Review of the Gluten-free Food Additional Pharmaceutical Service
A review of the Gluten-free Food Additional Pharmaceutical Service being provided on a trial basis in NHS community pharmacies.
Annex 6
Evaluation of Gluten Free Food Service
Survey of Patients, Community Pharmacists and GPs
1. Introduction and Methods
The views and experience of patients, Community Pharmacists and GPs were gathered to inform the Evaluation of the Gluten Free Food Service (GFFS) being provided as an Additional Pharmaceutical Service in NHS community pharmacies.. An on-line questionnaire comprising mainly closed questions was developed for each group (Annexes 1-3). GPs and Community Pharmacists were sent links to the relevant questionnaire and asked to complete and submit it. The patients' questionnaire was made available on-line and in hard copy and advertised through relevant bodies, i.e. Coeliac UK. Community Pharmacists were also provided with flyers to pass onto patients in receipt of gluten free food. These gave information on completing the questionnaire on-line or obtaining a paper copy of the survey from the Pharmacist. The patients and Community Pharmacists were surveyed in March 2015 and GPs in May 2015.
2. Survey of Patients - Analysis and Findings
2.1 Patient Responses
Patients completed a questionnaire comprising 14 questions on; their experience of the service; the impact of the service on their food selection; the Adult Coeliac Disease Health Check; and an invitation to give comments. A total of 1571 patients completed and returned the survey, and of these 1494 (95%) were using the new Gluten Free Food Service (GFFS). Practically all (95%; n=1570) respondents had previously received gluten-free food prescriptions from their GP.
2.2 Main Findings
There is strong support from patients responding to the survey for the GFFS, with the vast majority liking the service and supporting its continuation.
There is an association between ease in changing their order and how often patients do so. In the majority of cases patient reported changing their order more often increased since the introduction of the GFFS.
Just under half of respondents had received a coeliac health check but less than one third had received a pharmacy check since starting the GFFS.
2.3 Profile of Respondents
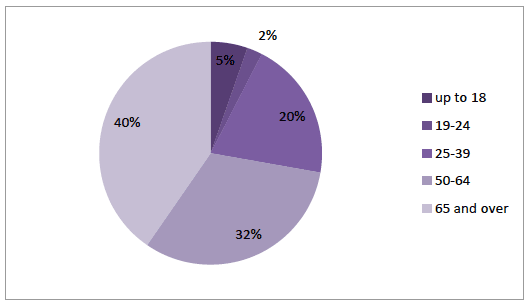
There were responses from: individuals living in all the Health Board areas in Scotland; men and women; a range of ages but the distribution was not even. Over twice as many responses were from women (65%; n=1016) as men (29%; n=463) (6%; n=92 did not indicate their gender) (Table 2‑1). The respondent age profile was towards older age groups, with 40% (n= 603) aged 65 and over and 32% (n=476) aged between 50-64 (Figure 2‑1). There were fewest respondents in the 19-24 age category (2%; n=33) and 5% (n=80) were aged under 18, of which just over one third (n=28) were under 10 and their parents had completed the survey.
Table 2‑1 Gender of respondents
| Number of responses | Percentage | |
|---|---|---|
| Male | 463 | 29% |
| Female | 1016 | 65% |
| Not Answered | 92 | 6% |
| 1571 | 100% |
Responses were broadly in line with population proportions in Health Board areas. Fife, Forth Valley, Tayside, Dumfries and Galloway and Borders had the highest proportion of responses and Grampian, Lothian and Lanarkshire the lowest (Table 2‑2).
Table 2‑2 Population and Survey Respondents by Health Board
| Health Board | Pop | % of pop | Response Count | Response % |
|---|---|---|---|---|
| Ayrshire & Arran | 372,210 | 7% | 115 | 7.7% |
| Borders | 113,870 | 2.1% | 69 | 4.6% |
| Dumfries & Galloway | 150,270 | 2.8% | 77 | 5.2% |
| Fife | 366,910 | 6.9% | 126 | 8.4% |
| Forth Valley | 299,680 | 5.6% | 125 | 8.4% |
| Grampian | 579,220 | 10.9% | 118 | 7.9% |
| Greater Glasgow & Clyde | 1,137,930 | 21.4% | 337 | 22.6% |
| Highland | 321,000 | 6.0% | 108 | 7.2% |
| Lanarkshire | 652,580 | 12.2% | 137 | 9.2% |
| Lothian | 849,700 | 15.9% | 99 | 6.6% |
| Orkney | 21,570 | 0.4% | 4 | 0.3% |
| Shetland | 23,200 | 0.4% | 12 | 0.8% |
| Tayside | 412,160 | 7.7% | 163 | 10.9% |
| Western Isles | 27,400 | 0.5% | 4 | 0.3% |
| 5,327,700 | 100% | 1494 | 100% |
2.4 Patients' Views of Service
The vast majority of respondents liked the service (90% n=1284) and want it to continue (93%; n=1318) (Table 2‑3). Indeed very few respondents disagreed with this (4%; n=52 and 2% n=34) and only a few more neither agreed nor disagreed (6% n=87 and 5% n=64 respectively).
Table 2‑3 Views on the GFFS and its continuation
| I would like this new Gluten Free Food Service to continue | I like the new Gluten Free Food Service | |||
|---|---|---|---|---|
| Number of responses | Percentage | Number of responses | Percentage | |
| Agree | 1318 | 93% | 1284 | 90% |
| Disagree | 34 | 2% | 52 | 4% |
| Neither Agree nor Disagree | 64 | 5% | 87 | 6% |
| 100% | 100% | |||
One question asked if respondents would prefer their prescription to be from the GP. In a further indication of support for the GFFS, 78% (n= 1093) disagreed and only 5% agreed (n=70) with this suggestion (Table 2‑4).
Table 2‑4 Prefer to Obtain Prescription from GP
| Number of responses | Percent | |
|---|---|---|
| Agree | 70 | 5% |
| Neither Agree nor Disagree | 170 | 12% |
| Disagree | 1093 | 78% |
| Not Applicable | 61 | 4% |
Whether respondents liked the GFFS was analysed according to health board in which they reside. In all Health Board areas the majority of respondents liked the service (Table 2‑5). This was highest in Orkney and Western Isles (100% n=3) (but the low response numbers should be noted). There were high levels of support in Borders (94% n=63) Forth Valley and Lanarkshire (93% n=108 and n=120 respectively). This fell to 82% in Fife, and 85% in Ayrshire and Arran. The areas that had the most, although still a small number and proportion, people disagreeing with statement "I like the Gluten Free Food Service" were; Fife (8% n=9); Dumfries and Galloway (7% n=5) and Highland (6% n=6).
Table 2‑5 Response to Statement "I like the new Gluten Free Food Service" by Health Board
| Ayrshire & Arran | Borders | Dumfries & Galloway | Fife | Forth Valley | Grampian | Greater Glasgow & Clyde | Highland | Lanarkshire | Lothian | Orkney | Shetland | Tayside | Western Isles | Total | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Agree | 85% | 94% | 89% | 82% | 93% | 89% | 91% | 90% | 93% | 92% | 100% | 91% | 92% | 100% | 90% |
| Disagree | 4% | 1% | 7% | 8% | 4% | 4% | 3% | 6% | 2% | 3% | % | % | 2% | % | 4% |
| Neither Agree nor Disagree | 12% | 4% | 4% | 10% | 3% | 7% | 6% | 3% | 5% | 4% | % | 9% | 6% | % | 6% |
| 100% | 100% | 100% | 100% | 100% | 100% | 100% | 100% | 100% | 100% | 100% | 100% | 100% | 100% | 100% |
2.5 Patients' Experience of service
The majority of respondents, 93% (n=1320) agreed with the statement, "It is easy to place a gluten-free monthly order with my community pharmacy" (Table 2‑6). 90% (n=1281) agreed that they are provided with enough information to use the service.
| Easy to place my Gluten Free Food order | I am provided with enough information | |||
|---|---|---|---|---|
| Number | % | Number | % | |
| Agree | 1320 | 93% | 1281 | 90% |
| Disagree | 51 | 4% | 50 | 4% |
| Neither Agree nor Disagree | 52 | 4% | 93 | 7% |
2.6 Impact of Service
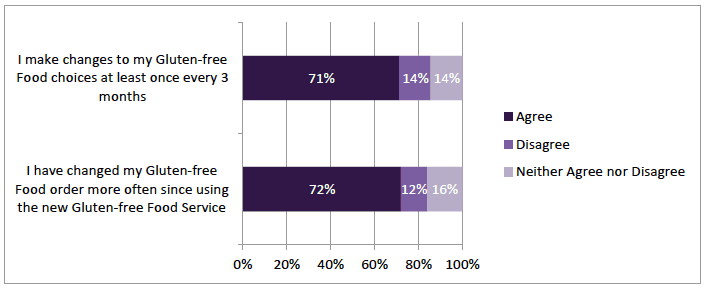
The service seemed to facilitate patients changing their order more often. 72% (n=982) altered their order more often than prior to the service introduction and 71% (n=995) had made changes at least once in three months (Figure 2‑2).
