A Study of Medical Negligence Claiming in Scotland
The study examined the current system for medical negligence claiming in Scotland. The study was commissioned to inform the work of the No-fault Compensation Review Group which was established in 2009 to consider the potential benefits to patients of the introduction of a no-fault compensation scheme for medical negligence claims in Scotland.
CHAPTER 2: RESULTS OF THE STUDY OF PRESENT SYSTEM
3.1 This chapter provides an analysis of the results of our research on the present negligence based system. It follows the structure of claiming as described by Mulcahy and Tritter (1998), who conceive patients' dissatisfaction with medical care as a pyramid with medical negligence claims as the tip and all patients who receive medical treatment at the base. The next level up from the base consists of patients who make a complaint. Overall, the proportion of patients who make a complaint is very small. The majority of people who make a complaint do not make a claim. A medical negligence scheme must be understood in terms of the way a dissatisfied patient moves up the pyramid.
3.2 Some of the desired objectives for a new Scottish scheme are linked to the parties directly involved, such as providing compensation that is acceptable to the patient and their family. Other objectives are concerned with the wider picture, such as organisational, local and national learning; patient safety; and quality improvement. These wider objectives may not be achievable by a medical negligence scheme alone. It is important that a new scheme is tied into the entire process by which patients attempt to resolve disputes. Any changes to each level within the pyramid are likely to have effects in the other levels, and so the interconnections need to be considered.
Adverse events
3.3 The base of our pyramid consists of patients who have been the victim of an adverse event. One of the expressed aims of a new scheme is to improve patient safety, and this implies reducing the number of adverse events. There is no data concerning the incidence of adverse events involving personal injury in Scotland, although research across the UK suggest that 10% of hospitalisations result in adverse events with half being preventable (Vincent et al. 2001). Audits of specific areas of medical speciality in Scotland and morbidity reports suggest that the frequency of adverse events in Scotland is similar to England and Wales (Crawford 1991, Christie 2003).
3.5 Interviews with stakeholders suggested that the current system achieves some of requirements of institutional learning and reporting of errors. There was evidence that some practitioners were prepared to be open about errors. For instance, several pursuers explained that they had been encouraged to see a solicitor after the doctor who performed the surgery told them that they had made a mistake, and that the patient should sue. These pursuers also described the steps the surgeon took in trying to remedy the error, such as referring to a new surgeon and following up with the patient to check that they had received ongoing medical care. All of these pursuers had met with the surgeon who was responsible for the error, had received an explanation of what had happened; and an apology. Medical practitioners and NHS managers also described how adverse events are reported and then explained to patients, and NHS staff mostly appeared satisfied that a system of reporting was in place which ensured lessons were being learnt. Interviewees explained that the NHS was a much more 'open culture' now relative to five years ago.
3.6 However, all of the NHS staff interviewed acknowledged that problems persist and identified a number of barriers to reporting of errors, including being worried about the threat of litigation, feeling a sense of professional shame or embarrassment and being fearful that an error may harm professional reputation. Most explained that medical records are not always complete, and one NHS manager suggested that medical records are sometimes changed retrospectively without the changes being recorded. Although several NHS managers claimed to have achieved an open culture, they expressed surprise that a medical practitioner would encourage a patient to sue.
3.7 Interviewees from within the NHS explained that individual clinical teams and departments were concerned that lessons were learnt from errors. They explained that team meetings were arranged regularly and that any patterns or reoccurring errors were picked up and dealt with seriously. However, there seemed to be less opportunity to learn from errors occurring across Health Boards. Several interviewees explained that they received reports about patterns of errors. However, they also explained that little attention is generally paid to these which were seen to get lost among the many other reports and correspondence received by clinical staff. Increasing administrative load was also seen to decrease the amount of time available to spend on reading adverse events reports.
3.8 Interviewees including NHS staff, medical practitioner representative bodies and MDS did not feel that compulsory reporting would make much difference. They described reporting as not necessarily being ideal, but that continuing cultural change would alleviate problems rather than stricter regulation.
3.9 Studdert and Brennan (2001), based on the relative openness of Swedish medical practitioners to report errors and encourage patients to make a claim, suggest that no-fault schemes are better than fault-based schemes at reducing adverse events. In a review of all admissions to 13 large hospitals in New Zealand in 1998, Davis et al. (2003) found that the reporting of errors was "remarkably high." They argued that these results suggest that no-fault schemes do not encourage medical practitioners to be afraid of litigation. Yet, in New Zealand the percentage of adverse events is similar to fault-based jurisdictions, including the UK (Davis et al. 2002, 2003).
3.10 The New Zealand scheme has been criticised for failing to provide institutional learning or deterrents for medical practitioners to avoid error. The goals of institutional learning and tracking of errors are not explicitly within the remit of a compensation scheme. They would need to be built in as additional features. Our research suggests that fear of litigation is only one of the barriers to reporting errors. Other research suggests that the main reason for not reporting errors is being unaware of how errors should be reported. Other reasons include fear of reprisals, and lack of confidentiality and time (Jeffe et al. 2004, Garbutt 2007, Kaldjian et al. 2008).
3.12 NHS interviewees pointed to higher staff to patient ratios, greater availability of consultants, greater focus on intern training and supervision relative to England, as being important in ensuring that patients do not feel aggrieved. While there appears to have been improvement in post-operative care, our research suggests that there is still room for progress. Several interviewees stressed that the level of one-on-one care that patients receive pre-operatively does not necessarily carry over into post-operative care. Staff ratios drop and consultants become less available. Patients' perceptions of this difference can lead to dissatisfaction, which if left unaddressed could potentially lead to a negligence claim.
3.13 Several pursuers also felt that there was a connection between resourcing and adverse events. These pursuers felt that an error had occurred as medical staff were being required to make decisions based on resourcing rather than medical needs; elderly or working class patients, were given lower standards of care; some also felt that patients who were overweight, alcoholic, smoked, or had a chronic illness were given sub-standard care; some explained that they had intimated a claim in order to highlight how the NHS was letting down 'the wee people', (people who were seen to be less deserving of care).
3.14 All interviewees working within the NHS, as well as patient support and advice groups, expressed concern about future decreases in resources. Most felt that further cutbacks will reduce standards of care, which will in turn increase the incidence of adverse events. Expectations of any new scheme need to be realistic. A scheme alone cannot achieve better institutional learning, reporting or reducing adverse events. These objectives are much broader, and require other measures also being put into place.
Patient grievances
3.15 Pursuers' narratives of what had gone wrong with their medical care were invariably complicated involving multiple overlapping concerns about medical care, general care, communication, staff attitudes, staffing levels, and resourcing.
3.16 Concerning medical care, pursuers' main concern focused on the failure of medical staff to take the patient's problem seriously. They were not listened to when they tried to convince medical staff that the problem was more serious. For some, the injury would not have occurred if medical professionals had done more tests, paid more attention to stated symptoms, or read the medical notes properly. For others delay was the problem. If medical professionals had acted sooner, the injury would not have occurred. Once the serious state of their (or their relative's) medical condition became known, the medical staff 'denied' that the delay or lack of diagnosis had been a problem. In a few instances, pursuers felt that the medical staff were unaware that an error had occurred, however, 'They should have known'.
3.17 Problems with general care, in particular, the lack of hygiene had led to infections. Several also complained that relatives were not being fed in the hospital, patients were left to self-medicate, and other basic needs were not being attended to. Medical staff were seen as inattentive, dismissive of family concerns, and failed to treat patients with sufficient care.
3.18 Most pursuers also felt that the injury was caused, at least in part, by poor communication on behalf of the medical staff. All said that they had tried to raise their concerns with medical professionals, but their concerns were not listened to. Some felt that staff lacked empathy and compassion, were 'bullying' or arrogant, and as a result failed to pay attention when the patient had tried to communicate that their problem was serious. Pursuers explained how a doctor or nurse did not fully listen to their concern and jumped to a preconceived idea or conclusion of what the problem was and how to treat it.
3.19 For some pursuers, consent had been forced by a medical professional who refused to listen to the patient's concerns particularly given the patient's emotional state. Pursuers felt that the doctor involved should have been aware that the patient was afraid, desperately ill and in a vulnerable position. For others, consent had been sought from the patient, who was not capable of providing consent and instead the family should have been more involved.
3.20 Discontent about the exclusion of family members from medical decisions was a recurring theme, especially if the patient had died. Family members recalled being denied access to the patient's medical notes, not being informed of what was going on, and not being treated compassionately. Some of these problems had occurred during treatment but some continued after the patient had died. One pursuer described how she had been promised a post-mortem which she felt would have provided insight into why her husband had died. The post-mortem did not occur. Another had to take the NHS to court to have her husband buried in the cemetery of her choice.
3.21 Further recurring themes were: insufficient staffing levels; lack of availability of consultants; and under-resourcing of the NHS (resulting in some groups of patients receiving a lower standard of care than others). Some pursuers felt that medical care had been left to nurses or junior doctors, who did not have the skills to recognise the seriousness of their problems. They stated that consultants were not sufficiently available, or refused to listen, were arrogant, did not examine the patient adequately or were uninterested.
3.22 Our research suggests that patient dissatisfaction is an outcome of multiple factors. Pursuers felt that the combination of poor communication, staff attitude to listening to patients, lack of availability of consultants, as well as failure to diagnose, resulted in a medical injury. An accumulation of problems led to a sense of disempowerment.
3.23 Similarly, previous research has suggested that patients do not sue simply because they have been injured. Complaints frequently focus on communication, attitudes, general problems and waiting times, not on issues of treatment, tests, diagnosis and surgery (Allsop 1994, Mulcahy and Tritter 1998). A patient may be injured by a serious adverse event but not take legal action. Another who has suffered a minor problem or has not been injured may make a claim (Studdert et al. 2006). A large number of researchers have suggested that communication breakdown between doctors and patients may lead to litigation (Adamson et al. 1989, Daniel et al. 1999, Hickson 2002, Huycke and Huycke 1994, Lester and Smith 1993, Levinson et al. 1997, Lloyd-Bostock and Mulcahy 1994, Penchasky and Macnee 1994, Press 1984, Shapiro et al. 1989, Vincent et al. 1994). Our findings are similar.
