Reset and Rebuild - sexual health and blood borne virus services: recovery plan
This plan, coproduced with our NHS and third sector partners, takes stock of the impacts of the COVID-19 pandemic on Sexual Health and Blood Borne Virus (SHBBV) services and people that use them, ahead of a more fundamental review of the SHBBV Framework in 2022.
COVID-19: the Challenges
In March 2020, the impacts of the COVID-19 pandemic were becoming apparent across the health service, in local communities, and throughout wider society as a whole. Protecting the NHS rightly became a primary focus; difficult decisions had to be made about which services to maintain. Patients themselves also began staying away from health settings, and, even where services could be maintained, COVID-safe measures, such as physical distancing and use of personal protective equipment, meant that appointments took longer and could not be conducted as normal.
These impacts were common in almost all aspects of healthcare. However, the characteristics of SHBBV services made them all the more severe. The services provided are complex and multifaceted, spanning treating, testing for and prevention of blood borne viruses (BBVs) and sexually transmitted infections (STIs); abortion; contraception and sexual and reproductive health. These often support wider healthcare protection goals, but are also often delivered outwith conventional healthcare settings, targeting individuals with complex needs who do not access healthcare elsewhere and require highly patient sensitive approaches to address stigma. Many service users are vulnerable – young people, LGBTQ+ individuals, those at risk of gender-based violence, refugee/asylum seekers/travellers, homeless people, people engaged in prostitution or people who inject drugs. The range of services, and the needs of the populations who use them, mean that the effects of service reductions are likely to be both significant and difficult to repair.
Yet many of the skills and resources built up in sexual health services and within academia over decades were exactly those that could be most useful in a pandemic: contact tracing and testing capability, in particular, have been vital tools and are likely to remain so even as vaccination changes the course of the pandemic. In 2020, staff were rapidly redeployed; testing laboratory facilities were repurposed for COVID-19; and premises were given over to meet COVID-19 priorities.
These were unavoidable and necessary changes. However, they required an almost immediate reprioritisation of available services. From March 2020, SHBBV clinical care was restricted to only urgent and essential care[4], focusing on diagnosing serious and symptomatic STI, BBV, and preventing unplanned pregnancies. In addition, measures to ensure the long term viability of services, such as in-person undergraduate and postgraduate training, had to be limited because of COVID-19 mitigation requirements.
Third sector organisations, which have always played a vital role in supplementing clinical services and offering practical and emotional support for people, were also forced to redesign or limit services almost overnight. The Sector had to prioritise the rapid scale up of a COVID-19 response; provide critical information about the virus to diverse communities and individuals experiencing uncertainty during this time; and work to address some of the health and social inequalities that COVID-19 presented.
Face-to-face care in all instances was almost entirely removed, except for those urgent priorities. Technology and innovation were rapidly redeployed to fill the gaps, but these could not always substitute adequately, particularly given the complexities of the issues, the need for intimate or physical examination and testing, and the populations who needed support. Those most vulnerable, for whom equality of access was already a known issue, are likely to have been further left behind.
Case Study: Impact on Services, Highland Sexual Health (HSH) is an integrated sexual health service based at Raigmore Hospital in Inverness with additional weekly outreach clinics in Invergordon, Fort William, Wick & Thurso. There are over 11,000 patient contacts per year. From 20th March 2020, in response to the COVID-19 pandemic, HSH limited all clinical provision to urgent and essential care only. Staff were asked to vacate the main HSH clinical department which was repurposed in response to the pandemic. All outreach services were closed. Almost 75% of HSH clinical staff was redeployed to COVID-19 facing roles. The majority of service provision was provided remotely from the small departmental office, through telephone and video consultation and posting of testing kits and prescriptions. The available space in the small office was inadequate for privacy for remote consultations, storage of medication and equipment from clinics, as well as safe social distancing.
In the eight months it took for clinical premises to reopen, HSH only had access to one clinical room for three mornings per week in the hospital's general out-patient department for emergency face to face care following phone triage. The service was unable to provide any long acting reversible contraception (LARC), even for those who were vulnerable or priority, with the exception of intrauterine devices (IUD) for emergency contraception and subdermal contraceptive implants (SDI) for postnatal women who were seen prior to discharge on the ward. All patients had much of their clinical care provided remotely and were then placed on a waiting list to be seen once clinical premises became available. HSH was, however, able to clear its LARC waiting list over an eight week period by running additional evening and weekend clinics when additional space was available in the general out-patient department.
HSH regained access to clinical premises in November 2020 (shared half time with another speciality) but was restricted in numbers of patients allowed into the clinics owing to social distancing rules, and therefore unable to resume routine asymptomatic screening or HIV or syphilis testing for symptomatic patients. HSH continue to signpost patients to HIV Self-Test Scotland for a home test. Since January 2021, HSH have continued to provide all essential care, including LARC for vulnerable and priority groups. Routine patients continue to be managed remotely. Limited office space and social distancing remains challenging. However, during the period since January 2021, HSH were grateful for the continued access to their clinical premises, additional laptops for remote working, and no staff redeployment.
