Scottish Health Survey - topic report: lung function
This report presents data from objective measurement of lung function in adults, measured by portable spirometers, using data from the 2008-
2011 Scottish Health Surveys.
Annex B Lung Function Protocol
1.1 Introduction
Lung function tests objectively assess respiratory function and are widely used in clinical practice to diagnose and monitor the progress of respiratory diseases such as asthma and chronic obstructive airways disease. A lung function test produces values across the various measures tabled below (Table 2). A wide range of variables can affect these factors, for example physical unfitness, smoking, chronic bronchitis, poorly controlled asthma, some muscular disorders and many other conditions. At a population level, these measures tell us a lot about the respiratory health of the population and are also indicators of general health.
Table 2 Lung function test values
| Test | Abbrev | Definition |
|---|---|---|
| Forced Vital Capacity | FVC | The total amount of air that can forcibly be blown out after a full inspiration, measured in litres. |
| Forced Expiratory Volume in 1 Second | FEV1 | The amount of air that can be blown out in one second, measured in litres. |
| FEV1% | FEV1/ FVC | The ratio of FEV1 to FVC. |
| Peak Expiratory Flow | PEF | The speed of air moving out of your lungs at the beginning of expiration, measured in litres per second. |
| Forced Expiratory Flow | FEF | The average flow (or speed) of air coming out of the lung during the middle portion of expiration. |
| Forced Inspiratory Flow | FIF | Similar to FEF except the measurement is taken during inspiration. |
| Forced Expiratory Time | FET | The length of expiration in seconds. |
| Tidal Volume | TV | The specific volume of air that is drawn into the lungs and then expired during a normal respiratory cycle. |
1.2 Exclusion criteria
Respondents are excluded from the lung function measurement if they:
Are pregnant
Have had abdominal or chest surgery in the preceding three weeks
Have been admitted to hospital with a HEART complaint in the preceding six weeks
Have had eye surgery in the preceding 4 weeks
Have a tracheostomy
1.3 Equipment
You will need:
A Vitalograph Escort spirometer and case
A 1 litre calibration syringe
Disposable cardboard mouthpieces
1.3.1 Caring for the spirometer
For the purposes of hygiene and accuracy, once a month or after every 50 respondents remove the flowhead and clean it in hot soapy water and allow it to dry overnight before refitting.
When necessary clean the exterior with a lint free damp cloth. DO NOT clean the two white cylindrical filters on the top of the unit.
1.3.2 Using the spirometer
Take a spare battery with you in case of battery failure. The spirometer uses a 9v pp3 battery.
Whenever the 'ON' button is pressed to perform a new test, ensure that the spirometer is placed on a flat surface with the mouthpiece pointing upwards.
Unpack the spirometer as soon as possible and keep it away from direct heat. Allow the spirometer to equilibrate to room temperature before the lung function tests are performed.
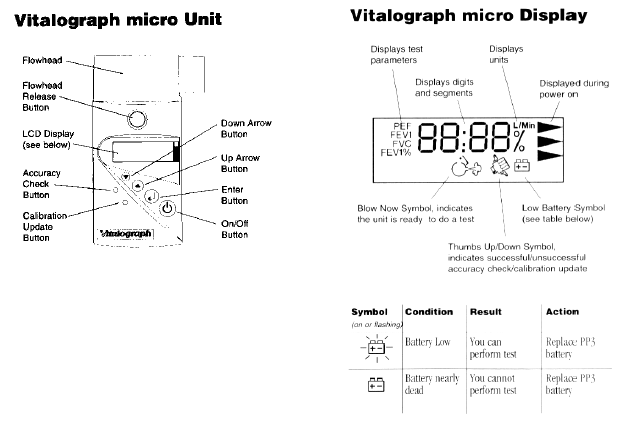
See Figure 6 for the spirometer unit and the display
Figure 6 The Spirometer
1.3.3 Calibration/accuracy test
1. Before using the spirometer its accuracy must be checked by calibrating it. This procedure can be done in your own home at the start of each day when you are working. If you have more than one visit in the same day you need to calibrate the spirometer only once. You should not need to take the calibration syringe with you when you make a visit.
2. Ensure that the spirometer and syringe have been in the same temperature environment for at least an hour.
3. Connect the spirometer, by the flow head, to the syringe. Pump through a few litres of air, then disconnect the spirometer.
4. Switch on the spirometer and press the small top most button to the left of the arrow keys (the accuracy check button). The display will show a number.
5. Check display is 01. If not, adjust with up/down arrow keys (see figure 6).
6. Press the left arrow key (the enter button) and wait until display shows 'blow now' and 'thumbs down' symbols.
7. Making sure the syringe piston is fully withdrawn, connect the syringe to the flow head. The handle of the spirometer should be pointing upwards.
