Scottish maternal and infant nutrition survey 2017
Results from the 2017 Scottish Maternal and Infant Nutrition Survey. This first Scotland-only survey gathered data on maternal nutrition and infant feeding.
2. Pregnancy Planning and Maternal Nutrition
By actively taking steps to prepare for pregnancy, women can improve their chances of becoming pregnant and having a healthy pregnancy. ( R10) The nutritional health of women prior to conception and during pregnancy is known to be important in influencing the growth and development of the fetus. ( R1) In addition, there is growing evidence that a woman's preconception health can influence the longer term health of her infants through childhood and into adulthood. ( R3)
In recognition of the public health benefits of preparing and planning for pregnancy, the Scottish Government has put in place polices which aim to encourage pregnancy planning and promote the adoption of appropriate preconception measures by all women who are trying to conceive. ( R10) A similar focus on the importance of preconception health can also be seen in other areas of the UK. ( R3)
Pregnancy planning recommendations in Scotland
General advice and guidance for women who are planning a pregnancy or who are already pregnant is to eat a healthy and balanced diet, keep fit and active and maintain a healthy weight. In addition to this general advice there are some specific actions recommended for women prior to and during pregnancy: ( R6, R10, R11)
Specific pregnancy planning recommendations:
- Folic Acid - A daily folic acid supplement (400 micrograms per day) should be taken by all women who are trying to conceive and by all pregnant women until the twelfth week of pregnancy. This is recommended to help reduce the risk of neural tube defects ( e.g. spina bifida) in the developing foetus. A higher dose of folic acid may be prescribed for women who have had a previous pregnancy with a neural tube defect or who have a family history of this condition. It may also be prescribed for those who are classified as obese, on medication for epilepsy or who have diabetes. ( R1)
- Vitamin A – Pregnant women should avoid foods and dietary supplements containing high levels of Vitamin A. (Dietary supplements specifically designed for use in pregnancy do not contain Vitamin A).
- Vitamin D – It is recommended that a Vitamin D supplement (10 micrograms per day) be taken throughout pregnancy and whilst breastfeeding. Although some Vitamin D can be obtained through diet and via exposure to sunlight the levels obtained via these means are usually insufficient therefore a dietary supplement is recommended.
- Smoking, drinking alcohol and drug use – women who are trying to conceive and who are pregnant should refrain from smoking, drinking alcohol or using recreational drugs.
The following section of this report provides information on pregnancy planning and the extent to which survey respondents made recommended nutritional and health adjustments both before and during pregnancy. The results in this section are based on responses given by women who completed the antenatal questionnaire. The vast majority of women who responded to this survey (95%) were at least 20 weeks pregnant; 3% were less than 20 week pregnant and 2% had recently given birth.
2.1 Pregnancy planning
As highlighted above, there are positive personal and population health benefits associated with actively planning and preparing for pregnancy. ( R10) However, information to allow health professionals and policy makers in Scotland to fully assess the extent to which pregnancies are being planned or unplanned is not readily available.
- Maternities: In Scotland in 2016 there were 53,898 maternities, resulting in 54,488 live births and 236 stillbirths (4.3 still births per 1,000 births). ( R12,) [2], [3] However, these figures do not include pregnancies that did not reach full term, either through miscarriage before 24 weeks gestation or through termination. It is not known how many maternities were the result of a planned pregnancy.
- Terminations: In Scotland in 2016 there were 12,063 terminations recorded (11.6 per 1,000 women aged 15-44). ( R13) It is not known how many of these terminations were as a result of an unplanned pregnancy and how many were carried out for other reasons.
- Miscarriage: Amongst women who are aware they are pregnant, it is estimated that one in six pregnancies will end in miscarriage. ( R14) However, exact figures for the number of miscarriages in Scotland are not available. Where miscarriages are recorded, it is not known if these miscarriages were associated with a planned or unplanned pregnancy.
To assess the extent to which respondents to the antenatal survey had planned their pregnancy, participants were invited to complete a psychometrically-validated measure of pregnancy planning / intention called the London Measure of Unplanned Pregnancy ( LMUP). ( R15) The measure does not assume that women have clearly defined intentions and allows them to express mixed feelings about pregnancy.
The LMUP consists of six questions, each of which is scored between zero and two depending on the response given. The scores for each question are then summed to give a final LMUP score ranging between zero and 12. Each increase in score from zero to 12 represents an increase in pregnancy planning / intention. Broadly speaking, scores can be categorised as follows:
- 0 - 3: Unplanned
- 4 - 9: Ambivalent
- 10 - 12: Planned
In general, according to the responses to the individual questions that make up the LMUP, the majority of women who responded to the antenatal survey intended to get pregnant (77%), wanted to have a baby (85%), and had agreed this with their partner (81%). However, 35% of respondents reported that they did not take any specific actions to improve their health in preparation for pregnancy.
[Figure 2.1; Table 2.1]
More than three-quarters of respondents intended to get pregnant, wanted to have a baby and had agreed this with their partner.
Figure 2.1: Responses to the six questions that form the London Measure of Unplanned Pregnancy (Percentage of respondents who selected each response in relation to each question).
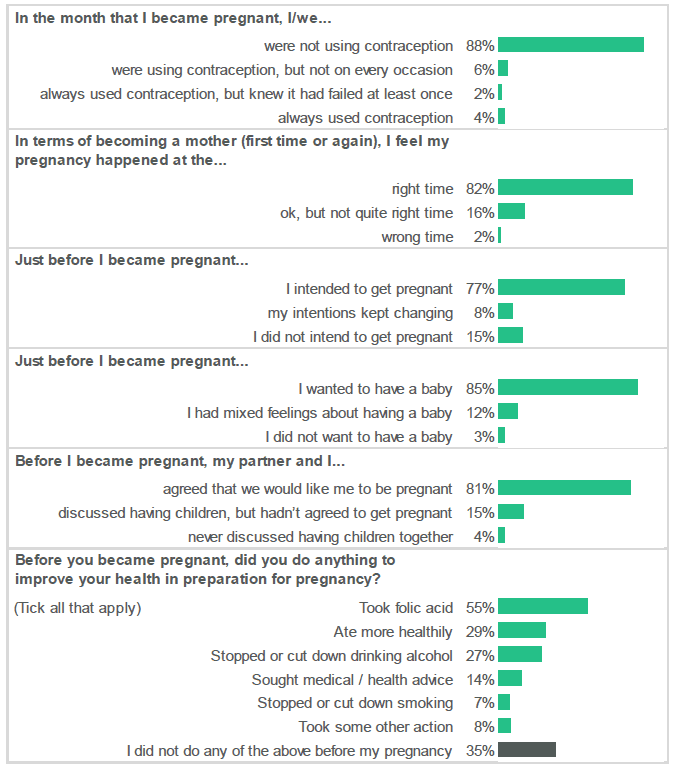
Source: Q5 - Q10, Antenatal Survey
According to the final LMUP scores, 74% of respondents "planned" to get pregnant, 22% were "ambivalent" and 3% of pregnancies were "unplanned". The median LMUP score for all respondents was 11 (Inter-quartile range ( IQR) = 9-12).
[Figure 2.2; Table 2.2a]
According to the London Measure of Unplanned Pregnancy, nearly three-quarters of respondents had "planned" their pregnancy.
