pharmaceutical input to be delivered by different sectors of the pharmacy profession depending on the care pathway and the complexity of the intervention. For example, there are opportunities to explore the role of community pharmacy in supplying both discharge medicines and outpatient medicines such as biologics and oral chemotherapy where it is considered safe and appropriate and the use of telecare devices to support adherence.
Action:
We will commission work to explore ways to improve all pharmacy-related aspects of the hospital discharge process utilising integrated models of pharmaceutical care.
Modern Outpatient Programme
The Modern Outpatient Programme is seeking to transform peoples' experiences by optimising the roles of all clinicians, utilising new technologies and putting the person at the centre of their care. It is being progressed over a three-year time period, building on the direction set within the Primary Care Transformation Programme and the National Clinical Strategy.
Hospital pharmacy teams are already considering opportunities to redesign their services with a clear focus on emerging clinical roles within acute services. These include better targeting of unscheduled acute high risk groups, better use of pharmacist independent prescribers in specialist clinics both in secondary and primary care and wider access to specialist support with the wider expansion of Teach and Treat clinics in primary care. These developments will need to be underpinned by improved information sharing and referral pathways.
Teach and Treat clinics
The first Pharmacy Teach and Treat service started in NHS GCC in 2014. It aimed at optimising people's treatment following a heart attack, utilising the skills of pharmacist independent prescribers ( IP). It is widely recognised that best evidence based care for this patient group requires optimising doses of specific medicines. The medicines are initiated in hospital at low doses and should be increased, with supervision and monitoring, over time. Research findings however demonstrated that frequently the medications were not altered as recommended. A pharmacy team were asked if they could help address this locally. Working closely with the multidisciplinary team, the pharmacists instigated pharmacist-led clinics to follow up with people after discharge from hospital. The clinic sessions consist of a 15 minute face-to-face consultation in the out-patients department. The consultations include taking a clinical history, appropriate blood tests, blood pressure measurement and a physical examination including chest auscultation. Following assessment, the pharmacist IP optimises the medicines, issues a prescription and arranges a follow up.
Alongside this, A Plan for Scotland [13] sets out the Government's clear commitment to shifting the balance of care in order to ensure that people get the right support from the right professional as close to home as possible. This means a transformational shift in how healthcare will be funded and by 2020/2021 more of the NHS budget will be spent in the community setting rather than in hospitals. This will necessitate collaboration between primary and secondary care to develop solutions that best meet the needs of the local population and at the same time appropriately manage workload across the system, valuing the contribution of all staff.
Action:
We will work with the Modern Outpatient Programme to ensure a strategic alignment of the pharmaceutical contribution to its work.
Continuous improvement
Measurement is central to the concept of hospital quality improvement and provides a platform to identify opportunities for improving outcomes as well as enhancing service delivery and performance. Hospital pharmacy services are an integral part of clinical service provision as well as driving productivity and efficiency improvements. Ensuring sufficient pharmacy capacity is key to delivering the optimal use of medicines and reducing unwarranted variation, wastage and harm. The use of a combination of improvement tools and performance and outcome measures has the potential to achieve a transformation in how hospital pharmacy services are provided as well as drive improved user experience and performance efficiencies across a range of areas from procurement to clinical service provision.
Action:
We will commission the development of a series of quality improvement tools and performance measures to support the transformation of hospital pharmacy services across Scotland.
Delivering safe use of medicines
Commitment 4:
Actions
Data measurement & monitoring
Medicines reconcilation
Pharmacy role awareness
Quality improvement in community pharmacy
Providing the focus, resources and tools to support the safer use of medicines.
Medicines remain the most common therapeutic intervention available to clinicians; however, the burden of harm relating to medicines is well reported. While every prescribing decision has the potential for a positive outcome or benefit, this must be balanced against the risk of causing harm.