Although these changes manifested in a variety of ways, a few illustrative examples show the early impact. There was:
- A near cessation of very long acting methods of contraception (vLARC) insertions (including intrauterine and implantable methods: graph 1) in particular, the discontinuation of post abortion long-acting reversible contraception (LARC) provision.
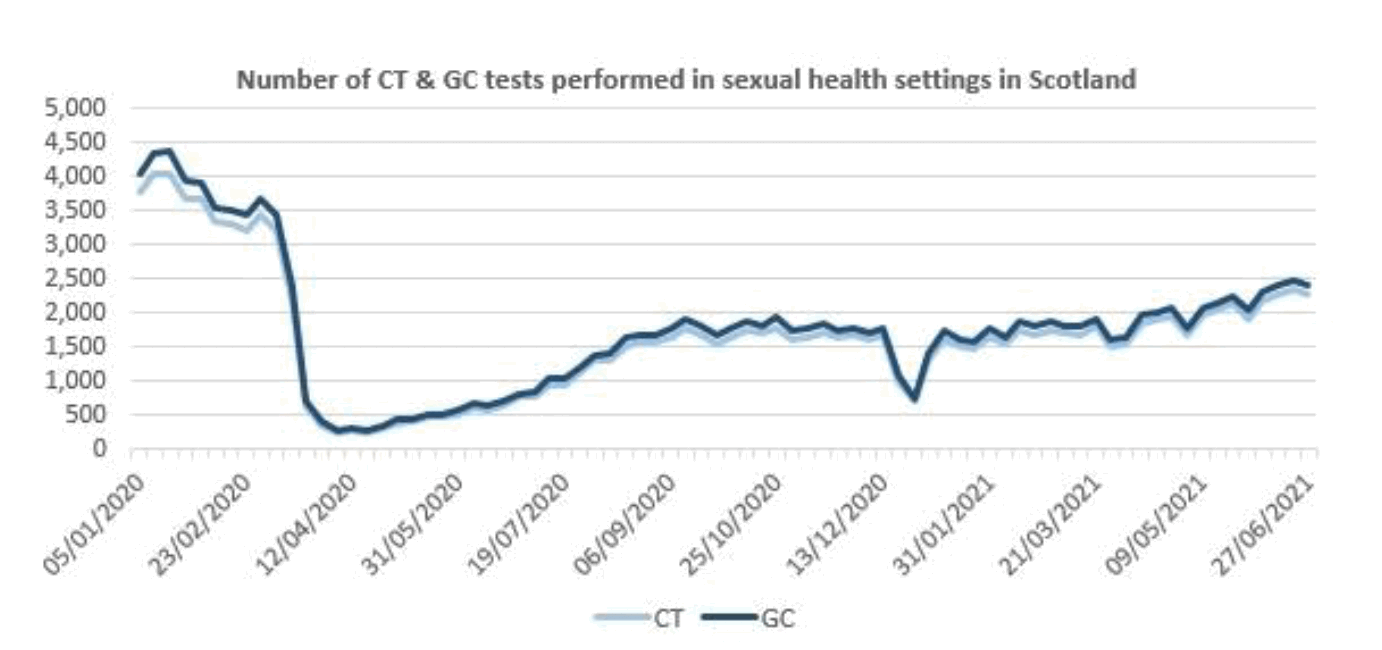
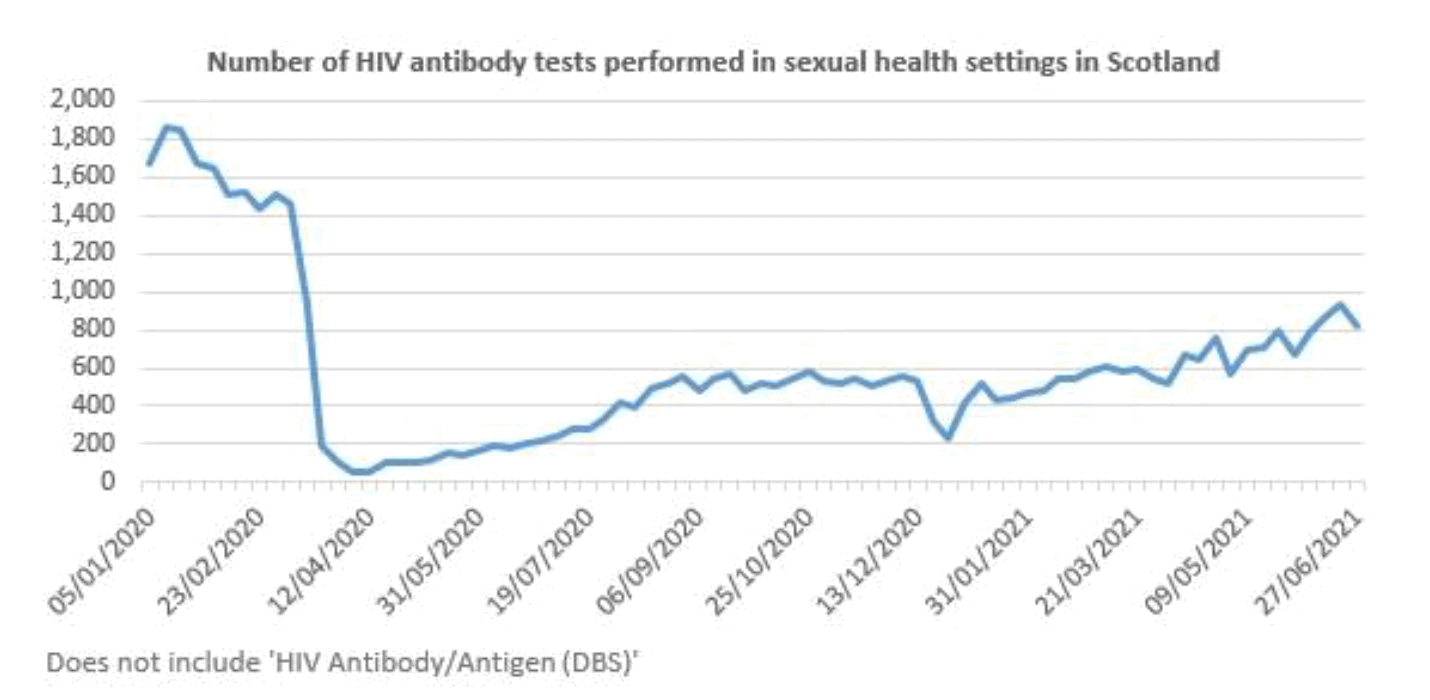
- A similar reduction in HIV testing across specialist sexual health services in Scotland (graph 2) including discontinuation of all outreach HIV and BBV testing for the most vulnerable populations.
