It's Not Rare to Have a Rare Disease
The Implementation Plan for Rare Diseases in Scotland
2. THE STRATEGIC CONTEXT
The NHS Scotland 'Quality Strategy'[8] and the associated '2020 Vision and its accompanying Route Map'[9], aim to deliver the highest quality of healthcare to the people of Scotland. Together they provide common principles through which the NHS, Local Authorities and the third sector, working together and with patients, carers and the public, can deliver a shared goal of world-leading healthcare; ensuring services are; safe, person-centred and effective.
Our workforce is key to the delivery of quality services. The 'Everyone Matters: 2020 Workforce Vision Implementation Framework'[10] sets out 5 priorities for action by NHS Boards: healthy organisational culture; sustainable workforce; capable workforce; integrated workforce; effective leadership and management.
This Implementation Plan for Rare Diseases in Scotland supports the drive to deliver the Scottish Government's 2020 Vision that by 2020 everyone is able to live longer healthier lives at home, or in a homely setting. By 2020 we will have a healthcare system where we have integrated health and social care, a focus on prevention, anticipation and supported self-management.
The Scottish Government has also set up a Task Force to consider seven day working. Many services are already delivered seven days a week and changes towards extending care are already happening in some areas, but the Scottish Government wants to accelerate the pace of change, by targeting enhanced weekend and out of hours services that will benefit patients the most. Additional clinical and non-clinical support, at key points over the weekend and overnight, will be focussed towards improving service provision and patient flow.
NHS Scotland Organisational Structures - Local, Regional and National
The Scottish Government has responsibility for the National Health Services in Scotland and its resource allocation. Legislation on the NHS in Scotland is made by the Scottish Parliament. The Cabinet Secretary for Health and Wellbeing has ministerial responsibility in the Scottish Cabinet for the NHS in Scotland.
The Scottish Government sets national objectives and priorities for the NHS, agrees delivery plans with each NHS Board and Special Board, monitors performance, and supports the Boards to achieve their objectives (figure 1).
Figure 1 NHS Planning Framework
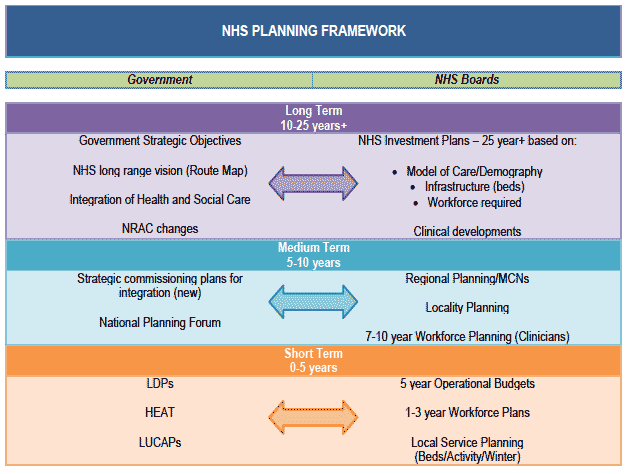
NHS Scotland strives to deliver equity of access, safe, effective and person centred care for all who need it across all age groups. The existing care and support services reflect many of the elements of the UK Strategy's[11] vision and are delivered through a range of local, regional and nationally provided services through local NHS Boards and NHS National Services Scotland National Specialist and Screening Services Directorate (NSD).
The 14 'territorial' NHS Boards in Scotland are unified organisations which plan, commission and deliver NHS services and take overall responsibility for the health of their populations. Their responsibilities cover hospital and community health services including services provided by GPs, dentists, community pharmacists and opticians, who are independent contractors.
Seven national or 'special' NHS Boards provide national support services and Healthcare Improvement Scotland provides the scrutiny and public assurance of Scotland's health services.
The NHS Boards work closely with partners including patients, staff, local authorities and the third sector to deliver effective healthcare services and to safeguard and improve the health of their residents.
NHS Boards work together regionally, in three planning groups (figure 2) covering: South East and Tayside; West of Scotland and North of Scotland. They also work together nationally to plan and commission specialist healthcare services such as heart and lung surgery, neurosurgery, and forensic psychiatric care. A number of local services are also shared between NHS Boards to maximise efficiency.