The call-to-action in Realistic Medicine aims to add value and limit the harm caused by medicines by reducing: unwarranted variation and waste; over-investigation; over-diagnosis; and over-treatment. It encourages clinicians to lead with the least invasive processes first, to manage risk proportionately and to understand the limits of evidence. A key area of focus includes working in active partnership with people to build a personalised approach to their care.
Realistic Medicine challenges healthcare professionals to adopt an approach to medicines in order to reduce harm that can be associated with medical care, ensure that treatments are tailored to people's preferences and deliver care that is of great value to people. To be effective, we also need to support people to understand their part in an effective healthcare partnership and enable them to express their preferences. These critical themes resonate strongly with the pharmacy profession. The follow-on report, Realising Realistic Medicine, includes a clear endorsement from the profession which signals their commitment to embed this in our practice.
National programmes
To support local NHS Board governance responsibilities, a number of Scotland-wide programmes are active in driving improvements in the safer use of medicines. These include the Yellow Card Centre Scotland, the Area Drug and Therapeutics Committee Collaborative, the Adverse Events Programme, the Integrated Digital Safer Medicines Programme ( IDSMP)and the Scottish Patient Safety Programme ( SPSP).
Importantly we need to continue to input to the wider work of the SPSP to improve the safety and reliability of healthcare and reduce harm across the six core work programmes: acute adult, primary care, maternal and children, mental health, healthcare acquired infection and medicines. In particular we are keen to build on the pharmaceutical dimension of the SPSP: Medicine programme to draw out some of the opportunities to improve the transition of care by ensuring pharmacists working in community pharmacy, GP practices and hospital pharmacy are working collectively to ensure seamless pharmaceutical care as people transfer across different settings.
Medicines reconciliation
The medicines reconciliation work within SPSP has potential to improve safety but has struggled to become embedded in hospital practice. To date it has been person-dependent and would benefit from becoming more widely embedded in existing and emerging systems. HEPMA will help to achieve this but as the transfer between care settings often results in poor medicines reconciliation it would also be beneficial to consider this in both a UK and international context and learn from others about what 'good' looks like.
Action:
We will work with SPSP: Medicine to continue to strengthen arrangements for medicines reconciliation at the interfaces of care across Scotland and ensure national guidance and local delivery are aligned. This may involve developing new recommendations for future practice.
Measuring harm
Whole system thinking and measurement are critical parts to an integrated approach to assessment, assurance and improvement. In addition, to underpin our understanding of medicine safety, the measurement of past harm is a critical dimension. Data on harm at a local and national level is key to informing the priorities for improvement as well as supporting shared learning.
Measuring and monitoring medicine safety
Multidisciplinary teams in NHS Forth Valley and Tayside are testing the application of the Health Foundation measuring and monitoring framework. This is to inform a more holistic understanding of medicines safety from the absence of harm to the presence of safety. Teams consider a number of dimensions including past harm, reliability of care and safety in the future.
Action:
We will commission Healthcare Improvement Scotland ( HIS) to work with National Services Scotland ( NSS) and NHS Boards to strengthen the available data on harm and establish measuring and monitoring parameters for medicines safety more broadly to consider past, present and predictable future harm.
Community pharmacy
Recent developments have included introducing continuous improvement as an on-going element of the community pharmacy funding arrangements with the aim of applying improvement methodology into day-to-day practice. This has included the national roll-out of the patient safety climate survey across community pharmacy. The work has been supported by Quality Improvement in Pharmacy Practice Collaborative ( QIPP) consisting of the Royal Pharmaceutical Society ( RPS), Community Pharmacy Scotland ( CPS), NHS Education for Scotland ( NES), Health Improvement Scotland ( HIS), The Health and Social Care Alliance Scotland (The ALLIANCE), Yellow Card Centre Scotland and NHS Boards. QIPP has provided a series of Quality Roadshows designed to raise awareness of and commitment to quality improvement across Scotland. The learning from the SPSP community pharmacy collaborative will be considered for wider translation and dissemination where appropriate.
