A TB Action Plan for Scotland
Scottish Government's policy on tuberculosis (TB)
1. Introduction and Background
Tuberculosis
1.1 Tuberculosis ( TB) is a global issue and it is estimated that TB continues to kill approximately 1.8 million people worldwide each year.
1.2 TB is a disease caused by infection with a bacterium called Mycobacterium tuberculosis. The organism is related to a number of different bacteria which together are called the Mycobacterium tuberculosis complex.
1.3 TB commonly infects people's lungs and respiratory tracts and in these cases it is known as pulmonary or respiratory TB. However, TB can infect almost any part of the body as non-pulmonary or non-respiratory TB.
- Pulmonary (or respiratory) tuberculosis is a TB infection of the lungs themselves, or of the bronchi or trachea (the windpipes) or of the larynx (the voice box)
- Non-pulmonary (or non-respiratory) tuberculosis is a TB infection of any other part of the body, provided there is also no TB infection of the lungs as described above.
1.4 The symptoms of TB vary, depending on which part of the body is infected. General symptoms include fever, night sweats, weight loss, loss of appetite and lethargy. Pulmonary TB usually causes a persistent, severe cough with sputum which may have blood in it. Non-pulmonary TB causes symptoms which are related to the organ infected. For example TB of the glands may cause swelling in the neck and a discharge.
1.5 TB infection can be latent or active. The symptoms of latent and active TB are summarised in Table 1 below. A person with active TB may spread TB infection to others, usually has a positive tuberculin skin test (see 1.11 below) or positive TB blood test, and may have an abnormal chest x-ray or positive sputum smear or culture.
TABLE 1: Latent and Active TB
Latent TB |
Active TB |
|---|---|
A person has:
|
Symptoms may include:
|
1.6 When a person is infected with TB, they may simply get better, recovering from the infection. However, in some cases the initial infection can progress to become active TB disease and in these cases it usually becomes a slowly progressive disease which is likely to be fatal if left untreated. An initial TB infection may also become a latent TB infection, where the infected person feels completely well while the bacteria remain alive but dormant in their body. A latent TB infection may become active later in life if, for example, the person's immune system is weakened (by age, other diseases or medical treatments). In this case, it progresses to the active TB disease, already described.
1.7 Treatment for TB requires a course of a combination of four antibiotics, which a patient must take for at least six months. Because of the particular drugs involved, which tend to be used only for TB, some doctors and nurses specialise in treating TB and work together as a team to look after TB patients.
1.8 The bacteria which cause TB can develop resistance to the drugs used to treat the condition. For this reason, it is very important that every patient completes their full course of TB treatment. If the bacteria develop resistance to the antibiotics the disease becomes much more difficult to treat. There has been an increasing risk of TB bacteria developing resistance to the main antibiotics used to treat the disease. This is known as multi-drug resistant TB ( MDR- TB). More recently, some TB bacteria have developed many more antibiotic resistances; this is known as extensively drug resistant TB ( XDR- TB) and is extremely difficult to treat. Treatment of drug-resistant TB also takes much longer than non-drug resistant TB and is also significantly more expensive.
1.9 When HIV and TB disease occur together they interact and treatment becomes very complicated, with several different drugs required. Those with such 'co-infection' may have a poorer outcome unless both conditions are identified early and treatment is very closely supervised.
1.10 Currently, the only available vaccine against TB is the Bacillus Calmette-Guerin ( BCG) vaccine. The BCG vaccine contains live bacteria that have been modified to be safe. Studies of the effectiveness of the BCG vaccine have given widely varying results, but meta-analyses have shown the vaccine to be 70 to 80% effective against the most severe forms of TB, such as TB meningitis in children. The vaccine is less effective at preventing respiratory disease, which is the more common form in adults. Protection has been shown to last for 10 to 15 years. There are few data on the protection afforded by BCG vaccine when it is given to adults aged 16 and over, and virtually no data for persons aged 35 years or over. For more information on the BCG vaccine see the Department of Health publication Immunisation Against Infectious Disease (the 'Green Book') which is available in electronic format at the following link: http://www.dh.gov.uk/en/Publichealth/Immunisation/Greenbook/index.htm.
