Self-directed Support: Practitioners Guidance
A practice guide on Self-directed Support for practitioners
Assessment
The Act is clear in relation to individual’s participation in their assessment. This is more than ‘consultation’. Whilst assessment is currently a legal duty for local authorities, this duty involves enabling people to co-produce their assessment if they so wish. This also extends to NHS partners involved in the assessment or who are contributors to the assessment and plan.
Legislative framework that guides practice around assessment.
- Section 12a of the Social Work (Scotland) Act 1968 – provides the legal basis for all community care assessments for adults.
- Section 22 of the Children’s (Scotland) Act 1995 – provides the legal duty to safeguard and promote the welfare of ‘children in need’.
- Section 23 of the Children’s (Scotland) Act 1995 – provides the legal duties in relation to children affected by disability.
- Section 24 of the Children’s (Scotland) Act 1995 – provides the duty to conduct carer’s assessment for carers of disabled children.
- Section 12aa of the 1968 Social Work (Scotland) Act states we have a duty to offer assessment to carers.
Exploration of the person’s needs and outcomes under self-directed support – background information
Assessment presents an opportunity to engage the individual and other key people involved in reflecting on what matters to them in their life, and also why these things are important (the outcomes) as well as challenges faced and opportunities to address these. The main focus in assessment until recently has been on individual needs. As needs are usually linked to eligibility criteria, which are used to determine whether the person’s needs call for provision of services, there is still a requirement to identify needs as well as outcomes. There can be a challenge to make this distinction. Often a factor identified by an individual as being important to them can be understood as both a need and outcome. However, the outcome should always answer the ‘so what’ question.
Although distinguishing needs and outcomes can be challenging, it may be necessary to do so in the context of eligibility criteria. In this context, it might be helpful to understand outcomes as clarifying direction and purpose, while needs can be interpreted as barriers to achieving those outcomes. An example might be that an individual wants to feel more confident about spending time with their peers (outcome) but they have lost confidence due to difficulty with walking following a car accident (barrier or need). It may be that the individual is beginning to experience symptoms of depression due to isolation and that failure to support the outcome of spending time with peers may exacerbate deteriorating mental health (risk).
In almost all cases, the assessment provides an opportunity for individual participation in decision-making and should involve consideration of the role the individual wants to play as well as the role of other people, supports and services. In adult services, the focus on outcomes is therefore consistent with a range of health and social care policy drivers which promote participation and support independence, including recovery, re-ablement, an assets approach and supported self-management. For children and young people, this approach is consistent with GIRFEC and the SHANARRI wellbeing indicators. For unpaid carers, it is consistent with the Carer’s Strategy.
Assessment may act as the starting point for development and improvement in an individual’s life. Alternatively, it may support a person to maintain the ‘status quo’, to slow the rate of deterioration or to ensure that any decline in a person’s situation is well managed. Individuals’ needs and outcomes can change over time, even over relatively short timescales. The assessment should respond to changing circumstances and needs, and changes during the course of the person’s life.
Good assessment practice and personal outcomes
An outcomes focused assessment is in tune with the general principles within the 2013 Act. It also fits with relationship based practice in particular and with the ‘exchange model’ which emphasises the collaborative nature of assessment, showing how the views of the person, carer, assessor and agency are brought together to negotiate, agree and record outcomes. The agency perspective acknowledges the need to operate within statutory, governance, duty of care and budgetary factors. Otherwise, while the range of individuals whose views are included may vary, it is critical within this model that the person’s views are represented. Although developed in relation to adult services, some of the principles apply to children and families, including the need to use the best possible sources of information available, and to consider the views of key people involved, to negotiate and identify outcomes. Although not emphasised within the model this should involve the views of other professionals as appropriate, particularly with reference to GIRFEC. It may not always be possible to agree on all outcomes. Recording differences can help with clarification and can support reflection and negotiation in the longer term. See Figure 1 below for an illustration:
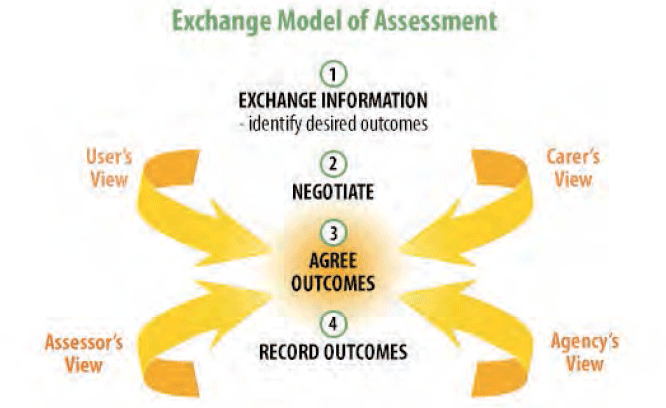
An outcome is generally understood as a result or effect of an action. However, it is also critical that the individual is involved from the outset in identifying the outcomes that are important to them. There are different understandings of outcomes in operation. For example there are national outcomes such as ‘we live longer, healthier lives’ and there are organisational outcomes which could include ‘improved ability to self-manage’. Personal outcomes are the things that matter to the supported person, and require an understanding of why these things matter to them.
