Advanced nursing practice - transforming nursing roles: phase two
Follow-up paper to the Transforming Roles paper on Advanced Nursing Practice (ANP) published in December 2017.
Annex B
ANP Supervision: Example from the West of Scotland Advanced Practice Academy
The West of Scotland Advanced Practice Academy supervisiondocument outlines practice supervision for trainee ANPs, robust arrangements for 'final sign-off' at the completion of training and more detail on Clinical Supervision for ANPs. The document below is an example of the ways in which an Academy may strengthen the governance and practice of ANPs across Health Boards.
ANP Clinical Supervision
Definition of clinical supervision
"Clinical Supervision is regular, protected time for facilitated, in-depth reflection on complex issues influencing clinical practice" Bond and Holland (1998, p15)
NMC and Revalidation
The NMC describe the benefits of clinical supervision as "improved capacity to identify solutions to problems, increased understanding of professional issues, improved standards of patient care, opportunities to further develop skills and knowledge and enhanced understanding of own practice" (NMC 2008). The principles of clinical supervision are closely linked to the NMC's revalidation process.
Models of Supervision
A number of different models of clinical supervision exist. These are conceptual frameworks that can guide practitioners and supervisors through the clinical supervision process. Proctor's three-function model (Proctor 1987) is one of the most widely used; however, other models can be used.
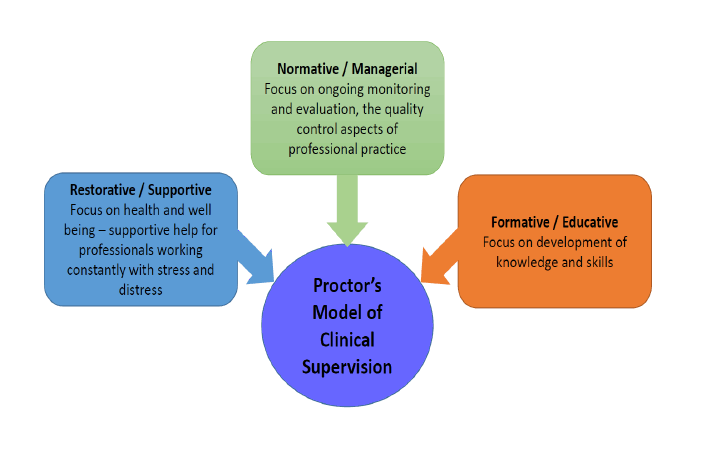
Proctor's Model
Proctor's model describes three functions that need to be addressed in supervision. Namely:
- Normative/managerial
- Formative/educative
- Restorative/supportive
The focus can be on one or more of these functions and will vary according to the needs and values of the supervisee. The different functions may also overlap.
Trainee to experienced ANP
Trainee ANPs will require closer and more intense supervision than experienced ANPs.
Clinical Supervision for Trainees
Trainee ANPs require supervision throughout their entire ANP education. A 'tripartite' approach is encouraged. This will involve:
- A Clinical Supervisor/trainer who will be an experienced senior clinician who is doing or is able to do the same job the trainee ANP is preparing for. This individual could be a suitably qualified and experienced ANP or they may be another suitably qualified and experienced healthcare professional, most often a consultant, General Practitioner or registrar.
- An Educational Supervisor who will be a suitably qualified and experienced educationalist (e.g. personal academic tutor). This could be the Programme Leader for the course the trainee is undertaking, or another member of the programme team the responsibility is delegated to
- The trainee's line manager who will be responsible for ensuring that the trainee is supported and appropriately clinically supervised throughout their entire training.
At least one of the Supervisors should be a senior registered nurse and ideally an Advanced Nurse Practitioner.
On occasion one individual may be able to undertake more than one of these roles. However, best practice would be to involve three separate people with distinct responsibilities.
