Residential rehabilitation: literature review
Reviews the existing evidence from the Scottish, wider UK and international literatures pertaining to various aspects of residential rehabilitation as well as identifying research gaps. Part of a wider suite of research exploring residential rehabilitation across Scotland.
5. Workforce
While literature exists on the wider workforce within alcohol and drug treatment sector, there is scant research explicitly focusing on issues in relation to the workforce within residential rehabilitation, both in Scotland and internationally. A recent Scottish Government report (2021) of a survey of 20 residential rehabilitation providers explored the composition of the workforce across the sector in Scotland. This report found that the majority of the workforce is made up of paid members of staff (85%), with the number of paid workers ranging from 4 to 130 across these facilities. Fifteen percent of the staff were voluntary, with numbers ranging from 1 to 20 across these facilities. Just over a third of staff (35%) were reported to have lived experience of recovery from problematic alcohol and/or drug use (although several providers reported not knowing this information).
The report highlighted that the Scottish workforce was made up of a number of roles, displayed in figure 1 below.
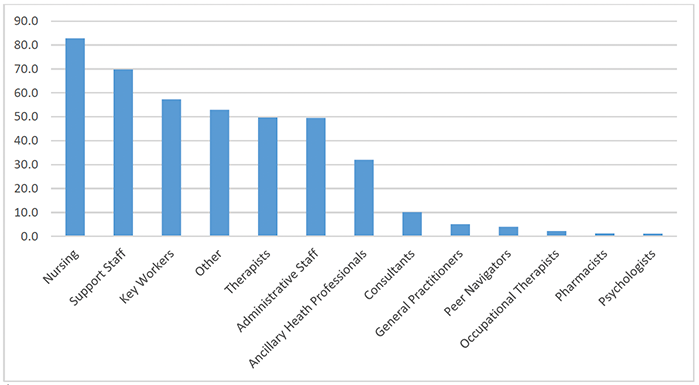
1 'Other Staff' included executives, management staff, cleaners and chefs.
2 Data on occupational role was missing for 38 working time equivalent (WTE) paid staff
Facilities which did not employ in-house medical and/or nursing staff primarily cited financial reasons, while others highlighted that they were a social model rather than a medical model. Twelve facilities reported external partnerships with external services, including Social Care, General Practitioner surgeries, NHS Occupational Therapists, consultant psychiatrists, medicine wholesalers, medical practices, pharmacies, NHS detox providers, sexual health nurses and opticians. Nine (45%) worked with other external partners, including Local Authorities (for accommodation); third-sector partners focusing on employability, training and education; Housing Agencies and other charities for housing; advocacy services, food distribution charities; and Jobcentres.
All 20 facilities reported that their staff received a range of training. Every facility reported health and safety training, while others reported drug and alcohol awareness training (n=18, 90%), emergency first aid (n=17, 85%), trauma awareness training (n=15, 75%) and Naloxone training (n=14, 70%). Mental health first-aid training was undertaken by around half (n=9, 45%) while other training included a range of courses on personal development, including those relating to employability skills.
Contact
Email: socialresearch@gov.scot