1.11 The tuberculin skin test is a diagnostic tool for TB. It helps to determine if someone has an immune response to the bacterium that causes TB. The skin test is administered and then read 2-3 days later. Administration involves injecting a small amount of tuberculin protein into the skin with a needle and syringe. A person who has been exposed to TB bacteria previously, who currently has TB, or who has had a BCG vaccination in the past, will normally mount an immune response in the skin containing the tuberculin bacterial proteins. If the test is positive, further investigation may be necessary.
1.12 New diagnostic tests for TB have recently been developed called Interferon Gamma Release Assays ( IGRAs). These are discussed further in section 2.
A Global Issue
1.13 Tuberculosis occurs across the world, although the World Health Organisation ( WHO) estimates that 95% of TB cases now occur in developing countries. The effective treatments for TB described above have been available since the 1940s and many countries have made great progress in controlling the disease. However, despite the availability of effective drugs TB remains one of the leading causes of human illness and premature death in the world. The WHO Global Tuberculosis Control 2010 report ( http://whqlibdoc.who.int/publications/2010/9789241564069_eng.pdf) indicates that there were an estimated 14 million people living with TB in 2009 (see Table 1, page 5 of the 2010 report).
1.14 In 1991 the World Health Assembly recognised that TB was a major global public health problem and adopted a resolution calling for increased efforts to control TB. In 2000, The United Nations adopted the Millennium Development Goals ( MDG). MDG 6 defines the objectives of halting and starting to reverse the incidence of several major diseases including TB by 2015. This has increased the need for work to control TB. On 23 May 2007 the World Health Organisation adopted a resolution ( WHA60.19 - (World Health Assembly)) calling for all Member States to develop and implement long-term plans for tuberculosis prevention and control in line with the Global Plan to Stop TB 2006-2015. Although there has been a small decline in worldwide incidence of TB, the reductions in incidence are not likely to meet the WHO target of halving the prevalence and mortality as a result of TB from 2006 to 2015.
1.15 The WHO has developed a new six point "Stop TB" Strategy ( http://www.stoptb.org) addressing the key challenges facing TB. Its goal is to dramatically reduce the global burden of TB by 2015 by ensuring all TB patients, including for example, those co-infected with HIV and those with drug-resistant TB, benefit from universal access to high-quality diagnosis and patient-centred treatment. The strategy also supports the development of new and effective tools to prevent, detect and treat TB. The six points of the Stop TB Strategy include:
1. Pursue high-quality Directly Observed Therapy expansion and enhancement (see http://www.who.int/tb/dots/en/ for more information on Directly Observed Therapy)
2. Address TB- HIV, MDR- TB and the needs of poor and vulnerable populations
3. Contribute to health system strengthening based on primary health care
4. Engage all care providers
5. Empower people with TB, and communities though partnership
6. Enable and promote research
1.16 While TB has been declining globally in recent years, it is actually increasing in Europe. Accordingly the European Centre for Disease Control ( ECDC) has a programme of work to tackle TB under its Framework action Plan to fight TB in the EU. (Available in electronic format at the following link :http://www.ecdc.europa.eu/en/publications/Publications/0803_SPR_TB_Action_plan.pdf).The programme aims to support Member States in TB prevention and control and thus reach the long-term goal of reducing and ultimately eliminating TB in the EU. The WHO defines "elimination" as an incidence of less than 1 per million population per year. It also intends to create a reference point for EU Member States that provides relevant expertise and information about trends in the epidemiology of TB, about emerging threats related to TB and about scientific advances in the field.
1.17 The Scottish Government takes seriously the WHO resolution and the work of the ECDC to tackle TB and recognises the impact of the global TB burden on the Scottish population. The Scottish Government has also made a commitment to Health is Global, a UK Government strategy in respect of global health priorities (published 30 September 2008 and available electronically at the following link: http://www.dh.gov.uk/en/Publichealth/Immunisation/Greenbook/index.htm). and TB is identified in this. Scotland is committed to global action on TB
The Scottish Dimension
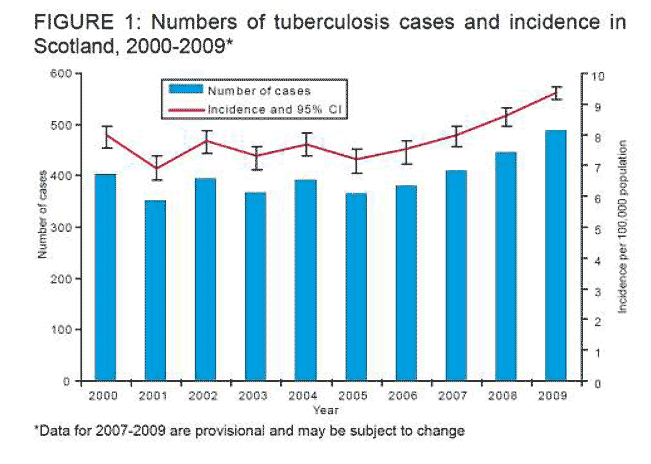
1.18 The impact of this global public health threat is very much felt in Scotland. The development of drug resistance due to inadequate treatment and higher prevalence of disease in certain countries (due to poor detection and high levels of HIV in the population) has a significant impact on the UK and Scotland. While in the recent past the number of TB cases in Scotland has been largely stable, epidemiological data from the last 4 years suggests that this picture is changing (see Figure 1 below) We are therefore seeing an increase in cases that mirrors the picture in some other parts of Europe (Sweden, Ireland). This presents a number of challenges for the NHS in Scotland.
