Achieving excellence in pharmaceutical care: a strategy for Scotland
Strategy aiming to transform the role of pharmacy across all areas of pharmacy practice, increase capacity, and offer the best person-centred care.
2. Executive Summary
As Chief Pharmaceutical Officer for Scotland, my focus is on achieving excellence in NHS pharmaceutical care provision to ensure safe, effective and person-centred pharmaceutical care and safer use of medicines are core components of health and social care services in all care settings. Achieving Excellence in Pharmaceutical Care sets out my vision of how pharmaceutical care will evolve in Scotland and the crucial contribution of pharmacists and pharmacy technicians, working together with other health and social care practitioners, to improve the health of the population and impact on health outcomes, especially for those with multiple long term and complex conditions.
Since the publication of Prescription for Excellence in 2013, much has changed in the Scottish Government's strategic approach to planning for, and delivering of, healthcare services. This strategy aligns what we are doing in pharmacy and the direction of policy now set out in the Health and Social Care Delivery Plan, the National Clinical Strategy, Pulling Together, the Modern Outpatient Collaborative, Realistic Medicine, the Mental Health Strategy, and the six essential actions to improve unscheduled care. Taken together these provide a clear vision for our NHS in Scotland.
Community Pharmacy
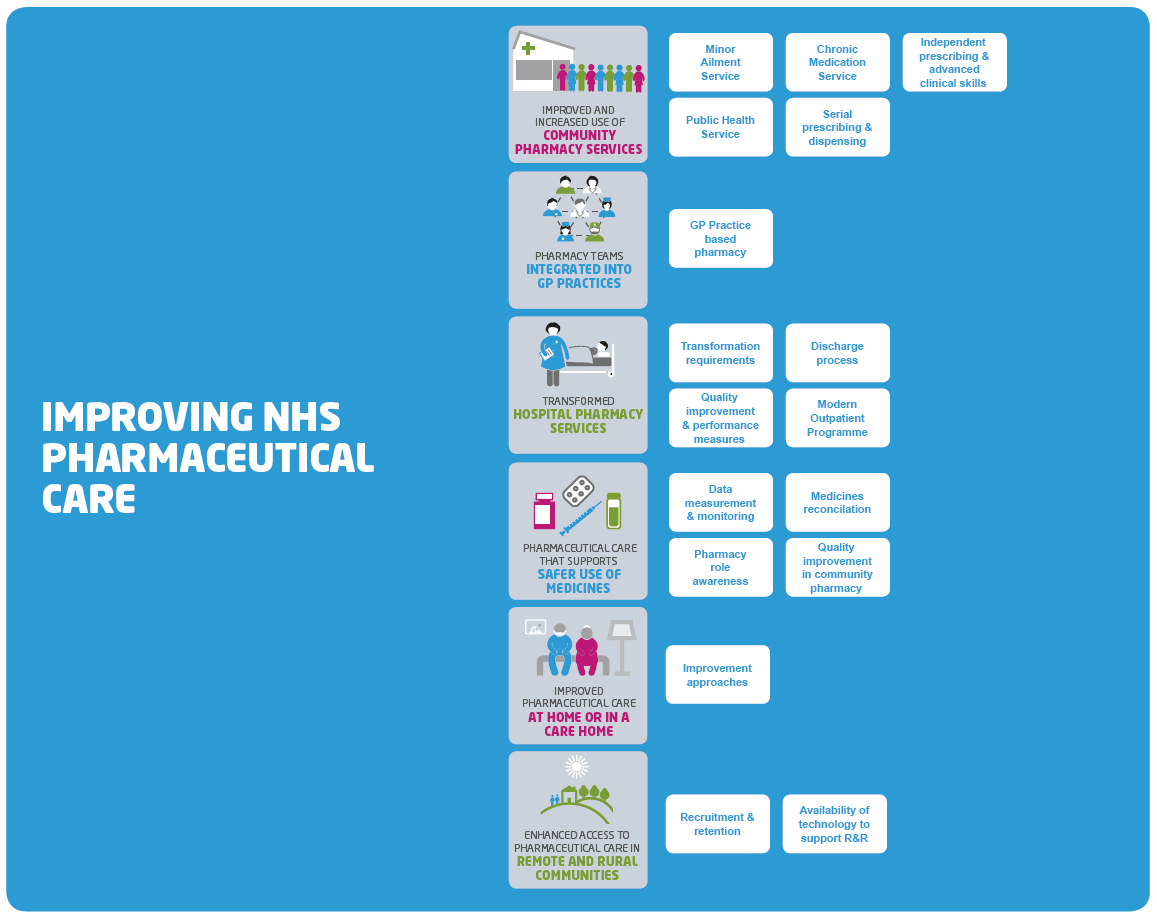
Community pharmacy already plays an important role in the provision of NHS pharmaceutical care, providing highly accessible services for people both in-hours and out-of-hours. We want more people to use their community pharmacy as a first port of call. Central to this is to ensure that services such as the Minor Ailment Service ( MAS), the Chronic Medication Service ( CMS) and Public Health Service ( PHS), core elements of the NHS services provided in community pharmacies, are being delivered to their full potential. It is through making full use of the clinical capacity in community pharmacy that real gains in clinical care can be made. It is also where the community pharmacist's contribution to multidisciplinary team working takes its place to open up access to primary care for everyone and reduce workload at GP practices and other local healthcare services.
GP Practice-Based Pharmacy