Figure 2‑2 Changes to gluten-free food order
The ease with which a patient could place their gluten-free food monthly order was associated with changing the order more often. Therefore 89% of respondents (n=935) who agreed it was easy to place their order also agreed that they had changed it more often (Table 2‑7). This was supported in the reverse with a majority (59% n=23) who disagreed it was easy to change the order were not changing it more often. Ease of changing was not essential and 41% (n=16) who didn't find it easier were still altering their order more often. There was a little variation with age, with older people a little less likely to change their order.
Table 2‑7 Ease of Changing Order with Increased Changes
| It is easy to place my Gluten Free Food monthly order with my Community Pharmacy | ||||
|---|---|---|---|---|
| Changed order more often | Agree | Disagree | ||
| Agree | 935 | 89% | 16 | 41% |
| Disagree | 121 | 11% | 23 | 59% |
2.7 Adult Coeliac Disease Health Check
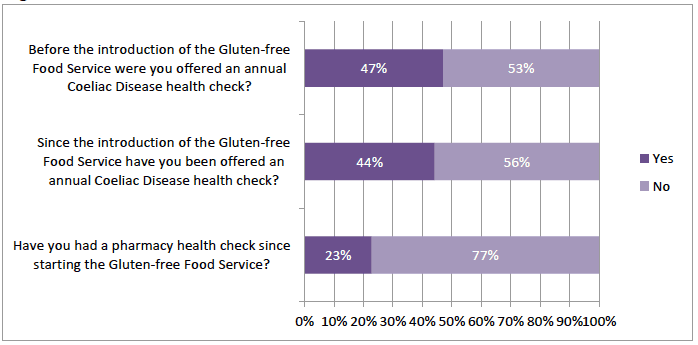
The survey contained a section on health checks for people with coeliac disease and there were 1398 responses to these questions. There was a fairly even split as to whether respondents had a health check. 47% (n=658) were offered an annual Coeliac Disease Health check prior to the GFFS and 44% (n=618) since the introduction (Figure 2‑3). This fell to 23% (n=325) that had actually had a pharmacy health check since commencing the GFFS. There were 10% (n=126) that reported needing onward referral to another health professional. These numbers suggest that this question was answered by more than those who had received a pharmacy health check.
Figure 2‑3 Coeliac Disease Health Checks
2.8 Analysis of patients comments
This section reports analysis of 962 respondents' additional comments made in the survey. These were primarily on the GFFS system, and most of the remainder were on six overlapping themes:
- Frontline services
- Administration and other process
- Choice of food
- Formulary lists - differences between health boards
- Costs and affordability of gluten-free food
- Units awarded
Respondents also raised general issues and provided a range of practical suggestions for the service.
2.9 GFFS system generally
Over 330 respondents who provided comments supported the new services. Some were very enthusiastic and wholly positive, others liked the arrangement overall but suggested potential improvements that are outlined below. Fewer than 30 respondents who gave written comments, disliked the new service, the primary reasons for this were; they found it less convenient or disputed their unit allocation.
2.10 Frontline services
Most respondents reported a good service from their pharmacy and were happy with the new arrangements. They received help and support from the pharmacist and though it was an efficient and worthwhile service. It was generally described as easy to use.
The vast majority that gave comments were very positive about the Community Pharmacy service. Respondents generally found it was easier to visit their local pharmacy since they could go at a time that suited them without needing an appointment as with the GP. Choose which pharmacy to use which was particularly convenient for working persons, although for others the "office" opening hours were not convenient.
Some commented that they felt more in control of their diet and lifestyle as a result of the new service. They were more inclined to try a variety of products since it was easier to change monthly orders. In addition several noted that they had been given helpful advice from pharmacy staff on products. There were positive comments about the flexibility offered by pharmacies and staff readily available to answer questions and provide advice.
"Ability to use community Pharmacist is easier and less time consuming. It provides greater flexibility to allow me to try alternative products."
Respondents also appreciated that the service freed up their GP's time. There were a number to the effect that their view was providing repeat prescriptions for gluten-free products was not best use of GP's time and resources. Indeed under the previous arrangements, they had not made appointments with their GP because they thought it was not good use of GPs time. Therefore they did not change their prescription or seeks advice on products. The GFFS was seen as a better use of local health services and allowed GPs to spend more time with other patients. The comments illustrate there is no desire to have the service transferred back to GP practices.
"This is a service that does not need to be undertaken by the GP so should free up some of their time."
"It is excellent and makes ordering food very easy without bothering the GP."
There were difficulties in practice reported. A small number of respondents had encountered problems in trying to change the pharmacy they used for GFFS. Some experienced slow transfer when they had moved area and one respondent case reported a month without food on prescription as a result. Moving from the GP to the GFFS could be problematic and there were reports of patients needing to negotiate between the GP and pharmacist. One respondent was told that they were required to remain with the pharmacist they had registered with although they were dissatisfied with the service. A few respondents reported communication difficulties between their GP and pharmacist or some lack of GP awareness of GFFS.
Some mentioned inconvenience getting to the pharmacy to hand in order forms due to their work hours. A solution proposed was introduction of a drop box or other out of hours box. Others to mentioned previously they use one system, it now involves two contacts; (i) GP for repeat prescriptions for medicines and; (ii) Pharmacist for gluten-free foods. Those with more complex food allergies and intolerances had also found the new service difficult to use. Finally, there was mention of the difficulty in discussing issues in confidence in a busy pharmacy.
2.11 Administrative and other processes
A wide range of comments were given on administrative and the service process, but the positive comments clustered under three themes; easier and more flexible system; more straightforward way to change the content of orders and reduced use of GP time.
Many respondents reported they found the GFFS easy to use. The reasons given included that access to a pharmacy was straightforward, the forms are simple to complete and the order can be collected within a couple of days. Being able to complete the order form at home was seen as beneficial. Others noted the GFFS was clear, flexible and a quicker in comparison to previous system.
Largely as a result of the ease of the arrangements, respondents noted that it was simpler to change the order in the GFFS. In part this was due to the administrative arrangements, for example the list of the products available attached to order forms was reported as helpful. For many the removal of the GP from the process was the other main reason for finding the system easier i.e. changes could be made through dropping off a form at the pharmacist and no longer necessitated an appointment with a GP or speaking to the surgery. Many recognised and supported the mutual benefits in being able to obtain gluten-free food without taking up GP time and GP time not used for prescribing foodstuffs.
"I would very much like for this service to continue as it is so much easier to place my order with the pharmacy using the forms and it saves me involving my GP whose time would be better spent seeing patients."
It was common for respondents to report they tried more new foods because it was easier to change their order, and because they knew there were not then committed for a period. This gave flexibility to try products to find which they liked best. Consequently people were using a greater variety of new foods. The information given on the products available also supported people trying new foods and generally more variety in products ordered.
Many believed that there were also indirect improvements resulting from the GFFS. More effective use of resources was mentioned, such as reduced food waste, as a result of the flexibility in ordering. For some the GFFS had reduced the number and length of trips for ordering and collecting food that produced environmental benefits. This could be the case in rural areas, where the pharmacy was nearer than a GP. The following quote below illustrates many of the points made on these themes:
"I think it is a very useful and easy to use service. I hardly ordered anything before as I felt it was a burden on the doctor to be constantly changing prescriptions based on what I need and doctors are overworked as it is. With the new service, I have been able to try different things at my leisure and decide what works for me. I vary what I order from month to month and don't waste food by working out what I need and when. It is simple to complete the form and hand into the pharmacy. Having the list with the pip codes makes the choices available much clearer, and possibly if I had had this list when ordering prescriptions prior to the new service, it would have been an easier process. Not knowing what points were allocated to each time, meant I would have to pester doctor to put a simple order in. I think the new system is far superior, but would be interesting to know if it costs the NHS more or saves money. Thank you."
There were also respondents who were not entirely content. For some people the new system was more cumbersome due to various reasons. The requirement to complete a monthly order form even when no changes were made was questioned. The necessity of completing a hard copy form in person, with no on-line option was a source of complaint, although some respondents did seem to be able to email orders to their pharmacist. In one example, under the previous system individuals had been able to telephone or email the GP for a repeat prescription. Now a trip to the pharmacist in person to submit an order in hard copy was required. It was suggested that an email or online ordering system would be useful for GFFS.