Responsibilities of supervisors
- The Clinical Supervisor/Trainer will be responsible for ensuring that the trainee is appropriately clinically supervised throughout their training. This may involve one-to-one supervision, especially near the beginning of the training, or may involve ensuring that a team of suitably qualified and experienced people are available to provide supervision if the Clinical Supervisor/Trainer is not present. The Clinical Supervisor/Trainer should meet with the trainee on a regular basis to discuss progress. As a minimum, this would be on a 6-8 weekly basis. The Clinical Supervisor/Trainer will liaise with the line manager at regular intervals.
- The Educational Supervisor will be responsible for ensuring that the trainee can access the modules on the programme, will provide academic advice and support to the trainee and will liaise with the Line Manager.
- The Line Manager will be responsible for ensuring that the Supervision model is working, that the trainee is getting the personal, academic and clinical support that they need. The Line Manager is also responsible for ensuring that the trainee has appropriate time for learning built into their job plan and that they can access all appropriate learning opportunities
The three supervisors should communicate with each other on a regular basis and it would be good practice for all three to meet together with the trainee at least once a year.
The three supervisors should have open lines of communication to share progress and discuss issues.
- The trainee also has responsibilities. The trainee should liaise with the line manager on a regular basis regarding progress and should raise any issues that might impact on training and development at an early stage.
- The trainee should also share relevant information with their clinical supervisor and education supervisor as appropriate.
- The trainee is an adult learner as is expected to identify their own learning needs, assisted by the clinical and education supervisors and line manager.
Designated Prescribing Practitioner (DPP)
Prescribing students can be supervised and assessed by any registered healthcare professional who is an experienced prescriber with suitable equivalent qualifications for the programme the student is undertaking.
NMC registrants who are undertaking V300 require a practice assessor and a named practice supervisor, which are two separate roles. Further information on becoming a prescriber can be found on the NMC website via the following link:
Becoming a prescriber - The Nursing and Midwifery Council (nmc.org.uk)
The link to the Royal Pharmaceutical Society (RPS) document 'Designated Prescribing Practitioner Competency Framework' can be found here:
Of note the NMC medicines standards have been withdrawn since January 2019 and the RPS standards have been recommended. More information can be found via the following link to 'Professional guidance on the safe and secure handling of medicines' on the RPS website:
Professional guidance on the safe and secure handling of medicines (rpharms.com)
Dissertation Supervisor
If the trainee goes onto complete the Masters programme, then they will require a Dissertation Supervisor. This Supervisor will be appointed by the Higher Education Institution.
Requirements of supervisors
The following are minimum requirements. Different Higher Education Institutions and/or additional awarding bodies (e.g. Royal College of Emergency Medicine (RCEM), The Faculty of Intensive Care Medicine (FICM), RCN) may have additional requirements.
- Clinical Supervisor/Trainer – must be a senior clinician who is technically skilled to undertake the role the trainee is preparing for. They must be registered by their Registering Body (NMC, General Medical Council (GMC), The Health and Care Professions Council (HCPC)) and not have any limitations on their practice. They also must be able to prescribe. Ideally, they should hold a masters level qualification.
- Educational Supervisor – must be part of the Programme Team at the Higher Education Institution the trainee is undertaking the qualification at. They must either be employed by the Institution or hold an Honorary Contract with that institution. Educational Supervisors must have access to the academic transcripts of the trainees they are supervising. They must hold a masters level qualification or above and ideally be an Advanced Practitioner
- Line Manager – must be willing to take on the responsibility to support the supervision of the trainee and to facilitate the training within the workplace
Collecting Evidence
Part of the role of the supervisors is to help the trainee build a portfolio of evidence to demonstrate their competence in Advanced Practice.
Professional Portfolio
All trainee ANPs and ANPs are expected to use the NES TURAS Professional Portfolio, details of which can be found via the following link: https://turasnmportfolio.nes.nhs.scot
Within the Professional Portfolio trainees need to demonstrate the following (as a minimum):
- Record of their learning including clinical experience as a trainee
- Completion of all academic requirements (record of all modules undertake, including results and copy of their final exit award certificate)
- Work Based Practical Assessments (formative and summative). This is likely to include:
- Mini-Clinical Evaluation Exercise (CEX)
- Direct Observation of Practical Skills (DOPS)
- Case Based Discussions
- Feedback from others
- Competencies – where appropriate competencies may be mapped to evidence elsewhere in the portfolio
- Supervision reports
Different Higher Education Institutions and/or additional awarding bodies (e.g. RCEM, FICM, RCN) may have additional requirements and may require other Portfolios to be used for different stages. Evidence can be shared between portfolios.