Figure 2.2: Distribution of LMUP scores (Percentage of respondents with each LMUP score (0-12)).
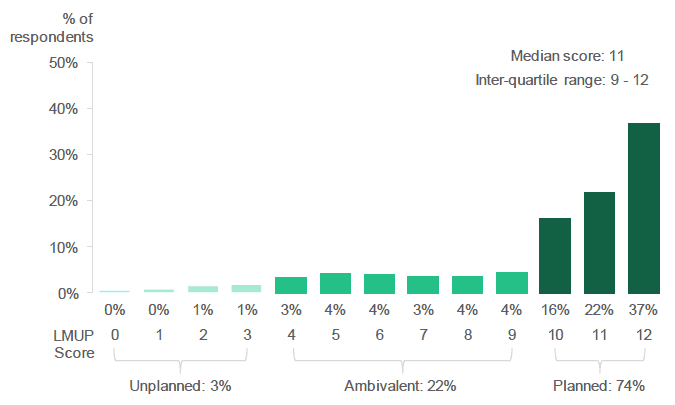
Source: Q5 - Q10, Antenatal Survey
In terms of the distribution of LMUP scores, there was no notable difference between respondents who were pregnant for the first time (median = 11, IQR = 9-12) and those who had been pregnant before (median = 11, IQR = 10-12).
[Table 2.2a & 2.2b]
Please note, previous research that also used the LMUP found that pregnancy planning status varied according to pregnancy outcome. ( R16) This earlier study showed that full term pregnancies were more likely to have been planned than those that ended in miscarriage or termination. It should be noted that the vast majority of women (84%) who responded to the MINS antenatal survey were at least 24 weeks pregnant; this is beyond the point that most miscarriages occur or that termination is an option. This being the case, it is perhaps unsurprising that the proportion of planned pregnancies observed in this survey is relatively high.
Age of respondent
There was some variation in the distribution of LMUP scores across age groups, with older respondents more likely to have a LMUP score indicating that they had "planned" their pregnancy:
- The majority of respondents aged 25 years and over had "planned" their pregnancy, with respondents aged 30-34 the most likely to have done so (86%).
- In contrast, less than half of respondents aged 20-24 had "planned" their pregnancy (46%).
- Respondents aged 19 or under [4] were the least likely to have "planned" their pregnancy (15%). Nineteen percent (19%) of pregnancies in this age group were categorised as "unplanned".
[Figure 2.3; Table 2.2b; Table A1: Antenatal – Results by Age of Respondent]
Older respondents were more likely to have "planned" their pregnancy.
Figure 2.3: Distribution of LMUP scores (Percentage of respondents with each LMUP score (0-12), by age of respondent).
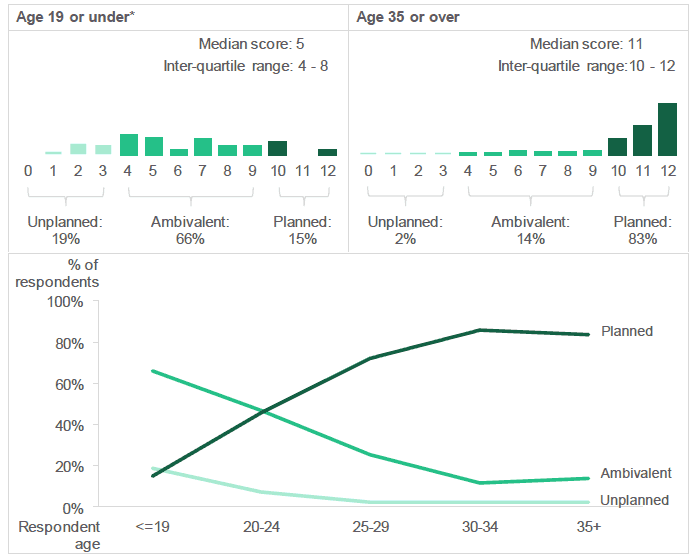
Source: Q5 - Q10 + Q41, Antenatal Survey
Deprivation
There was also variation in the distribution of LMUP scores by deprivation:
- Respondents who lived in the least deprived areas were more likely to have a "planned" pregnancy ( SIMD 5: 84%) than those who lived in the most deprived areas ( SIMD 1: 61%).
- The proportion of respondents whose pregnancy was categorised as "unplanned" was relatively low in all SIMD quintiles, ranging between 2% and 5%.
[Figure 2.4; Table 2.2b; Table A2: Antenatal – Results by SIMD]
Respondents who lived in the least deprived areas were more likely to have "planned" their pregnancy.
Figure 2.4: Distribution of LMUP scores (Percentage of respondents with each LMUP score (0-12), by deprivation).
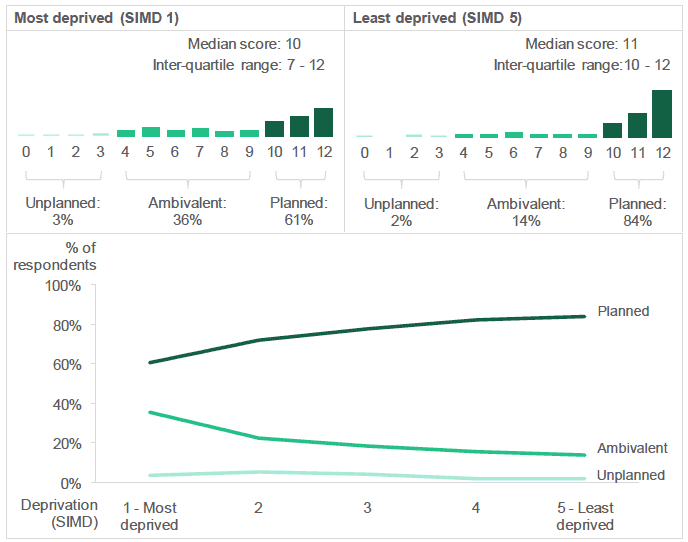
Source: Q5 - Q10, Antenatal Survey
2.2 Folic acid intake before and during pregnancy [5]
It is recommended that women begin taking a folic acid supplement (400 micrograms per day) as soon as they start trying to conceive, and continue to do so for the first 12 weeks of pregnancy. This action is recommended in order to reduce the risk of having an infant with a neural tube defect (for example, spina bifida). ( R11)
Just over half of antenatal survey respondents reported taking folic acid prior to becoming pregnant (53%), with a further 37% beginning to take it as soon as they knew they were pregnant. Nearly one in ten respondents (9%) did not take any folic acid before they became pregnant or in the first month of pregnancy.
[Figure 2.5; Table 2.3]
Just over half of respondents reported taking folic acid prior to becoming pregnant.
Figure 2.5: Did you take folic acid before you became pregnant? (Percentage of respondents who selected each response).
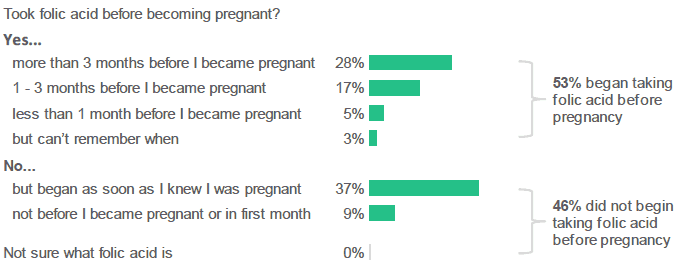
Source: Q12, Antenatal Survey
Age of respondent
Younger respondents were less likely to report taking a folic acid supplement before becoming pregnant.