3.24 NHS staff interviewed largely concurred that communication breakdown, family members feeling excluded, and the lower availability of consultants post-operatively were the main reasons behind patient dissatisfaction. Several described patients as often being reluctant to speak up directly if they are unhappy, and instead practitioners need to be more attuned to indirect signs, such as a patient becoming withdrawn. They also described that some practitioners simply did not have strong patient listening skills, and that despite efforts to take a more patient-centred approach, problems with poor communication have not decreased. They explained that while it may be well-known within a hospital that some consultants were more likely to receive complaints relating to attitude and communication, it was unfair to give these practitioners less patients. It was felt that little could be done to improve these problems as they are largely due to consultants' individual personalities.
3.25 These findings point towards ways to potentially decrease patient dissatisfaction, which are not necessarily tied to the implementation of a new scheme. Most grievances are associated with communication breakdown, and while this appears to be well known, it appears that little headway is being made. The focus of medical practitioners on clinical aspects of care, and the belief that problems cannot be alleviated due to individual personalities act against improving practitioner-patient relationships. A new scheme would not address these problems, and it seems that these issues need to be addressed institutionally and before the patient makes a complaint.
3.26 In addition, our findings suggest that pursuers cannot easily make a distinction between communication and general care problems, and instances involving a negligent clinical error. The growing complexity of issues being raised suggests that a new scheme will receive a mix of problems, and pursuers cannot be relied upon to isolate the issues involved. There will need to be a screening and investigation process to sort out claims where a clinical error has occurred. It is possible that many claims will not contain a serious clinical error, yet the pursuer will want their problems acknowledged, and possibly, to receive compensation. To dismiss poor communication as not being of serious concern may risk some pursuers continuing to be dissatisfied.
Complaints
3.27 The complaints procedure in Scotland provides a single, simple route for making a complaint against any NHS service. Complaints can be made in any format, including raising a concern in person, via email, or in writing. There is a strong emphasis on local resolution, with the expectation that investigation and resolution will be completed within 20 days. Complaints managers explained that within this timeframe, they needed to obtain medical records, talk to the staff involved, and write to the patient. Patients who are dissatisfied with the outcome of their complaint can then proceed to the Ombudsman. The complaints procedure is intended to provide patients with an investigation, explanation, and where appropriate an apology; however, it does not provide financial compensation.
3.28 The number of complaints in Scotland has remained relatively stable in recent years (Table 1). In 2008/09, a total of 10,967 complaints were recorded. Of these 6904 were made against hospitals and community services the bulk of which (4921) were made against acute services. A total of 3175 complaints were made against family health services, the bulk of which were made against GPs. Over half of the complaints related to staff attitude/behaviour and 29% concerned treatment, which again reflects the importance of improving communication in order to avoid patient grievances. Of these complaints, 29% of complaints were upheld, 33% partly held, and 39% not upheld.
Table 1: Number of medical complaints since 2006
| 2006/2007 | 2007/2008 | 2008/2009 | 2009/2010 | |
|---|---|---|---|---|
| Complaints | 11,230 | 11,144 | 10,967 | 7,123 |
| Ombudsman | 632 | 599 | 684 | 859 |
(Note: changes to the logging of complaints to the Ombudsman were made in April 2007. The 2006/07 figures have been adjusted. However, adjustments cannot be made for data collected prior to 2006).
3.29 The large majority of pursuers interviewed had used the complaints procedure. Of those that did not, the injury was clear and the doctor involved admitted immediately to the pursuer that there was a problem. In one case, the doctor encouraged the pursuer to see a solicitor. In another instance, the pursuer described that the Clinical Director arranged a meeting in order to avoid "lots of letters", and promised to get back to the pursuer following an investigation. When the patient did not hear anything further, they contacted a solicitor.
3.30 Pursuers appeared to be knowledgeable about the complaints procedure, and the main source of dissatisfaction consisted of the failure to provide a 'real' explanation rather than the process. The main complaint about the process was that it lacked independence. For many of the pursuers, the investigation of complaints about medical professionals by the NHS represented a 'cover up.' Some had received explanations and apologies, but felt that these were simply platitudes intended to prevent pursuers asking further questions. There were some other problems with the process, for instance, the Clinical Director who did not take forward the promised investigation (above). Another pursuer explained that she had not received a reply to her complaint despite her efforts at following up.
3.31 Our results suggest that, for the most part, the process of filing a complaint is accessible; however this finding may be an outcome of our research method. We only interviewed people who pursued a claim, and pursuers described themselves as being determined and resilient. We did not speak to people who attempted to negotiate the complaints procedure or make a claim, but gave up. In addition, pursuers tended to focus on the narrative of the problems they had experienced with their (relative's) medical care. The process of trying to resolve their claim, including the use of the complaints procedure, did not seem to be so central to pursuers.
3.32 There is some other evidence that Scottish patients are satisfied with the complaints process, at least relative to patients in England. Despite only one third of complaints being fully upheld, only a very small proportion of complaints are made to the Ombudsman in Scotland. In 2009/10 the Scottish Ombudsman received 859 health related complaints, of which only 20 (2.3%) related to the way in which the initial complaint had been handled. In contrast, in 2007/08, 20% of complaints made to the Ombudsman in England related to poor handling of the initial complaint. In England, the complaints procedure has been criticised for being too complex and lengthy, and patients have experienced lost complaints, long delays, and feel that healthcare staff are not open about errors. One survey found that 30% of complainants felt that the complaints procedure was pointless (The Patients Association 2008).
3.33 This is not to say the Scottish procedure could not be improved. Older research conducted by McCrindle and Jones (1998) describe the complaints procedure as being too complex, not being user friendly, taking too long to make decisions, producing defensive responses and failing to give satisfactory explanations. More recent research recommended better training for staff involved in handing complaints, that information about making complaints was made more accessible, and that there was a greater provision of face-to-face and telephone contact rather than such a heavy reliance of written communication (The Expert Group on Financial and Other Support 2003:33). Since these findings, however, the complaints procedures have been changed. In addition, it has been suggested that complainants are not always satisfied with the explanation that they are given, do not always receive an apology, or feel that they were listened to (Britain et al. 2009).
3.34 Britain et al.'s (2009) recent evaluation of the complaints procedures in Scotland also showed that there was a heavy reliance on written material and written communication. NHS staff in Scotland reported that the increasingly complex nature of complaints made the 20 day limit difficult and that complaints managers were feeling overwhelmed by relatively trivial complaints. We were also told by NHS staff that complaints were becoming increasingly complicated and multi-faceted. They explained that the process of investigating was often difficult to complete within 20 days, especially if medical records had to be located across different sites, medical notes were not complete, or the staff involved were on leave. It was suggested that patients would possibly prefer that complaints were investigated thoroughly rather than replies provided within 20 days. Incomplete responses may leave patients feeling that the Health Board is being evasive or is supporting a 'cover up'.
3.35 Our research found that the strongest critics of the complaints procedures tended to be NHS staff who were directly involved in handling complaints. Several criticisms of the ways in which complaints were dealt with were given: medical staff sometimes react defensively; a suggestion that medical reports are occasionally changed retrospectively; replies to their inquiries are often written using complex medical jargon; and while explanations may be given, the response is not always written empathetically or shows that the patients' concerns were listened to. Nevertheless, NHS staff felt that very few complaints were not resolved at the local level, and that even if a patient felt that there may have been negligence, the explanation of what had actually happened was usually accepted by patients.
3.36 Patient support and advice groups also identified several problems: complaints can take a long time to be dealt with; the NHS can be defensive, even aggressive, towards patients who complain; and the process is intimidating, especially for people who are vulnerable. It was argued that the types of complaints patients usually raised such as poor communication, were related to issues not recorded in medical records and that the complaints system is not geared towards recognising these issues. Likewise, a survey of patient dissatisfaction in Ayrshire and Arran found that most criticisms focused on staff being too busy, not being helpful, not understanding admission procedures, and poor 'hotel' services such as meals (Ayrshire and Arran Health Board 1993). Our interviews suggested that NHS staff may dismiss many of these concerns as being 'trivial' and instead only see serious concerns about clinical treatment as 'real' complaints.
3.37 The main problem with the complaints procedure does not appear to be the process of complaining, but patients' reluctant to use the process. A number of studies in Scotland have highlighted that disgruntled patients tend to take no action. For instance, a survey of NHS Scotland patients in 1992 showed that while only 3% of patients felt the need to complain, only a third of these patients actually did so. Patients did not know whom to complain to, they felt that complaining would make no difference, were fearful of retribution, and felt in awe of medical professionals (HMSO 1992). Dissatisfied patients may be reluctant to act out of concern that they will damage their relationship with the doctor (Pleasence et al. 2003), especially if there are no alternative providers (Annandale and Hunt 1998) or patients are concerned that services may be denied (Mori 1997).
3.38 Most stakeholder interviewees felt that the concern about damaging the relationship with the doctor and fear of being unable to find an alternative healthcare provider remain. However patients are increasingly challenging medical professional dominance. They explained that the social hierarchy has started to change and patients are more aware of their rights. This can potentially be seen in the changing nature of complaints. According to stakeholders, complaints in the past focused more on a single clinical event, but were now more complicated with general care and poor communication increasingly being challenged. They also described patients' letters as having greater sophistication and that patients often will have done considerable research on the internet before making a complaint.
Supporting patients through the complaints process
3.39 The majority of pursuers received support from their family or friends to make a complaint and then a claim. One of the problems with the complaints process identified by support and advice groups is that patients are often too ill or feel too vulnerable to make a complaint. It would appear that the support of family and friends is very important in overcoming the power imbalance between patients and the medical profession. The involvement of family members in the medical complaints process has also been noted by other researchers. Several previous studies have suggested that relatives may feel more dissatisfied than the actual patient (Allsop 1994, Annandale and Hunt 1998:125, Lloyd-Bostock and Mulcahy 1994, Mulcahy et al. 1996).
