The Scottish Child Health Programme: Guidance on the 27-30 month child health review
Guidance on the core issues which should be addressed and recorded at the 27-30 month review, and standardised methods of assessment to ensure consistency of practice across Scotland.
Assessing children's needs
General approach
14. Assessing children's wellbeing and needs within the context of their family and wider environment is a fundamental part of the 27-30 month review. Assessment is a complex task that requires a high level of professional knowledge and skill.
15. Successful needs assessment takes place within the context of a positive relationship between Public Health Nurse - Health Visitor (PHN-HV) and the family. It is recognised that PHN-HVs may have had minimal contact with some children and their parents since early infancy. Re-establishing relationships may therefore be a challenging task that requires more than one contact.
16. There is broad agreement that structured professional judgement supported by the informed use of validated tools offers the best general approach to needs assessment4-6. The benefits of using standardised tools to support (not replace) professional decision making include creating consistent thresholds for intervention, supporting communication with families and between practitioners, and providing consistent data that allows the prevalence of problems in different population subgroups to be explored.
17. This guidance provides an overview of assessment tools (particularly those assessing child development) that are appropriately validated and considered likely to be of practical use in Scotland. Checklist or tick box approaches to assessment and/or the use of unvalidated assessment tools not included in this guidance are unlikely to be helpful and should be avoided, unless their use is part of a robust research process.
18. The assessment process is ultimately aiming to provide a balanced view shared by the PHN-HV and parents of a child's development and health, the factors in their life that are likely to influence (positively or negatively) their future progress, and their need for additional support to attain good outcomes. It is recognised that occasionally there may be significant discrepancy between the PHN-HV view and that of parents, for example in cases of child neglect, and such circumstances require a sensitive approach.
The GIRFEC framework
19. The Getting it right for every child (GIRFEC) approach provides a useful general framework for assessment, analysis and planning covering both general and specific assessments. GIRFEC encourages practitioners to keep children's wellbeing, and what they can do to support and advance that, as their primary consideration at all times4. The approach breaks down the concept of children's wellbeing into eight indicators: safe, healthy, achieving, nurtured, active, respected, responsible, and included. Whenever practitioners come into contact with children, they are encouraged to consider the child's wellbeing and ask themselves five key questions, namely
- What is getting in the way of this child's or young person's wellbeing?
- Do I have all the information I need to help this child or young person?
- What can I do now to help this child or young person?
- What can my agency do to help this child or young person?
- What additional help, if any, may be needed from others?4, 7
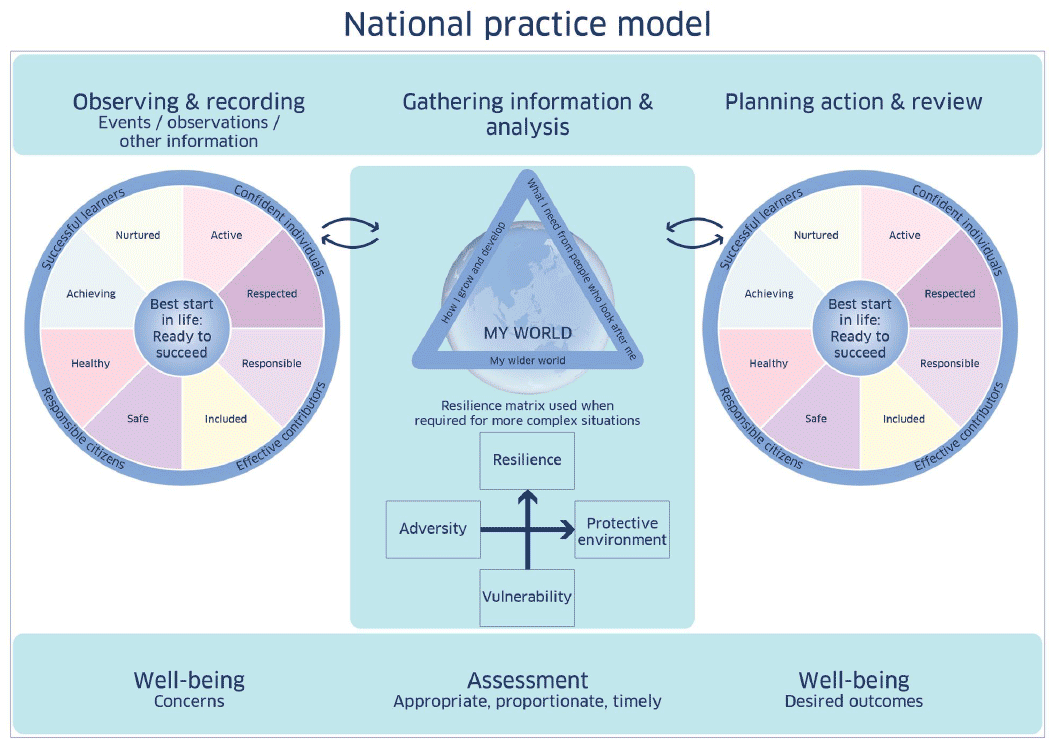
20. Underpinning this approach is the use of the national practice model (see Figure 1) to support more detailed assessment of children's circumstances when required7,8. This more detailed approach to assessment is appropriate for 27-30 month reviews.
