Adolescents' screen time, sleep and mental health: literature review
Systematic review summarising the published experimental and longitudinal evidence on adolescent screen time, sleep and mental health.
Research Question 3: What are the implications of the potential impact of mobile device screen time on sleep for adolescents' mental health and wellbeing?
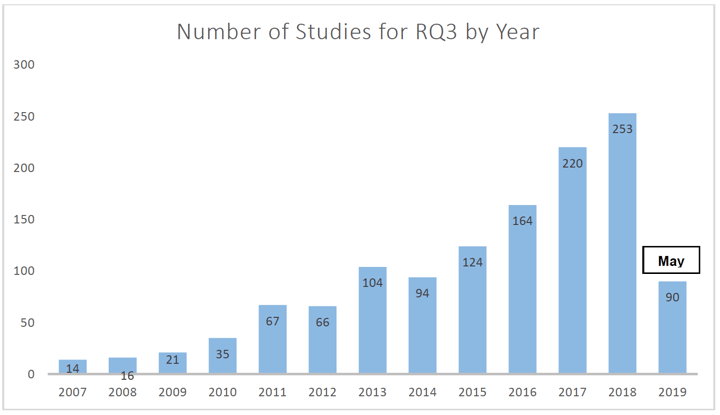
As for Research Question 1, publications about the links between adolescent electronic media use, mental health and wellbeing, and sleep increased substantially over the last decade, from 14 publications in 2007 to 253 publications in 2018 (Figure 5). Much of the research included cross-sectional studies and looked at direct associations between media-sleep or media-mental health and not the indirect pathway between media-mental health via sleep. Therefore, most studies were not eligible for inclusion (see Figure 2).
Figure 5. Primary studies returned by year for RQ3
Three studies met the inclusion criteria for this Research Question (21-23). The characteristics of included studies and the findings are summarised in Appendix Table F.
Description of studies
Study design, geographical location and setting
All three studies were conducted in Australia (21-23). Two were longitudinal observational studies that used the same cohort of adolescents (21, 22), and one pilot study (i.e. the same small scale, preliminary study included in RQ1) offered an intervention to all study participants using a one group before-after study design without control group (23). One of the longitudinal studies tracked the effects of problematic social networking on adolescent psychopathology and examined sleep as a mediating variable between the two (21). The other longitudinal study examined the relationship between changes in adolescent night-time mobile phone use and sleep behaviour over time (22). The pilot study sought to test the effects and acceptability of an app that aimed to help adolescents with sleep difficulties (23).
The two longitudinal studies collected data through administering questionnaires at schools using laptops or iPads (21). For the pilot study, participants received an app and reported on their experiences using it in the home setting as well as participated in an in-depth semi-structured interview.
Sample size and participant characteristics
Sample sizes ranged from 50 to 1101 participants. The longitudinal studies had 874 participants (21) and 1101 participants (22). The pilot study had a sample size of 50 but complete outcome data for only 29 to 34 individuals in the study (23).
Participants ranged in age from 12-16 years. One study did not report the age range and only provided the mean age of 14.4 years (21). The majority of participants were female (57-66%). The Vernon et al (21, 22) studies used the same cohort of recruited students. The pilot study authors recruited adolescents with at least mild insomnia (23).
Vernon et al (21) had a sample that was 57.2% Caucasian, 7.2% Asian, and 1.6% Aboriginal or Torres Strait Islander, 23.3% other (e.g. Middle Eastern, African, Indian, or Maori), and 10% did not report ethnicity. Vernon et al (22) reported that 14 out of 27 schools that students were recruited from, were at or below the median for socioeconomic status, making 44% of the sample lower SES. The authors of the pilot study did not report ethnicity or socioeconomic status of their participants (23).
Exposures
Exposures for the three studies were related to problematic social network use (21), night-time mobile phone use (22), and an app that sought to improve sleep outcomes (23). The two longitudinal studies used self-report questionnaires to assess social network and phone use. For the pilot study, authors assessed app/intervention acceptability and non-adherence through questionnaires and interviews (23).
Outcomes
All three studies reported on mental health and wellbeing outcomes using a range of scales (e.g. the Generalised Anxiety Disorder 7-item scale or GAD-7) (23). Only one measure, coping, used a single question (22). Outcomes assessed included depressed mood, anxiety, externalising behaviour, self-esteem, and coping.
Quality of studies
Table 3 shows the quality rating of the three included studies. Each of these three studies was included in RQ1 and because they reported also on mental health and wellbeing outcomes, they received a separate quality assessment here. All three studies were of low risk of bias for assessment of mental health and wellbeing outcomes. Vernon et al (2018) was of high risk of bias due to methodological shortcomings in the assessment of night-time media use. Werner-Seidler et al (2019) was of high risk for population selection and attrition bias. Vernon et al (2017) showed limitation in reporting and did not allow assessment of the level of risk of bias for most quality items.