3.40 Several pursuers also stated that they received support from a number of different sources, including Scotland Patients Association (SPA), Independent Advice and Support Service (IASS) and Action Against Medical Accidents (AvMA). They explained that they received help in writing letters. For several pursuers who did not have strong literacy skills, this support was seen to be invaluable. Pursuers also explained that support groups had assisted in asking the 'right questions.' The importance of support and advice groups in providing this assistance was reflected in the interviews with NHS staff, several of whom stated that the letters written by complainants had become increasingly sophisticated (as stated above). They suspected that patients who wrote letters which were focused and asked specific questions had received support from a knowledgeable family member or patient support or advice group.
3.41 Not all complaint letters, however, appear to have been written by people with knowledge of the complaints procedure. Several NHS interviewees stated that it was often very difficult to work out what a complainant wanted and that some letters expressed a vague 'concern.' Some pursuers did not receive any help, and it is these pursuers that seemed to struggle to raise their concerns in a clear manner. For instance, one pursuer had sued after her husband had died, and the legal claim hinged on delayed diagnosis. Once the pursuer's husband was diagnosed he underwent urgent and major surgery, during which he suffered a serious injury. The pursuer explained that she understood that the surgery had been high-risk and that the surgeon had been unlucky rather than careless. However, her complaint focused on the surgery and she did not ask any questions about the missed diagnosis. She felt that she should have asked more questions about this aspect of the claim, but did not realise its significance.
3.42 The complaints procedure requires patients to be provided with an information leaflet which encourages them to seek assistance from a support or advice group. Pursuers, however, appeared to have found these groups somewhat by chance, rather than having followed the leaflet's advice. For instance, they had walked past an advice or support group while in the hospital, and one walked past an office while shopping in a mall. Others found support while searching the internet. While NHS staff could clearly discuss the process of dealing with complaints in terms of what actions they needed to take, no-one raised the need of ensuring that the patient was also supported through this process. They said that patients were directed to the leaflet on the NHS website, but no-one stated that they encouraged patients to seek support. We understand that standard acknowledgements to complaints included advice on the Independent Advice and Support Service established in 2006 but feel that more could be done to ensure that patients seek support.
3.43 This also raises the issue of how potential pursuers are to be informed of any new scheme, and how advice and support groups are to be tied into the process. At the moment, the leaflet seems to have little benefit. The process of complaining appears to work because it is simple and involves multiple pathways (email, verbal, written complaint). Patients, however, do not appear to be locating additional material themselves, and so there will need to be a significant education programme to make patients aware of any changes.
Medical negligence claims
Relationship between complaints process and claiming
3.44 Figure 1 shows the number of closed claims in the CLO data according to calendar years. It should be noted that the year in which the case is 'closed' in this data set is the year in which the claim record was marked as 'closed'. This may differ from the year in which the case settled or when the award was paid.
Figure 1: Number of claims received since 1992
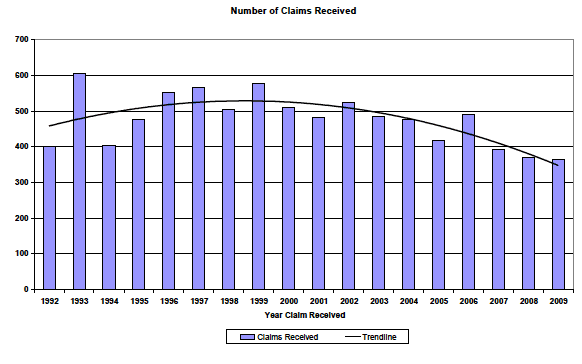
3.45 The CLO data reveals that the number of claims rose during the 1990s but there has been a declining trend since 1999. This is illustrated in Figure 1.
3.46 A few pursuers described the complaints procedure as a mandatory procedure that must be completed prior to making a legal claim. For several, this procedure was described as a hurdle that needed to be 'jumped over' before they could see a solicitor. They felt that the NHS would never admit what had really happened and that their complaint would not be listened to, and so making a legal claim was 'inevitable'. This is not actually the case, and pursuers are entitled to make a legal claim without first having made a complaint. It seemed that some pursuers had been given confusing advice from advice or support groups, and that their expectations that the NHS would refuse to be open about adverse events were given validation.
3.47 In Scotland, complaints and legal claims cannot be run at the same time, although this has recently changed in England and Wales. Pursuer solicitors explained that they may send a patient pursuer back to the complaints process in order to get an explanation and that this may suffice. Several NHS staff disputed the usefulness of sending a potential pursuer back to the complaints procedure, explaining that once someone has decided that they want to make a legal claim they become focused on obtaining financial compensation.
Barriers to claiming
3.48 Our sample is limited to people who have made a legal claim, and therefore were proactive in pursuing their rights. However, very few patients, including patients who have expressed a grievance or gone through the formal complaints procedure make a legal claim (Annadale and Hunt 1998). It may be that this is the case because the complaints procedure satisfies most disgruntled patients and they are happy with the explanation that they received. On the other hand, some patients may not continue with a claim because of barriers to access to justice such as lack of resources, information, or support.
3.49 While the number of adverse events is relatively high in the UK, as well as other jurisdictions (Vincent et al. 2001), the proportion of claims remains very small. This suggests that patients may be reluctant to make a claim. We are unable to provide direct evidence concerning barriers to claiming. However, previous research highlights some potential problems. Following concern about the increasing failure of people to seek legal remedies for 'justiciable' problems (problems with a potential legal solution), Genn and Paterson (2001) conducted a survey in Scotland to investigate what types of legal problems people face and their efforts at reaching resolution. Although the researchers did not analyse data specifically concerning medical negligence, they did find that a relatively high proportion (a third) of people who experienced other types of personal injury requiring medical treatment did nothing. In fact, people who had experienced a potentially justiciable personal injury were less likely to take action relative to any other type of justiciable problem. A follow up study by the Legal Services Research Centre suggests that people who felt that they had suffered from a medical negligence event were significantly less likely to take action relative to other types of problems, except for issues relating to mental health (Pleasence et al. 2006, Pleasence et al. 2003). The main reasons for the lack of action were the injury was minor or the other side had already taken action.
3.50 Genn and Paterson's (2001) research followed an earlier survey in England and Wales which used the same research instruments as Genn (1999). There were some differences between findings reported in Scotland and those in England and Wales. The Scottish respondents were more likely to pursue self-help remedies compared to people living in England and Wales, who were more likely to do nothing. Scottish respondents were also marginally less likely to seek legal help, which may reflect their tendency to try and resolve problems without assistance. Genn and Paterson (2001) also suggest that Scottish people were also less likely to report having experienced a justiciable problem, rather than there being a lower incidence rate.
3.51 Pleasence et al. (2003), however, argue that the nature of legal problems is likely to be significantly different in Scotland relative to England and Wales. They suggest that social and demographic differences, including Scotland's lower population density, greater number of people living in local authority housing and/or in flats, lower personal income and divorce rate, and small minority ethnic population are all likely to impact upon the types of justiciable problems experienced in Scotland relative to England, as well as reporting rates. Their results, however, show that people who are economically inactive, on benefits, and live in the rented sector or in flats, are more likely to experience justiciable problems. This would suggest that Scottish people are more likely to experience problems, and that the difference between Scotland and England is most likely attributable to a reluctance to report.
3.52 Potential reasons for the failure to pursue a claim include believing that there was not a dispute, the other side was right (Genn 1999), nothing could be done, there was no-one to blame, the other side had already taken action, and fear of a defensive response or retribution (Mulcahy and Tritter 1998, Pleasence et al. 2003). Patients are also less likely to sue if they do not know a medical error has occurred, and if they cannot locate or pay for legal representation (Baker 2005, Weiler 1991).
3.53 It would appear that some of the reasons for not making a claim would persist regardless of the nature of the medical negligence scheme, including potential pursuers not knowing that an error has occurred. However, if a scheme was introduced that lifted the potential barrier of finding legal representation, and which was aimed at providing compensation for lower level claims, then it could be expected that some of the people currently deterred would make claims. In addition, if improvements in the way in which errors were reported and disclosed were also introduced, then a further increase in claims would also be expected.
Pursuers' motivations
3.54 Previous research suggests that when an error has occurred, patients expect doctors to make an apology, provide an explanation and take steps to prevent the error from recurring (Allsop 1994, Hickson 2002, Hickson et al. 1992, May and Stengel 1990, Mazor et al. 2004, McCord et al. 2002, Vincent et al. 1994, Witman et al. 1996) To a much lesser extent, injured patients wanted financial compensation (Mulcahy et al. 1996, Shapiro et al. 1989, Genn and Lloyd-Bostock 1995), and compensation is usually discussed in the context of fulfilling a particular need (Genn and Lloyd-Bostock 1995). Our results are broadly similar to previous studies. However, there has been little in-depth consideration of what pursuer's really mean by an explanation, prevention of future errors, apology or compensation. In addition, our results suggest that one of the most important motivations for pursuers' is the desire to have their perception of what had caused the medical injury validated. The significance of validation has not been noted in other research.
Pursuers want their perceptions validated
3.55 The main motivation for pursuers appeared to be the desire for validation of what they believed had happened, which they described as being 'the truth' or 'the real explanation'. These pursuers explained that they had uncovered the real explanation only after thinking through the events carefully afterwards, gradually realising that there were important points at which errors had occurred. They had initially overlooked these 'contributory factors', but in hindsight had come to understand their 'real' significance. For others, the 'real explanation' had been suggested by another doctor, a friend or relative with medical expertise, or they had researched the medical condition on the internet. Some felt that the real explanation was just 'commonsense', especially as there was such a stark contrast between their (or their family member's) healthy state and their eventual state after the alleged error had occurred.