1.19 Cases of tuberculosis are currently recorded in Scotland using two different systems. The first is a system of "notification" of infectious diseases. This notification system has been in place since 1976 and simply records whether a patient with tuberculosis has pulmonary or non-pulmonary disease. The second system is the Enhanced Surveillance of Mycobacterial Infections ( ESMI) system which has been operating since 2000. This system records much more information about tuberculosis cases, including details of their diagnosis, treatment and how well they have recovered. The detailed information on tuberculosis in Scotland is based on the ESMI data.
1.20 Scotland has had a continuing increase in the numbers of tuberculosis cases and the incidence of TB since 2005 (see Figure 1, below).The incidence in Scotland was lower than that of the whole of the UK population in 2009: 9.4 per 100,000 population in Scotland compared with 14.6 cases per 100,000 population across the UK. However, the incidence in Scotland is rising and is catching up with the rest of the UK. The 487 cases reported in 2009 were an increase of 8.8% in the incidence compared with 2008.
1.21 Historically, Scottish TB incidence has been higher in Glasgow and its surrounding area. In 2009, Greater Glasgow and Clyde notified 235 TB cases (48% of Scotland's total, an incidence of 19.6 per 100,000 of the population). Lothian had 78 cases and Grampian had 52 (incidences of 9.4 and 9.5 per 100,000 respectively).
1.22 In 2009 TB was more common amongst males, with 298 cases representing 61% of TB cases. The age group which had the most TB cases was aged 25-34 years, while TB was least common amongst those aged 5-14 years. The rate of TB among children aged under five years has remained stable at 3.1 cases per 100,000. This is important as infections in this age group do not occur from reactivation of latent TB infections, so this implies recent infection with TB. The fact that this figure has remained constant therefore suggests that transmission of TB within the population is continuing in Scotland.
1.23 The main risk factor for TB infection in Scotland is being non- UK born. In 2009, 53% of TB cases in Scotland were described as White Caucasian, while those of Pakistani or Indian origin accounted for 15% each and Black Africans represented 8%. 47% of those whose place of birth was known, were born outside the UK. Patients who were born in the UK had a higher average age when they were diagnosed (53 years) than those who had been born abroad (34 years). Of those born abroad, 31% were born in India and 28% were born in Pakistan while Nigeria and Nepal each accounted for 4% of these cases. 74% of those who were born abroad had entered the UK two or more years before they were diagnosed with TB and 38% had entered five or more years earlier. It is not fully understood why individuals develop TB more than 2 years after arriving in the UK but this could also be related to either latent infection on entry to the UK, infection once within the UK or perhaps frequent travel abroad.
1.24 Aside from place of birth, the other main risk factor for TB is problem alcohol use. The incidence of TB is also influenced by - and associated with - adverse social circumstances such as poverty, poor nutrition, reduced access to healthcare, homelessness, problem drug use and imprisonment (although TB is not a significant problem in Scottish prisons, with very few cases in the last ten years).
Current Policy
1.25 In Scotland, the most recent national and strategic document that set out policy on TB was The Control of Tuberculosis in Scotland, published by the Scottish Office Department of Health in 1998 (available in electronic format at: http://www.scotland.gov.uk/Resource/Doc/158121/0042779.pdf). This document has been supplemented by CMO letters and other instructions since it was published.