Figure 2 NHS Board Membership of Regional Planning Groups
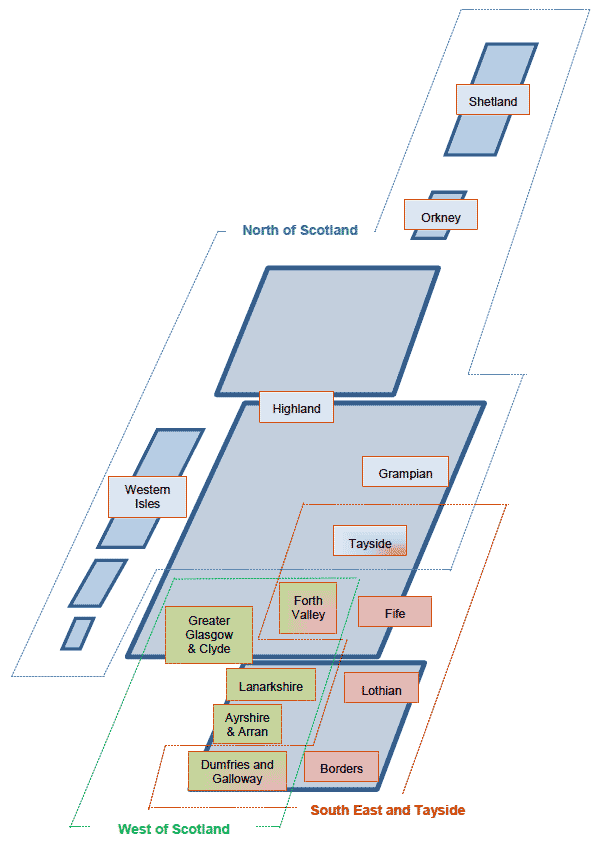
The NHS Boards are guided by an annually reviewed 'Local Delivery Plan' (LDP) agreed by each Board with Scottish Government. The LDPs and associated Improvement and Co-production Plans provide a means for NHS Boards to set out and to be reviewed against their plans to deliver against local and national priorities, including service developments.
The Public Bodies (Joint Working) (Scotland) Act was granted royal assent on April 1, 2014. The Act is a landmark in health and social care reform for Scotland which will require NHS Boards and Local Authorities to integrate their services resulting in more joined-up, seamless health and social care provision closer to home to improve people's lives.
There are two integration models available to NHS Boards and Local Authorities allowing the choice of model to be selected based on local needs:
Option 1 - The NHS Board and Local Authority delegate the responsibility for planning and resourcing service provision for adult health and social care services to an Integration Joint Board.
Option 2 - The NHS Board or the Local Authority takes the lead responsibility for planning, resourcing and delivering integrated adult health and social care services.
These developments and associated guidance also support the new Health and Social Care Partnerships as they take on an important role in delivering integrated services.
NHS National Services Scotland, through NSD manages specialised commissioning and service provision across a wide range of highly specialised services, some of which are nationally designated and provided within NHS Scotland. Others are provided by designated services/bodies in NHS England. Some of these highly specialised services work in the area of one or more rare diseases. All have an important role in supporting people with rare diseases.
It is most likely that anyone requiring investigations to identify a specific disease will be referred to local diagnostic services through a specialist service or directly by their GP (as appropriate) for a specific investigative procedure or tests. However, dependent on the eventual diagnosis, individuals will be assessed to ensure the most appropriate and effective treatment is made available. This may not be available locally if the treatment/service concerned is highly specialised. People may be referred through specialist centres regionally or nationally within Scotland or they may need to access services through designated centres in NHS England, or further afield, dependent on where the required service is provided.
Examples of specialist services in NHS England accessed by people living in Scotland include alkaptonuria, complex neurofibromatosis type 2; rare mitochondrial diseases for adults and children; rare neuromuscular disease; and amyloidosis.