- Only 6% of respondents aged 19 and under, [6] and 23% of those aged 20-24, reported taking folic acid before they became pregnant.
- Nearly two-thirds of those aged over 30 reported taking folic acid before becoming pregnant (65% of those aged 30-34 years and 65% of those aged 35 or over).
[Table A1: Antenatal – Results by Age of Respondent]
Deprivation
- Respondents who lived in the most deprived areas were less likely to report taking folic acid before pregnancy ( SIMD 1: 41%) than those who lived in the least deprived areas ( SIMD 5: 67%).
[Table A2: Antenatal – Results by SIMD]
High dose folic acid
While all women are advised to take folic acid prior to conception and in the first 12 weeks of pregnancy, a higher dose of folic acid (5 milligrams per day) is recommended for women whose pregnancy is identified at higher risk of experiencing neural tube defects. This may be because the woman or her partner have a personal or family history of neural tube defects, or may be due to medical conditions such as diabetes and epilepsy. ( R11) A high dose folic acid supplement is also recommended for women who are classed as obese. ( R2)
Fifteen percent (15%) of respondents were prescribed a higher dose of folic acid just before pregnancy or in early pregnancy. Three percent (3%) of women began taking high dose folic acid before they became pregnant and 12% after they became pregnant. Less than 1% of respondents were prescribed a higher dose of folic acid and chose not to take it.
The use of high dose folic acid is discussed in more detail in sections 2.5 and 2.8 below.
[Table 2.11]
2.3 Other dietary supplements before and during pregnancy
Currently, there is no specific recommendation that women should take multi-vitamin supplements when trying to conceive. However, it is recommended that women should take Vitamin D supplements during pregnancy and whilst breastfeeding.
Where women do decide to take a supplement it is advised that they avoid taking those containing Vitamin A, including fish liver oils. Dietary supplements specifically designed for use in pregnancy will not contain Vitamin A.
Multi-vitamin supplement use before pregnancy
Thirty-eight percent (38%) of respondents reported taking multi-vitamin supplements prior to becoming pregnant. A further 42% of respondents reported starting to take a multi-vitamin supplement as soon as they knew they were pregnant. Please note, the survey did not ask respondents to specify whether multi-vitamin supplements taken before pregnancy were specifically designed for use during preconception / pregnancy.
[Table 2.4a]
In general, respondents who took folic acid before becoming pregnant (see section 2.2 above) were also more likely to report taking a multi-vitamin supplement pre-pregnancy:
- 65% of respondents who took folic acid before they became pregnant reported that they had taken a multi-vitamin supplement pre-pregnancy.
- Amongst those respondents who had not taken folic acid before becoming pregnant, only 7% reported taking a multi-vitamin supplement before pregnancy.
[Table 2.4b]
Dietary supplement use during pregnancy [7]
More than four out of five respondents (86%) reported that they were taking a vitamin or mineral supplement at the time they completed the antenatal survey. Amongst respondents who were taking a supplement, the majority reported taking them every day (81%) or on most days (15%).
[Figure 2.6; Table 2.5a & 2.5b]
The majority of respondents were taking a vitamin or mineral supplement during pregnancy.
Figure 2.6: Are you currently taking any single vitamin, mineral or multi-vitamin supplements? / How often do you take these vitamin or mineral supplements? (Percentage of respondents who indicated that they were taking a supplement / percentage of respondents who selected each frequency (respondents who were taking a supplement)).
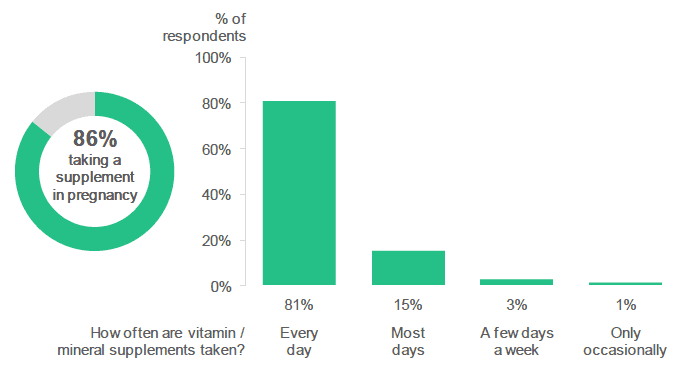
Source: Q14, Q16, Antenatal Survey
Half of respondents (50%) who said they were using dietary supplements, at the time of survey completion, reported taking Healthy Start vitamins. [8] Forty-two percent (42%) reported taking another multi-vitamin specifically designed for use in pregnancy. Fewer respondents reported taking another type of supplement with Vitamin D / Vitamin D with calcium (9%).
A small proportion of respondents (1%) reported that they were taking a multi-vitamin that was not specifically designed for use during pregnancy.
[Figure 2.7; Table 2.5c]
Half of antenatal respondents were taking Healthy Start vitamins when they completed the survey.
Figure 2.7: What type of vitamin or mineral supplements are you taking? (Percentage of respondents who selected each type of supplement. Respondents who were taking a supplement).
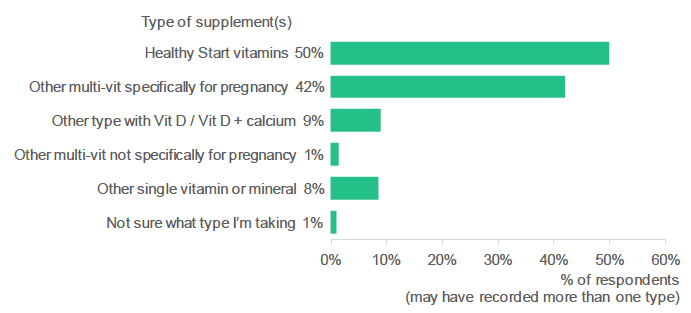
Source: Q15, Antenatal Survey
Eight percent (8%) reported taking another single vitamin or mineral supplement. Iron was the most frequently mentioned 'other single' supplement (5%). Other single supplements mentioned by respondents were Vitamin C, Vitamin D, folic acid and Omega 3.
[Table 2.5c]
2.4 Alcohol consumption [9]
Recently published advice from the UK's Chief Medical Officers regarding alcohol and pregnancy is:
- If you are pregnant or think you could become pregnant, the safest approach is not to drink alcohol at all, to keep risks to your baby to a minimum.
- Drinking in pregnancy can lead to long-term harm to the baby, with the more you drink the greater the risk. ( R6)
To investigate observance of this advice, antenatal survey respondents were asked about their alcohol consumption prior to and after pregnancy. It should be noted that the reliability of self-reported alcohol consumption, particularly during pregnancy, is known to be problematic. ( R17) Women may underestimate or under-report their alcohol intake for a number of reasons.
Alcohol intake before pregnancy
Respondents to the antenatal survey were asked how often they drank alcohol before pregnancy. Over half of respondents (53%) reported never drinking alcohol or drinking it infrequently before pregnancy (Never 14%; Monthly or less 39%).