- An almost complete cessation of outreach BBV testing in the community, delivered using Dried Blood Spot (DBS) or Point-of-care-testing (PoCT) technologies to groups with elevated prevalence of BBVs and/or multiple vulnerabilities including people who inject drugs (PWID), homeless populations, those involved in prostitution or at risk of gender-based violence.
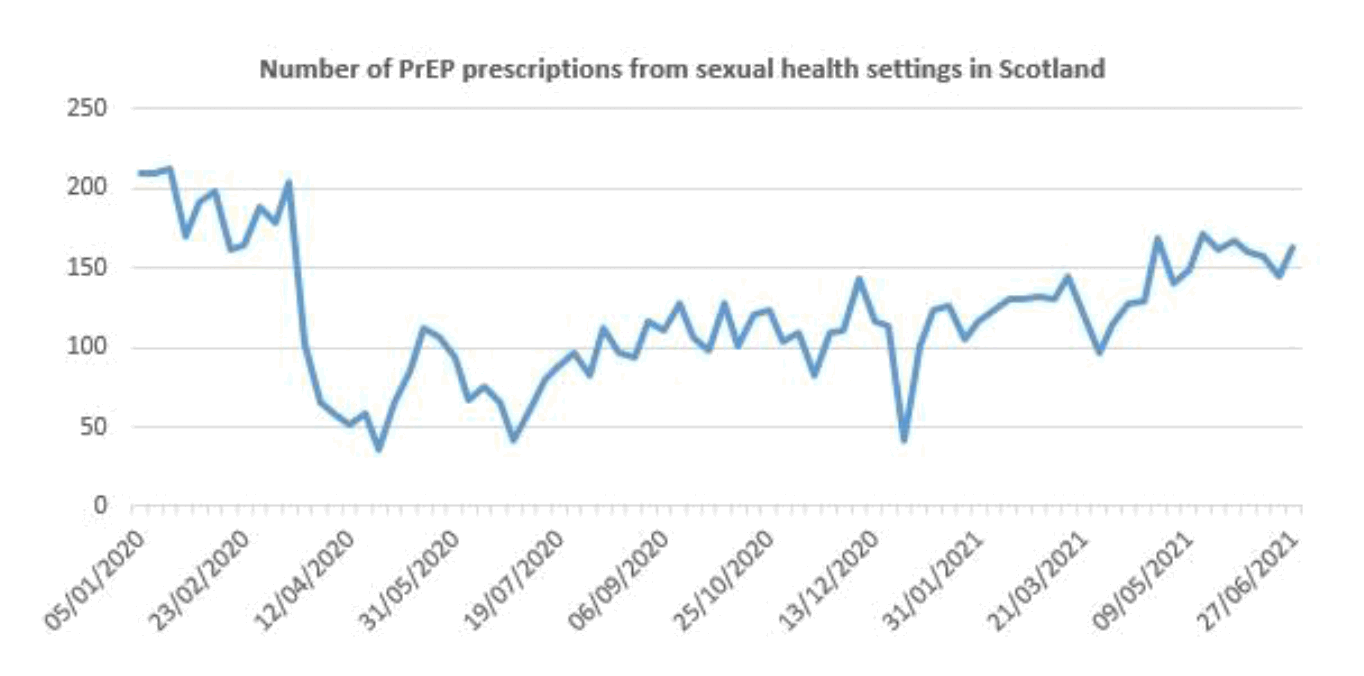
- A parallel reduction in HIV PrEP (HIV Pre-exposure Prophylaxis) provision (graph 3).