New duties – assessment processes
Referral
People engage with services for a variety of reasons and circumstances. For some, they will be seeking advice and information that can be best supported through good initial communication, information and signposting. Often, referral for social work support will not be initiated by the person themselves. Clear information needs to be given to both the person and the referrer about the purpose of any involvement as well as the legislative framework which is guiding involvement in someone’s life.
The duty to provide information at this stage currently exists under Section 12 of the Social Work (Scotland) Act 1968 and the NHS Community Care Act 1990.
Dermot’s story
Dermot, aged 51, has had a long history of recurring depression and anxiety for which he receives medication. When Dermot was feeling unwell he abused alcohol. Eventually, his health deteriorated further, he was admitted to hospital and formally diagnosed with schizophrenia. Dermot was later discharged to the Community Mental Health Team and allocated a Mental Health Officer. At this point, he was encouraged to consider support as there were concerns about him refusing his medication and abusing alcohol. Initially Dermot did not like the thought of having a Mental Health officer and the thought of any further ‘assessment’ for support heightened his anxieties as he knew it might mean being asked very personal questions about his personal life and family. The Mental Health Worker recognised this fear and established a relationship through fully explaining the purpose of her involvement, being sensitive to his situation, and going at a pace that Dermot felt comfortable with. Through on-going conversations, Dermot felt reassured by this. He was also assured by her knowledge and experience of working with people who experience poor mental health.
Dermot found it hard to make decisions or even think about his future, it was something he found very hard to think about in any shape or form, let alone on an aspirational level. Dermot had spent many years just trying to survive so the concept of identifying personal outcomes was difficult. Dermot’s Mental Health Officer understood this and supported him to take small steps, firstly by giving him choice about when and where they would meet, moving on to talking about the things that were important to him but small manageable chunks and at Dermot’s pace.
Following many conversations Dermot started to recognise that there were important things that he hadn’t been able to think about for a long time. Dermot wasn’t really sure about what having support meant or what it would look like so time was spent fully explaining this, how it would be planned and who else might need to be involved. The Mental Health Officer advised of how Dermot’s support could be something he could have choice and control over himself and fully explained some options. It took Dermot some time to get his head around this, however, he felt safe to ask questions about what different options might look like and mean. He also found it helpful reading through information about how to direct your own support, particularly examples of people’s stories about how they planned and used support. Through on-going conversations, Dermot identified that he wanted a hobby, to make contact with his family, and to be able to go out of his house with confidence (personal outcomes). He decided he would like his Mental Health Officer to arrange his support, as he wasn’t ready to take the step to handling a budget. However, he still wanted to be fully included in all aspects of the support planning – identifying an agency to provide a support worker.
Dermot was able to advise on the kind of personality and qualities he valued in a support worker. Dermot was able to identify small goals and work through how these might be achieved and who could help. Dermot found it helpful to know that whilst his plan was agreed and the support put in place, it didn’t have to be ‘set in stone’ and if things did deteriorate he could ask for it to be looked at again.
The assistance and information given to Dermot at a level and pace he understood was crucial in helping Dermot feel more in control about the process and help him develop confidence to make choices important to him. Dermot was also aware that if things did move on in terms of his recovery that he would consider thinking about the agency holding the budget for him or even eventually managing his budget himself.
Initial screening assessment
This concerns the process of determining how to action a referral and what priority is afforded to it. Self-directed support requires skilled practitioners to take a holistic approach to screening, working in partnership with the person to help explore their existing resources and natural and community networks. There are many ways of exploring alternative solutions at an early stage. For example, providng information and helping the person to identify personal and community assets. NHS policy mirrors this approach of self-care and community resilience. Skilled assessment and screening processes may often enable a person to remain independent of formal services.
Self-screening also has an important role, for example, accessing website information, thereby enabling informed choice as to whether or not to continue. This applies to both individuals and families. The principles of participation and dignity underpin all assessment and screening processes.