21. The national practice model encourages practitioners to adopt an integrated approach to assessment and planning by:
- Initially considering a child's wellbeing in the round using the wellbeing indicators
- Gathering more detailed information about a child's intrinsic characteristics and their immediate and wider environment using the My World assessment triangle9
- Analysing the information to build a picture of the strengths and pressures in a child's life, using the resilience matrix10, and
- Using the information gathered as the basis for planning, implementing, and reviewing the actions necessary to secure and promote the child's wellbeing, again using the wellbeing indicators.
22. All practitioners should be familiar with the national practice model. Full information on the GIRFEC approach can be found at http://www.scotland.gov.uk/Topics/People/Young-People/gettingitright.
Figure 1: GIRFEC national practice model8
Assessing children's development
23. Although formal screening for developmental delay is not currently recommended by the National Screening Committee, the 27-30 month review should include systematic consideration of all children's development as part of ongoing surveillance11,12. Staff undertaking the review should have a good understanding of normal child development. Mary Sheridan's classic work in this field has been recently updated and provides a very helpful framework13. The Personal Child Health Record (Red Book)14 also contains relevant pages on developmental milestones that most (at least 90%) children have reached by specified ages.
24. All reviews should entail a structured discussion with parents to assess the extent to which children are attaining expected milestones and to elicit any concerns that parents have about their child's development. The Parents' Evaluation of Developmental Status (PEDS) questionnaire offers a well validated approach to eliciting parental concerns that Boards may wish to use15,16. The PEDS: Developmental Milestones questionnaire offers a systematic way of assessing whether children have attained key milestones17. Formal scoring of the PEDS and/or PEDS:DM indicates children at increased risk of having problems in the various developmental domains.
25. There is good evidence that in most instances, parental reporting of children's developmental status, for example attainment of specific milestones, is highly accurate18,19. If parents express significant concerns about an aspect of their child's development, these should always be taken seriously and investigated appropriately20. It is recognised that some parents will have difficulties in accurately reporting their children's development21, for example due to learning difficulties or mental illness.
26. There is a general trend towards greater reliance on parental reporting of children's developmental status rather than practitioners always having to seek 'proof' through direct testing of children. Nevertheless, careful observation of children during the course of the review will provide PHN-HVs with useful additional information on their developmental status22,23. A greater reliance on direct testing will be required for children whose parents are less able to objectively report on their development.
27. If after initial structured discussion and observation there are any uncertainties or concerns regarding a child's developmental progress, a more in depth assessment should be undertaken using a validated developmental assessment tool. A very large number of tools are available but the following are suggested as a core set that should be available to PHN-HVs across Scotland. Further detail on the tools, how to access them, and available manuals and training resources is provided in Appendix 2.
28. The Ages and States Questionnaire 3 (ASQ)16 and the Schedule of Growing Skills II (SOGS II) both assess all developmental domains (although they are relatively light on social/emotional development). Both provide standard questionnaires that can be completed by the PHN-HV in discussion with the parent and both involve the PHN-HV in observing children's ability to undertake specific tasks during guided play.
29. Both questionnaires are 'scored'. Children do not pass or fail but the profiles of scores generated do provide clear suggestions for subsequent action, for example provision of additional support and retesting or formal referral. Both cover the whole pre-school age range hence can help to track children's progress over time and monitor the effectiveness of interventions provided. The process of working through the questionnaires with parents can be a useful way of structuring discussion about children's developmental ability and their strengths and areas of concern.
30. Both are already widely used in Scotland and areas that are already using these tools report very high satisfaction with them. The tools are relatively low cost to purchase (see Appendix 2), come with dedicated training resources, are easy to administer and are acceptable to parents. Furthermore, they have been found to provide clear pointers to subsequent action and to support communication, for example when making referrals.