Scottish Patient Safety Programme: community pharmacy collaborative
Community pharmacy teams in NHS Fife, Grampian, Highland and Greater Glasgow and Clyde ( GG&C) have been testing a series of tools and resources to help people taking a range of high risk medicines to use them safely. Work has also been taken forward examining the safety culture within community pharmacies through the early adoption of the Patient Safety Climate Survey. Current pilots between community and hospital pharmacists in NHS Forth Valley, GG&C and Grampian are demonstrating how providing shared access to clinical data can strengthen the effective contribution of pharmacy in delivering safe clinical care and supporting medicines reconciliation. This programme was funded by the Health Foundation and has been evaluated by the Strathclyde Institute for Pharmacy and Biomedical Sciences.
Action:
We will make quality improvement an integral element of community pharmacy funding arrangements in a similar way to GPs and introduce a programme of continuous improvement.
Involving people and supporting meaningful participation
A baseline survey of people's perceptions of pharmacy services and their use of medicines [14] , conducted in association with the Scottish Health Council's Our Voice Citizen's Panel, tells us that people tend to default to going to their GP for advice about medicines and are not fully aware of the expertise and services offered by their local community pharmacy. For example, only 23% people were aware that they could have their medicines reviewed by a pharmacist. We need to improve awareness of what support pharmacists can provide and encourage people to go to their local community pharmacy in the first instance where appropriate.
Work is already underway to provide information to the public and people receiving care about medicines taking into account health literacy needs. HIS has produced a factsheet, 'Medicines in Scotland: what's the right treatment for you?', which explains how healthcare professionals make prescribing decisions, how to find out more about medicines and what to do if side effects are experienced. But there is more work to be done to ensure we deliver person-centred pharmaceutical care. This includes considering how to make better use of tools and interventions to assist people in using their medicines effectively.
Action:
We will commission work to raise awareness of the role of pharmacists and pharmacy services. We will work with others to facilitate the co-production of tools and interventions that can be used to help support shared decision making around the use of medicines.
"Quality improvement encompasses activities which ensure we provide person-centred, safe and effective care which meets people's needs and expectations."
Care homes and care at home
Commitment 5:
Action
Improvement approaches
Care homes
Concerns about the variation in the quality of pharmaceutical care in some care homes have been well documented and were highlighted in the Wilson and Barber Review of NHS Pharmaceutical Care in the Community [15] in Scotland. This report identified the need for high quality pharmaceutical care to meet the medication needs of the whole cohort of care home residents, many of whom have increasing dependency and multimorbidity. There is an opportunity to build on the role that community pharmacists already fulfil in terms of the supply of medicines and related advice and support for people in care homes.
More recently there have also been new models emerging with community pharmacists, GP practice-based pharmacists and pharmacy technicians providing more tailored pharmaceutical care in care homes. Opportunities exist to determine national standards for documentation and recording systems which can support integrated information exchange, including medicines reconciliation at admission, transfer and discharge for residents. Additional benefits include the introduction of national standards for the safe administration of medicines, the development and delivery of quality assured training for care home staff and regular multidisciplinary reviews of medication.
Providing pharmaceutical care to care homes
A prescribing support pharmacist working across two GP practices in north-east Glasgow carries out annual medication reviews for elderly residents in local care homes to reduce polypharmacy and rationalise medicines, including reducing the use of high risk medicines where appropriate. This involves working closely with the care home liaison nurses to improve compliance with wound formulary and attending care home meetings with GPs to review a person's pharmaceutical care needs.
Care at home
Many of the principles which relate to pharmaceutical care in care homes are also applicable to services for people who require supported care at home. That said, the situation can be even more complex with a wide variety of formal and/or informal carers of varying capabilities and with the growing implications of self-management and self-directed support. Again opportunities arise to standardise aspects of the support provided including documentation and training, supported by digital tools for secure mobile working.