[Figure 2.8; Table 2.6]
Around half of respondents never drank alcohol, or drank alcohol infrequently, before they became pregnant.
Figure 2.8: In general, how often did you have a drink containing alcohol before this pregnancy? (Percentage of respondents who selected each frequency).
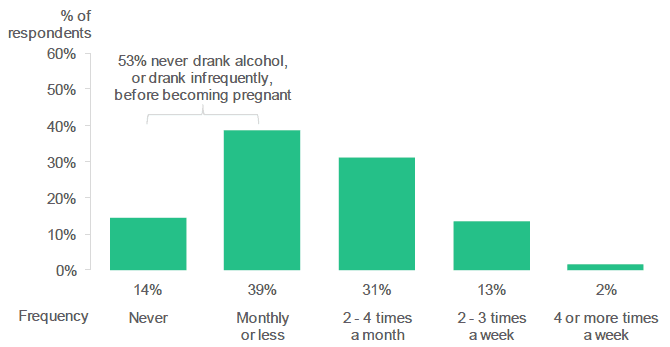
Source: Q28, Antenatal Survey
Age of respondent
Younger respondents were more likely than older respondents to report avoiding alcohol or drinking infrequently before they became pregnant.
- Nearly two-thirds (64%) of respondents aged 19 and under [10] reported that they never drank alcohol (23%) or drank it monthly or less (40%) before pregnancy.
- Less than half (45%) of respondents aged 35 years and over said that they never drank alcohol (13%) or drank it monthly or less before pregnancy (32%).
[Table A1: Antenatal – Results by Age of Respondent]
Deprivation
Respondents who lived in the most deprived areas were more likely to report avoiding alcohol or drinking infrequently before they became pregnant.
- Nearly two-thirds (63%) of those living in the most deprived areas ( SIMD 1) reported that they never drank alcohol (23%) or drank it monthly or less (40%) before becoming pregnant.
- Only 38% of those living in the least deprived areas ( SIMD 5) reported never drinking alcohol (7%) or drinking it monthly or less (30%) before becoming pregnant.
[Table A2: Antenatal – Results by SIMD]
Stopping drinking before pregnancy
Respondents were asked if they had stopped drinking before they became pregnant.
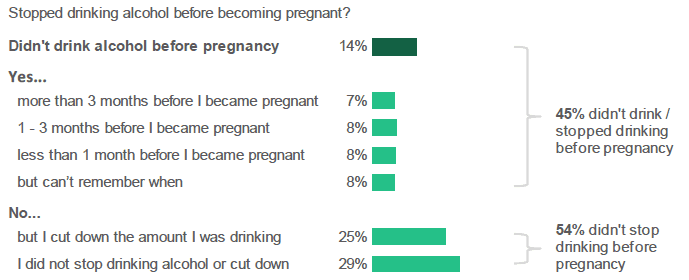
- Forty-five percent (45%) of respondents either did not drink or stopped drinking alcohol before pregnancy. This includes 14% who did not drink alcohol in general before pregnancy and 31% who did drink, but stopped before pregnancy.
- Over half of respondents (54%) reported that they did not stop drinking alcohol before pregnancy, although 25% did say that they had "cut down" the amount they were drinking.
[Figure 2.9; Table 2.7]
More than half of respondents did not stop drinking alcohol before they became pregnant.
Figure 2.9: Did you stop drinking alcohol before you became pregnant (regardless of whether this pregnancy was planned or not)? (Percentage of respondents who selected each response).*
Source: Q28 / Q29, Antenatal Survey
* Note that this analysis includes all respondents, including the 14% of respondents who did not drink alcohol in general before pregnancy (see Figure 2.8 for details alcohol consumption in general before pregnancy).
Alcohol consumption before / after pregnancy awareness
The UK Chief Medical Officers' Low Risk Drinking Guidelines advise that the risk of harm to a baby is likely to be low if an expectant mother has drunk only small amounts of alcohol before knowing she was pregnant or during pregnancy. ( R6) Women are advised that, should they find out they are pregnant after drinking alcohol during pregnancy, they should avoid further drinking.
Respondents were asked about their possible consumption of alcohol in early pregnancy, before they realised they were pregnant:
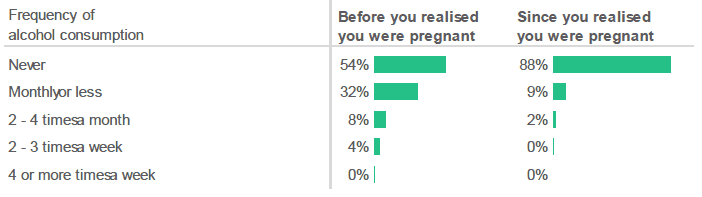
- Just over half of respondents (54%) reported that they had not consumed any alcohol before they realised they were pregnant.
- A further third (32%) had drunk alcohol only infrequently (monthly or less) at this stage.
Respondents were also asked about their alcohol consumption since they realised they were pregnant.
- The majority of respondents (88%) reported that they had not consumed any alcohol since realising they were pregnant.
- However, more than one in ten respondents (11%) indicated that they had continued to drink alcohol after they realised they were pregnant.
[Figure 2.10; Table 2.8a & 2.8b]
Respondents were less likely to report drinking alcohol after they realised they were pregnant.
Figure 2.10: Do you think you drank any alcohol while you were pregnant, but before you realised you were pregnant? / How often have you had a drink containing alcohol since you realised you were pregnant? (Percentage of respondents who selected each frequency).
Source: Q31, Q30, Antenatal Survey
Another recent study undertaken in Scotland also found that most women who drink alcohol stop once they realise they are pregnant. ( R18) However, it also found that the relationship between pregnancy and alcohol consumption is complex, particularly with regard to deprivation. The study showed that while women in a higher deprivation area were more likely to say they sometimes drank alcohol before they knew they were pregnant, women in a lower deprivation area were significantly more likely to drink at least once each week and to drink above recommended levels.
The levels of alcohol consumption reported during pregnancy in the study were also higher than those reported in this survey. However, it should be noted that the methodology used in this survey and in the above mentioned study differed.
2.5 Weight
Body Mass Index
Body Mass Index ( BMI) is a widely used measure for assessing body composition in adults. It is calculated using an individual's weight and height and generally gives a good indication of whether weight is in proportion to height. ( R8)
BMI can be used to classify individuals into the following categories:
- Underweight ( BMI <18.5)
- Healthy ( BMI 18.5 - <25)
- Overweight ( BMI 25 - <30)
- Obese ( BMI 30+)
It is recommended that women should enter pregnancy with a healthy BMI (18.5 - <25). ( R1, R11)
Maternal obesity is associated with poorer outcomes for both mothers and their children. ( R1, R3) Obese women are at greater risk of:
- Early miscarriage and still birth.
- Maternal gestational diabetes and hypertension. There is also a greater risk of their infants going on to develop these chronic conditions.
- Labour, birth and postnatal complications.
- Premature or small / large for gestational age babies.
Conversely, low maternal weight is associated with low birth weight in infants which is also linked to the infant later developing conditions such cardio vascular disease, diabetes and hypertension. ( R1, R3)
The antenatal survey asked respondents to provide their BMI as recorded at their maternity booking visit. This information is usually recorded in a women's hand held maternity record ( SWHMR) [11] . However, one in five respondents (21%) were either unable to, or chose not to, provide this information on their completed questionnaire. The proportion of respondents who did not provide this information was higher amongst younger women and those who lived in the most deprived areas.