31. It should be emphasised that these tools should support rather than erode or replace PHN-HV professional decision making. None of the suggested tools should be used in a mechanistic way: professional judgement should be used when deciding the appropriate clinical response to an individual child.
32. When developmental assessment tools are being produced, they are usually applied to a relatively large number of children to see the distribution of scores at a particular age in the general population. Cut offs are then set to indicate children scoring below a certain threshold. The cut offs can be set to identify a certain proportion of children (e.g. the lowest scoring 10%) or children known to be having functional difficulties related to development (e.g. those identified by educational staff as struggling at pre-school). Further cut offs may also be set to identify children near the threshold that may benefit from additional ongoing monitoring or support. The tools are then usually tested again on different populations of children to ensure that the cut offs remain meaningful across a range of settings.
33. The proportion of children expected to score below a cut off can therefore be predicted for any given test. It should be noted that this proportion is often quite high - usually around 10% of children in the general population and potentially considerably higher in vulnerable groups such as children living in poverty. Systematic use of developmental assessment tools can therefore be expected to increase the numbers of children identified as developmentally vulnerable. This in turn has implications for other services that families may be already using or be referred on to e.g. parenting programmes, early learning and childcare, family support, Speech and Language Therapy, physiotherapy, occupational therapy, developmental paediatrics, Child and Adolescent Mental Health Services, etc. Local areas will therefore need to develop clear care pathways for children identified at their 27-30 month review as having possible developmental problems and ensure adequate capacity among all relevant services.
34. Additional tools are available that assess particular developmental domains or assess the risk of particular pathologies. The ASQ: Social-Emotional (ASQ:SE)24 and the Strengths and Difficulties Questionnaire (SDQ)25,26 both assess social and emotional development. The SDQ is freely available and results have been shown to indicate the risk of future mental health problems26. Traditionally it has been used for children aged 3-16 years but recently it has been provisionally validated for use in 2 year olds25,26 [a].
35. The Sure Start Language Measure (SSLM)27,28 assesses children's language development by asking parents whether they have concerns about their child's language, whether their child is starting to combine words, and which, from a standard list of 50 words their child can say. At 27-30 months, children who can say fewer than 10 words from the 50 list are likely to be around or below the 10th percentile for expressive language development at that age and hence may warrant further investigation, support or referral28,29.
36. The Modified Checklist for Autism in Toddlers (M-CHAT)30-34 is a further useful tool that assesses the risk of Autistic Spectrum Disorder and may be useful prior to making referrals to services such as Child and Adolescent Mental Health or developmental paediatrics. The Eyberg Child Behaviour Inventory (ECBI)35-37 can also be used to provide an assessment of childhood behavioural problems.
37. Many of these tools are already in widespread use in Scotland. The ASQ and ASQ:SE are routinely administered to all children receiving the Family Nurse Partnership service38. SOGS II is used when necessary within the 24-30 month reviews already being delivered in Dumfries & Galloway to facilitate more in depth assessment of selected children's development. NHS Greater Glasgow & Clyde has been routinely administering the SDQ and SSLM in the universal 30 month review that they have been piloting for some time.
38. It is likely that, at least in the shorter term, Boards will take different approaches to the use of the recommended tools. Some may choose to use one or more tools on a universal basis, i.e. routinely offer them to all children at their 27-30 month review. Some may choose to use the tools on a more selective basis, i.e. only offer them to children if initial discussion and observation suggest they are required. Some tools, in particular the M-CHAT and Eyberg scales should definitely only be used on a selective basis when indicated.
39. The national dataset to be returned on all completed 27-30 month reviews (see later chapter) has been designed to capture information on the tools used to assess children's development, the outcome of the overall assessment process (e.g. whether any new concerns about any developmental domain have been identified), and the actions that have been planned as a result (e.g. recall to PHN-HV for early reassessment, referral to GP or more specialist services for more detailed assessment, and/or provision of parenting support). It is anticipated that over time the data generated will allow exploration of any associations between different approaches to developmental assessment, identification of developmental concerns, interventions, and ultimately children's outcomes and hence inform further refinement of policy and guidance on this issue.