"The service would be much easier to use online. As it is I have to fill in a blank template paper form each time I want to make an order and physically take it to the local chemist's. Then I have to go again to pick up the GF items (which I would have to do using an electronic ordering system). I also need regular medical repeat prescriptions from my Dr so that requires another, separate, trip to the Chemist's to collect. An online ordering system would cut out one monthly trip to the chemist and make monitoring much easier. I'd also be able to select favourite items, instead of handwriting out all the information every time."
In some cases, forms were completed in the pharmacy and some patients felt pressure to make the selection quickly. These irritations were compounded by the style of the form that required the order and PIP codes to be completed each time. One proposal was for a pre-printed form with the core items. This could avoid the necessity of looking up PIP codes and points values and make calculation easier. Another proposal to improve the order system was inclusion of pictures of the goods with the order form. This could also help deal with a problem for some people that arose from the lack of information on the product list on the weight and amount of food. This was confusing and the source of waste. Finally the need to plan in advance the food that was wanted/required was disliked by a few respondents.
One recurring theme was the minimum order size, primarily for fresh bread where a single bread order was often a pack of eight loaves. Those without freezers, or small freezers, in particular found this problematic and bread would go off and be wasted. If they were not alerted the order was available, the bread and other fresh food could be near or past its use by date by the time it was collected. Proposed solutions were to be able to order less bread more often and sharing orders of fresh food.
"It is good because you have a chance to try any gf products available. It is not so good because you need a freezer to store the months supply of bread, or more to the point enough room available which is rarely the case in the household one. Also the supplies of fresh items when they arrive often have very short use by dates maybe just 2-3 days and I have had supplies past there date which the pharmacy would not take back because they said it was in date when they received it."
Storage of many bulky items was an issue for both pharmacists and patients. Transporting large and heavy items was very difficult for people without cars and the possibility of a delivery service was raised. There was differing experiences in the delivery of food as some arrived as one order and could be collected in one journey, while for others collection took several trips. One suggestion was a text message service from pharmacists when orders were ready for collection.
The fixed monthly ordering cycle did not suit all; for some this is too infrequent for the changes for others it seemed unnecessary to order so frequently. The inflexibility could be problematic, for example additional items could not be ordered to cover a holiday period.
Having accurate, up to date information on availability of products was a theme in the comments. There was some concern about how frequently the list of products was updated and whether new products would be added to the list. It was proposed that new food be added more regularly to the list. There were also a number of comments about supply difficulties where the pharmacy could not order, or did not receive, requested products. Several respondents reported supply problems, missing items or a lengthy wait for products to arrive or incorrect orders.
"It was a nightmare to set up, no one knew what they have to do. The forms weren't easy. The pharmacy doesn't update the list of products available free. Not really set up as it should."
Whilst there was not a problem with this service, some expressed a preference for obtaining food form a supermarket and wondered if a vouchers system could be introduced.
2.12 Choice of food
A number of respondents were very positive about the range of gluten-free food and thought there were more products available on the NHS; others thought the range of choice too limited. There was a view from many that there was more limited choice that they had experienced when previously receiving gluten-free food via a GP prescription. Many respondents stated the names of particular brands or products that they would like to see available through the GFFS. There was no clear consensus with this and a very wide range of different products were mentioned as personal preferences.
"Good range of products though inevitably there are a few things I like which are not available."
"The choice is fairly limited and I am not keen on a lot of the products on offer."
There was some potential for confusion with information about new products that were available through the GFFS. Some stated that they were unsure if new items would be added to the list of prescribable products and how they would find out about any additions or changes.
"I wish they would introduce new items to the list and update it every so often as it gets a bit repetitive."
There were some comments that the products available through the GFFS were less palatable than gluten-free food available in supermarkets. Several respondents noted that biscuits and cakes were not available and were of the view that they should be included. Those with other food allergies found it particularly difficult to find suitable products and there were calls for better nutritional information about each product to help inform choices. There was also a suggestion that there should be a wider choice that would appeal to children.
2.13 Formulary lists - differences between health boards
There were comments on the variation between Health Boards on the gluten-free products permitted and this overlapped with feedback on the produce choice more generally. Some respondents wondered why it was that some products were available on some health boards' lists but not others. There was questioning of the variation in the availability of types of items, e.g. biscuits; or a brand of a food. There was an example where the respondent's experience was differing units allocated for the same item in two areas, meaning they received less food. Solutions proposed were; to have a Scotland-wide list or the full Coeliac list and/or include all foods with a PIP number. A perceived lack of user involvement in drawing up the list was raised and it was felt this should be improved in the future. The quote illustrates the points outlined:
"Although I like the new service, I am not very happy with the choices available. Some reason NHS X have drastically reduces the choices of gluten-free foods, in comparison with other regions. I have checked out the choices available to other regions. NHS X have 2 pages of choices, whereas other regions have 5 or 6 pages, and some with even more (9/10 pages for one region). I feel this is very unfair, and some foods that I was able to have through my doctor are now no longer allowed. Is there any way to find out why NHS X have done this?"
Respondents reported both more and less choice than under the previous system, but these did not prevent support for the new system overall.
2.14 Cost and affordability of gluten-free food
Given gluten-free food can be expensive a number of respondents noted that receiving the food on prescription was important. If all food had to be purchased diet adherence would be difficult and trying new foods would be less likely. Some respondents found their supply adequate. For many, there was a need to supplement items provided by GFFS by purchasing additional food from supermarkets. Given gluten-free food is higher in price, several respondents stated that the GFFS was important in providing them with the basic foods. Another suggestion was to increase units on the GFF system or restrict the price of gluten-free food.
"So grateful for this service as our food is so expensive in the shops. Now I can have the basics on prescription and it allows me a bit more variety."
Views seemed split on the type of products that should be available. For some, non-basic food such as biscuits and cakes should be on prescription because these are expensive; prohibitively so for some respondents. For others basic food such as bread, pasta and flour were the priority for prescription.
"This type of food is somewhat restricted - no biscuits or fruit loaf or cakes but I can understand the logistics must be pretty horrific. The choice is adequate and from a financial point of view it is great. I purchased GF Food until I was informed about GFFAPS and the savings are considerable."
2.15 Units awarded
Respondents had differing opinions on the points allocated. For some it was adequate, indeed one reported they were sufficient to feed a family and was concerned the system is open to abuse. For others the unit allocation was insufficient. Some made specific cases; such as an individual who worked on a building site and was really restricted to taking sandwiches so most of their units were used on bread. One proposal was to be able to rollover unused units to the next month since some people did not use their allocation every month. Some also proposed that there are transferred to cash to spend on commercial gluten-free products.
2.16 General Issues
There were more specific issues raised, generally by one or a few respondents. A group of respondents reported that GFFS played a part in them managing their condition. One parent pointed out their 13 year old child could now choose their own food and this supported their learning for future self-management of the condition.
The issue of diagnosis was raised, both being diagnosed and the length of time this could take. Whilst there was support for the service and consequential reduction in GP time, a note of caution was sounded to ensure that this did not impact on diagnosis. It was also queried as to whether the service should be expanded to people who are wheat intolerant.
One respondent found an NHS list reassuring of quality and had negotiated with their pharmacist to supply other additional items not readily available that the patient then paid for.
There were respondents who only first heard of the service through the survey and one who had checked with their pharmacist who was also unaware. Another asked why the service was limited to adults, although this is not the case.
2.17 Health Checks
Respondents expressed differing views on who should carry out a health check; pharmacist; GP, coeliac nurse specialist or a dietician. Some respondents had doubts as to whether the Pharmacist had the skills or suitable venue to take blood and thought that this needed to be done as an individual service by a dietician or GP. Others thought it sensible, and that pharmacists are well able to deal with standard blood tests for people with coeliac disease. Indeed one comment proposed this would reduce much duplication in the current system:
"The annual check the pharmacist provided was identical to the annual check my GP provides except that the GP also requests the bloods. It doesn't make sense for the pharmacist to complete 95% of the review, only for the GP to replicate it a week later."
Comments indicated that patients often had not been offered an annual coeliac health check. Some were aware that this existed but others had not heard of it. In one case, the Pharmacist had advised an individual to contact their GP if they had any problems, and this left the individual with the responsibility of booking a regular health check. Some confusion was apparent around who would now conduct blood and bone density tests, and when these tests would occur. There was also mention of lack of contact with hospital nurses.
2.18 Practical Suggestions
There were a number of suggestions about how the GFFS might be improved. The most common suggestion was that the order form should be made electronic so that it could be completed online and emailed direct to the community pharmacy. There were also calls from a few respondents for the GFFS to be replaced by vouchers or a card for gluten-free food that could be used at supermarkets. There were several complaints about multiple pack sizes requiring orders of 8 loaves at a time and the resulting waste.