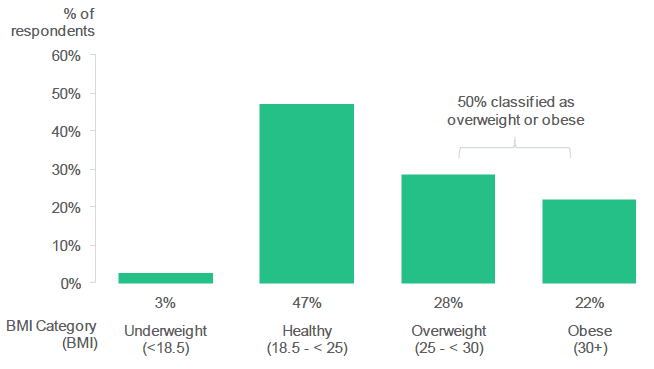
Of respondents who did provide their BMI, half were classed as either overweight (28%) or obese (22%). Only 3% of respondents were classed as underweight with the remaining 47% being classed as being a healthy weight. These figures are similar to routinely published national figures relating to maternal BMI. ( R8)
[Figure 2.11; Table 2.10a & 2.10b]
Amongst respondents who provided a BMI, half were classified as overweight or obese.
Figure 2.11: What was your Body Mass Index ( BMI) at your maternity booking visit? (Percentage of respondents in each BMI category. Excludes respondents who did not specify a BMI).
Source: Q17, Antenatal Survey
Age of respondent
There were no clear differences between age groups in terms of BMI at booking, but this analysis may have been impacted by the disproportionate number of younger respondents who did not provide their BMI.
[Table A1: Antenatal – Results by Age of Respondent]
Routinely collected national data shows that the risk of having a sub-optimal maternal BMI does vary by age. National data for the year ending March 2017, indicates that women aged 19 and under are the least likely to be overweight or obese at booking (35%), whereas those aged 40 and over are the most likely to be overweight or obese (59%). ( R8)
Deprivation
Maternal BMI varied depending on the levels of deprivation in respondents' areas of residence. Amongst those who provided a BMI:
- Respondents who lived in the most deprived areas were less likely to report having a healthy BMI at booking ( SIMD 1: 41%) than those living in the least deprived areas ( SIMD 5: 56%).
- Respondents who lived in the most deprived areas were more likely to have a BMI that suggested that they were obese ( SIMD 1: 27%) than those who lived on the least deprived areas ( SIMD 5: 12%).
[Table A2: Antenatal – Results by SIMD]
Routinely collected national data also shows that the likelihood of having a sub-optimal maternal BMI is higher in areas with the highest levels of deprivation. Official national statistics, based on national data for the year ending March 2017, showed that women from the most deprived areas were more likely to be overweight or obese (56%) than mothers from the least deprived areas (44%). ( R8)
Body Mass Index and high dose folic acid
The Scottish Government's Improving Maternal and Infant Nutrition Framework advises that women who are classed as obese should take a higher dose of folic acid (5mg). ( R1)
Findings from the survey suggest that this advice was followed for some respondents:
- Half of respondents (50%) classed as obese were prescribed a higher dose of folic acid.
- Two-fifths of respondents (40%) classed as obese reported that they began taking high dose folic acid after they became pregnant.
By comparison, only a small proportion of respondents with a BMI classified as healthy or overweight were prescribed a higher dose folic acid (4% and 7% respectively).
Note that no information is available about when the higher dose of folic acid was actually prescribed – only when the respondent started to take it.
[Table 2.11]
Perception of weight
The majority of respondents (61%) described their weight as "normal" before they became pregnant. Three percent (3%) perceived that they were "underweight", 27% thought they were "slightly overweight", while 8% described themselves as "very overweight / obese".
[Table 2.12a]
However, a respondent's own description of their pre-pregnancy weight did not always correspond with their actual weight ( BMI recorded at their booking appointment).
[Figure 2.12]
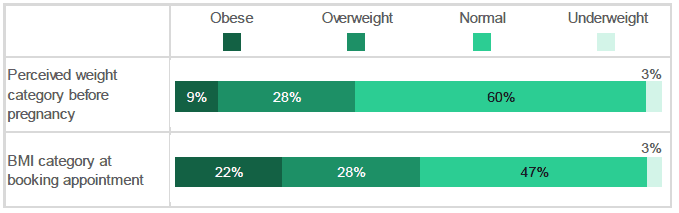
A respondent's own description of their pre-pregnancy weight did not always correspond with their BMI category at booking.
Figure 2.12: How would you describe your weight before you became pregnant / What was your Body Mass Index ( BMI) at your maternity booking visit? (Percentage of respondents who selected each weight category / were in each BMI category at booking. Only includes respondents who provided both their perceived weight prior to pregnancy and their BMI at booking).
Source: Q18, Q17, Antenatal Survey
The majority (94%) of those with a healthy BMI described themselves as "normal", with only a small proportion of this group describing themselves as "underweight" (3%) or "slightly "overweight" (3%). However, amongst those whose BMI indicated they were underweight, overweight or obese there were sometimes a difference between the BMI recorded and the respondent's perception of their weight:
- Only around half of respondents (52%) whose BMI indicated that they were underweight described themselves as "underweight". The remaining 48% described themselves as "normal".
- Half of respondents (50%) whose BMI indicated that they were overweight, described themselves as "normal". Most other respondents (49%) in this BMI category described themselves as "slightly overweight".
- Only 40% of respondents whose BMI indicated that they were obese, described themselves as such. Three percent (3%) thought that their pre-pregnancy weight was "normal"; the remaining 57% described themselves as "slightly overweight".
[Table 2.12a]
Attempts to change weight
Respondents who described themselves as either "slightly overweight" or "very overweight / obese" were more likely to have tried to change their weight before becoming pregnant:
- 61% of those who thought they were "slightly overweight" and 72% of those who thought they were "very overweight / obese" had tried to change their weight prior to their pregnancy.
- Less than half of those who thought they were "underweight" had tried to change their weight before pregnancy (44%).
[Figure 2.13; Table 2.12b]
Respondents who described themselves as overweight were more likely to have tried to change their weight before pregnancy than those who described themselves as underweight.
Figure 2.13: Did you try to change your weight before you became pregnant? (Percentage of respondents who indicated that they tried to change their weight, by respondent description of pre-pregnancy weight).
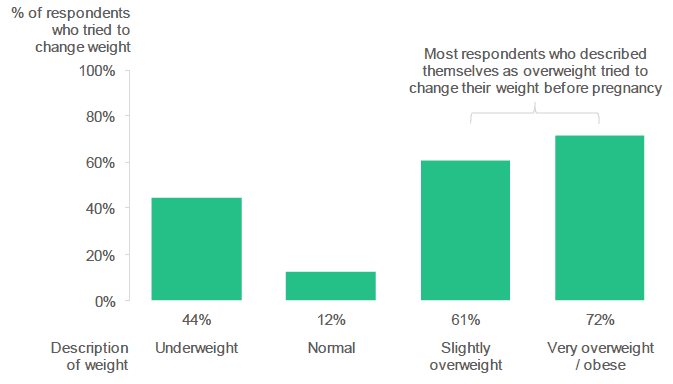
Source: Q18, Q19, Antenatal Survey
2.6 Diet and cooking skills
Women are advised to eat a healthy and balanced diet containing at least five portions of fruit or vegetables a day both during pregnancy and as part of a healthy diet at other times.