40. The national dataset asks PHN-HVs to note their assessment of children's development in each of several domains, such as social, gross motor, vision, etc. It is important that all developmental domains are given due consideration but it is likely that the main focus of assessment will be on children's social/emotional and language development as these are the areas in which issues are mostly likely to be coming to light at the 27-30 month stage. Assessment of other domains may be quite brief, for example enquiring whether parents have any concerns about a child's vision and whether they have noticed a squint, and observing how a child manipulates small toys during the course of the review, is likely to be sufficient to assess a child's visual development in most cases. The 27-30 month review provides a useful opportunity to remind parents of the pre-school vision screening that all children will be offered.
41. Some of the developmental assessment tools will not be appropriate for children with obvious, severe developmental problems that have been previously diagnosed, and PHN-HVs will need to tailor their approach accordingly. Conversely, it should not be assumed that children with known problems in some developmental domains do not need any developmental assessment. Children with motor development problems due to cerebral palsy may well still benefit from assessment of their social/emotional and language development, for example.
Assessing children's nutrition, physical activity, and growth
42. The National Screening Committee does not currently recommend formal screening for growth problems at 27-30 months39 but surveillance of children's nutrition, physical activity and growth will be an important part of the 27-30 month review.
43. The 27-30 month review can contribute to the promotion of child healthy weight by providing all families with consistent messages on healthy eating, family meals, physical activity, screen time, and adequate sleep. Relevant health promotion resources and evidence summaries on this issue are included in Appendices 3 and 4.
44. The National Obesity Observatory40 has produced helpful resources that outline how the Child Health Programme can contribute to the promotion of child healthy weight and has also developed relevant training for staff through the HENRY programme41. Some children are known to be at higher risk of developing childhood obesity than others and these health promotion messages will be particularly important for them. Key risk factors for developing obesity in childhood include parental obesity, high maternal weight gain in pregnancy, gestational diabetes, inappropriate weight for gestational age, rapid weight gain in infancy, bottle feeding, early weaning, Asian ethnicity, and poverty20, 42-44.
45. In Scotland around 25% of children aged 27-30 months are already overweight according to the epidemiological definition (BMI ≥85th centile) with around 5% clinically obese (≥98th centile) and 3% clinically underweight (≤2nd centile)[b]. There is some debate about how stable overweight is in this age group but in general children with severe overweight at 27-30 months are likely to remain overweight (particularly if there is coexisting parental obesity)45-50. The long term adverse physical and mental health implications of child and adult obesity have been well documented although there is little specific evidence relating to children aged 27-30 months44, 46, 51-55.
46. The 27-30 month review can therefore also contribute to the promotion of child healthy weight (CHW) by referring children with established obesity to child healthy weight interventions. There is some debate about the effectiveness of CHW interventions but in general evidence is accumulating for both preventive and treatment interventions, including in the pre-school age group56-59. Multifaceted family interventions can lead to sustained meaningful changes in eating, activity and weight.
47. The Child Healthy Weight HEAT3 target60 has been specifically designed to increase capacity within Boards to deliver child healthy weight interventions to children from age 24 months upwards. Almost all Boards have developed some capacity for delivering CHW interventions to pre-school children in response to the target although the precise services available vary between Boards. NHS Board Child Healthy Weight coordinators will be able to advise on services available in specific areas. The 27-30 month review will provide an important early opportunity for families to be referred to these services as appropriate.
48. Children found to be clinically underweight may need more detailed medical assessment to exclude underlying pathology.
49. The relative merits of weighing and measuring all children, or only selected children, at the 27-30 month review have been robustly debated during the process of producing this guidance. Differences of view persist but on balance it is recommended that all children should be offered measurement of weight and height as part of their 27-30 month review. This recommendation will be kept under review. Measurement is not necessarily straightforward, particularly of height (standing height is used to assess growth from 24 months onwards) but accuracy is important. Appropriate equipment and good technique are required61. Good practice guidance is provided on the A4 World Health Organisation (WHO) growth charts and through the Royal College of Paediatrics and Child Health62. The Scottish Government has also produced guidance on weighing and measuring children to support the Child Healthy Weight HEAT3 target61.
50. All weight and height measurements should be plotted on the appropriate UK-WHO (0-4 years) growth chart62 and returned as part of the national dataset to the Child Health Surveillance Programme - Pre-School (CHSP-PS) information system. UK-WHO growth charts are available from the Royal College of Paediatrics and Child Health63 and from Harlow Printing63.