In the latter months of 2020, there were some hopeful, if early, signs of recovery. This recovery has continued, albeit slowly and with some dips, through the first six months of 2021. LARC recovery in sexual health services was particularly strong. Boards reported a return of some staff and increases in testing capacity, and some face-to-face appointments began to resume. However, by almost all measures, services remain at reduced capacity than before the pandemic:
- HIV testing through sexual health services has seen a welcome increase through the first six months of 2021. However, as of June 2021, numbers were around 40% fewer than pre-COVID-19 levels.
- There is reduced Public Health Scotland capacity for SHBBV surveillance and data reporting owing to reassignment to COVID-19 work.
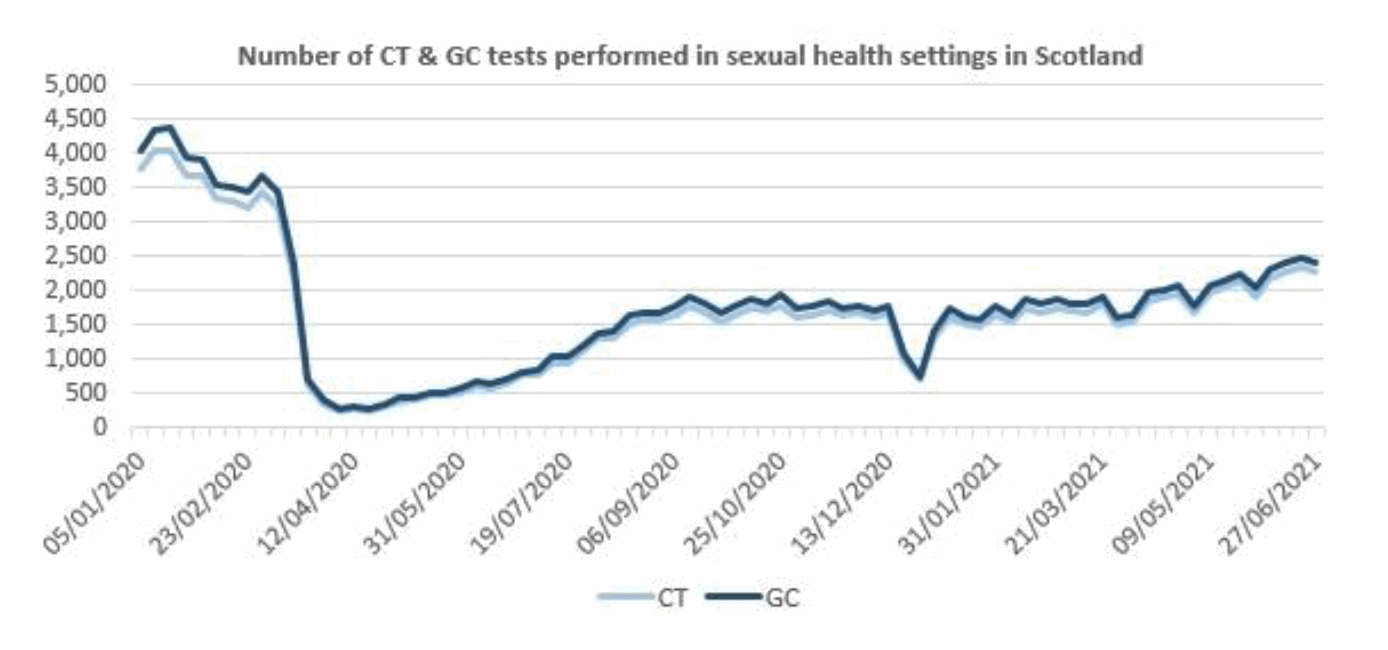
- Testing for other infections including Chlamydia and Gonorrhoea has now recovered to at, or just over, 50% of pre-COVID-19 levels across Scotland (see graph 4). Reduction in testing and specifically near person microscopy availability was replaced by postal testing and empirical treatment.
