A Refreshed Framework for Maternity Care in Scotland: The Maternity Services Action Group
The Framework outlines the principles which govern maternity services from pre-conception, through pregnancy, childbirth and postnatal care and into parenthood in Scotland.
2. IMPROVING HEALTH AND REDUCING HEALTH INEQUALITIES-THE UNIQUE ROLE OF MATERNITY CARE SERVICES
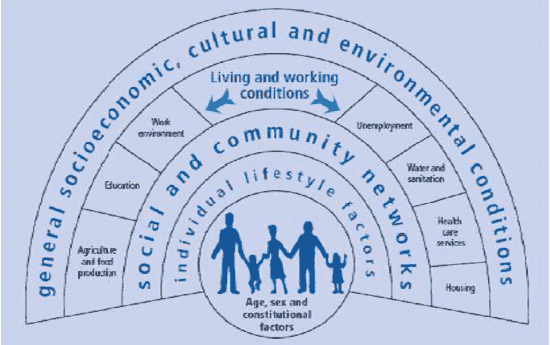
The model 9 below shows that the many determinants of health are complex and interlinked. Inequalities in health arise because of inequalities in access to and/or benefit from the determinants shown in the model. Clearly t hen, they cannot be addressed by health policy or healthcare alone. They require action at structural 10, individual, and collaborative public service level. Crucially effective collaboration requires each service to be clear about its own unique contribution.
Dalgren and Whiteheads' determinants of health model (1991)
We know that health inequalities follow a social gradient and as such affect all population groups 11. The importance of strengthening universal services is important to reduce the gap between groups. NHS maternity care services are unique in that they are the only universal public service for women and their babies during pregnancy and the early period of an infant's life. As such they are a vital component of, and gateway to, wider early years services including social care services, housing services, welfare services and the Third Sector.
Maternity care services have been working hard and creatively to continually improve the quality of the care they deliver. Many innovative and tailored services have been developed to meet the needs of women, babies and their families. However inequalities in access to, and or, the quality of antenatal healthcare received continue to contribute to health inequalities. There is a clear correlation between poorer pregnancy outcomes, including higher rates of maternal and infant deaths and morbidity in women who book later for antenatal care, attended infrequently or never attend for care. At present in Scotland, women and babies who are at the greatest risk of poor health outcomes are the least likely to access and/or benefit from the antenatal health care that they need. This significantly hampers the contribution maternity care services can make to improving health and reducing health inequalities. A key component of this framework is to drive measureable improvements in early access to antenatal care that is person centred, safe and effective, and of equitable quality regardless of the circumstances and characteristics of individual women and families.
We know that improving access to antenatal care is insufficient; it needs to be accompanied by a focus on continuous, effective, assessment of health and social need in order to identify any prevention and early intervention actions needed before babies are born and in the early days of their lives. We know that to do this effectively, maternity care staff need to work in partnership with each other and with women and their families, using health asset or strengths based approaches 12.
Guidance to help strengthen NHS Board capacity to reduce antenatal health inequalities has been developed to support implementation of this framework 13.
The Framework
The refreshed framework is intended as a flexible, overarching framework, within which NHS Boards can strengthen the unique contribution of maternity care services. It is intended to support and facilitate the planning and provision of high quality outcome focussed services, whatever the geographic or demographic nature of the communities they serve. The framework integrates key elements of the 2001 framework and the subsequent Expert Group on Acute Maternity Services report with current evidence and policy, together with continual service improvement measures.
The framework describes a number of overarching principles together with specific service descriptors for each part of a woman, baby and family's journey through maternity care. The overarching principles and the specific service descriptors are designed to strengthen two key aspects of maternity care provision:
1. the quality of the care and support provided by NHS services- ensuring it is person centred, safe , effective , equitable, tim ely and efficient for every woman, baby and family every time.
2. The contribution of maternity services as partners with Local Authority and other public services, including the Third Sector.