3.56 These pursuers strongly rejected any efforts at an explanation which did not tally with their 'truth'. They felt that medical professionals were a 'closed shop' who denied the truth, and that medical staff were 'telling lies'. Solicitors who did not validate this truth were described as being 'disinterested' or even 'corrupt', and medical experts who provided different accounts were seen to 'lack independence' and to have sided with their medical colleagues. While the pursuer solicitors felt that it was possible to locate appropriate independent medical experts in Scotland, some pursuers considered that it was impossible to obtain independent advice in a small jurisdiction. They cited problems with medical experts turning the case down due to former connections with either the hospital or the doctor who was alleged to have caused the injury. In all of these claims where pursuers were critical of the medical experts, the claim was withdrawn after the medical expert on behalf of the purser agent found that there had not been negligence. For pursuers, it was blatantly obvious that negligence had occurred. However, no-one was prepared to listen to their views. Even some pursuers, who had obtained compensation and seemed very satisfied with most aspects of their claim, still stated that they had not received an adequate explanation.
3.57 Pursuers also appear to cling to opinions that provided any validation, even if the confirmation was only slight, of this 'real' explanation. They described doctors who had suggested that an error had occurred as being 'fantastic', 'understanding' and 'prepared to listen'. One pursuer described a response from the Ombudsman stating that she understood the pursuer's 'disquiet', as suggesting that her views may finally be listened to. Several found validation from support or advice groups.
Need for an explanation
3.58 The majority of pursuers explained that their main motivation for pursuing a claim was the desire for an explanation of what had gone wrong. The only pursuers who did not stress this as their main motivation were the few who had been told from the outset that an error had occurred, and were provided immediately with an explanation and apology. The majority of pursuers had gone through the complaints procedures, and several had also had their claims heard by the Ombudsman. They explained that they had used these processes in an effort to gain an explanation.
3.59 Pursuers' desire for an explanation appears to be linked to the desire to receive validation of their perceptions of what had happened. While pursuers explained that they had received a response to their complaint, they felt that this response had failed to answer their questions. For many pursuers, it does not appear that there was a lack of explanation per se, instead they appear to be dissatisfied with the explanation that was given, and felt that there must be a more accurate explanation which the NHS refused to provide.
Desire to protect future patients
3.60 Pursuers explained that while it was too late to improve their own medical condition, they were motivated by a desire to help others and ensure that medical errors did not occur in the future. For most pursuers, however, in order to do this, they felt that the real explanation had to come to light. For a few pursuers, the desire to produce change seemed to focus on an individual medical professional, although no pursuer stated that they wanted a doctor to be dismissed or prevented from practicing.
3.61 For most pursuers, the best way to ensure that future patients were protected was to bring about systemic change. They wanted medical professionals to pay more attention to the views of patients and to take more care. Pursuers described themselves as "ordinary people" and "wee people", who were up against a powerful and impersonal system, and they wanted an acknowledgment of their importance.
3.62 For several pursuers, systemic change was also related to the need to ensure that the NHS was appropriately resourced. Although we had spoken only to people who had made a claim against the NHS, pursuers also tended to be very supportive of the NHS. Several stated that they no longer had trust in doctors or hospitals, and that they had felt angry and let down. However, they still felt that the NHS was an essential institution, and that change should also consist of providing more resources to the NHS. None of the pursuers could recall being told of any actual changes that had occurred as a result of their claim.
Need for an apology
3.63 Previous research finds that injured patients want an apology which is not simply a matter of saying 'sorry', but is sincere and formal (i.e. in a written format), that is accompanied by an explanation and that the medical professional accepts responsibility (Hickson 2002, Hickson et al. 1992, Mazor et al. 2004, May and Stengel 1990, McCord et al. 2002, Vincent et al. 1994, Witman et al. 1996). If these expectations are not met then patients may feel even more aggrieved (Cohen 2004).
3.64 The pursuers that we have spoken to, however, did not focus on wanting an apology as one of the prime motivations. Some of the few pursuers who had received financial compensation felt that an apology and explanation should have been offered. However, most pursuers did not focus on the provision of apologies. It may be that as pursuers had already gone through the complaints procedure, some had received an apology. Pursuers recalled receiving an apology in writing from the Health Board or specific medical professional involved. Some recalled receiving an apology in person at the time of the injury, as well as during a later face-to-face meeting. Some seemed to believe that the apology was sincere; however, they were not satisfied with the accompanying explanation. They explained that they did not want an apology so much as 'answers.'
Desire for financial compensation
3.65 Most pursuers strongly denied that they wanted compensation and instead were adamant that the only outcome they wanted was an explanation, although not all took this view. A few, explained that while they initially had complained in order to obtain an explanation, after their questions were not answered they had started to focus on trying to gain financial compensation. For these pursuers, the most powerful means by which the NHS could be forced to 'change its attitude' and 'listen to patients' was for the Health Board to risk losing money. For others, compensation seemed to take on symbolic value, with compensation representing an acknowledgment that the pursuer (or a relative) had suffered. These pursuers described themselves as being very traumatised by the medical error, and they felt that their distress should be recognised.
3.66 A few pursuers had also clearly suffered financial loss following the medical injury, and these pursuers explained that they needed the money to cover expenses. In one case, these expenses were significant, and while the case had taken over a decade to resolve, there had been no provision of interim support. In several instances, the pursuer had lost their job as a result of the injury, and so needed financial compensation for economic support. The pursuers who suffered some form of economic loss seemed to appreciate that compensation provided support to assist the pursuer back to a pre-injured state. Others, however, did not appear to appreciate the nature of compensation, for instance, one pursuer described her settlement as "a windfall".
3.67 The relative lack of focus on compensation needs to be treated with caution as these comments may well be tempered with a social desirability bias. It may be socially undesirable to admit to being primarily motivated by the desire to obtain financial compensation. It is impossible to know with complete certainty what motivates pursuers. Several pursuers explained that they did not want to be seen as the type of person who pursues claims for money or would go to a solicitor who was only interested in obtaining a financial outcome.
3.68 Notably, stakeholder interviews and focus groups suggest that social actors with direct contact with pursuers, such as solicitors and support groups, do not believe that the desire for financial compensation is the primary motivation for most pursuers. They argued that a desire for an explanation and an assurance that future problems will be prevented are the prime motivations, although most felt financial compensation may still play a role. In contrast, medical professionals and defenders were more likely to believe that pursuers' primary motivation was compensation.
3.69 Our finding that medical professionals and patient/patient rights groups have divergent views concerning pursuers' motivations is replicated in other research. For instance, Ennis and Vincent (1994) show that doctors' perceive vindictiveness to be the main motivation for clinical malpractice claims. A survey of New Zealand doctors showed that only 11% of respondents felt that patients' complaints were warranted, and just under a third felt that complainants were not 'normal' people (Cunningham 2004b). Cunningham (2004b) argues that these perceptions act as a barrier to institutional learning.
3.70 It may be that the difference between pursuers' and doctors' perceptions can be partly explained by the ways in which medical professionals experience complaints and legal claims. Previous research has shown that medical professionals find the experience of being sued to be very stressful. They experience a sense of betrayal and anger, and do not understand why a patient that they have tried to help has turned against them. To be accused of making a serious mistake leads to a sense of humiliation and medical professionals are fearful of recriminations (Cunningham, 2004a, Charles et al. 1984, 1985, 1988, Martin et al. 1991, Saberi et al. 2009, Shapiro et al. 1989, Ennis and Grudzinskas 1993, Ennis and Vincent 1994, Rosenblatt et al. 1990). Doctors' emotional reactions to claims may increase adversarialism. In a survey of doctors who had been sued, Peeples et al. (2000) found that over half of the respondents responded to being sued with a desire for vindication. Whereas solicitors saw the benefits of settling a case, doctors resisted efforts at resolution outside of court as this implied fault. This point was also raised in interviews with several medical defence organisations, who explained that earlier resolution can be hampered by defendants' desire for vindication or concern that settlement implies fault.
3.71 In our interviews, medical professionals explained that a patient may be harmed out of carelessness, but a doctor would never harm a patient out of malevolence, and that it was perplexing that a patient could not understand this. They explained that patients did not understand the stress caused by a complaint. Several pursuers also described incidences where the doctor alleged to have caused the injury had tried to express their emotions to the pursuer. However pursuers felt that this was inappropriate. These pursuers felt that the doctor was only concerned about their own emotional reaction, and was not willing to listen to what they had to say. Thus, it seems that narrative conflict lies at the heart of a medical complaint or negligence claims. It appears that each side wants the other side to understand what has happened to them. However, neither side is prepared to listen.
Funding for claims
3.72 Funding sources for pursuers' claims were quite varied, with the bulk of pursuers receiving a grant of legal aid, some had legal protection insurance, and several paid privately. No pursuers had been accepted on a speculative fee arrangement. For the pursuers who paid privately, the costs were of a major concern, and most felt that the solicitors' fees and the costs of the medical expert reports were too high. One felt that their initial solicitor had not been upfront about fees and changed to a specialist solicitor whose fee schedule was made transparent. All of the other pursuers explained that solicitors had made them aware of the costs from the first meeting in which some solicitors indicated ways to keep the costs lower. For some pursuers, the focus on funding suggested that the solicitor was primarily interested in obtaining fees.
3.73 Pursuer solicitors explained that the main source of funding was legal protection insurance and legal aid, although not all of the specialists accept legal aid cases. They also explained that the outlays allowed by the Scottish Legal Aid Board (such as the costs of medical expert reports) were more generous once a claim had been established; however, they received much less for initial investigation work. They explained that medical negligence work can accrue high disbursement costs in the form of medical expert reports and advocates' fees, and that after these expenses are paid there is often very little left to pay the solicitor's fees. Legal protection insurance does not return the entire award to the pursuer. Solicitors felt that most pursuers would be satisfied to receive most of the award rather than nothing.