- Needle Exchange Surveillance Initiative (NESI) data (which is not linked to patient identifiers) suggests concerning numbers of undiagnosed HIV infection in people who inject drugs (PWID) in parts of Scotland[5]. Significant concerns remain regarding the possibility of undetected onward transmission in vulnerable groups, in particular PWID[6]
- Treatment targets for hepatitis C virus (HCV) for 2020-21 were suspended due to the challenges faced by treatment services. Additionally there were radical changes in the provision of opiate substitution therapy and harm reduction services for PWID which have also limited opportunities for HCV diagnosis and treatment.
Understanding the impacts of these changes may take years, but as the examples set out above show, they will be wide-ranging.
There may also be harm that is harder to quantify. While COVID-19 mitigation measures, such as physical distancing and significant curbs on social mixing, may have reduced the short-term prevalence of risky sexual behaviours and sexual contact between households, the longer term impact will be affected by access to SHBBV services and prevention interventions, as well as compensatory behaviours once COVID-19 restrictions have been reduced. Evidence also suggests the harm may be greatest amongst more vulnerable populations: UK data reporting on the sexual behaviour of 18-44 year olds in the first four months of lockdown[7] suggests in general, the majority of people reported no change to their sexual behaviour and sexual relationships, but those reporting change tended to be in less stable phases of life, including young people. In addition 81% of those reporting new partners since lockdown also reported condomless sex with a new partner.