Duties in relation to assessment
- To undertake an initial assessment with the person, ensuring they are involved in the development of the assessment along with those who matter to them.
- Where it is identified as needed, ensure the person is supported to participate as fully as possible at this stage of assessment.
- The principles of participation, dignity and collaboration apply, along with the stated values.
- The right to participate in society and community and to live with dignity may guide to other solutions.
Issues of choice vs safety will guide decisions regarding further assessment or crisis engagement.
Holistic Assessment
Social work is based on the premise that people can change and that social workers are agents of change. Health and education, along with others, are key partners in ensuring the person remains at the centre of all decision-making.
Holistic assessments consider the person’s assets and wider supportive network, leading to creative solutions that can delay or negate the need for formal intervention. This promotes opportunities for early intervention and preventative solutions through jointly created and alternative means.
- the new Act emphasises the importance of the assessment being undertaken in a manner that ensures the individual feels they have helped shape the assessment rather than be a passive party in the assessment.
- the importance of assessment based on personal outcomes is acknowledged, identified through genuine partnership.
- people should be considered experts in their own lives – therefore staff need to work in partnership to explore and agree solutions and to mitigate risks together.
- where there is risk, the principles of self-directed support still apply but must be explored from a protective perspective. When providing a service/support for children, protecting them from harm remains the paramount concern. However, there is a need to understand and balance any risks and consequences of proposed actions.
- crisis situations can present challenges in considering the consequences of various options for the delivery of self-directed support. It should also be remembered, however, that change can be more possible at times of crisis. As with all cases, professional judgment should be applied.
- when a person is considered not to have capacity/capacity is diminishing – appropriate information and support should be provided to enable participation, with due attention given to risk factors in the assessment and planning activities.
The ‘Talking Points’ Approach developed by Miller and Cook 2012, (http://www.jitscotland.org.uk/resource/talking-points-personal-outcomes-approach-practical-guide/) suggests it is helpful to explore the following areas during assessment:
- being as well as possible
- improved confidence
- having friendships and relationships
- social contact
- feeling safe
- living independently
- being included
When undertaking assessments with children, practitioners should be guided by the Wellbeing Indicators (Often known as SHANARRI):
Safe • Healthy • Achieving • Nurtured • Active • Respected • Responsible and Included
Barbara’s story
Barbara is an Independent single woman who in her mid-70s was working as a volunteer in a university.
She has no family but lots of friends and church activity, as well as a volunteering role and is in adult continuing education.
In a fall, she sustained a severe brain injury; this resulted in – loss of capacity, loss of daily living skills, loss of mobility and loss of choice.
All of this was confirmed in a traditional deficit-based assessment in hospital which led to a care home placement plan. This was entirely appropriate, eligibility clear, but not what Barbara had ever thought would happen and this impacted on her motivation and sense of self.
Barbara’s Hospital Report
- Barbara mobilises with a walking frame but has no recall on how to use her walking frame as a result of cognitive impairment
- Barbara requires supervision from staff to ensure that she is using a walking frame safely as she is at risk of falls
- Ward staff advised that there are times during the night when Barbara gets up to go to the toilet and forgets the location of the toilet or her bed.
- Barbara has expressive dysphasia
- Barbara requires support with speech, reading and writing
- Barbara requires prompts with all activities of daily living
An outcomes focused assessment using Talking Points themes to guide it, developed an alternative and longer-term goal which in turn changed the support plan.
Outcomes support planning using a talking points themed conversation had an immediate impact on helping Barbara feel there was something now worth working toward. Her outlook changed and it was identified that Barbara wanted the chance to try to move back home eventually. This took time and skills and required a collaborative approach.
A team approach was identified using collaboration and joint planning – mental health officer, social worker, nurse, occupational therapist, physiotherapist, advocate, care home staff. All worked together on a rehabilitation programme. This was monitored and where risks were identified they were explored, explained and planned around.
The first stage was mainly around regaining strength and mobility, and relearning again basic communication skills.
Gradually care home staff stopped doing for and stood back while Barbara was encouraged to relearn self-care skills and eventually cooked her own meals.
Nine months later
Barbra went back to her own home. Her capacity is being monitored by MHO – this is the only formal service. She has a full life with support and encouragement of friends and is learning new skills to help her manage her changed circumstances.
There are no other services – other than a brief intervention when support was requested to assist with house move to a new flat.
Outcomes
For Barbara:
- Chooses to live with some risk
- Is independent
- Is in control
- Has regained a sense of well worth
- Managing her own life and decisions
For authority:
- Positive example of team working.
- Risk is managed
Short term; resource intense – longer term; resource light.