Other suggestions included:-
Order form
- A simpler text only order form without bold headings so that it uses less printer ink
- More space on order form for writing in PIP codes
- Pre-printed form with details previous order to save writing out item name, PIP codes etc each month
- Add tick boxes to order form
Order process
- Email confirmation/ text message from pharmacy to advise order is ready for collection
- Ability to place phone order with pharmacy to save two visits
- Ability to order a two month supply at one time - more convenient for holidays and also for freezer/storage space
- Enable rollover of unused units to the next month - this would enable less frequent ordering e.g. a larger order every three months
- Patients to retain own copy of list of products available so can decide orders at home
- Provide patients with updated list of products when new items are added
- Quicker delivery times to pharmacy, particularly for fresh bread
- Home delivery
Food
- More choice and variety
- Add seasonal items such as at Christmas
- Suggestions to add specific named products to the list of available foods.
- Smaller samples to try different products without a lot of waste
- Better information about the products available e.g. nutritional information, weight - in advance of ordering them
- Pictures of the foods available to assist decision making
- Make it a national service instead of a service that varies by Health Board.
3. Survey of Community Pharmacists - Analysis and Findings
3.1 Main findings
The three main findings from the survey of community pharmacists are:
The majority of community pharmacists reported a positive experience with GFFS and support its continuation. It is an easier system and can bring savings.
Community pharmacists reported the GFFS had improved service to patients.
Practically all agreed there should be an IT solution to replace writing Community Pharmacy Urgent Supply (CPUS) Forms by hand.
Almost half had carried out health checks and this was beneficial in patient engagement, it can be time consuming and can involve raising sensitive issues.
A minority found the service had improved relations with wider healthcare team.
3.2 Introduction and Respondents Profile
Community pharmacists' views and experience of the Gluten Free Food Service provided as an Additional Pharmaceutical Service (GFF APS) were gathered via on-line survey. This comprised 40 questions on the service covering: experience; views on patients' experience; the impact of the service; views on the Adult Coeliac Disease Health Check and core factual information. This section reports the findings from the analysis of the 367 responses from the survey electronically via Health Boards and Community Pharmacy Scotland to approximately 1250 community pharmacies.
A total of 358 (98%) of the respondents provide the GFFS service. The spread of responses are generally in line with the populations covered by the health boards, with most responses returned from Community pharmacies in Greater Glasgow; Lothian, Grampian and Lanarkshire (Table 3‑1).
Table 3‑1 Which NHS Board do you usually work in?
| Health Board | Population | % of pop | Response % | Response n |
|---|---|---|---|---|
| Ayrshire & Arran | 372,210 | 7.0% | 5.5% | 18 |
| Borders | 113,870 | 2.1% | 3.4% | 11 |
| Dumfries & Galloway | 150,270 | 2.8% | 0.9% | 3 |
| Fife | 366,910 | 6.9% | 7.0% | 23 |
| Forth Valley | 299,680 | 5.6% | 9.2% | 30 |
| Grampian | 579,220 | 10.9% | 12.8% | 42 |
| Greater Glasgow & Clyde | 1,137,930 | 21.4% | 18.3% | 60 |
| Highland | 321,000 | 6.0% | 5.2% | 17 |
| Lanarkshire | 652,580 | 12.2% | 11.6% | 38 |
| Lothian | 849,700 | 15.9% | 15.0% | 49 |
| Orkney | 21,570 | 0.4% | 0.0% | 0 |
| Shetland | 23,200 | 0.4% | 0.3% | 1 |
| Tayside | 412,160 | 7.7% | 10.7% | 35 |
| Western Isles | 27,400 | 0.5% | 0.0% | 0 |
| 5,327,700 | 100% | 100% | 327 |
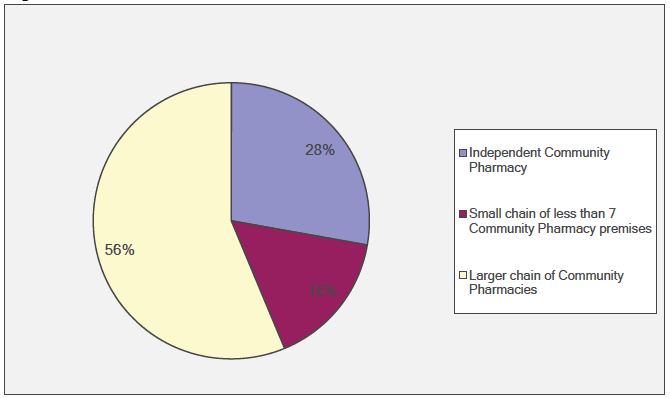
Most of the respondents were from community pharmacists (97%; n=315) and the remaining 3% pharmacy technicians (n=9), although 43 respondents (12% of the total) did not answer this question. In this report the term "community pharmacist" is used for all respondents. The largest group (56%; n=184) worked in larger chains of pharmacies, followed by independent community pharmacies (28%; n=91) and the fewest respondents worked in small chains, of fewer than seven, pharmacies (16%; n=52) (Figure 3‑1).
Figure 3‑1 Usual Place of Work
3.3 Community Pharmacist Experience
The majority of community pharmacists reported a favourable experience of the GFFS. A total of 82% (n=279) agreed that their overall experience of GFFS had been positive. 88% (n= 301) agreed it was "easy to implement" and 82% (n=283) it was "easy for my pharmacy staff to place patients' orders for GFF" (Figure 3‑2).
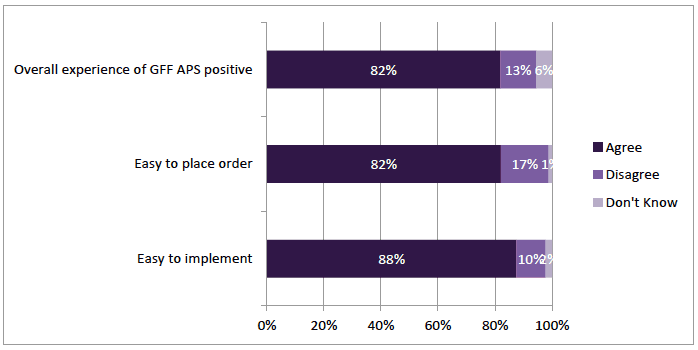
GFFS was preferred to the previous service; most respondents, 76% (n=262) disagreed with the statement: "I prefer patients to order their GFF via GP prescription" (Table 3‑2). There were 17% who agreed (n=59) and 6% responded "Don't Know" to the statement.
Table 3‑2 Response to statement "I prefer patient to order their GFF via GP prescription"
| Agree | 17.2% | 59 |
|---|---|---|
| Disagree | 76.4% | 262 |
| Don't Know | 6.4% | 22 |
The following illustrates the positive aspects of the service for community pharmacists:
"very good service, patients have given a very positive response and are finding it easier to order and change their GFF orders than with GPs"
In the opinion of the majority of respondents, 92% (n=300), GFFS should continue as an ongoing service (Figure 3‑3). In all Health Board areas the majority wanted the service to continue. The responses from the following Health Boards had the most, although still a minority, respondents who did not want the service to continue; Lanarkshire 25% (n=7) and 18% (n=5) in Greater Glasgow & Clyde and Tayside. Where reasons were offered, these questioned whether the NHS should be giving food on prescription and whether it was a good use of time for a healthcare professional. Where this was accepted, there were suggestions to issue vouchers that could be used at supermarkets instead. The following quote illustrates the points made:
"The NHS should not be funding food for coeliacs. Other patients with allergies have to buy their own goods (eg lactose intolerant patients."
Figure 3‑3 In your opinion should the trial GFF APS continue as an ongoing service?
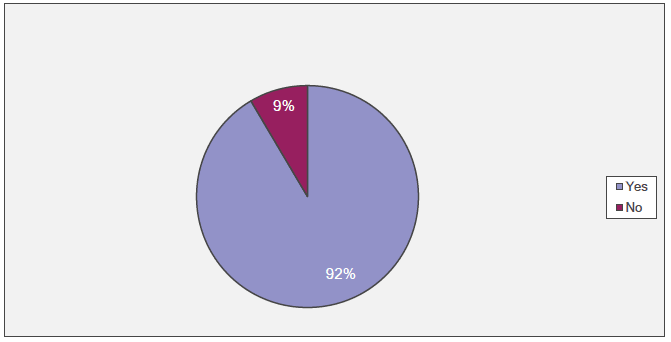
Other comments indicated that the providing the service was additional work; time consuming, although it alleviated GPs time, and the storage of goods could be problematic.