The elements of NSD's work in support of rare diseases are:
National Specialist Services - Before services are nationally designated their clinical and cost effectiveness is considered by two key committees, the National Patient, Public and Professional Reference Group (NPPPRG) who advise the National Specialist Services Committee (NSSC). All NSSC recommendations are referred to NHS Board Chief Executives' prior to submission to Scottish Ministers for approval. NSD also commissions on behalf of all NHS Boards some UK Specialist Services for adults and children. These services cover medical, surgical and scientific provision for those rare conditions where access to specialist expertise and treatment is not available in Scotland.
National Screening Programmes - These are aimed at early identification of a range of diseases/conditions, to allow clinical services to initiate early treatment and follow up. The UK National Screening Committee (UKNSC) provides advice to all four UK Governments on the adoption of new national population screening programmes or changes to existing ones. It is a matter for each country to consider UKNSC recommendations. Newborn screening in Scotland covers; Phenylketonuria; Congenital Hypothyroidism; Cystic Fibrosis; Medium Chain Acyl-CoA Dehydrogenase Deficiency and Sickle Cell Disease.
National Managed Clinical Networks (NMCNs) - Link together health professionals, patients, third sector, service managers and other partners to improve access to and performance of specific services for people, who often have complex needs. The NMCNs are required to deliver continuous quality improvement, pursuing opportunities to achieve better value for money through the delivery of optimal, evidence-based care that adds value from the patient's perspective, optimises productivity and reduces unwarranted variation.
Managed Diagnostic Networks (MDNs) - There are four Scotland-wide networks covering pathology, imaging, clinical biochemistry and microbiology/virology. These networks aim to deliver improved and quicker diagnosis and service efficiencies by quality improvement work and reduction of waste, harm and variation.
Other structures in Scotland have an important role to play in supporting people with rare diseases:
The National Specialist Services Committee (NSSC) considers proposals for national commissioning of highly specialist health services (described above) applications for National Managed Clinical Networks. Each element of this provision is reviewed every 3-5 years to ensure service arrangements remain relevant.
The Scottish Molecular Genetics and Cytogenetics Laboratory Consortium is the forum through which service developments in genetic testing are agreed. The genetic diagnostic laboratory services ensure equitable access to a comprehensive range of diagnostic genetic tests (provided within and outwith Scotland). Developments in this area are overseen by the Molecular Genetics and Cytogenetics Consortium and the Molecular Pathology Consortium.
Many rare diseases are genetic in origin and require specialist genetics input to diagnosis and treatment. The consortia link the four regional genetics centres in Aberdeen, Dundee, Edinburgh and Glasgow. This approach provides genetic testing for a wide range of conditions.
The Molecular Pathology Consortium is the forum for collaborative discussion and decision making on molecular pathology testing in Scotland agreeing which tests will be provided in Scotland, in which laboratories and the priorities for introducing new tests. The group aims to ensure that everyone in Scotland has access to the same high quality and timeliness of molecular pathology tests, regardless of geographical location.
The Scottish Government's Innovation Partnership Board brings industry and health interests together to advance Scotland as a world leading centre for innovation and health in medicines, medical technology and digital health.
The Scottish Government is a member of the UK Rare Diseases Forum established by Department of Health (UK) to monitor how the vision and actions outlined in the UK Strategy for Rare Diseases are being responded to across the UK.
Palliative Care
Some people with life limiting and progressive rare diseases may require palliative care support. This is defined by the World Health Organisation as "…an approach that improves the quality of life of patients and their families facing the problem associated with life-threatening illness, through the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychosocial and spiritual."[12]
Related to this, specialist palliative care[13] is the active total care of patients with progressive, advanced disease. Care is provided by a multi-professional team who have undergone recognised specialist palliative care training to provide physical, psychological, social and spiritual support.
Living and Dying Well[14] was Scotland's first national action plan for palliative and end of life care and set the direction for service planning and delivery. Work carried out as a result clearly demonstrated that there is a strong will to continuously improve and enhance the availability and quality of palliative and end of life care for all.