The last two years have seen significant Government investment in the introduction of GP practice-based pharmacists with advanced clinical skills. These pharmacists and, more recently, pharmacy technicians are working alongside GPs and other health and social care professionals. They are helping to build multidisciplinary team working and improve medication management through, for example, providing polypharmacy reviews and specialist clinics in order to get the best possible outcomes from prescribed medication - including prescribing, monitoring and adjusting treatment where appropriate.
Hospital Pharmacy
There is recognition that hospital pharmacy services need to respond to the changing environment in their service. This is particularly so with an increasingly frail elderly population, a drive to decrease the length of stay, improve flow, the move towards seven day services, and new developments to modernise outpatient services.
Safer Use of Medicines
Medicines remain the most common therapeutic intervention available to clinicians; however, the burden of harm relating to medicines is well reported. The Chief Medical Officer's vision of Realistic Medicine challenges healthcare professionals to adopt an approach to medicines to reduce harm that can be associated with medical care and ensure that treatments are tailored to people's preferences and deliver care that is of great value to people. To be effective, people need to be supported to understand their part in an effective healthcare partnership, to be informed and to be able to express preferences. We are committed to embedding these themes into pharmacy practice.
Care Home and Care at Home
Concerns about the variation in the quality of pharmaceutical care in some care homes have been well documented highlighting a need for high quality pharmaceutical care for this particularly vulnerable group of people whether they are adults or children in residential care. Many of the principles of pharmaceutical care in care homes also apply to services for people who require supported care at home, where the situation can be even more complex.
Remote and Rural Communities
Nearly 20% of our population live in rural Scotland. Remote and rural communities are growing at a faster rate than the rest of Scotland, and have higher levels of older people. Consideration needs to be given to how we introduce technology enabled care initiatives into mainstream practice. We want to overcome barriers to attracting, educating, and training pharmacists and pharmacy technicians to work in remote and rural communities in order to improve access to pharmaceutical care, deliver better health outcomes for people and help sustain service in remote and rural communities, including dispensing doctor practices.