3.4 Community Pharmacist View on GFFS Impact for Patients
There had been an improvement in the services for patients in the view of the vast majority of pharmacists. Around 9 in 10 agreed "it is easy for patients to receive their monthly order of GFF with the pharmacy" (93%; n=313) and that order receipts are faster (86%.; n=288) (Figure 3‑4).
Figure 3‑4 Pharmacist View of Service for Patients
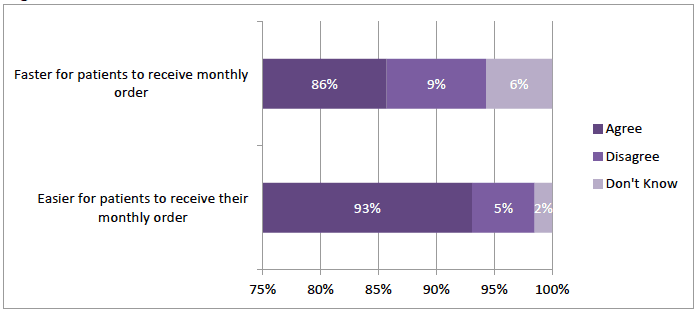
Over 9 in 10 respondents thought that the service made it easier for patients to change their GFF order (Figure 3‑5). A majority, albeit fewer, 67% (n=222) agreed that patients were changing their orders more often and 79% (n=270) reported that "patients using the GFF APS are trying out different gluten-free foods". However 20% (n=66) disagreed that patients were changing their order more frequently and 13% (n=43) did not agree that they were trying different foods (Figure 3‑5).
Figure 3‑5 Pharmacist View on Changing Order
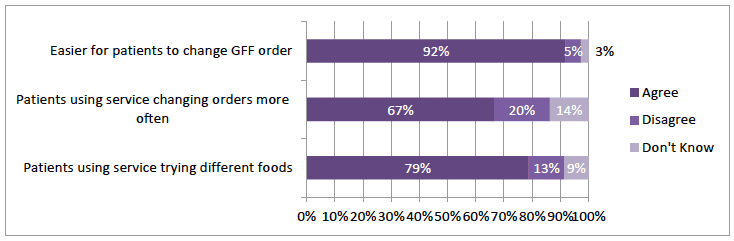
The survey had a series of questions on the impact of the GFFS service. A large majority (94%; n=316) agreed the community pharmacy is contributing to healthcare through this service (Figure 3‑6). There were 84% (n=283) who agreed that the GFFS helped the pharmacy improve service to patients and 85% (n=287) that "I have better interaction with patients". In response to both 10% of respondents (n=34 and n=33 respectively) disagreed (Figure 3‑6). The following comment illustrates the broader benefits reported:
"I think the GFF service is a very good concept as it takes a workload off the GP, allows customers to have more control on what they want to order and pharmacists have more opportunities to interact with patients."
Figure 3‑6 Impact of GFF on Service
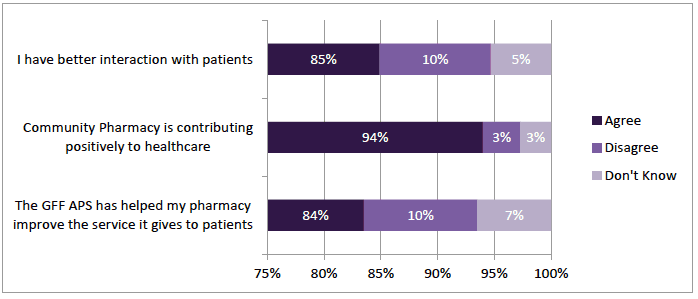
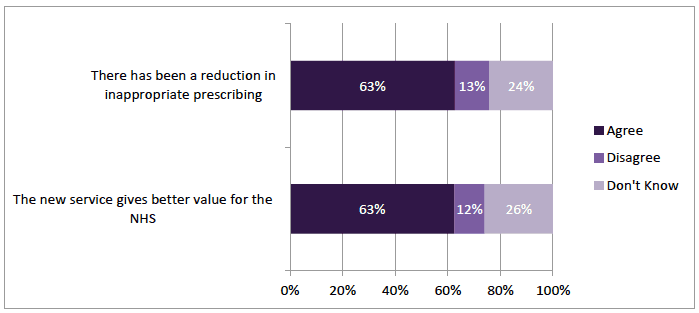
Two questions invited pharmacists' views on the effect GFFS had on reducing costs and providing value. A majority, 63% (n=212) agreed that "there had been a reduction in inappropriate prescribing" and the same percentage that the "the new service gives better value for the NHS" (Figure 3‑7). Nearly one quarter (24% n=82; 26% n=88 respectively) responded "Don't Know" to these questions and only just over 10% disagreed (13% n=44; 12%, n=39).
Figure 3‑7 GFFS Impact on cost effectiveness
The following comment illustrates many points:
"I am totally in favour of this service continuing. I have found an increase in patient confidence, reduction in waste and an increase in my confidence in being able to care for my patients. I have produced my own GF order forms and a CPUS template to print prescriptions. My main concern is how best to record what I am supplying, points wise, to my patients to prove I am remaining within the constraints of the system. The GP practices I serve, are very happy with pharmacy doing the GF service as more often than not, the wrong items were prescribed leading to GF foods being wasted, new prescriptions issued and delays in supply to my patients."
Community pharmacists (83% n=281) agreed with the statement that the service supports patient self-management; and only 9% (n=29) disagreed (Table 3‑3).
Table 3‑3 GFFS supports patient self-management
| Answer Options | Response Percent | Response Count |
|---|---|---|
| Agree | 83% | 281 |
| Disagree | 9% | 29 |
| Don't Know | 8% | 27 |
One aim of the service is to support improved collaborative working, and the survey asked if "relations with the wider healthcare team (e.g. dieticians) had been improved as a result of the service". Just over half, 54% (n=182) disagreed with the statement; 30% replied "Don't Know" (n=99) and only 16% agreed (n=55) (Table 3‑4).
Table 3‑4 Relations with the wider healthcare team improved as result of the service
| Answer Options | Response Percent | Response Count |
|---|---|---|
| Agree | 16.4% | 55 |
| Disagree | 54.2% | 182 |
| Don't Know | 29.5% | 99 |
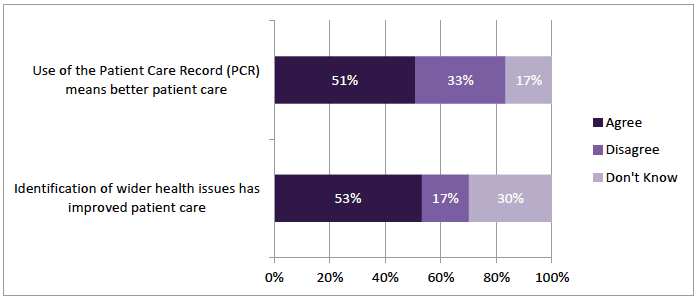
Views were more divided as to whether the service had contributed to holistic care. There were 51% (n=170) of community pharmacists that agreed "use of Patient Care Record (PCR) means better care" but 33% (n=109) disagreed (Figure 3‑8). Similarly 53% (n=178) agreed that "Identification of wider health issues has improved patient care" and whilst only 17% (n=57) disagreed; 30% (n=100) "Don't Know".
Figure 3‑8 Improved Care: Patient Care Record & Identification Wider Health Issues
3.5 Improving Provision and Process
One set of questions probed how the provision of GFFS could be made easier for community pharmacies. There were a series of statements that asked about IT and patient transfer; and two questions on a single food list and whether items should receive out of pocket expenses.
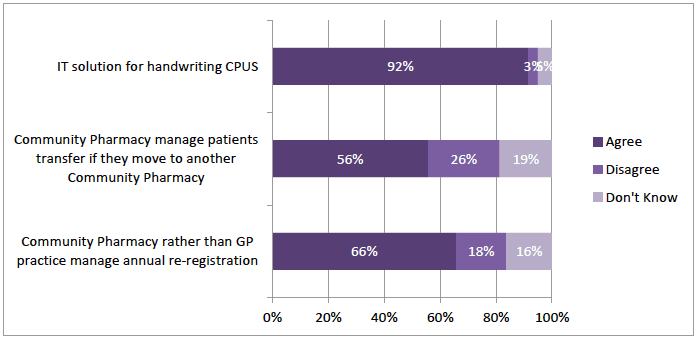
A majority agreed with the statements that community pharmacy rather than a GP practice should manage annual re-registration (66%; n=220) and transfer from another community pharmacy (56%; n=187) (Figure 3‑9). The overwhelming majority agreed that there should be an IT solution for CPUS (92%; n=308). Respondents' comments supported this and many proposed an IT solution was a requirement for the service. Without it the process was very time consuming, and that was time that could be spent with patients.