3.74 Several pursuers explained that they had wanted to avoid a 'no-win no-fee' solicitor, as they felt that they and claims companies lacked medical negligence expertise and were primarily interested in obtaining high legal fees. They also felt that these firms would only aim to obtain financial compensation, when they wanted an explanation of what had happened. The specialist pursuer solicitors explained that they did not take on cases on a speculative fee basis, although many potential clients expect them to. The limited size of firms and the smaller number of cases means that Scottish firms have not been able to draw on the same economies of scale as some large English firms. Kritzer (2001) argues that large-scale specialised firms in England have enough reserves to be able to take on high-risk and large, complex cases that would be beyond the resources of smaller, more generalised firms. In the UK, the losing party is liable for the other party's costs, and this has added to the risk of running speculative fee cases. Scottish firms lack sufficient resources to be able to bear these risks.
3.75 The pursuer solicitors explained that one of the largest barriers facing people who potentially have been the victim of medical negligence is finding a solicitor prepared to take on their case. The main reasons for a client being turned away was limited sources of funding and a lack of solicitors prepared and able to take on medical negligence work in Scotland. This problem was reflected in the pursuer interviews, and several pursuers described difficulties in finding a solicitor to take on their case.
Legal specialisation
3.76 The routes used by pursuers to locate a solicitor were quite varied. Some were advised to contact a particular solicitor by an advice or support group. These pursuers seemed aware of the benefits of having a specialist in the field. Others had family members who were solicitors; had researched specialists on the internet; contacted the Law Society; been directed to a particular solicitor by their insurance company; or had asked advice from work colleagues.
3.77 The issue of speciality is important, as there are only six accredited pursuer specialists in Scotland. Accreditation is provided by the Law Society of Scotland. Specialists involved in a focus group explained that there were several non-accredited solicitors who also could be defined as specialists. Nevertheless, this is a tiny proportion of solicitors practicing in Scotland, and all of these solicitors were based in either Glasgow or Edinburgh. The lack of specialisation reflects the relatively generalist nature of Scottish legal practice, and contrasts strongly with England and Wales (Kritzer 2001). Ross (2003:25-27, 35-36) also found evidence that potential pursuers found it difficult to find legal representation, felt that the greater involvement of support and advice groups in Scotland may help to alleviate this problem and recommended that SLAB increase solicitor fees for medical negligence claims.
3.78 The data provided to the research team by CLO includes the name of the firm of solicitors representing the pursuer. Examination of this data reveals that the firms most frequently representing a medical negligence pursuer are not necessarily those containing an accredited specialist. Firms with accredited specialists are ranked second, fourth, sixth, eighth and twenty-second out of the 320 firms whose name is listed at least once in that period. The ten firms with the most cases account for 36% of the claims listed over this period. The firm with the most claims appears in 192 claims and the firm with the tenth largest number of claims has 30. One hundred and sixty firms appear only once in the data base since 2004 and a further sixty-one firms only twice. Thus 282 pursuers were represented by a firm who had represented two or fewer pursuers during this five year period.
3.79 The database also enables us to examine the number of claims handled by firms over a longer period. However, over a longer period movement of solicitors between firms and mergers of firms would render the data less reliable as a measure of 'specialisation'. In the analysis below when considering 'specialisation' we distinguish between the top five most frequently mentioned firms and firms outside the top five.
3.80 A few pursuers had gone to a non-specialist beforehand, and most were clearly unhappy with the representation that they had initially received. These pursuers lived outside Glasgow and Edinburgh, and explained that they had found it very difficult to find a solicitor to take on the case. This is in contrast to their views of the specialised firms they eventually selected. In one case, a pursuer used a 'no win no fee' firm and was pleased with the outcome-both in terms of the settlement and the information the pursuer solicitor obtained for the pursuer.
3.81 Interviews with pursuer solicitors and medical defence organisations also highlighted that having a specialised solicitor has an impact upon outcomes. Pursuer solicitors explained that while the nature of medical negligence law itself may not necessarily require particular expertise, in that it follows the same principles of other areas of personal injury law, specialism is still important. Specialists are better able to find the most appropriate medical experts and advocates. They are also better at knowing when a claim will not succeed, at producing good settlements for their clients, and at selecting claims that need to proceed to court. Significantly, defenders explained that they are more likely to try to settle for a lower amount or to deny a claim if the pursuer is represented by a non-specialist. The data supplied to the research team supports this view: a statistical analysis of claims closed from 1998 reveals that the probability of a claim being repudiated is statistically significantly lower if the pursuer's solicitor is one of the five firms with the highest number of claims during the period. This result holds no matter what the medical speciality involved in the claim is. Defenders also know that the case will not be as well prepared, that the expert report for the pursuer may not be as strong, and that the solicitor will be more likely to fold under pressure. These views have support in previous research, which suggests that specialised solicitors obtain higher awards for their clients (Genn 1987).
4.82 The CLO data has allowed the research team to examine whether there is any statistical relationship between the trajectory of a claim and the experience in medical negligence claiming of the firm representing the pursuer. We use the term 'claim trajectory' to cover a number of characteristics of closed claims. No single characteristic can summarise the 'outcome' of a claim. The outcome has many dimensions. Among those which we examined are: the reason the claim was closed; the length of time between a claim being received and it being closed; whether or not the claim was initially repudiated; and the total of payments made to the pursuer. The statistical analysis undertaken is designed to identify characteristics of claims which appear to be associated with each dimension of a claim. We do not attempt to suggest that there is necessarily a causal connection between these characteristics and the dimensions of claim trajectories, merely a statistical association. We would also stress that the characteristics which we have identified account for a very small proportion of variation in claim trajectories across all claims. Nevertheless, the associations which we discuss below satisfy the normally accepted criteria for statistical reliability.
4.83 The statistical analysis reported upon below uses panel data regression techniques (Wooldridge, 2000) to take account of any effect of the medical speciality to which the claim relates. Consequently, the results reported below correct for any differences in claim trajectories associated with particular medical specialities. However, there may be other characteristics of claims which affect the trajectory of a claim. Thus we must examine the factors which are related to case trajectory in a multivariate context rather than a bivariate context.
3.84 The statistical analysis we have carried out suggests that a claim is more likely to be closed because it has been settled if the solicitors' firm representing the pursuer is one of the five most frequently used law firms. It is less likely to have been initially repudiated if the firm is one of the top five. The claim length (measured as the number of days between receipt of the claim and the claim being marked as closed) is higher if the firm is one of the top five. However the claim being closed because of it being subject to a decree of 'absolvitor' or abandoned is likely to be higher if the firm is one of the top five. There is no statistically significant relationship between the magnitude of total payments (award and expenses) and the firm being in the top five. Whilst this result appears to be inconsistent with the evidence from our interviews, this is likely to be because the connection is indirect. Total payments are higher in those claims which were not initially repudiated but the claim is less likely to be repudiated if the firm is one of the top five.[3] Overall the statistical analysis would appear to be consistent with the subjective impressions of pursuers' solicitors and defenders.
3.85 Some pursuers clearly recalled that their solicitor had been initially careful not to build up the prospects for their case. They described how the solicitor had explained that there was no guarantee that they would receive compensation. Nevertheless, several pursuers who did not receive any compensation were still very disappointed that the solicitor had taken on their case. Some felt that they had been 'deceived.' According to several pursuers, one area in which the pursuer solicitors indicated that they could help the pursuer was to get explanations for their case, and the failure to do so may be a reason for pursuers' frustration. Others felt that their solicitor had not been honest with them from the very start. They explained that the pursuer solicitor had constantly promised that the pursuer would obtain compensation, whereas in the end, they received nothing. Some pursuers also felt that they had been promised 'closure', explanations, and apologies, but none of these outcomes were obtained.
Initial investigation and disclosure of errors
3.86 One of the main distinguishing features of medical negligence cases is the marked information asymmetry between pursuers and defendants (e.g. Bebcheuk 1984, Spier 1992). As a result, pursuer solicitors have to do considerable work upfront in order to assess whether an error had occurred, and then whether the error constitutes negligence. Many claims withdraw after this initial investigation.
3.87 Pursuers generally felt certain that negligence had occurred, although most also explained that they had pursued a claim in order to find out what 'really' occurred. Some pursuers discovered that an error had occurred because the medical practitioner concerned informed them immediately. Others discovered that something had gone wrong after talking to friends who had medical expertise. Most pursuers did not discover what had happened until they accessed the medical reports.
3.88 Previous research has shown that one of the greatest barriers to making a complaint or a claim is not being aware a problem has occurred. Studies show that medical professionals may be supportive in theory of disclosing errors to patients, but are often reluctant to do so in practice. US studies suggest that less than a third of adverse errors are disclosed to patients and their families (Blendon et al. 2002, Soleymani Lehmann et al. 2005, Weissman et al. 2005, Wu et al. 1991) This also appears to be the case in the UK (Schoen et al 2005). Medical professionals are more likely to disclose if the patient is in good health or needs further treatment and less likely if the error was preventable or not serious (Lopez et al. 2009, Schwappach and Koeck 2004). There is no duty of disclosure in any of the UK jurisdictions. This may mean that patients are unaware that an error has occurred.
3.89 There are a number of possible reasons why medical professionals fail to disclose errors: fear of litigation (Berlin 1997, Chan et al. 2005, Gallagher et al. 2003); sense of shame; fear of loss of referrals and registration (Mazor et al. 2004, Wu et al. 1997); worry about threat to reputation (Shaw and Coles 2001); uncertainty about how to report (Bateman et al. 1992, Belton et al. 1995, Lawton and Parker 2002). A number of barriers to disclosure have been identified, including a medical culture of blame and punishment, assumptions of perfection, code of silence (Andrews 2005). Doctors tend to see errors as unfortunate side effects (Schwappach and Koeck 2004), and when they do disclose, they choose their words carefully so that they do not explicitly admit that an error has taken place (Gallagher et al. 2006).
3.90 Medical professionals' reluctance to admit errors does not fit well with patients' expectations. Patients want doctors to acknowledge errors and accept responsibility (Hingorani et al. 1999, O'Connor 2010, Schwappach and Koeck 2004,), to be informed about all harmful errors, not just those that are obvious (Hingorani et al. 1999, Hobgood et al. 2002, Mazor et al. 2004). However, disclosure does not always prevent a claim from arising. Research suggests that once a patient knows that a serious error has occurred, they are more likely to sue (Hobgood 2005, Mazor et al. 2004).