8. Using one swift, smooth stroke pump in the volume of air (about 1 second). Don't cover the outlet with your hand.
9. Wait for a double beep then withdraw the piston fully and repeat step 8 until five single beeps occur. It is very important to wait for the double beep before withdrawing the piston each time.
10. If 'thumbs up' is displayed, the spirometer has been correctly calibrated.
11. If a 'thumbs down' sign appears on the display, then the spirometer is outside the accuracy requirements, contact Brentwood to arrange for a replacement.
12. Press the On/Off button to switch off.
1.3.4 Technical faults
Refer to table 3 if technical difficulties are experienced with the spirometer
Table 3 Troubleshooting for the spirometer
| Fault | Action |
|---|---|
| Nothing is displayed when the ON button is pressed |
|
| False readings suspected |
|
| Calibration values vary greatly |
|
If any problems persist, contact Brentwood for advice.
1.4 Preparing the respondent
- Before commencing the spirometer procedure explain the following to all eligible respondents:
- The purpose of the test and how to use the spirometer.
- To ensure an accurate reading they must 'blow' as hard as they can so long as it does not cause them any pain and/or discomfort.
- The definition of an acceptable level of lung function depends on the person's age, sex and height.
- A diagnosis of abnormality is not based on a reading from a single occasion but is rather based on several measurements and on the person's clinical history.
1.4.1 Demonstrating
For an accurate reading of lung function it is very important that you demonstrate the blowing technique to each respondent. Do this using a spare mouthpiece that is not connected to the spirometer and follow the procedure below:
1. Explain that the mouthpiece should be held in place by the lips, not the teeth and that the lips are wrapped firmly around the mouthpiece so no air can escape.
2. Demonstrate a blow, pointing out afterwards the need for full inspiration, a vigorous start to exhalation and sustained expiration. The blow should be at least 3 seconds in duration and not interrupted by coughing, laughing or leakage of air. The torso should remain in an upright position throughout the blow, not hunched over at the end.
1.5 Procedure
1. The respondent must be standing, unless chairbound, and they should loosen tight clothing to allow for a bigger inspiration. If the respondent wears dentures, it is preferable that they leave them in as they will get a tighter seal with their mouth around the mouthpiece which will result in a more accurate result.
2. Following the demonstration, hand the respondent a clean disposable mouthpiece and allow the respondent at least one practice blow using the mouthpiece alone. Correct their technique where necessary.
3. Attach the respondent's mouthpiece and turn the unit on using the 'ON/OFF' button. Check that the 'low battery' symbol is not showing.
4. Gently hand the spirometer to the respondent as sudden jerky movements can destabilise the unit. If a single beep sounds at this point, wait for the spirometer to stabilise, indicated by a further double beep, before proceeding with the test. The display should also display the 'blow' symbol.
5. Ask the respondent to take as deep a breath as possible, keeping the spirometer away from their mouth, and then to hold the mouthpiece with their lips and seal their lips around it so that air does not escape while they are blowing. Check that the spirometer is held below the flowhead with the handle pointing downwards and the subject's hand is not obstructing the flowhead outlet.
6. Then say "now blow!" As the respondent is blowing encourage him/her by saying "keep going, keep going, keep going..." to get the maximum expiration possible. Observe the respondent closely for satisfactory technique. If the blow was technically unsatisfactory, they will need to blow again (refer to section 10.6).
7. Take the spirometer from the respondent and record the appropriate readings in CAPI by using the down arrow to scroll through the display.
8. Switch off the spirometer to reset the unit. This is very important, otherwise the subsequent readings are based on the best of a series of tests and not on individual blows.
9. Repeat steps 3-8 until you have obtained the required number of technically satisfactory blows (refer to project specific instructions). Most respondents should be able to manage what is required but there may be some that cannot. You must strike a balance between encouragement and over-insistence.
10. If the respondent wishes, record the results on their measurement record card, recording the highest obtained reading for each measure, even if they came from different blows.
1.6 Technically unsatisfactory blows
The following may result in a technically unsatisfactory blow, and if any of these occur the test should be repeated.
- Unsatisfactory start: excessive hesitation or "false start". It is probable that the spirometer will not record this blow (or give lung capacity as zero), but sometimes it will give a spurious reading.
- Laughing or coughing, especially during the first second of the blow. Some people will cough a little towards the end of expiration (particularly if this extends to 5 or 6 seconds) but this is acceptable.
- Holding the breath against a closed glottis (Valsalva manoeuvre). This results in spuriously high peak expiratory flow (see table 2).
- Leakage of air around the mouthpiece.
- Obstruction of the mouthpiece by tongue or teeth.
- Obstruction of the flowhead outlet by hands.
- If the spirometer takes more than 3 seconds to display the results after the end of the blow, it is likely that the results are spurious.
Contact
Email: Julie Landsberg