Enabling NHS Pharmaceutical Care Transformation
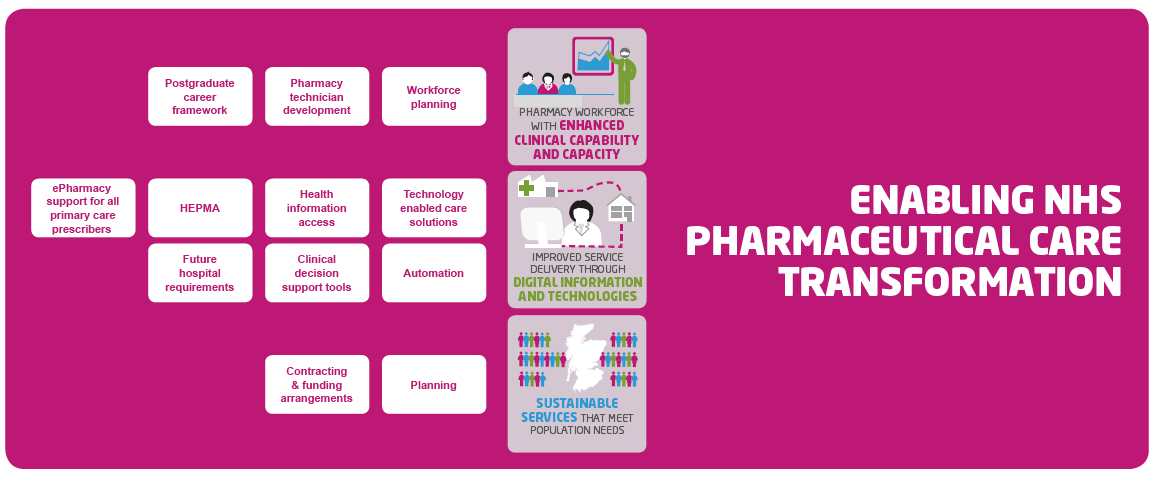
While playing to the strengths of the pharmacy team is crucial to achieving excellence, they must also have the resilience to be able to respond and adapt to the needs and pressures facing our modern health and social care system. We have identified three key enablers as priorities for action: developing the pharmacy workforce; improving access to and use of digital information and technologies; and planning for sustainable, flexible and resilient approaches to delivery of NHS pharmaceutical care across Scotland.
Pharmacy workforce
As the balance of care shifts and pharmacists take on expanded clinical roles, it is important people are confident that they are receiving the best NHS pharmaceutical care which meets their needs and wishes. With the demand for pharmaceutical care set to increase we want to strengthen our pharmacy workforce planning. This includes ensuring pharmacists and pharmacy technicians have the necessary clinical, decision-making and digital skills needed to care for people effectively.
Digitally enabled infrastructure
Going forward, technology and data will have a crucial role in improving pharmaceutical care, underpinning our safety culture, ensuring efficiency of services, unlocking capacity within pharmacy teams and facilitating improved sharing of information between health and social care settings. We are committed to this transformative programme of work which includes automated technologies, technology enabled approaches to support people to better manage their medication and the implementation of Hospital Electronic Prescribing and Medicines Administration ( HEPMA) in every NHS Board across Scotland. These developments will improve patient safety and release capacity not only in pharmacy but across a range of healthcare professional groups.
Sustainable pharmaceutical care services
Importantly, the Scottish Government will develop, consult on, and provide NHS Boards and their Health and Social Care Partnership ( HSCP) partners with the tools and legislative underpinning for a new approach to pharmaceutical care service planning and contracting. This will mark a departure from the current arrangements which are largely governed by terms and conditions in regulation, the fitness for purpose of which is nearing its limits.
Conclusion
The nine commitment areas and programme of supporting actions will help to not just put in place the key foundations for Achieving Excellence in Pharmaceutical Care, but will create the conditions for the future responsiveness of NHS pharmaceutical care services and the tools to help deliver this.
Achieving Excellence In Pharmaceutical Care - Summary
Contact
Email: David Jamieson, david.jamieson@gov.scot
Phone: 0300 244 4000 – Central Enquiry Unit
The Scottish Government
St Andrew's House
Regent Road
Edinburgh
EH1 3DG