"Paperwork extremely time consuming, writing up order forms as most patients don't, then writing and copying CPUS, as well as labelling in PMR"
Figure 3‑9 Make Provision of GFFS easier
A large majority of respondents agreed there should be a single Scottish food list (86%; n=286) and an even higher number agreed that no items should require out of pocket expenses (OPE). (91%; n=305) (Figure 3‑10).
Figure 3‑10 Make Provision of GFFS easier: Single Food List and No OPE
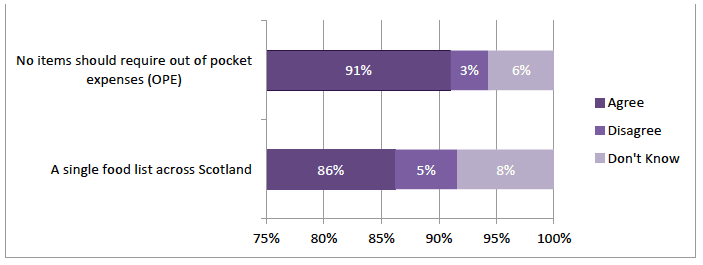
Views were more divided as to whether the variation between health board lists affected service to patients. The largest group (43%; n- 144) disagreed this was the case but almost one third agreed (32%; n=107) and one quarter (n=85) didn't know (Table 3‑5).
Table 3‑5 The variation in HB food lists affects my service to patients
| Answer | Response Percent | Response Count |
|---|---|---|
| Agree | 31.8% | 107 |
| Disagree | 42.9% | 144 |
| Don't Know | 25.3% | 85 |
3.6 Training and Support for GFFS
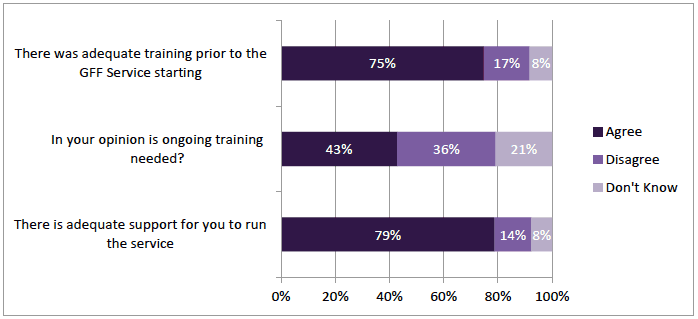
There was a generally positive view on training and feedback from community pharmacists for the GFFS. 75% (n=243) agreed that prior to the service commencing, there was adequate support and 79% (n=256) there is adequate support to run the service (Figure 3‑11). On whether ongoing training is needed, opinion was more split; 43% (n=140) agreed and 36% (n=119) disagreed and 21% (n=68) replied "Don't Know" (Figure 3‑11).
Figure 3‑11 Service Implementation - Training and Support
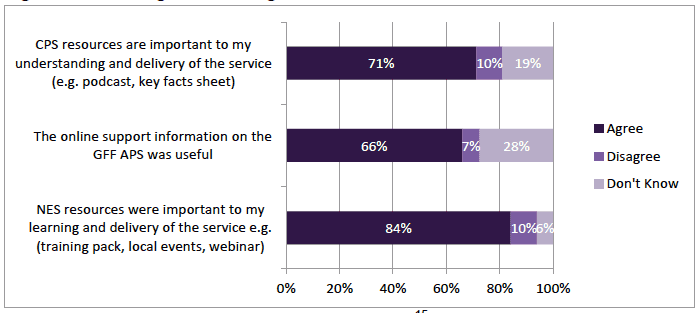
84% (n=274) agreed that NES resources were important to community pharmacists' learning and delivery of the service. 71% (n=233) agreed CPS resources "are important to my understanding and delivery of the service"; although 10% (n=32) disagreed and 19% (n=62) replied Don't Know (Figure 3‑12). In a similar pattern 66% (n=214) agreed the online support information for GFFS was useful; 7% (n=21) disagreed and 28% (n=89) replied Don't Know (Figure 3‑12). This may be because they were not sure of the impact of the training or it may be that they are indicating they are unaware of the training and support.
Figure 3‑12 Training and Learning Resources
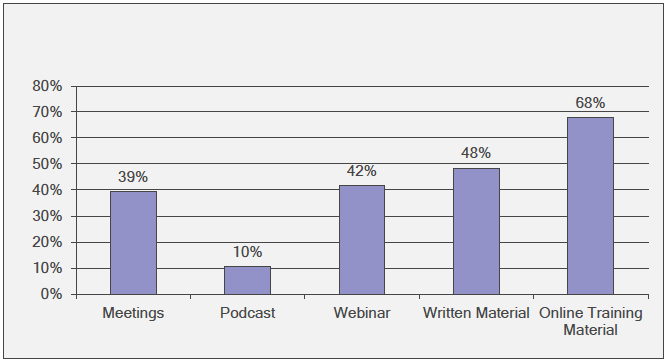
Those who thought additional training was needed[15] were asked how they would want this delivered and given five options. The single highest group preferred online training material (68%; n=143) followed by written material (48%; n=102) and webinars (42%; n=88) (Figure 3‑13).
Figure 3‑13 If additional training is needed, how should it be delivered?
3.7 Adult Coeliac Disease Health Check
There was a fairly even split between community pharmacists who had undertaken any adult coeliac disease health checks; 49%; (n=160) had and 51% (n=169) not.
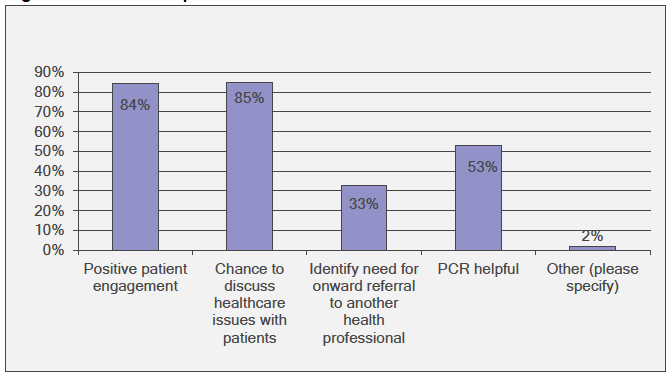
Those who had undertaken the health checks were asked about the positive and negative aspects. They were given stated options and asked to select all that applied and give any other reasons. On the positive side, the majority thought that this offered an opportunity for positive patient engagement (84% n=133) and a chance to discuss healthcare issues (85%; n=134). One respondent stated this contributed to patients' awareness as to what pharmacists can offer (Figure 3‑14).
Figure 3‑14 What was positive about the adult coeliac disease health checks?
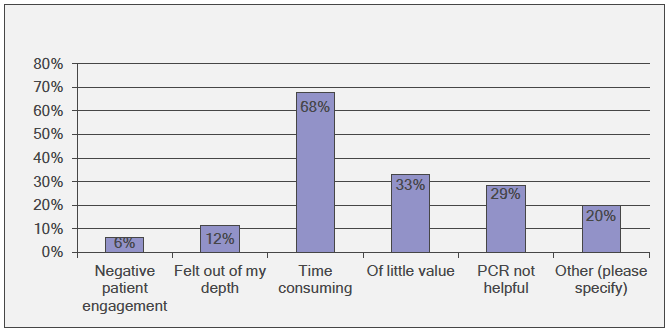
For the negative aspects, the majority (68%; n=88) selected "Time consuming". Otherwise views were more spread between the following reasons; of little value 33% (n=43) and PCR not helpful ( n=37) (Figure 3‑15).
Figure 3‑15 What was negative about the adult coeliac disease health checks?
One fifth (n=26) gave other reasons that fell under the following themes.
Too basic for patients with coeliac diagnosis for many years
The PCR system is not efficacious and there were IT problems
Difficulties in gaining patient participation due to: individual not collecting own prescription; reluctance to discuss weight; lack of knowledge about the service
community pharmacists lacking knowledge on other monitoring tests, requesting a more concise ''flow chart'' since not doing regularly and time pressures.