Competencies
The ANP role continues to evolve and new frameworks are being developed on a regular basis. As a minimum ANPs in Scotland must meet all the 'high level' competencies for an ANP, all the Prescribing competencies and the competencies for one of the broad groups of ANPs (e.g. neonatal, paediatric, primary care/community, adult acute care, or mental health).
Additional competencies may be required by different Higher Education Institutions and/or additional awarding bodies (e.g. RCEM, FICM) and/or the employer.
The supervision team will help the trainee identify all the required competencies for their role.
Final Sign-off
Completing a course of academic study is not sufficient to demonstrate that an individual is competent to practice as an ANP.
Each employer needs to ensure an appropriate mechanism is in place for 'final sign-off'. Final sign-off is required when an individual:
- Completes initial training
- Changes job especially if it's in a new speciality
Final Sign-off involves:
- The individual's line manager who will take the lead on the sign-off process
- The Clinical Supervisor/Trainer
- The Education Institution – this would usually be through evidence of completion of a programme of education (for example a copy of the Postgraduate Diploma in Advanced Practice and/or academic transcript)
The Line manager would set a date for the trainee ANP to submit a 'Share Pack' of their portfolio. The line manager would share this with the Clinical Supervisor/Trainer. Both would be expected to review the portfolio and confirm it is completed to a satisfactory standard. As a minimum, the following is expected.
- Record of their learning including clinical experience as a trainee.
- A minimum of 400 hours of supervised practice[7] over a minimum of 1 year
- Evidence of learning:
- Clinical assessment
- Clinical reasoning, judgement and diagnostic decision making
- Anatomy and physiology
- Non-medical prescribing
- Leading, delivering and evaluating care
- Worked based learning
- Completion of all academic requirements (record of all modules undertake, including results and copy of their final exit award certificate) and recorded as a non-medical prescriber with the Nursing and Midwifery Council.
- Copy of a masters level qualification in advanced practice (or evidence of equivalence [this would normally be 120 credits with a minimum of 50% at masters level).
- Evidence of being recorded with the NMC as a Nurse Independent Prescriber
- Evidence of being recorded with Health Board as a prescriber
- A range of Work Based Practical Assessments demonstrating competence is managing the broad range of patients seen within the role. This is likely to include:
- Mini-CEX
- DOPS
- Case Based Discussions
- Feedback from others
- Completed competencies – where appropriate competencies may be mapped to evidence elsewhere in the portfolio
- Satisfactory Supervision reports which confirm the trainee has completed training and has been assessed as competent performing as an ANP
The Clinical Supervisor/Trainer and Line Manager will together determine whether the trainee has:
- Passed - Satisfactorily passed all academic requirements and evidence of competence to practice in ANP role contained within TURAS Professional Portfolio
- Provisional pass – satisfactorily passed all academic requirements, but some minor gaps in evidence of competence.
- Fail – either has still to pass all academic requirements or has major gaps in evidence of competence or both.
If the trainee has passed, the line manager would inform the individual within the Board who is responsible for recording ANPs on the Scottish Standard Workforce Information System (SWISS). The trainee, employed as Band 7 Annex 21 or Band 6, would be expected to move to a Band 7 at this stage.
If a provisional pass, the line manager would set a period of time (no less than 1 month and usually no more than 6 months) for the individual to obtain the required evidence. Trainees employed as Band 7 Annex 21 or band 6 would not normally move until competence has been achieved. The trainee would not normally move to a Band 7 until after confirmation that satisfactory evidence has been submitted.
If a fail, the line manager, in consultation with others (which may include the clinical supervisor, education supervisor and Human Resources) the most appropriate course of action for the individual. This may include re-doing part of the training or termination of the traineeship.