Only a quarter (26%) of respondents said that they had eaten the recommended "five-a-day" on every day in the last week (at the time of survey completion). Around half (49%) reported that they done so on between three and six days. A small proportion of respondents (4%) said that they had not eaten the recommended five portions of fruit and vegetables on any day in the last week.
[Figure 2.14; Table 2.13]
Around a quarter of respondents ate the recommended five-a-day or more fruit and vegetables every day in the last week.
Figure 2.14: How often did you eat the recommended 5-a-day or more fruit and vegetables in the last week? (Percentage of respondents who selected each frequency).
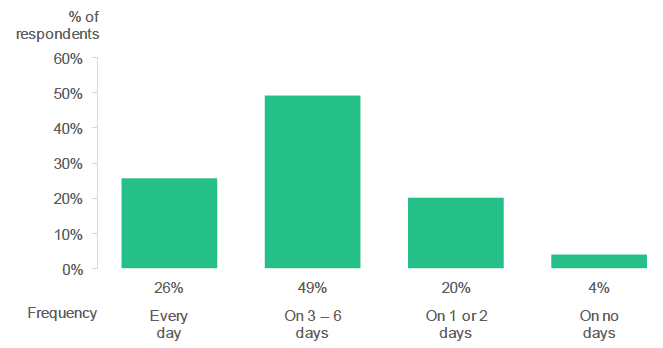
Source: Q24, Antenatal Survey
Age of respondent
Older respondents were more likely to have eaten five portions of fruit and vegetables every day:
- 30% of respondents aged over 35 years reported that they had eaten "five-a-day" every day in the last week, compared to 21% of those aged 20-24 and 20% of those aged 19 and under. [12]
[Table A1: Antenatal – Results by Age of Respondent]
Deprivation
- Nearly a third of respondents (30%) living in the most deprived areas reported eating "five-a-day" infrequently (on only one or two days or on no days). Only 17% of respondents who lived in the least deprived areas ( SIMD 5) reported this.
[Table A2: Antenatal – Results by SIMD]
Change in diet since pregnancy
Over half of respondents (58%) said that they were eating more fruit since becoming pregnant, while over a third (37%) said they were eating about the same amount as before pregnancy. By comparison, only 37% or respondents reported eating more vegetables, with just over half (53%) saying that they ate the same amount of vegetables as they did before becoming pregnant.
[Figure 2.15; Table 2.14]
More than half of respondents reported eating more fruit since becoming pregnant.
Figure 2.15: During this pregnancy are you eating more, less or the same amount of fruit and/or vegetables than you ate before you were pregnant? (Percentage of respondents who selected each response).
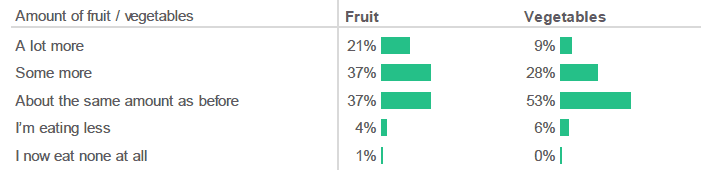
Source: Q25, Antenatal Survey
Types of diet
The vast majority of respondents (86%) reported that their diet included meat, fish and animal products.
- Only 2% of respondents said that they ate a vegetarian diet. A further 2% stated that they were pescetarian.
- Very few respondents (<0.5%) said that they were vegan.
- 8% of respondents reported that while they were not vegetarian, pescetarian or vegan, they avoided some foods. The foods that these respondents most frequently mentioned avoiding were red meat, fish, foods containing gluten and dairy products.
[Table 2.15]
Cooking skills
As described in the MIN Framework, various local initiatives have taken place in Scotland over the last decade to help provide families with practical advice on nutrition, food shopping, budgeting, menu planning and the development of cooking skills. ( R1)
- Two-thirds (66%) of survey respondents said that they could "cook most meals from scratch" and a further 26% reported that they could "cook some meals from scratch".
- 6% of respondents said that they only had "basic cooking skills", but very few (0.5%) said that they "can't really cook any meals".
- Younger respondents were more likely to report that they only had "basic cooking skills". Thirty-four percent (34%) of those aged 19 and under [13] and 13% of those aged 20-24 described their cooking skills as basic, compared to 3% of those aged 35 and over.
- Similarly, respondents who lived in the most deprived areas where more likely than those who lived in the least deprived areas to report that they only had "basic cooking skills" ( SIMD1: 11%; SIMD 5: 3%).
[Table 2.16]
2.7 Pregnancy planning and taking pre-pregnancy actions
The antenatal survey results indicate that women who "planned" their pregnancy (according to their LMUP score) were more likely to take recommended actions before pregnancy. This was particularly evident with regard to starting to take folic acid:
- Over two-thirds (69%) of respondents who "planned" their pregnancy reported taking folic acid before pregnancy.
- Only 7% of respondents whose pregnancy was "ambivalent" and 5% of those where the pregnancy was "unplanned" reported taking folic acid before they became pregnant.
However, around half of respondents who had "planned" their pregnancy did not take some recommended pre-pregnancy actions, such as avoiding alcohol (only 48% did so) or ensuring that they had a healthy BMI (only 48% had a healthy BMI).
[Figure 2.16; Table 2.17]
Respondents who "planned" their pregnancy were more likely to follow pregnancy planning recommendations, but even those who "planned" their pregnancy did not always take recommended actions.
Figure 2.16: Summary of pregnancy planning. (Percentage of respondents who indicated that they had taken a particular action, by LMUP category).
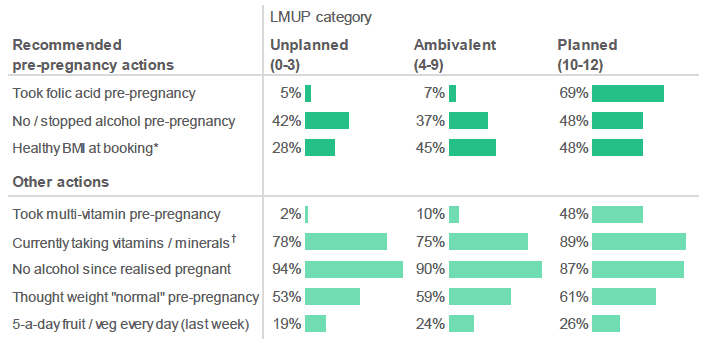
Source: Q5-10, Q12, Q29, Q17, Q11, Q14, Q30, Q18, Q24, Antenatal Survey
* Results for "Healthy BMI at booking" are based on a sub-set of respondents who provided a valid BMI.
† Respondents who had already given birth have been excluded from the "currently taking vitamins / minerals" analysis.
2.8 Previous pregnancy / medical history and pregnancy planning
Previous pregnancy experience and certain pre-existing medical conditions can be particularly relevant when planning for pregnancy. Additional recommendations and advice may be given to women based on their previous pregnancy and medical history ( e.g. increased screening, a change in medication). ( R3)
Nearly half (47%) of antenatal survey respondents reported that they had been pregnant before their current pregnancy. Of those who had been pregnant before:
- The majority (69%) reported that they already had one child.