With this group, there is also a particular need to focus on reablement and the active involvement of family and carers. This includes better use of person-generated data and information, the use of tools to help identify those at greatest risk requiring more intensive support and harnessing advances in technology-enabled care including remote monitoring systems, telecare devices, video consulting and apps.
There may also be benefits in implementing a single shared assessment which addresses the use of multi-compartment compliance aids only where they are identified as appropriate for an individual's needs. More extensive and specialised care needs to be provided to some individuals or groups of people involving healthcare professionals who may have traditionally been more hospital-based, and with whom there has to be effective communication and exchange of information.
Action:
We will work with Chief Officers of Integrated Joint Boards to identify national approaches to improve NHS pharmaceutical care for residents in care homes and people being cared for in their own homes.
"We need to ensure high quality pharmaceutical care is delivered to people in care homes and in their own homes, many of whom have increasing dependency and multiple conditions."
Remote and rural communities
Commitment 6:
Actions
Recruitment & retention
Availability of technology to support R&R
Digitally enabled infrastructure
Rural Scotland accounts for 98% of the land mass and nearly 20% of our population live there. Rural populations continue to grow at a faster rate than the rest of Scotland and also have higher levels of older people, which increases demand for core services. This, in turn, makes the co-ordination and delivery of health and social care in remote and rural areas more challenging. A number of innovative ways of delivering healthcare in rural areas are being developed and tested, including solutions such as technology enabled care and urban and rural hospital networks.
NHS Highland technology enabled project
A team from NHS Highland has been awarded funding from the Health Foundation to test an innovative technology enabled project designed to help improve people's access to pharmaceutical care in remote and rural areas across the region. The project involves pharmacists providing medication reviews and advice on taking medicines to people registered with dispensing medical practices. The pharmacists work closely with the dispensing practices but are located remotely from them. People are able to speak to the pharmacist from their own home, workplace or medical practice via a secure video link. A face-to-face version of this service, in which a pharmacist visits dispensing practices, has already been developed by NHS Highland in a pilot involving four practices.
Consideration needs to be given to how to scale up these technology enabled care initiatives so that they become mainstream practice in order to improve access to pharmaceutical care, deliver better health outcomes for people and help sustain services in remote and rural communities, including dispensing doctor practices. This also requires ensuring the digital literacy of the pharmacy workforce as well as the people they are caring for so that they are confident and competent to use technology in their daily practice.
Action:
We will work with the TEC Programme and NHS 24 to ensure the availability of technology enabled care solutions to support remote and rural communities.
Recruitment and retention
There can be difficulties in attracting pharmacists and pharmacy technicians to work in more remote and rural areas communities. The barriers are similar to those identified for other healthcare professionals. We are committed to improving both the recruitment and retention of staff in these areas. Improving the exposure of pharmacy undergraduate students to remote and rural working is one such way of achieving this and there are examples of innovative solutions being tested in other professions such as medicine.
Education and training
Education has a key role to play in supporting service improvement and developing new or expanded ways of working across the whole workforce and more specifically in remote and rural communities. Providing education and training that is local, flexible and affordable is a key component to ensuring the appropriate mix of skills, competency and ability across the pharmacy workforce in remote and rural communities. NES Pharmacy recently commissioned the School of Medicine at the University of Dundee and the School of Pharmacy and Life Sciences at Robert Gordon University ( RGU) to provide a three-day clinical skills training course in Shetland for pharmacist practising in Orkney, Shetland and the Western Isles. This has allowed a tailored education and training programme to be provided locally.
Action:
We will commission NES to work with remote and rural NHS Boards to explore mechanisms to attract more pharmacists and pharmacy technicians to work in remote and rural communities and ensure any associated education and training needs are flexibly met. We will test a pharmacy longitudinal clerkship.
Contact
Email: David Jamieson, david.jamieson@gov.scot
Phone: 0300 244 4000 – Central Enquiry Unit
The Scottish Government
St Andrew's House
Regent Road
Edinburgh
EH1 3DG