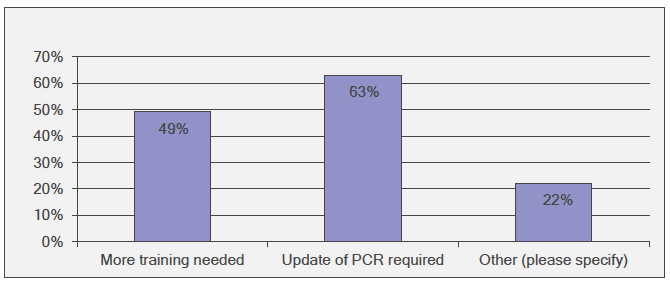
One improvement that could be made to the health check seemed to be updating the PCR. A majority (63%; n=77) of those responding to this question gave this answer, and this is 21% of the total survey respondents (Figure 3‑16). The open comments echoed this with many raising the issue of the operation of the PCR; specifically that it should interface with the pharmacy Patient Medication Record (PMR). 49% (n=60) agreed that more training was needed. Comments also proposed making prescription process more effective through IT. Others proposed using more specialist skills; e.g. coeliac clinic and dieticians.
Figure 3‑16 How could Adult Coeliac Disease Health Check be made better?
3.8 Comments from Community Pharmacists
This section reports on the comments from community pharmacists primarily to add to or include those covered in the earlier sections.
Most pharmacists were supportive of the GFFS, although many called for the system to be streamlined particularly to transfer as much as possible to an on line system. Indeed a few commented that their support for the service was contingent on it becoming electronically based and eradicating much of the current need for manual processing. This was the case with prescriptions but was also raised in relation to the process for sourcing and ordering stock i.e.:
"The service has been a positive one but it needs to be streamlined as currently we are tripling our workload by - ordering the stock by pipcode as descriptions don't match computer - labelling the stock so it goes through PMR - handwriting the Rxs It could surely be done a lot easier by using the PCR???"
Comments were made to the effect that patients liked the service and were using the pharmacist's expertise and flexibility to change their order more often.
"Patients prefer this service. They can easily try new products/brands. They appreciate our input with suggestions about what other patients have tried and liked."
The wider and knock on effects were raised:
"I think the GFF service is a very good concept as it takes a workload off the GP, allows customers to have more control on what they want to order and pharmacists have more opportunities to interact with patients."
The supply chain was the subject of a range of comments. The availability of items was problematic as was the time delay in delivering fresh products. Dealing with a number of suppliers could be very time consuming and it was proposed that choice in core products could be reduced. One comment was critical of the delivery costs that are borne by the NHS. The formulary list updating could also be improved.
There were views that staple foods only should be supplied since biscuits, for example, were contrary to the NHS health messages. The issue of storing and wastage of fresh food was raised:
"It's good that it takes time away from gps however i do feel fresh bread should be excluded as many don't bother to pick it up even after a phonecall also many patients get bags of items making storage very difficult. I now trip over bags as nowhere to store them. I think maybe vouchers in retail to subsidise prices or charges to prescriptions rather than it all free. Maybe then less wastage esp fresh bread"
Moving more, or even all patients into the service was a theme that emerged and there were various reasons for this. One commented that GPs should be given active encouragement to do so. There was also a proposal that this could be a template for chronic disease management, responsibly for which could lie with pharmacists.
"all ongoing chronic disease management should be carried out in the pharmacy (but will require extra resource, training and funding). However this would provide best value for money and an improved service"
One suggestion was that it should be compulsory to use the service to reconcile the different foods and quantities that people could receive via GPs.
"I think it should be mandatory for all patients to be on the service as its not fair that some patients are limited to amounts and others are not and leave with 4 times the allowance of someone else."
One community pharmacist was seeking more patients on to this service, particularly to improve value given the investment in training they had made and received to prepare to deliver it.
A couple of respondents suggested a voucher scheme with supermarkets as an alternative arrangement.
There was some difference on the basis of payment for the service with comments supporting the status quo but others suggesting it should relate to the number of patients registered. The inequity of the same payment for one or 25 patients was raised.
4. Survey of GPs - Analysis and Findings
4.1 Patient Responses
This section contains the findings from the survey of GPs. The questionnaire was issued electronically via Health Boards and the Scottish General Practitioners Committee of BMA Scotland to approximately 1000 GP practices and a total of 516 responses were received from individual GPs. The questionnaire comprised 19 closed questions on their experience and views of the GFFS service and Adult Coeliac Disease Health check and core factual information. The analysis gives the findings by those who responded to these questions. Around one quarter of respondents gave additional comments in the free text box. These are included as Illustrative examples in relevant sections and at the end of the chapter.
4.2 Main findings
The three main findings from the survey of GPs are:
The majority of GPs who responded support the GFFS service and found it to have benefits and want it to continue
Although most GPs agree with the statements on the positive impact for patients, a sizable minority responded "Don't Know".
The majority did not know the effect or value of the Adult Coeliac Health Check.
4.3 Profile of Respondents
The spread of responses are generally in line with the populations covered by the health boards, with most responses returned from GPs in Greater Glasgow and Clyde; Lothian, Lanarkshire and Grampian (Table 4‑1).
Table 4‑1 What NHS Board area does your GP practice reside?
| Answer Options | Population | Percent of population | Response % | Number of responses |
|---|---|---|---|---|
| Ayrshire & Arran | 372,210 | 7.0% | 6.9% | 35 |
| Borders | 113,870 | 2.1% | 5.5% | 28 |
| Dumfries & Galloway | 150,270 | 2.8% | 2.2% | 11 |
| Fife | 366,910 | 6.9% | 4.1% | 21 |
| Forth Valley | 299,680 | 5.6% | 11.0% | 56 |
| Grampian | 579,220 | 10.9% | 9.4% | 48 |
| Greater Glasgow & Clyde | 1,137,930 | 21.4% | 22.8% | 116 |
| Highland | 321,000 | 6.0% | 6.1% | 31 |
| Lanarkshire | 652,580 | 12.2% | 9.6% | 49 |
| Lothian | 849,700 | 15.9% | 14.9% | 76 |
| Orkney | 21,570 | 0.4% | 0.0% | 0 |
| Shetland | 23,200 | 0.4% | 0.8% | 4 |
| Tayside | 412,160 | 7.7% | 6.5% | 33 |
| Western Isles | 27,400 | 0.5% | 0.2% | 1 |
| 5,327,700 | 100% | 100.0% | 509 |
4.4 GPs experience of the GFFS
91% of GPs responding to the survey had patients who were using the GFFS (Table 4‑2).
There were 47 not using the service and the reasons given were; unaware of the service 82% (n=31); not available in their area 11% (n=4); patients do not want to use the service 13% (n=5).
Table 4‑2 Does your GP practice use the Gluten Free Food Service (GFFS)?
| Answer Options | Response Percent | Response Count |
|---|---|---|
| Yes | 90.9% | 469 |
| No | 9.1% | 47 |
Other reasons included increased workload, problems with the community pharmacist and believed it was only available in pilot areas. The areas with the highest non participation were also those with few respondents, so may be unrepresentative and should be treated with caution. These included Western Isles; Shetland; and Highland. Dumfries and Galloway; Fife; Grampian; Lanarkshire and Tayside all had 10% of respondents not participating in the GFFS.
4.5 Experience and Impact of GFFS
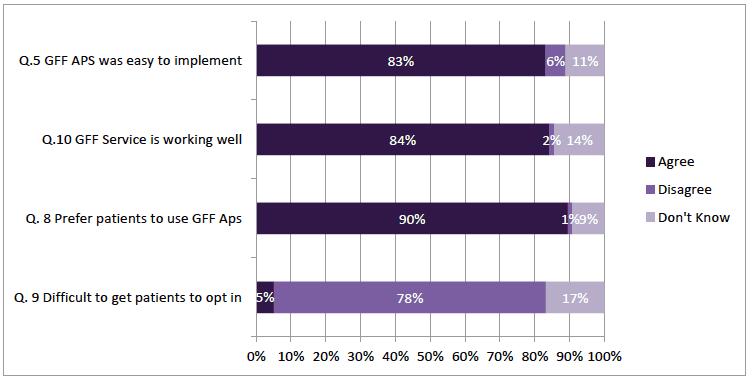
Of the GPs responding, 83% (n=398) agreed with the statement "the GFF APS was easy to implement in my practice"; only 6% (n=28) disagreed and 11% (n=53) stated Don't know. Similarly, 84% (n=390) agreed with the statement "in my experience, the GFF Service is working well" (Figure 4‑1). With regard to patients, 90% (n=426) of GPs agreed they preferred patients to use GFFS. In support of this, 78% (n= 366) disagreed and only 5% (n= 24) agreed that it "is often difficult to get patient to opt into the service[16]".
Figure 4‑1 GP's Experience of Service
There was overwhelming support (98% n= 442) for the trial GFFS to continue as an ongoing service. There was support for similar services for other Advisory Committee on Borderline Substances (ACBS) foods, with 89% (n= 403) stating they would like a similar service. However there was one note of caution in the comment box:
"extension to other ACBS food would need to meet rigorous criteria to avoid huge costs and possible inappropriate prescribing".