3.91 Several pursuers had accessed their medical reports during the complaints procedure. Some had done so without any help, whereas several had received support from advice and support groups. One pursuer had even engaged an independent medical expert to review the medical reports. The main barrier to obtaining medical reports was cost, and as one pursuer explained, although the cost was only £70 she still struggled to find the money. Most pursuers, however, did not seem to consider that there were any problems obtaining medical reports at this stage. There were no reports of obstruction or delays. Pursuers and pursuer solicitors, however, reported difficulties obtaining medical reports once a claim had been intimated. These problems were described as one of the main sources of delay (see below).
3.92 Some pursuers had obtained medical reports following advice from their solicitor. In some areas of law, solicitors will 'unbundle' the types of services that they can offer, and ask the clients to complete some, or part, of an aspect of the running of a case independently. Unbundling is largely done in an effort to reduce clients' fees and usually only occurs if solicitors are confident that the client has the ability to cope with these tasks. There is little research on solicitors' use of unbundled service. Its use is controversial. Some solicitors are concerned that they will lose control over a case or leave themselves open to negligence claims (Hunter et al. 2000). Here, it appears that solicitors have unbundled the collection of medical reports, although the assessment of the reports was then handed over to the independent medical experts.
Sources of Delay
3.93 For pursuers, one main source of delay was in having to go through the complaints procedure prior to making a claim. As discussed above, several pursuers believed that it was mandatory to first make a complaint. Another delay for pursuers was waiting until they had the emotional energy to handle making a claim. Some explained that they had been too ill or traumatised to act immediately, and in some instances, the pursuer had wanted to wait until the patient died before taking action. Others waited in the hope that the doctor or hospital would respond to their initial inquiries and that this would resolve the problem itself. Pursuers described the process of claiming as being stressful. For people who were already facing difficult circumstances or were also grieving, making a claim added to their sense of trauma. In one instance, this delay meant that the pursuer had missed the limitation date. We did not speak to other pursuers where the limitation date was a problem. Presumably this was because solicitors would be reluctant to take on the pursuer as a client if the limitation date had passed.
3.94 While most claims seemed to settle relatively quickly, several claims involving large settlements, took quite a number of years to resolve. These claims were strongly contested and the pursuers did not receive any interim payments. This left the pursuers in very difficult financial situations. While some ultimately won, they lost their jobs and, in one case, also their home.
3.95 Claim length is one of the characteristics of what we have called above a claim's trajectory. The CLO data on the time between a claim being received by CLO and it being closed is illustrated in figure 2. This shows that the mean (average) length of a claim on this definition rose over the first half of the period but has declined slightly thereafter. The figure also shows the median for each year over the period. The median is the length of claim for which 50% of claims take longer and 50% less. When a distribution is skewed the median is a better measure of central tendency than the mean. As can be seen from the figure the average length of claim is much higher than the median. This indicates that some very long claim lengths are inflating the mean length.
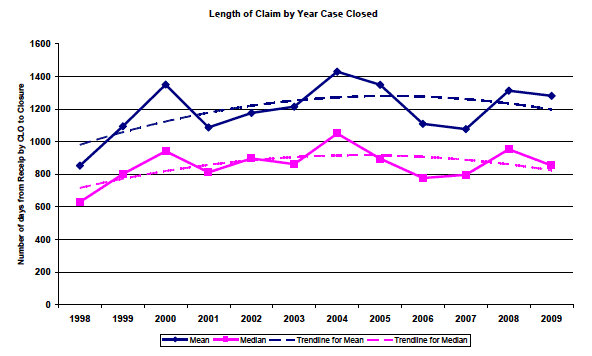
3.96 Figure 2 also illustrates that although the trend in the median over the period is similar to that of the mean the gap between the mean and the median has widened suggesting that over time the distorting effect of very large claims has increased. This is confirmed by examining the relationship between the median and the longest 5% (95th percentile) and 10% (90th percentile) of claims over time. The ratio of the length of the claim at the 90th percentile to the median in 2009 is greater than the ratio between the 95th percentile and the mean in 1998.
3.97 We have carried out statistical analysis of factors which appear to be related to case length (as defined above). We used the panel data technique mentioned earlier to account for the influence of medical specialism. The results indicate that claim length has increased over time, is lower if the claim was initially repudiated, is higher if a settlement was reached, increases with the 'value of the claim' and is higher if the firm acting for the pursuer is one of the five most frequently listed firms. However, we were not able to examine the influence of expert reports in this analysis. The 'value of the claim' is an artificially constructed variable since not all claims are initially lodged with a specific financial value attached to them. The 'value' used here is the higher of the value in the initial claim or CLO's estimated value of the claim when lodged.
3.98 All stakeholder groups explained that delay is often caused by problems in obtaining medical reports, e.g. due to medical staff being on leave, or records being missing. Several pursuers explained that their medical records were incomplete or missing. This clearly led to the impression that the NHS was 'covering up' important information. In one instance, the pursuer explained that it had taken several years for the solicitor to obtain the medical report and when it was obtained the notes had been re-written. We were also told that the CLO tends to wait until claims accumulate and then they are progressed as a group. The CLO advises that this will only occur in 'class actions'. While defenders were not seen to be overly litigious or to deny liability maliciously, it was stated that there are no incentives for the NHS Health Boards to take a more proactive approach.
3.99 This problem may be related to the failure in Scotland to bring in reforms similar to the Woolf reforms in England and Wales, which introduced case management reforms in medical negligence claims. These set time limits by which parties needed to produce responses and progress claims, allow for offers to be made without the admission of liability (Part 36 offers) and ensure the exchange of expert reports. Admittedly, not all of the Woolf reforms have been a success, for instance, the use of mediation appears to still be minimal (Mulcahy 2001). On the other hand, defenders argued that the reforms are not necessary, as there is no incentive to delay a case once a decision concerning whether to accept or refute a claim has been made, settlements are often made without an admission of liability, roundtable discussions and other forms of informal dispute resolution are commonplace, and once the case has reached proof there are opportunities for the exchange of evidence.
3.100 Case management reforms for medical negligence claims were also recommended by Ross (2003:32-39). This Expert Group suggested prior exchange of factual evidence. It appears that this recommendation was not taken up. It was acknowledged that unnecessary delay and expense for straightforward claims had been resolved by the Coulsfield reforms, but that further case management reforms were needed to assist complex cases. In addition, they also recommended that further research was needed into the advantages of mediation for medical negligence.
Claim outcomes
3.101 Only a small number of the pursuers we interviewed were satisfied with the outcome of their legal claim. This result may be, in part, an outcome of the methods we used to contact pursuers. Research which relies on an opt-in response (which we have) is typically biased towards people who are dissatisfied. Only one of the pursuers received an explanation from the legal process with which they were satisfied. Whereas pursuers tended to receive an explanation, apology and assurances of change from the complaints procedure (even if they did not accept these outcomes), the legal process did not produce any such outcomes. A few pursuers received financial compensation which was seen as inadequate in the absence of the other outcomes.
3.102 Pursuers who received compensation were very happy with their legal representation, although some still expressed discontent with the outcome. Most described their solicitor as supportive, hard-working and thorough. However, pursuers who had their claims withdrawn tended to describe their solicitor as disinterested in the case and only interested in obtaining fees. Dissatisfied pursuers explained that they had wanted their solicitor to 'fight' their case, and were sure that negligence had occurred but the solicitor had refused to listen to their story. Some felt that their solicitor had not been honest, that they had failed to gather all the medical reports, and had dropped the case once the pursuer ran out of money.
3.103 Dissatisfaction was also directed toward medical experts. For some pursuers, medical experts were not independent, but instead were engaged in order to provide support to their case. When this support was not forthcoming, they described the expert as having 'sided' with the defendants. As mentioned earlier in the report, two medical experts declined to review files because of their previous affiliation with the hospital or doctor. Whilst this could be viewed as a medical expert being honest about a conflict of interest, pursuers viewed this as medical experts not being able to be neutral or honest.
3.104 For pursuers who were deeply dissatisfied, there was a strong sense of powerlessness and lack of closure. Most had gone through the complaints process, and then the legal process, and at each stage had been told that their narrative of events did not match with that of the NHS. These pursuers insisted that negligence had 'still' occurred, but no-one was prepared to listen. The lack of closure also appeared to be strong in pursuers who felt that questions had still not been answered. They felt that there were answers 'somewhere' but that they were inaccessible to them. Some pursuers explained that their solicitor had stated that their legal case would bring an explanation and therefore closure, when in fact this had not occurred. These pursuers said that they were 'bitter' and 'angry' about 'everything'.
3.105 The outcome of the legal process was, for many pursuers, not the end of the impact that the injury had on their lives. There appeared to be a lack of a sense of closure. Pursuers had lost their jobs, suffered from chronic pain, had their social lives curtailed, were no longer mobile, had lost their independence, or suffered from depression. One person committed suicide as a result of the impact of their injury. Some pursuers expressed a 'niggling doubt' that if they had acted differently, then the injury may have been prevented. Pursuers discussed how they wished that they had spoken up or been more assertive at the time of the adverse event. Some stated that they felt that they were partly to blame, especially if a family member had died.
3.106 It appeared that pursuers' ongoing problems were not well considered within the legal process. No pursuer whom we interviewed had received interim payments, or support to stay in employment, although several did receive physical rehabilitation. Many of the pursuers were obviously grieving and, especially for those who had lost a close relative, the death was described as being inexplicable. None of the pursuers described having been offered grief counselling, and there also appeared to be a lack of support from palliative care.
3.107 As we have explained above claim outcomes are multi-dimensional. We have used the term 'case trajectory' to indicate this. We have analysed the CLO data set to identify those case characteristics which are associated with the elements of a case's trajectory. .