Case study: impact on people who inject drugs (PWID) in Glasgow/Lanarkshire
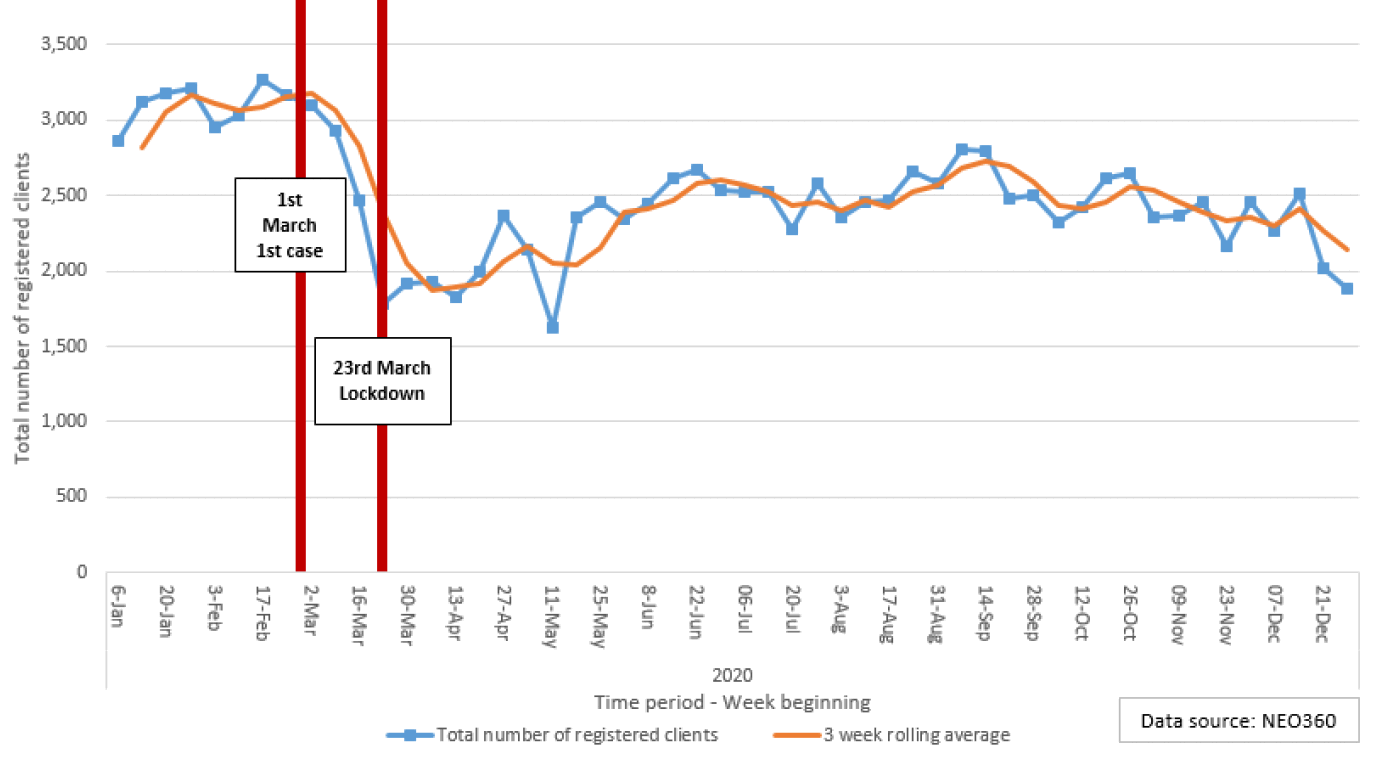
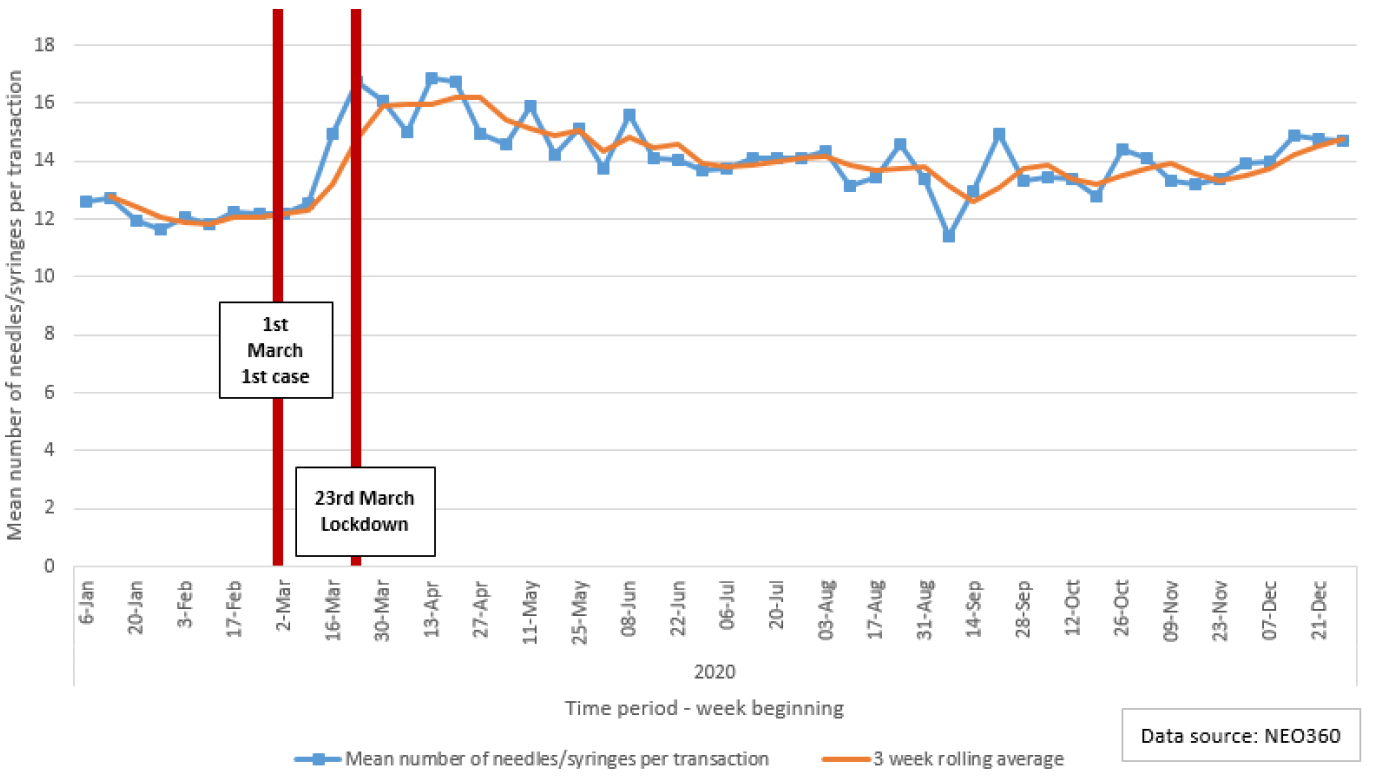
Services for PWID were impacted severely during the first wave of the COVID-19 pandemic as a result of the restrictions placed on individual movement and face-to-face consultation. For example, since the first lockdown policy was implemented on 23 March 2020, the available data suggests that the number of registered clients attending injecting equipment provision (IEP) sites weekly across mainland Scotland fell sharply and has only partially recovered. Specifically, the average number of registered clients fell from around 3,000 pre-lockdown to 2,500 per week, having been as low as 2,000 per week in the immediate period post-lockdown (Figure 1). In response, services adapted rapidly and innovatively to ensure the needs of PWID were met as best as possible to reduce the risk of harms. For example, increased volumes of injecting equipment were given out, secondary distribution was actively encouraged, assertive outreach was enhanced and new injecting equipment provision (IEP) phone/mail order services were established. This translated to an increase in the number of needles/syringes dispensed per transaction from around 12 per week pre-lockdown to 14 per week, having been as high as 16 per week in the immediate period post-lockdown (Figure 2).