Respondents also proposed that a similar service could be extended to nursing homes and similar arrangement should "be introduced for prescribing devices for colostomy and catheters". Finally one comment proposed integration with the Chronic Medication Service (CMS): "It should be linked with CMS prescribing and should be able to register directly with the pharmacy."
4.6 Impact of the GFFS for GPs
Most GPs had found the GFFS to have a positive impact on their work. The majority (85%; n= 409) agreed their workload in gluten-free prescribing had reduced due to the GFFS (Figure 4‑2). Almost three quarters (73%; n=343) have had fewer disputes with patients over obtaining gluten-free food since the introduction of the service.
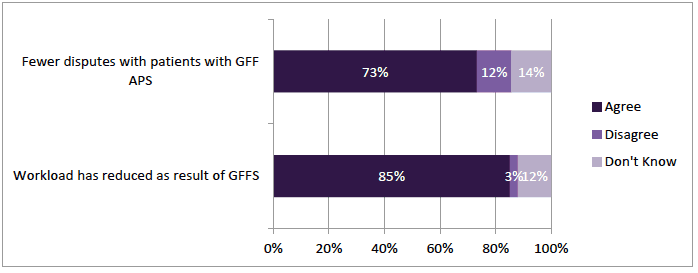
In the additional comments, there were many were general positive views on the GFFS and strong statement of support for it to continue. GPs reported the service impact, for example, it had reduced their workload in this area and this enabled them to spend time on their other responsibilities.
"This is one of the best patient care systems invented! streamlines their gluten-prescription service, more efficient for patient & professionals. Allows GPs to get on with treating illness rather than 'conditions'."
"The GFF APS has been very welcome and allows me to concentrate in other more complex health issues and workload."
It was noted that prescriptions for gluten-free food could be time consuming and not best use of GPs time and expertise.
"I cannot praise the logical and sensible person who devised this scheme. It has had huge impact on my prescribing workload.( and sanity, to boot !!! ). Withdraw it at your peril !!!"
In line with this there were suggestions for the service to be amended, from example given coeliac is a lifetime condition, removing GPs from the requirement to sign forms annually.
Some suggested that the GFFS contributed to improved quality of services for example:
"This has been a huge success. I absolutely hated doing gluten free product prescriptions before. I frequently made mistakes and certainly was very unclear about appropriate total amounts. I am sure this is far better regulated through the new system with definite cost savings to the NHS."
But for one respondent there were immediate benefits but criticism of the overall approach:
"Whilst I am happy that patients do not need prescriptions for GF foods I am unhappy that they have to do this through pharmacy. This is food we are talking about. I don't go to Boots to buy my spaghetti so why should anyone else? This is discriminatory and stigmatising."
There were views that monitoring units was also more effective, since GPs could do this effectively, and this should save money but fair and equitable. This was noted as important in that patients were provided with an improved service:
"fantastic service saving GPs a huge amount of time and giving patients easier access to foods they are entitled to get on prescription."
4.7 GPs views on impact for patient
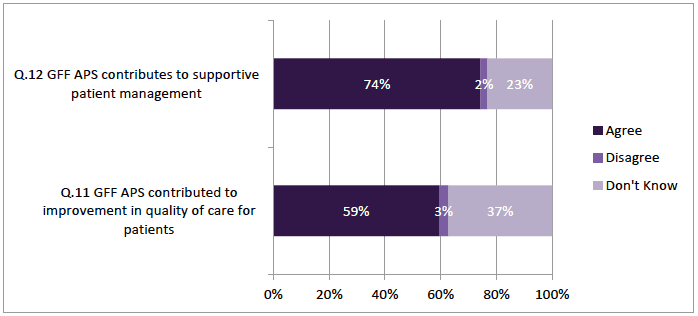
GPs responses indicate that GFFS was helpful for patients, although a sizable minority were unclear as to whether this was the case. Almost three quarters (74%; n= 345) agreed that it "contributes to supportive patient self-management" but nearly one quarter (23%; n= 108) replied "don't know" (Figure 4‑3). A majority, 59% (n=278), agreed that "the GFFS contributed to the improvement in the quality of care of patients" but over one third (37%; n= 174) didn't know if this was the case (Figure 4‑3). This indicates that there would be benefits in further research into the actual impact and outcomes for patient on such a service.
Figure 4‑3 Contribution to Improvement for Patient
A few GPs commented that patients preferred the GFFS for the reasons such as; it increased choice; delivered the products they wanted and could support self-management of the condition. However, patients had complained about the absence of certain products from the list. For other patients the GFFS should reduce waste:
"It is much easier for the pharmacy to limit the patients requests than for GPs with GF food on repeat. I suspect this will stop patients getting inappropriate quantities. A positive patient also said it allowed her to change and try different GF foods much more easily."
It was suggested that more flexibility would benefit the system, for example the GP could vary the number of units and range of foods.
Sourcing foodstuffs sought by patients was reported as more time consuming for GPs given this is not a field of expertise, so has been reduced by the GFFS.
That the GFFS is non-mandatory was problematic and the following quotes indicate a couple of practical problems and concerns:
"It has been hard to get patients to 'opt in', especially as not all preparations are on the pharmacy list. At the outset we were given different versions of the forms for registration, and this caused confusion for GP and pharmacy. It would be disappointing, after putting effort into registering people, for the system to be cancelled."
"The answers above may seem a bit confusing as we are only using the new system for new patients, so we have some using the new system but most still using the old. It was not unique in not taking GP time in transferring folks from one system to another into account, and it was a complete cop out to make it optional and leave both systems in place."
4.8 The Adult Coeliac Disease Health Check
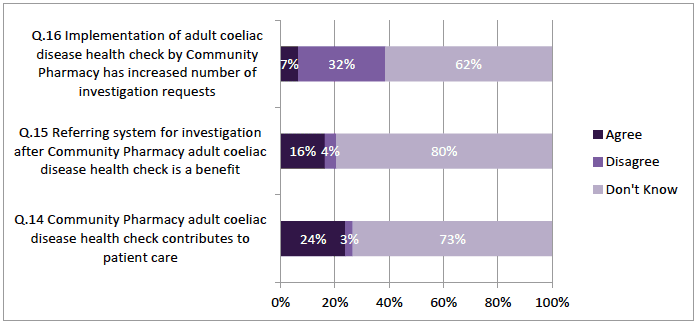
Almost one third (32%; n=148) disagreed that the community pharmacy health check had increased the number of investigation requests, 7% (n= 30) agreed, but the majority, 62% (n=284) responded "Don't Know (Figure 4‑4). In the comments there was reference to the lack of awareness of this aspect of the service. Some mentioned that they did not receive feedback from pharmacists so did not know if health checks had been carried out.
Nevertheless the majority (81% n=375) disagreed with the statement "I am concerned that there may be negative health consequences because patient who received GFF APS have less contact with a GP" and 16% (n=72) responded "Don't know" and only 4% (n=17) agreed (Figure 4‑4).
Figure 4‑4 Impact of the Adult Coeliac Disease Health Check
Comments in at the end of the survey indicated that GPs were unaware of the adult coeliac disease health check generally. It was remarked that they had not received a health check report from the Community Pharmacist which would make them aware of the services and provide information on the patient.
Occasionally GPs expressed doubt as to whether community pharmacists should be carrying out health checks.
"I was not aware that pharmacists were carrying out coeliac health checks or that they had training to do so. [I do not think pharmacy training includes non-drug disease management]."
"Completely inappropriate to carry out coeliac "health checks" without doctor contact beforehand and appropriate discussion and counselling."
4.9 Comments from GPs survey
This section is comments by GPs that relate less directly to the survey question but are relevant to the evaluation of the service.
There were views expressed that indeed GPs should not be involved in prescribing food at all. The following quotes illustrate these views, the strength in which they are expressed and where responsibility should lie:
"Would like all FOOD to be removed from medical prescribing. If a dietician wants supplementation, they can be responsible for cost effective prescribing and monitoring, working to the top of their license."
"GPs should not be involved in this process at all - amounts required should be calculated by the Gastroenterologist diagnosing the condition or dietician and GPs should merely be copied in to the decision. We have no role to play here. Patient should not be able to opt out and expect the GP to continue to prescribe. If they do not comply they should be made to buy their products - it is a waste of scarce GP time for them to be involved."
In some instances the view the NHS should not be responsible for providing such food, and that this was ineffective us of NHS funds was given.
"Do not think that health service should fund a food source for patients when other options available in supermarkets. No-one has to eat wheat. Diabetics don't get sugar free food on prescription."
"There is no reason why GPs should have to prescribe food. I am not sure that food should be a prescription item in the first place given the massive strain on health budgets and the need to use resources elsewhere."
Contact
Email: Elaine Muirhead