Table 2: Reason Claim Closed 1998 - 2010
| Reason | Number | Percentage |
|---|---|---|
| SETTLED | 2166 | 34.3% |
| ABSOLVITOR/ABANDONED | 1164 | 18.4% |
| REPUDIATION | 994 | 15.7% |
| TIME-BARRED | 455 | 7.2% |
| DISMISSED | 154 | 2.4% |
| OTHER | 1388 | 22.0% |
| of which: | ||
| REFUSAL OF LEGAL AID | 32 | 0.5% |
| NO INSTRUCTIONS | 925 | 14.6% |
| OTHER | 427 | 6.8% |
| GONE TO INSURERS | 4 | 0.1% |
| TOTAL | 6321 | 100% |
3.108 Table 2 shows the number and percentage of each reason given in the CLO data set for a case being closed. The table shows that just over one third of the claims closed since 1997 were settled. We have examined the pattern of settled claims over time. This is shown in Figure 3. The trend over time is for a higher percentage of claims to be closed because they have settled, although there has been a slight decline in the most recent years.
Figure 3: Percentage of Closed Claims Settled, 1998 - 2009
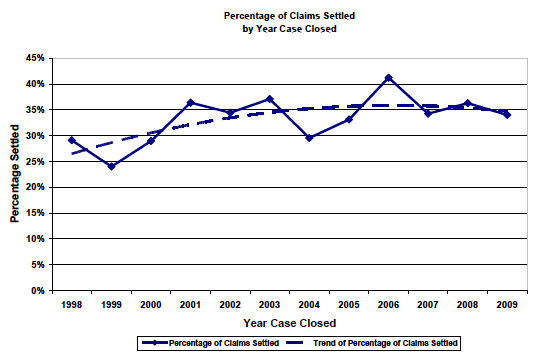
3.109 We have looked at a number of factors which might be associated with the reason the case was closed. These include the medical specialisation associated with the claim, whether the solicitors firm representing the pursuer was one of the five firms who appeared in the data base most frequently during this period, whether the claim was initially repudiated, the financial value of the claim and the length of the claim (measured as the time between receipt of the claim and the claim being closed). We also took account of the calendar year in which the claim was closed. As explained above, the 'value of the claim' is an artificially constructed variable since not all claims are initially lodged with a specific financial value attached to them. The 'value' used here is the higher of the value in the initial claim or CLO's estimated value of the claim at the time it was lodged. There was sufficient information in the CLO data set to allow us to examine statistically the factors associated with the reason for closure for 5,734 claims closed over the period 1998 - 2009.
3.110 The probability of a claim being closed due to being settled: has increased over time; is lower if it was initially repudiated; is higher if the solicitors firm is one of the five most frequently mentioned; is higher the larger the 'value of the claim'. It should be noted that the probability of the claim being initially repudiated has declined over time and is lower if the firm is one of the 'top five' firms.
3.111 These results imply that after other relevant factors (including medical specialism) have been taken into account the higher the 'value of a claim' the more likely it is to end in settlement. In other words, claims with a low implied financial value are less likely to result in settlement.
3.112 We have carried out a similar statistical analysis of the characteristics associated with the other reasons for closing a case. For most of these this shows the obverse relationships from settled claims. A major exception is for those claims which have been marked as closed because a decree of 'absolvitor' has been granted or the case has been abandoned. This has risen over time. The probability of the claim being closed for this reason is higher if the firm is from the top five. This is may be because a claim pursued by one of the top five firms is more likely to go to proof.
3.113 When the analysis is carried out for all non-settled claims except for those granted a decree of 'absolvitor' or abandoned, the results are simply the obverse of those for settled claims.
3.114 Overall this statistical analysis suggests that low 'value' claims are less likely to terminate with a settlement than those with high 'values'. The analysis also suggests that a settlement is more likely if the pursuer is represented by a 'specialist' medical negligence firm of solicitors. It is also the case that these specialist firms are likely to be associated with high value claims. However it should be noted that our statistical analysis cannot distinguish between cause and effect here. It may be that a pursuer is more likely to choose a specialist firm if the claim is potentially of high value but it could also be that specialist firms are only willing to take on claims with high potential 'value'.
3.115 We have also examined whether there is a statistical association between the total payments made on a claim and various characteristics of the claim. The results suggest that total payments: have risen over time; are lower if the claim was initially repudiated; is higher the longer the claim length; is higher the higher is the claim value. There appears to be no direct effect of the pursuer being represented by one of the five most frequently listed firms. However, there is an indirect effect since the claim is less likely to have been repudiated if the firm is one of the five most frequently listed.
3.116 The statistical analysis taken as a whole suggests that a claim's trajectory is influenced by the 'value of the claim' and directly or indirectly by whether the firm representing the pursuer is experienced in medical negligence claiming. One implication of this analysis is that claims with a relatively low 'value' may be better dealt with outside the delict system. However, our interviews with pursuers suggest that this may not resolve the narrative conflict which appears to be at the root of medical negligence claims.
3.117 In the light of the statistical results which suggest that all other things being equal higher value claims are likely to result in settlement and in higher total payments being made we have looked at the differing trajectories of closed claims with either a value less than £20,000 or total payments less than that sum.
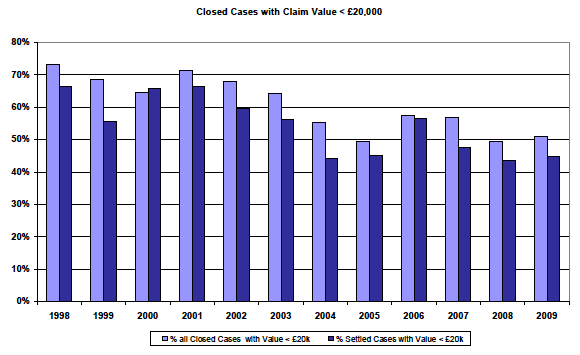
3.118 Figure 4 shows the percentage of all closed claims with a claim value of less than £20,000 together with the percentage of settled claims with a value of less than £20,000. As can be seen in all but one year the proportion of settled claims with a claim value less than £20,000 was below that for closed claims as a whole suggesting that these low valued claims are less likely to settle.
3.119 An examination of total payments (awards plus expenses) made on closed claims using the CLO data base shows that for every year over the period 1998 to 2009 50% of closed claims received no payment. A further 25% of closed claims received payments of less than £10,000. In the most recent years less than 18% of closed claims received total payments of £20,000 or more.
Claim costs
3.120 Data supplied by CLO to the research team has allowed us to examine not only the amount paid out as awards on settled claims but also to examine the costs in terms of CLO chargeable costs and outlays of achieving those settlements. For settled claims we also have data on the cost of outlays awarded to successful pursuers or agreed by CLO. We also have information on CLO chargeable costs and outlays for unsettled claims.
3.121 Figure 5 shows the awards and costs of claims closed for each year from 1998 to 2009. It should be noted that the sums of money plotted in this figure do not necessarily correspond to actual CLO expenditure in these years. The year refers to the year the claim was closed by CLO. Awards and adverse costs are quite likely to be paid out in that year but CLO expenditure on fees and outlays will have been incurred over the life of the claim.
Figure 5: Total Awards and Costs of Closed Claims
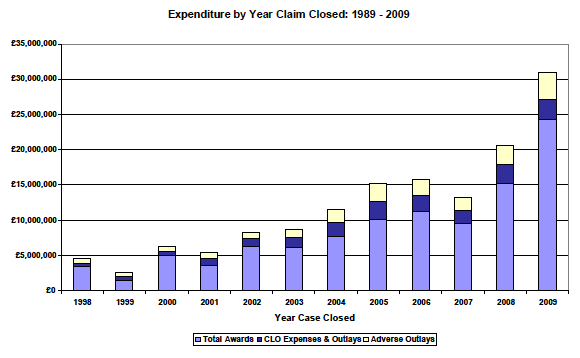
Figure 6: Total Awards and Number of Settled Claims
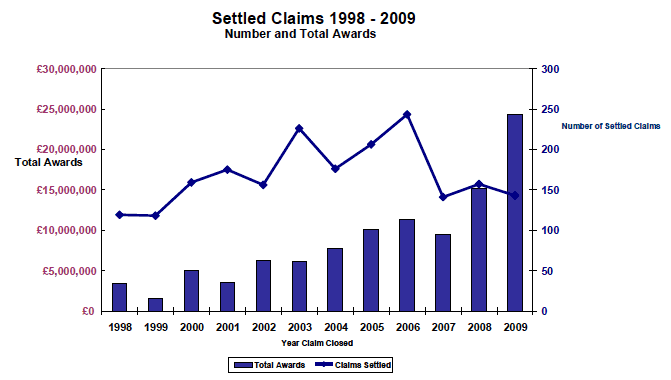
3.122 It is clear from the figure that total awards and costs have risen more or less steadily over this period in absolute terms. The sums quoted, however, are in current prices and have not been adjusted for inflation. As Figure 3 has illustrated only around one third of closed claims in any year have been settled. Figure 6 shows the total of awards and their number for settled claims. Although the value of awards has risen by more than five fold over the period, the number of settled claims 2009 was only slightly above those at the beginning of the period. This of course suggests that the average sum awarded has risen significantly over the period even after inflation has been taken into account.
3.123 Earlier in this report we have shown that the claim trajectories of claims below £20,000 are somewhat different from those above that sum. Figure 7 shows the average award and average costs associated with settled claims where the total award was less than £20,000.
Figure 7: Average Award, Costs and Expenditure for Settled Claims with Award below £20,000
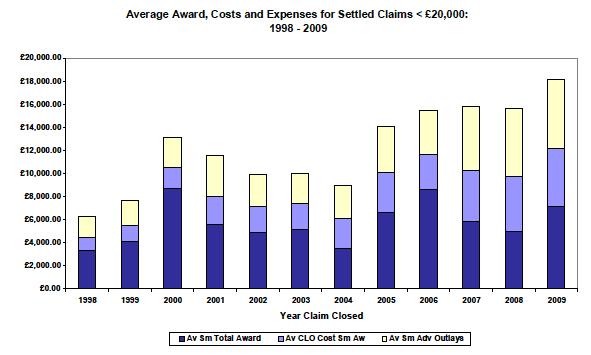
3.124 The average award in these settled claims has fluctuated over the period and at the end of the period was slightly higher than at the beginning. However, the chargeable costs and outlays to the CLO have risen quite significantly as have the sums paid out in adverse costs. Indeed the latter two items taken together are on average higher than the award. This is illustrated in Figure 8. In recent years costs have been much greater than the awards made for these low value awards.