- A quarter (25%) had more than one child.
- 6% reported that they had no children.
[Table 2.18a & 2.18b]
Situations encountered in previous pregnancy
The majority of respondents (81%), who had previously been pregnant, stated that they had not experienced any issue around birth weight, prematurity or certain specified fetal abnormalities before.
[Figure 2.17; Table 2.19]
Around one in five respondents, who had previously been pregnant, had a previous pregnancy where the baby was over / underweight, premature or had a specified fetal abnormality.
Figure 2.17: Have you had a previous pregnancy where any of these situations applied? (Percentage of respondents who indicated each situation. Respondents who have been pregnant before).
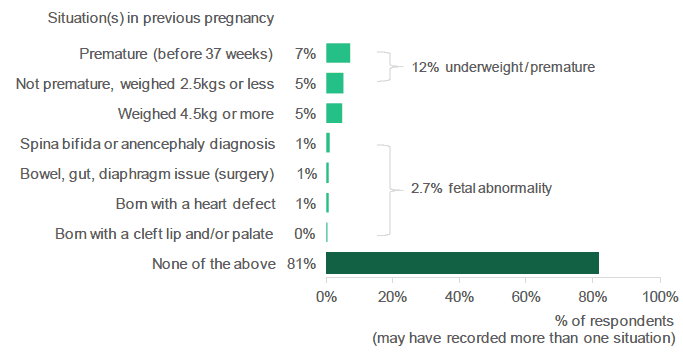
Source: Q4, Antenatal Survey
Amongst respondents who had previously been pregnant:
- 7% reported a previous pregnancy where the baby was born prematurely (before 37 weeks gestation).
- 5% reported that they had previously had an underweight baby (weighing 2.5kgs or less).
- 5% said they had previously had a heavier baby, weighing 4.5kg or more.
A small proportion of respondents who had previously been pregnant reported that a fetal abnormality had been encountered in a previous pregnancy (2.7% overall, and 1% or less for each type of fetal abnormality specified in the questionnaire). Although relatively rare, these conditions can have a significant impact on an infant's future health.
[ Figure 2.17; Table 2.19]
Previous pregnancy situations and planning for pregnancy
According to scores obtained using the LMUP:
- Just under three-quarters of respondents (72%) who had previously had a premature baby or an infant weighing 2.5kg or less "planned" their current pregnancy.
- Just over half of respondents (54%) who had previously had a baby weighing 4.5kg or more "planned" their current pregnancy.
- More than four in five respondents (83%) who had previous had a pregnancy where there had been a fetal abnormality "planned" their current pregnancy.
[Figure 2.18; Table 2.20]
Less than three-quarters of respondents, who had previously had a premature or underweight baby, "planned" their current pregnancy.
Figure 2.18: Summary of pregnancy planning. (Percentage of respondents who indicated that they had taken a particular action, by situations that occurred in previous pregnancies).
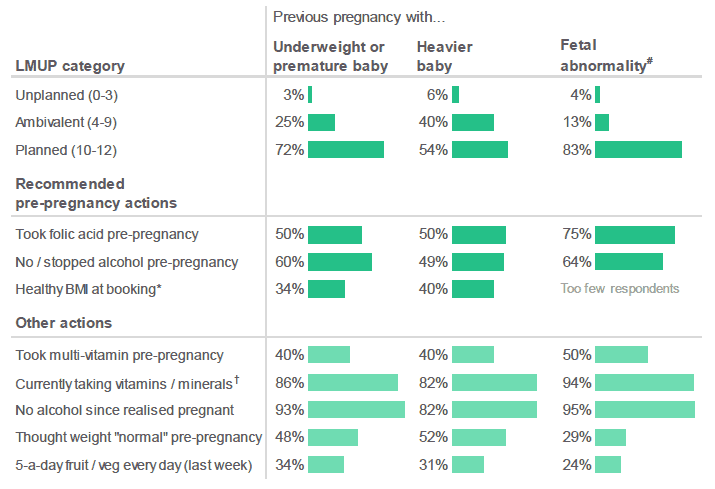
Source: Q5-10, Q12, Q29, Q17, Q11, Q14, Q30, Q18, Q24, Q4, Antenatal Survey
* Results for "Healthy BMI at booking" are based on a sub-set of respondents who provided a valid BMI.
† Respondents who had already given birth have been excluded from this analysis.
# Results for respondents who had previously had a pregnancy where there had been a fetal abnormality should be treated with extreme caution. There were only a small number of respondents in this group (weighted base = 32; unweighted base = 28).
Pre-pregnancy medical history
There is an increased risk of complications during pregnancy and birth associated with health conditions such as diabetes, epilepsy and/or high blood pressure. ( R19) Respondents were specifically asked if they had a history of any of these health conditions prior to their current pregnancy.
A small proportion of respondents (5%) reported that they had a history of diabetes, epilepsy and/or high blood pressure prior to their current pregnancy.
[Figure 2.19; Table 2.21]
Five percent of respondents had a pre-pregnancy history of diabetes, epilepsy and/or high blood pressure.
Figure 2.19: Did you have a history of any of the following health conditions before this pregnancy? (Percentage of respondents who selected each condition).
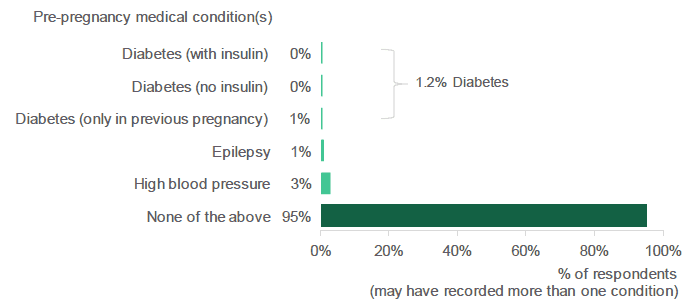
Source: Q32, Antenatal Survey
Pre-pregnancy medical history and planning for pregnancy
According to scores obtained using the LMUP:
- 70% of respondents with a pre-pregnancy history of diabetes and/or epilepsy had "planned" their current pregnancy.
- A similar percentage (69%) of respondents with a pre-pregnancy history of high blood pressure had "planned" their current pregnancy.
[Figure 2.20; Table 2.22]
Around 70% of respondents with a pre-pregnancy history of diabetes, epilepsy and/or high blood pressure "planned" their pregnancy.
Figure 2.20: Summary of pregnancy planning. (Percentage of respondents who indicated that they had taken a particular action, by pre-pregnancy medical history).