51. There is good evidence that both parents and practitioners are poor at identifying children with over or underweight just from 'eyeballing'64-69. BMI centile is the appropriate measure of child (un)healthy weight from 24 months onwards61. It will not be necessary to calculate a BMI centile for all children as part of the 27-30 month review, for example if a child's weight and height are both near to the 50th centile, calculation of BMI would not be required. If there is possible concern about a child's growth, for example their weight is above the 75th centile or below the 9th centile, or there is marked discrepancy between weight and height centiles, BMI centile can be estimated for children aged two to four years using the conversion chart provided on the A4 UK-WHO growth charts63.
52. The CHSP-PS system calculates an accurate BMI centile for each child from the weight and height data that is entered. These additional data can then be used for population monitoring of child growth at the local and national level.
53. The weighing and measuring of children should not be seen as an end in itself and it should not dominate the 27-30 month review. Weighing and measuring should be seen as part of wider promotion of healthy eating, family meals, physical activity, active play, and child healthy weight and should clearly link to subsequent action, for example PHN-HV support and re-measurement or referral onto more specialist services depending on findings.
Assessment of other specific issues
54. It will be important for PHN-HVs to have access to up to date information on children's physical health and any parental health issues prior to the 27-30 month review to ensure the assessment process is as comprehensive and efficient as possible (see later chapter on Delivering the review).
55. Some children will have had specialist assessments that could provide very rich information relevant to their 27-30 month review. For example, children who were in Neonatal Intensive Care due to premature birth are all offered a detailed developmental assessment when they attain two years of age as part of their routine follow up. It would be helpful if PHN-HVs had access to the results of these assessments prior to conducting children's 27-30 month reviews so that the review can add value to the specialist follow up (for example by considering the child's development within the wider context of their family circumstances) rather than unnecessarily duplicate assessment processes. Similarly, the results of the 27-30 month review would be valuable to those providing ongoing specialist follow up and information should be shared with parental consent.
56. Although parent-child attachment is very important to children's outcomes70,71, formal assessment of attachment is not feasible within a universal child health review. Nevertheless, PHN-HVs will be able to use their observation of the parent-child relationship in their overall assessment of the child's family environment.
57. A number of Boards have implemented routine enquiry about domestic abuse as part of post-natal/early child health surveillance services in response to CEL 41 2008 on gender based violence72. Some Boards have indicated that they also intend to incorporate routine enquiry about domestic abuse into the 27-30 month review and this approach is supported given the widespread nature of domestic abuse and its known detrimental effects on children's development and long term physical and mental health73.
58. If there are concerns about a child's physical health following their 27-30 month review, a general medical assessment can be requested from the General Practitioner. If there is any doubt about testicular descent this should be assessed on examination and prompt referral initiated if required. Similarly, if there is any concern about a child's gait, in particular presence of a limp that may indicate previously unsuspected congenital dislocation of the hip, this should be formally assessed and referral initiated as appropriate.
59. Exposure to second hand smoke is detrimental to children's health. It increases the risk of respiratory and middle ear infections, and exacerbates asthma symptoms. ASH Scotland has recently published a REFRESH 'how to' guide for practitioners on assessing parental smoking and discussing smoke free homes74.
60. Parental substance misuse can have a profound impact on children's development and wellbeing, both through direct in utero exposure and through impairment of parenting capacity after birth75. Fetal Alcohol Spectrum Disorder is a common and under-recognised cause of childhood developmental problems in Scotland76. Effective interventions are available for children affected by fetal alcohol harm, for example tailored parenting and educational support. Effective interventions for mothers are also available to help avoid further affected pregnancies76.
61. The HOME inventory is a useful validated tool to support assessment of parenting and the home learning environment77. PHN-HVs may wish to use this for families experiencing particular challenges and to monitor the effectiveness of support provided to such families over time.
62. PHN-HVs should be aware of the Scottish Government National Risk Framework to Support the Assessment of Children and Young People (published in final form in 2012)78. This document is a national risk assessment 'toolkit' for child protection to support practitioners in identifying and acting on child protection risks in children and young people
63. There are complex relationships between many of the topics to be covered in the review that all contribute to the wellbeing of the child. For example: relationships between motor development, play opportunities, physical activity and injury prevention or between social/emotional development, language/cognitive development, parenting and wider family circumstances. Equally, many different issues may underlie particular problems, for example growth problems will usually reflect unhealthy eating and physical activity patterns within the family but may indicate a specific underlying medical condition.
64. Dealing with this level of complexity requires substantial professional skills. It also means that assessment of apparently very specific issues (such as language development) can be seen as a lens through which to consider various issues (such as parenting and the home learning environment, autism risk, and hearing).
Contact
Email: Mary Sloan