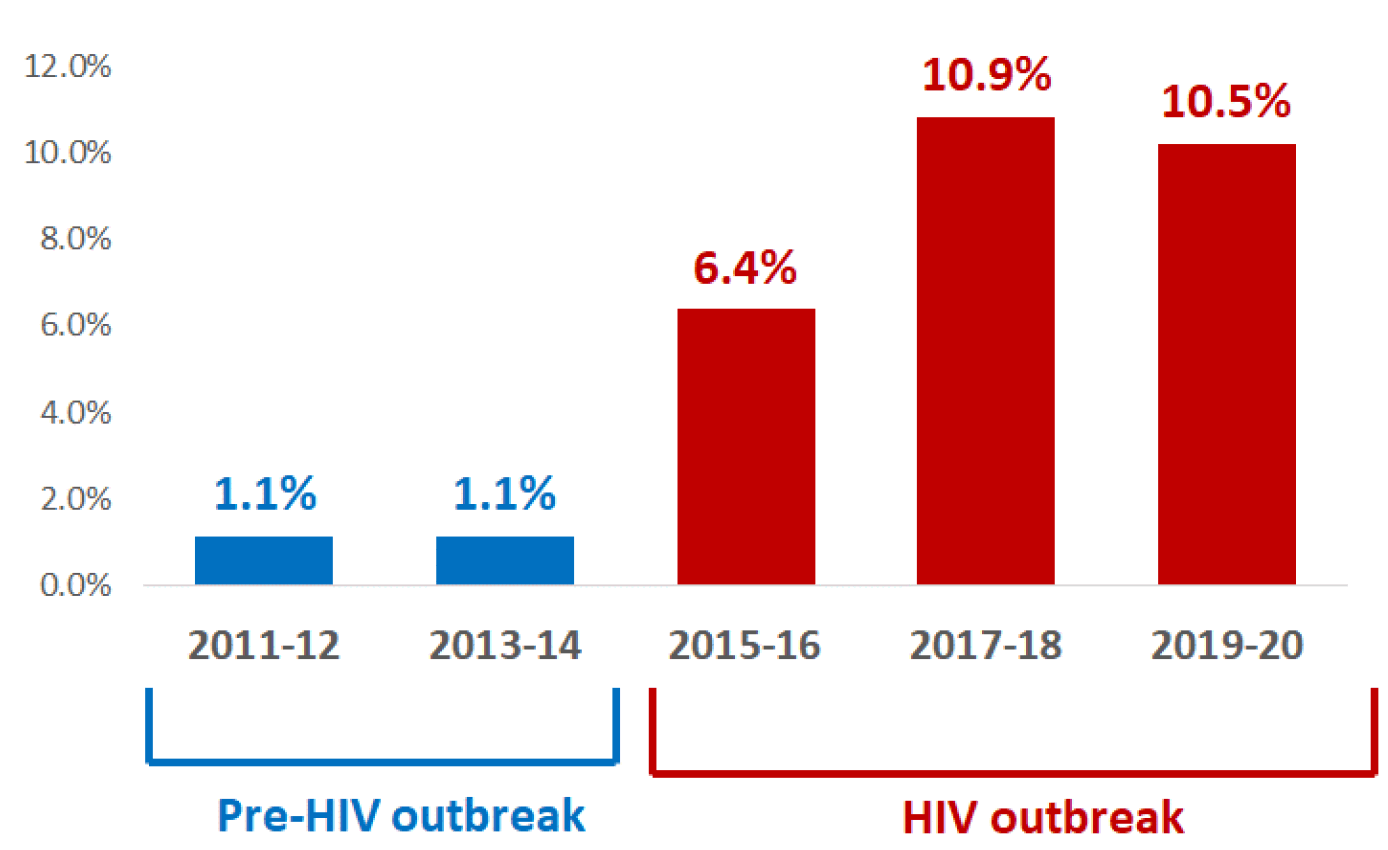
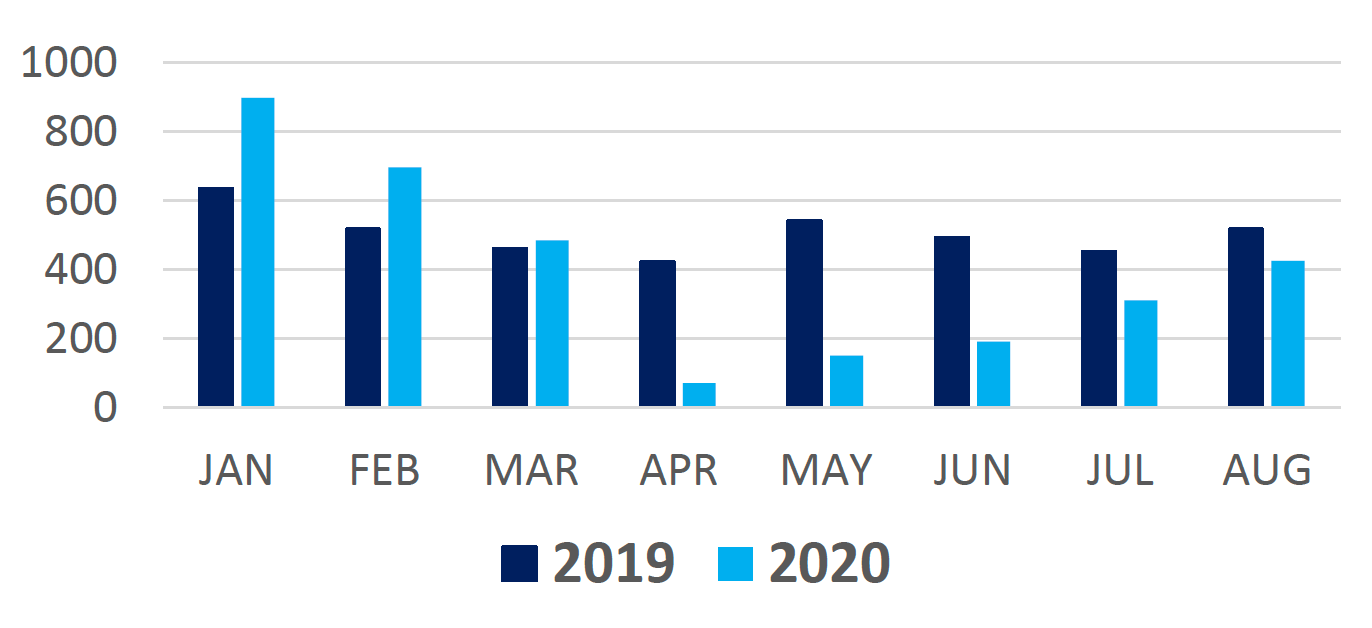
An HIV outbreak among PWID in NHS Greater Glasgow & Clyde, first identified in 2015, is ongoing. Almost 200 individuals have been diagnosed over that period. Bio-behavioural surveillance from the NESI study has illustrated the wider impact of the outbreak on HIV prevalence among PWID; increasing 10-fold from 1% to 11% in Glasgow City between 2013 and 2017 and plateauing thereafter (Figure 3). Data also suggest increasing prevalence in recent years in areas outside of the city centre boundary. However, we have limited understanding of the impact of COVID-19 on the outbreak due to suspended HIV testing as a result of the COVID-19 restrictions. In the first month following the first lockdown, HIV tests in drug services and prisons were down 83% compared to the same period in 2019, but were approaching pre-COVID levels at the end of the summer. More recent intelligence suggests that HIV testing numbers have decreased again during the final quarter of 2020. Even within this restricted environment, there were 20 new diagnoses confirmed in PWID in Glasgow during 2020 indicating ongoing transmission of the virus.
The above findings form part of a recent review of the HIV outbreak among PWID undertaken by Public Health Scotland/Glasgow Caledonian University, in association with NHS Greater Glasgow & Clyde and NHS Lanarkshire and on behalf of the National HIV PWID Oversight Group. The findings of the review will inform further efforts locally by NHS Boards to prevent HIV transmission among PWID and also inform recommendations within a proposal for a National HIV Transmission Elimination Strategy to be considered by Scottish Government.
In the months ahead, the pace of recovery will inextricably follow to some extent the course of the pandemic, and even in the best case scenario, there will be no immediate solution to all of the harms inflicted by COVID-19. However, it is clear that a number of actions must form the basis of recovery, and as soon as is feasible.