Assessment in relation to carers
The majority of support provided in communities is undertaken by unpaid carers – usually, though not always, by family members. It is good social work practice to work with the person who may require support and their carer(s) to identify intended outcomes and agree how needs will be met. Beyond this, carers have legal rights to have their own needs independently assessed and they may require information, advice and support in their own right. Very often this will be a combination of agreeing what the local authority can provide or facilitate and what support a carer is able and willing to provide.
Evidence suggests that key areas to consider/address with carers in this context are:
- the quality of life of the carer; maintaining health and wellbeing: opportunities to follow own interests; relationship with the person cared for; freedom from financial hardship.
- the quality of life of the cared for person.
- managing the caring role – choices in amount of/type of caring undertaken; ensuring the carer feels informed/skilled/equipped; satisfaction in caring; positive partnership working with services and practitioners.
- the carer feeing valued/respected and their expertise recognised.
- having a say in services that are flexible and responsive to changing needs.
New duties relating to assessment of all carers
- Involvement and collaboration.
- The opportunity, information and support to jointly produce their assessment.
- Ensure language, format and arrangements are appropriate to ensure participation is confirmed.
- Identify personal outcomes and goals; determine if these can be achieved through natural supports and solutions created in partnership with others (agencies, family, informal networks).
- Ensure the principles of participation in society and community are guiding and help carers retain or regain independence when required.
Assesment: Considerations for:
Practitioners
- assessment remains core to the social work task.
- the person or their family should have a clear understanding of the assessment process and knows what happens next.
- the level of assessment undertaken should be proportionate to the needs, circumstances and risks presented.
- the assessment should be informed through personal outcomes and the Wellbeing Indicators (SHANARRI).
- all reasonable measures should be taken to ensure full participation in the assessment including consideration of any assistance required including, if appropriate, access to advocacy, translation support or the use of communication aids.
- the practitioner has a primary role in guiding the conversation.
- it should clearly identify what matters most to the person being assessed and why, thus providing a clear signal as to how the assessment will shape and inform future planning.
- an individual or family’s own strengths and assets will be explored to enable community or family based solutions.
- assessments should clearly evidence the process of collaboration and that thorough networking and information gathering has taken place. Most importantly, it needs to demonstrate that the person’s perspective is reflected and valued.
- the person should ideally have a copy of their assessment and this should be in a helpful format and language.
- NHS practitioners should have an awareness and understanding of the principles of self-directed support in relation to assessment in order to promote collaborative working.
Organisations
- Do your initial screening systems support good early assessment including exploration of risk and, when appropriate, is there clear signposting to other informal solutions?
- Do assessment processes encourage an outcomes based approach?
- Do practitioners have the opportunity to reflect on outcomes based approaches within supervision and within the wider team?
- Do you have information systems that enable you to record intended outcomes and connect them to the subsequent review process?
- How will your pathway or process to self-directed support ensure there is evidence of collaboration with the person?
- Do your current assessment, support planning and care management procedures and processes support the requirements of the Act?
Capacity and assessment
The law assumes capacity for any adult over 16 years unless otherwise assessed. The emphasis should be on the presumption of capacity, providing support and assistance to enable the person to make informed choices. In some instances the supported person would benefit from receiving additional support and assistance to contribute to their assessment. The SDS Act requires practitioners to take reasonable steps to identify people who can assist the supported person, and, if the supported person agrees, to involve the relevant people in assisting the supported person with their assessment. There are a number of organisations, aids, equipment and natural community and family supports that may be able to assist the practitioner in this task.
Incapacity can only be confirmed by an assessment from a medical professional. It is important, during assessment, that practitioners are alert to the potential that someone’s capacity may be impaired. If such concerns arise, there is a legal requirement to consider if statutory measures need to be applied and action taken to protect the person’s welfare, property and financial interest. Families should also be provided with information and guidance in relation to Power of Attorney.
When someone lacks capacity, it is important to remember that this does not necessarily impact on all their decision making. It is crucial that the person is supported to make full use of their abilities in shaping their care and support. Careful consideration requires to be given to a person’s capacity at all stages of the process to properly inform judgments about the extent they are able to make decisions about their own needs and support.
There is some concern that the implementation of the Act could lead to an unintended increase in applications for welfare guardianship for adults in order to be supported to participate in assessment and, if eligible, to access one of the four options. Therefore a clear understanding of duties under the Adults with Incapacity (Scotland) Act 2000 is important for all practitioners undertaking assessment and support planning where issues relating to capacity may be present.
Practitioners should refer to established local procedures and seek the expertise within their organisation.
Contact
Email: Heather Palmer