Table 3. Quality assessment of included studies with mental health outcomes
| Quality items | Vernon et al 2018 | Vernon et al 2017 | Werner-Seidler et al 2019 |
|---|---|---|---|
| Selection bias | (Y) | (Y) | (R) |
| Performance bias | (R) | (Y) | (G) |
| Detection bias | (G) | (G) | (G) |
| Attrition bias | (G) | (Y) | (R) |
| Selective reporting bias | (Y) | (Y) | (Y) |
Green=low risk of bias, yellow=unclear risk of bias, Red=high risk of bias
Findings
Table 4 summarises the findings on the implications of the potential impact of mobile device screen time on sleep for adolescents' mental health and wellbeing. The findings described below must be interpreted with caution since most are based on studies of poor quality and may be subject to bias.
Table 4. Summary findings for RQ3
| Exposures |
Number of studies |
Number of participants + ages |
Mediator |
Outcomes |
Summary findings |
|---|---|---|---|---|---|
| Night-time mobile use |
1 |
N=1101 Age: 13-16 years |
Sleep quality |
Depressed mood |
- |
| Externalising behaviour |
- |
||||
| Self-esteem |
- |
||||
| Coping |
- |
||||
| Social media use |
1 |
N=874 Age: 14 years |
Sleep quality |
Depressed mood |
- |
| Externalising behaviour |
-/+ |
||||
| Smartphone app |
1 |
N=50 Age:12-16 years |
App-based sleep education |
Depressive Symptoms Anxiety |
+ + |
+/- no mediation effect, - negative mediating effect, + positive mediation effect
Night-time mobile phone use
Findings from a single study (21) suggested that sleep quality influenced the statistically significant associations between night-time mobile phone use and mental health outcomes (Appendix Table F). High levels of night-time mobile phone use at 13.5 years of age on average (baseline) were linked to poor sleep quality, which in turn was associated with higher levels of depressed mood, externalising behaviour, low self-esteem and poor coping abilities one year later. Poor sleep quality explained 91%, 83%, and 77% of the observed association between night-time mobile use and low self-esteem, poor coping ability, and high levels of depressed mood, respectively. The role of poor sleep quality was less strong for the association between night-time mobile phone use and externalising behaviour. Externalising behaviours are problem behaviours directed at the external world like physical aggression or disobeying rules.
Similar findings were reported when participants showed an increased night-time use of mobile phones over a duration of two years. Change in sleep quality influenced the effect of change in night-time mobile phone use on subsequent change in all mental health outcomes. Change in sleep quality explained the association between change of night-time mobile use and depressed mood with 73%, followed by 60% for poor coping abilities, and 50% for low self-esteem.
Social media use
Using the same cohort of adolescents as for night-time mobile phone use, Vernon et al (22), assessed the mediating effect of sleep quality on the association between social media use at an average age of 14.5 years and mental health outcomes (depressive mood and externalising behaviour, like disobeying rules or physical aggression) two years later.
Findings indicated that poor sleep quality partially influenced the association between high levels of social media use and high levels of depressed mood and externalising behaviour. This means that poor sleep quality explained some of the observed link between social media use and mental health but the direct associations between social media use and the two mental health outcomes remained statistically significant.
However, when considering changes of social media use, sleep quality, depressed mood and externalising behaviour over a duration of two years, change in sleep quality fully influenced the association between changes of social media use and changes of depressed mood. Change in sleep quality partially influenced the relationship between change in social media use and change in externalising behaviour.
Smartphone application
Findings of the smartphone app intervention (a pilot study, with no comparison group) suggested an improvement in depressive symptoms immediately after using the app by -3 scores on a scale of 0-24 points (Appendix Table F). Higher scores mean more depression. This indicated that on average, adolescents aged 12-16 years with sleep difficulties remained in the "mild symptom" category (10-14 scores) while shifting from scale point 13 at baseline to scale point 10 at follow-up. The intervention effect was small and the study was of poor quality (Appendix Table F). The effect of the app on anxiety was also small. Participants changed on average from 10 scale points indicating "moderate anxiety" (10-14 scores) at baseline to 7 scale points indicating "mild anxiety" (5-7 scores).
RQ3 Summary
The three included studies provided findings on the indirect association between three different types of mobile device exposure in adolescents and six different mental health and wellbeing outcomes. Eight unique exposure-mediator-outcome relationships (see Figure 1) were assessed across the three included studies of which each relationship was explored by no more than one study. Available evidence indicated that night-time mobile use and problematic social media use were linked to depressed mood through experiences of poor-quality sleep. A pilot study found that use of a smartphone app that teaches healthy sleep habits was potentially associated with lower depressive symptoms and reduced anxiety in the short term follow up period. Poor sleep quality also mediated the link between night-time mobile phone use and low self-esteem, poor coping skills and higher externalising behaviour. Table 4 provides a summary overview of the body of evidence on the difference exposure-outcome relationships.
Our confidence in validity of the reviewed evidence is limited for the following three reasons: (i) only one study was available for each exposure-mediator-outcome association, (ii) evidence was available for only two different cohorts of participants, and (iii) the quality of included studies was at unclear or high risk of bias. Therefore, the available evidence on the role of sleep in the association between adolescents' mobile device screen time/use and mental health is incomplete.
Contact
Email: socialresearch@gov.scot