If the Clinical Supervisor/Trainer and Line Manager cannot agree on a grade, the view of the internal moderator should be sought. If agreement can still not be reached then advice can be sought through the external quality assurance mechanism system i.e. the Academy.
Moderation
A sample of portfolios will be internally moderated and externally quality assured each year. Each Board will put in place a mechanism for internal moderation.
The Advanced Practice Academy will put in place a mechanism for external quality assurance of a sample of portfolios from each board every year. This mechanism will involve a suitable expert(s) from another Board reviewing Professional Portfolios and providing feedback to the line manager, the Board Advanced Practice Lead and the Board Nurse Director.
External Experts will be recorded within their employing Board as an ANP or NMAHP Consultant and either have teaching and assessing qualification or be recognised by the Academy as an 'External Expert'.
The Academy's recommendations will be advisory only. Ultimately, it will be for the employer to determine whether an individual has met all the requirements to practice.
Clinical Supervision for Qualified ANPs
The Clinical Supervision model for qualified ANPs differs significantly from the practice supervision model used for trainee ANPs. The model that should be used for qualified ANPs is the NES Clinical Supervision model, details of which can be found via the link below.
See https://learn.nes.nhs.scot/3580/clinical-supervision
Qualified ANPs will have a network of support and supervision that will support day-to-day practice. This network may include the on-call medical consultant, senior medical staff, ANP colleagues, other Advanced Practitioners, the individual's line manager, lead and or chief nurse and consultant nurse.
In addition to this, each ANP will have a named Clinical Supervisor who will either meet with the supervisee on a one-to-one basis or in a group with other supervisees. Supervisees should meet with their Clinical Supervisor at least once a year.
The ANPs line manager will be responsible for ensuring that each qualified ANPs has a named Clinical Supervisor.
Clinical Supervision will consist of:
1. A reflective component
2. Support from a skilled facilitator
3. Focus on clinical practice (including team dynamics, communication and personal coping)
4. Professional Development
5. Improving patient treatment and care
Record Keeping
The Clinical Supervisor and Supervisee are jointly responsible for ensuring records are kept of supervision sessions. Records will help supervisees:
- revisit their discussions, reflections and action points over time
- provide evidence that they have participated in clinical supervision which can be used for revalidation
- document and commit to any agreement to take anything out of a session
Clinical Supervisor
The Clinical Supervisor for a trained ANP will be an experienced senior clinical who is doing or is able to do a similar job to the ANP. Ideally this individual should be a suitably qualified and experienced ANP however they may be another suitably qualified and experienced healthcare professional for example a GP. Clinical Supervisors will undertake preparation for the role[8].
Annual review
ANPs are responsible for compiling, maintaining and sharing an ePortfolio[9] that evidences their competence to practice as an ANP. At least once a year the ANP should meet with their line manager for an annual review. If the line manager is not an ANP it would be good practice to either undertake a joint review with the ANP's Clinical Supervisor. If a joint meeting is not possible, the Clinical Supervisor should provide the line manager with a report which details the clinical supervision sessions[10].
Annual review will involve the following:
- Professional Portfolio review
- Record of learning activities, reflection, feedback from others (including clinical supervisor)
- Case notes for discussion and review which should related to the individuals level of competence, prescribing practice and include reflection as well as learning/action points (either for review by the line manager, or evidence of peer review or review by the Clinical Supervisor)
- Feedback from patients through compliments, complaints, patient satisfaction surveys or adverse events can be used to inform discussion and reflection
- Job planning – this should follow the Board's Job Planning guidance for ANPs. Job Plans should include time for Supporting Professional Activities (including Continuing Professional Development and contributions towards the other pillars of Advanced Practice: facilitation of learning, leadership, and research).
Normally the KSF would also be completed at this review and revalidation every three years.
NMC revalidation
Evidence of Clinical Supervision should be included within your evidence for revalidation.
Summary
These guidelines set out the minimum standards for Clinical Supervision of Advanced Nurse Practitioners within the West Region. Individual Boards, Higher Education Institutions or other awarding bodies may have additional requirements.
Contact
Email: ian.roxburgh@gov.scot