1.26 In March 2009 the Scottish Health Protection Network published Tuberculosis: Clinical diagnosis and management of tuberculosis, and measures for its prevention and control in Scotland, (available at: http://www.documents.hps.scot.nhs.uk/about-hps/hpn/tuberculosis-guidelines.pdf) which was adapted from the similar publication by the National Institute of Clinical Excellence ( NICE) in England. This document provided updated guidance to professionals on clinical approaches to management of TB and effectively superseded the 1998 Scottish Office document.
1.27 Given the changing epidemiology within Scotland and other developments across the UK and globally this TB Action Plan provides an opportunity to build on and support the implementation of the existing Scottish Health Protection Network guidance.
An Action Plan for Scotland
1.28 Recognising these commitments and developments, in 2008, the Minister for Public Health and Sport requested the Scottish Government and Health Protection Scotland to develop a TB Action Plan for Scotland. The aim of this Action Plan is to identify where current practices and services could be improved or enhanced, with the long term goal of a reduction of TB incidence in Scotland.
1.29 A Working Group, chaired by a Senior Medical Officer from the Scottish Government, was convened to take forward this work. To support the Working Group, four topic specific Subgroups were convened, each of which was tasked with reviewing evidence and experience in respect of one or more of the key areas of work for the Action Plan. Subgroups provided their conclusions to the Working Group which then consolidated the Subgroup recommendations into this Action Plan.
Membership of all groups is attached at Annex A and B.
Themes
1.30 As requested by the Minister for Public Health and Sport, the Working Group agreed to provide recommendations for actions specifically covering the following themes:
- Effective laboratory services and diagnostic tools - consideration of the best models of service for Scotland in terms of laboratory diagnostic services for TB.
- Effective clinical services in the broad sense - considering issues around identification, management and treatment of TB; around models of care; and best use of resources locally and nationally. It was also agreed that this strand of work would also consider associated issues such as drug resistant TB and co-infection issues ( HIV).
- Effective surveillance - assessment of current surveillance systems and the need for/options for improvement.
- Effective public health services - considering issues around population level approaches to tackling TB, including contact tracing; detecting TB in risk groups; approaches to vaccination, and awareness raising.
1.31 In delivering this work, the Working Group and sub-groups considered recent evidence and experience including, but not limited to:
- Surveillance information in Scotland showing an upwards trend in incidence of TB in Scotland;
- A lack of knowledge around the current effectiveness and application of the selective vaccination programme and the need to reinforce professional practice to ensure the programme is effective;
- The results of a stocktake of TB services within Scotland carried out by Health Protection Scotland as part of the Action Plan development process.
- Some evidence of varying levels of clinical performance and practice in Scotland in respect of TB;
- Recent TB related public health incidents;
- The guidance document, Clinical Diagnosis and Management of TB and Measures for its prevention in Scotland;
- Tuberculosis in the UK, the Health Protection Agency annual report on tuberculosis; and
- The experience elsewhere in the UK, particularly in respect of Stopping Tuberculosis in England, the Department of Health action plan on TB, published in October 2004.
- Evidence and action plans for Europe ( ECDC's Framework action Plan to fight TB in the EU) and the World ( WHO's Stop TB Strategy)
The Healthcare Quality Strategy for NHSScotland
1.32 The Scottish Government published its Healthcare Quality Strategy on 10 May 2010 (available at http://www.scotland.gov.uk/Topics/Health/NHS-Scotland/NHSQuality). The Strategy sets out the Scottish Government's vision for health and health care in Scotland and, in particular, three Quality Ambitions that provide a focus for all activity.
1.33 In developing the TB Action Plan and finalising recommendations the Working Group has kept the key themes of the Quality Strategy in mind, in particular the three Quality Ambitions. These are central to what this Action Plan is seeking to achieve. Specifically:
- Mutually beneficial partnerships between patients, their families and those delivering healthcare services which respect individual needs and values and which demonstrate compassion, continuity, clear communication and shared decision-making
- There will be no avoidable injury or harm to people from healthcare they receive, and an appropriate, clean and safe environment will be provided for the delivery of healthcare services at all times
- The most appropriate treatments, interventions, support and services will be provided at the right time to everyone who will benefit, and wasteful or harmful variation will be eradicated.
1.34 The recommendations contained within this Action Plan seek to reduce the future number of people developing TB and improve delivery of services to those affected by TB in Scotland in line with these ambitions.