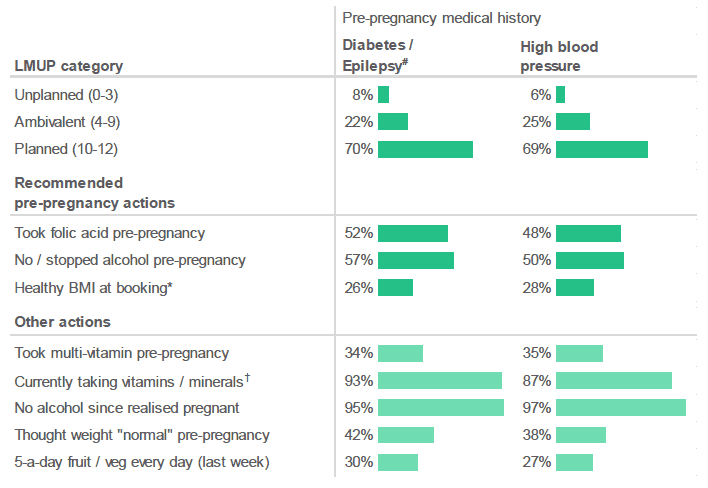
Source: Q5-10, Q12, Q29, Q17, Q11, Q14, Q30, Q18, Q24, Q32 Antenatal Survey
* Results for "Healthy BMI at booking" are based on a sub-set of respondents who provided a valid BMI.
† Respondents who had already given birth have been excluded from this analysis.
# Results for respondents who had a pre-pregnancy history of diabetes and/or epilepsy should be treated with caution. There were only a small number of respondents in this group (weighted base = 49; unweighted base = 49).
Pregnancy / medical history and high dose folic acid
A higher dose of folic acid is recommended for women with certain conditions, including diabetes, epilepsy and/or a history of some fetal abnormalities.
- 64% of respondents who had a previous pregnancy with a fetal abnormality were prescribed a higher dose of folic acid; 40% reported that they began taking high dose folic acid before becoming pregnant with their latest pregnancy. *
- A slightly lower proportion (59%) of respondents with a pre-pregnancy history of diabetes and/or epilepsy was prescribed a higher dose of folic acid. Twenty-seven percent (27%) of this group reported that they began taking this higher dose before their current pregnancy. #
Please note that no information is available about when the higher dose of folic acid was prescribed, only when the respondent reported that they started to take it.
[Figure 2.21; Table 2.23]
Less than two-thirds of respondents, who had previously had a pregnancy with a fetal abnormality or who had a pre-pregnancy history of diabetes and/or epilepsy, were prescribed a higher dose of folic acid.
Figure 2.21: Were you prescribed a higher dose (5mg) of folic acid just before pregnancy or in early pregnancy (the first 12 weeks)? (Percentage of respondents, by pregnancy / medical history).
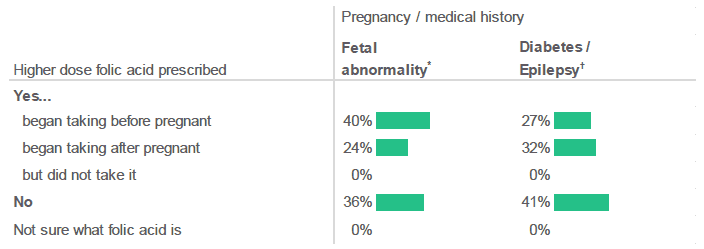
Source: Q13, Q4, Q32, Antenatal Survey
* Results for respondents who had previously had a pregnancy where there had been a fetal abnormality should be treated with extreme caution. There were only a small number of respondents in this group (weighted base = 32; unweighted base = 28).
† Results for respondents who had a pre-pregnancy history of diabetes and/or epilepsy should be treated with caution. There were only a small number of respondents in this group (weighted base = 49; unweighted base = 49).
2.9 Sources of information
In order to enable women to make informed choices, both before and during pregnancy, it is important that they have access to clear, high quality and timely information. This is particularly important for advice relating to the preconception period such as general guidance about maintaining a healthy pre-pregnancy lifestyle and diet, along with specific recommendations around the need for a folic acid supplement while trying to conceive and during pregnancy.
Pre-pregnancy information sources
A large proportion of respondents to the antenatal survey (63%) said they had not received any information about diet, vitamin supplements, smoking or drinking alcohol before becoming pregnant.
Those who said they had received information prior to becoming pregnant were asked where they had obtained this information from. The main sources of information reported were health care professionals (22%) and Internet / web based resources (15%). Sixteen percent (16%) of respondents who had been pregnant before reported using information from previous experience.
[Figure 2.22; Table 2.24a & 2.24b]
Most respondents did not get any information about adapting their diet, taking vitamins, or stopping smoking and drinking alcohol before they became pregnant.
Figure 2.22: Did you get any information about adapting your diet, taking vitamins, or stopping smoking and drinking alcohol before becoming pregnant? / Where did you get this information from? (Percentage of respondents who selected each source, by whether this is respondent's first pregnancy. Most common sources highlighted in green).
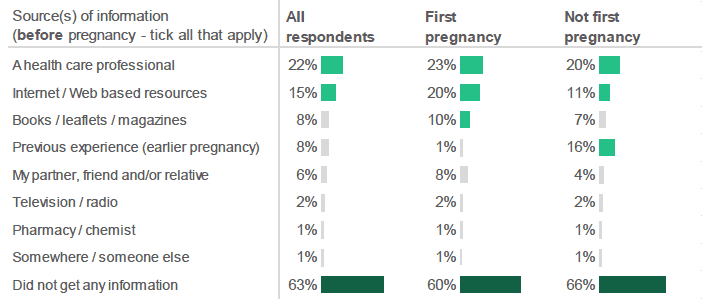
Source: Q20, Q21, Q2, Antenatal Survey
Information sources during pregnancy
By comparison, a much lower proportion (17%) reported that they had not obtained information about diet, vitamins, smoking and drinking during pregnancy.
Amongst those who had received information, the most frequently cited source was from a health care professional (74%). Respondents who were pregnant for the first time were more likely to report obtaining information from NHS Health Scotland's "Ready Steady Baby" book (34%) [14] or from Internet / web based resources (33%) than women who had been pregnant before (23% and 15% respectively).
Women who were pregnant for the first time also frequently indicated that they had used other books / leaflets / magazines (18%) or had received information from friends and family (15%).
Nearly a third (31%) of respondents who had previously been pregnant reported using previous experience as a source of information. However, almost a quarter of these respondents (22%) said that they did not get any information during pregnancy.
[Figure 2.23; Table 2.25a & 2.25b]
Most respondents did get information about adapting their diet, taking vitamins, or stopping smoking and drinking alcohol after they became pregnant.
Figure 2.23: Did you get any information about adapting your diet, taking vitamins, or stopping smoking and drinking alcohol during pregnancy? / Where did you get this information from? (Percentage of respondents who selected each source, by whether this is respondent's first pregnancy. Most common sources highlighted in green).
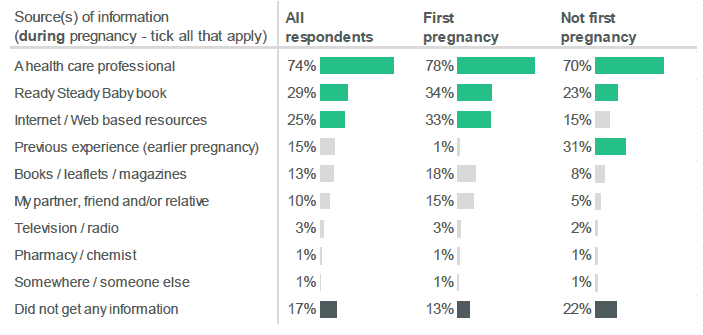
Source: Q20, Q21, Q2, Antenatal Survey