3.125 In addition to the costs of settled claims CLO incurs costs for chargeable costs and outlays in claims that are not settled. On some occasions CLO will make a payment to the pursuer for fees incurred by the pursuer even where the claim is not settled. The total of the costs for unsettled claims is shown in Figure 9. These costs have risen over the years from around £300,000 to over £1M. This analysis is unable to estimate the costs to pursuers of unsettled claims where the NHS Health Boards do not make a contribution.
Figure 8: Average Cost as a Percentage of Average Award for Awards Below £20,000
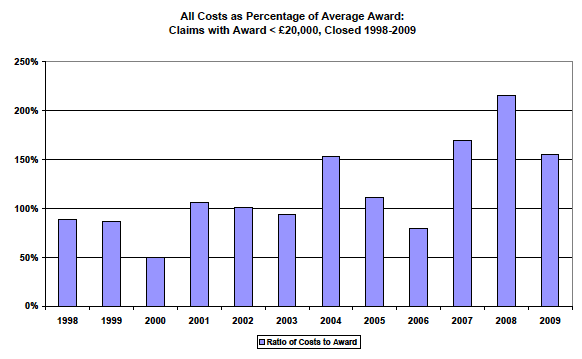
Figure 9: Costs of Unsettled Claims
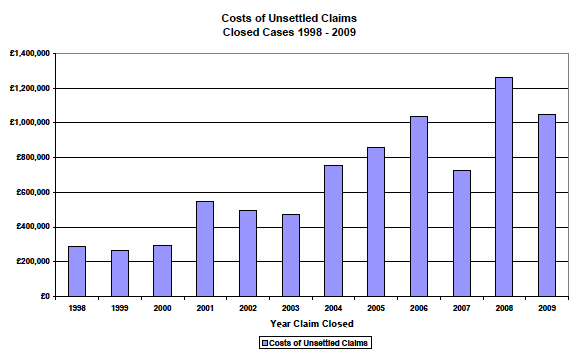
3.126 This brief survey of costs indicates clearly that significant costs are incurred for unsettled claims and that the costs associated with small claims have been rising and currently are greater than the awards made.
Potential impact of an alternative scheme
3.127 Most pursuers felt that improvements to the current system must be made. There was a clear preference from them for a 'no-fault' scheme, although the limits of such a scheme were obviously not appreciated. There was very little support from across most of the other stakeholders for an alternative scheme.
3.128 Pursuers suggested that the NHS should listen more to the views of patients. Several emphasised the importance of doctors or the NHS following through with their communication with the patient. They also felt that more should be done to ensure that patients (and their relatives) receive adequate explanations, apologies and compensation. Some pursuers who had received a negative medical report also expressed the need for an 'independent' expert, suggesting that all medical professionals regardless of their relationship with the NHS are involved in a 'closed shop'. It seems that some pursuers will see experts from outside the NHS as being independent, but that was not the case for all pursuers. Some pursuers clearly felt that every avenue to dealing with a grievance, from making a complaint, going to the Ombudsman and then making a claim was too connected to the NHS.
3.129 Almost all pursuers who did not obtain an award explained that their claims had failed because negligence is 'too hard' to prove. Most felt that an alternative scheme should lower the bar against which negligence should be proved. Many pursuers felt that they should have been entitled to some form of financial compensation, and wanted recognition that they suffered distress and that their lives had been adversely affected. They felt that a 'better' scheme would provide 'fairer' compensation, meaning that they would have received the compensation to which they felt they were entitled. Some were also clearly puzzled that they had received nothing, especially in claims where the doctor had admitted that they had made an error and had encouraged the patient to pursue a legal claim. For these pursuers, the doctor had 'admitted liability', and so they should be guaranteed financial compensation. It would appear that pursuers consider that a no-fault scheme would automatically entitle any patient who has suffered an injury to financial compensation. Pursuers were not able to make distinctions between liability and causation, or in lay terms, negligence and a medical error. Having a medical professional admit liability was seen to be sufficient to show negligence.
3.130 Our analysis of the CLO data on closed claims suggests that the vast majority of claims result in either no payments or only relatively small sums. Indeed, almost half of recently closed claims had an estimated claim value of less than £20,000. The number of those which are closed without being settled suggests that payment of an average of £5,000 would increase annual expenditure by significantly less than £500,000. However, our analysis is not able to estimate whether the number of such claims would rise.
3.131 Most medical practitioners expressed concern about the potential costs of a scheme, worrying that resources could be diverted from front-end staff to cover a rise in claims. They acknowledged that the complaints mechanism was not perfect, but it offered timely resolution that satisfied the majority of patients. It was not clear to many interviewees how an alternative scheme would be different from the existing complaints system. There was a strong opinion that pursuers were primarily motivated by compensation, and that an alternative scheme would encourage a 'flood' of financially-motivated claims. Most pursuers had intimated a claim as they felt that there had been a breakdown of communication, medical staff had been dismissive or arrogant, and general care had been poor. They felt that these concerns were not addressed within the legal process. It is unlikely that these issues will be addressed by an alternative scheme.
3.132 Practitioners and interest groups with direct experience of claims mostly felt that there were some advantages to the legal system. Some felt that solicitors helped pursuers take on realistic expectations, and would not push unmeritorious claims. Their removal would potentially limit the types of 'sensible' advice being provided to pursuers. While interviewees may have acknowledged the potentially useful role of pursuer solicitors, most also considered the legal process to be adversarial, time-consuming and very rarely producing good outcomes for pursuers. Most interviewees felt that pursuers did not really want compensation, and those that wanted compensation were considered to be opportunistic and 'greedy'. There was acknowledgement that some pursuers may have a genuine need for financial assistance, especially those where a baby had been brain damaged. For the most part, defenders and practitioners seem sceptical about pursuer motives.
3.133 It was felt by the majority of stakeholders that any effort to cap a scheme would be unacceptable to Scottish patients and would face strong resistance. There was strong opposition for a New Zealand style 'no-fault' scheme, in that it would set unrealistic expectations. There were also concerns about the lack of independent review, caps on awards, and the overall costs of the scheme. Almost all interviewees felt that any new scheme should add to patients' rights, rather than limit their entitlements. There was also strong opposition to any scheme that would be expensive to implement and run. Concern was raised about implementation costs such as the need to educate complaints managers and other NHS staff, to link in with support and advice groups, and to raise awareness with patients and their families.
3.134 One suggested alternative which appears to already be working in a rather ad hoc way is the reimbursement of costs incurred rather than compensation. Several IASS advisers and NHS managers stated that if a patient could show that they needed equipment or had directly incurred other expenses as a result of an injury, and that these costs were relatively low and 'reasonable', the patient could receive reimbursement. Not all Boards were prepared to do this. It appeared that claims were considered on an ad hoc, case-by-case basis. The willingness of the Boards to reimburse was not formalised or advertised. This system does not provide pursuers with the additional independent investigation which they hope would give them the explanation not provided by the complaints procedures. Ross (2003:30) noted that NHS Boards had the power to make ex-gratia payments to complainants to cover relatively small losses, however, they expressed disappointment that such payments were rarely used.
3.135 This is similar to the current system of reviews and panels in Wales Patients unsatisfied with efforts at local resolution made through the complaints process can go to an independent review or panel made up of independent lay persons, who are informed by independent clinical assessors who are not members of the panel. The reviewer and the panel have the powers to award 'modest' financial compensation. An unhappy patient can take a claim to the Ombudsman (or go directly to the Ombudsman). This system has not replaced the option of pursuing a legal claim. It was viewed favourably by several advice and support groups.
3.136 This system has some features in common with the office of the Health and Disability Commissioner (HDC) in New Zealand. The HDC resolves complaints by referring to the ACC, other appropriate agencies, or directly to the practitioner involved, calling for a mediation conference, conducting further research, or conducting a formal investigation. It draws on the services of independent advocates and an independent prosecutor (Farrell et al.,2010).
3.137 These systems provide for greater independent investigation, and may assist people who would otherwise sue in order to get answers. They are able to provide a range of outcomes, including investigation, explanations, apologies, and financial compensation. In Scotland available outcomes differ between the complaints procedures and the legal system. The systems in Wales or New Zealand do not require proof of liability or causation. Therefore non-negligent events and patients' non-clinical concerns can be addressed. In New Zealand, claimants have no right to legal redress. In Wales, the legal route remains an option. There has been some criticism of the HDC.
3.138 Ron Paterson, the former New Zealand Health and Disability Commissioner, has warned that:
…emerging evidence shows that complaints are not necessarily the treasure trove that quality improvement gurus would have us believe. Instead of providing reconciliation and closure, complaints can have toxic effects on patients and doctors, and may perhaps more accurately be described as 'toxic treasure' (Paterson 2004:1).
3.139 A 2001 review of the HDC complaints system shows that patients found the process to be confusing, cumbersome, difficult to access, and has high emotional and financial costs. A review in 2004 showed that 80% of providers were satisfied with the service compared to 46% of complainants, suggesting that HDC may be one-sided. There have been efforts to address some of these concerns: a single point of entry; greater capacity for mediation; greater flexibility to refer back to the provider for resolution (Paterson 2004).
3.140 Support and advice groups in particular felt that the Working Group should not lose the opportunity to bring in radical change. However, calls for change from other stakeholders tended to be more modest. This group made suggestions such as: funding for legal claims needed to be improved; reforms akin to the Woolf reforms should be implemented; mandatory reporting of adverse events should be introduced as well as a duty of disclosure; and that there be better mechanisms to collate data in order to ensure systemic learning.
Contact
Email: Fiona Hodgkiss