Four key actions, in particular, are required to minimise harm to public health to enable services to be in a position to implement the next SHBBV Framework from 2022:
1. Staff capacity – in line with wider NHS remobilisation plans, and as quickly as possible, staff should be returned to SHBBV services, and every effort should be made to ensure that, wherever possible, highly skilled SHBBV staff are not diverted to COVID-related work which does not make the most of their expertise. Likewise, services should develop coherent and localised plans to build capacity, by continuing to use new technologies or ways of working that have delivered benefits throughout the pandemic. The needs of SHBBV services should be considered when future savings targets are implemented.
2. Testing capability – laboratory capacity is likely to remain under COVID-19 pressure for the foreseeable future, meaning alternative solutions must be found to increase testing for BBVs and STIs, including more coordinated or national solutions.
3. Maintaining and supporting non-specialist capacity. A large proportion of clinical service provision, and SHBBV prevention and health improvement activity is provided through general practice, Health and Social Care Partnerships, the education sector and third sector agencies, all of which rely on specialist services for education, training and governance support. This support has been particularly affected by the pandemic and will require focussed and sustained efforts to rebuild capacity in the face of competing pressures – while also continuing to raise awareness that referral pathways are open for use again with the wider health system.
4. A robust understanding must be developed of the short, medium and long term impacts of both the SHBBV service reductions and changes of the last year, and the impacts of COVID-19 and the associated social isolation, physical distancing, financial hardship, relationship and mental health impacts, loss of education and associated potential changes in people's sexual and emotional health and wellbeing.
Contact
Email: healthprotection@gov.scot