The Scottish Government through the development of a Strategic Framework for Action will provide a focus to support a wide range of organisations, clinical and care staff to reliably and sustainably spread good practice in high quality palliative and end of life care. The development of the Framework will be linked to the 2020 Vision for Health and Social Care[15].
The Scottish Government will work with a newly constituted National Advisory Group for Palliative and End of Life Care in supporting key stakeholders to apply the '3-Step Improvement Framework for Scotland's Public Services'[16] to deliver the changes that they identify to support the Strategic Framework.
Following an announcement in December 2013 that the Liverpool Care Pathway will be phased out in Scotland during 2014, Interim Guidance on Caring for people in the Last Days and Hours of Life[17] was published. In recognition of the impact on staff and teams, work is underway to develop a national statement on the requirements for care in the last days and hours of life. This national statement will reflect the principles set out in the Interim Guidance and support NHS Boards to signpost and prompt clinical and care teams to develop local assessment and care planning materials, policies and guidance to be applied in all care settings.
Training, Education and Information
The UK Plan for Rare Diseases acknowledges that it is unrealistic for most clinicians to have detailed knowledge of treatment and management of every rare disease. This applies across all specialties, across the UK.
It is expected however that clinicians should be aware of the appropriate referral procedures within their own healthcare system. In Scotland this means clinicians should know how to make appropriate referrals for rare diseases within their own NHS Boards or to other NHS Boards and specialist services through NSD.
The Royal College of General Practitioners GP training curriculum includes genetics in primary care. The very rarity of individual conditions makes it unlikely many of these diseases will be seen by individual GPs over their working life. However, across the average practice population, a number of rare conditions may be managed. In some cases, conditions may present within individual families.
Decision support systems have the potential to support GPs to recognise key groups of symptoms which may suggest a rare disease and to refer patients to the appropriate specialists for diagnosis, for treatment plans and when advice is needed on the management of a patient's condition. In support of this, quality assured information on rare diseases is needed for all health practitioners. Such information would also benefit patients and families
NHS Boards, post graduate deaneries, NHS Education for Scotland (NES) and others undertake continuing professional development to meet GPs' educational needs.
Other staff training, education and support needs are addressed through various approaches. The 2020 Vision for Workforce encourages innovation among teams and individuals, supporting them to utilise new technology. It supports 'on-the-job' learning and provides time for and access to learning and development opportunities to develop professional and technical skills, knowledge and competencies. The associated implementation plan for 2014-15 sets out the initial arrangements to deliver workforce developments.
Awareness raising of rare diseases needs to be incorporated into training for the multidisciplinary healthcare team and it would be relevant to direct attention towards childcare and education settings also.
Developments in Education
NES (NHS Education for Scotland) is working to tailor education delivery methods to meet the educational needs of staff in services for remote and rural populations. The RRHEAL (Remote and Rural Healthcare Educational Alliance) provides an education platform through which remote, rural and island healthcare teams can access clinical and other support information.
The Scottish Genetics Education Network (ScotGEN) provides a range of high quality teaching materials for genetics education and patient information and has a wide range of information leaflets and support information on rare conditions of genetic origin.
Within NHS Scotland there are several National Managed Clinical Networks (NMCNs) for rare diseases and complex conditions. These networks are required to develop and implement an education strategy for health professionals and patients/carers. Many are now at the stage of developing online education packages in collaboration with NES.
The NMCNs also support the development and provision of information to support increased recognition. In paediatric epilepsy the network developed an individually tailored patient booklet for a child to take to school to ensure awareness of their needs. The network has also run awareness raising sessions for teachers. Similar work on the dietary needs of affected children was done in the metabolic network.
Infrastructure for Rare Disease Developments
Life sciences and technology innovation
Scotland has ambitions to develop its role as an international centre for innovation in health technologies and in life sciences to improve care for patients. These technologies, some of which are produced by Scottish-based technology and life sciences companies, hold promise to develop support and treatments across a range of health conditions, including for rare diseases.
Many Scottish universities have existing bio-park or similar ventures with NHS Board, life sciences and enterprise partners. These initiatives bring together universities delivering internationally recognised research, a possibly unique integrated health service, with universal population coverage and cutting edge innovation companies.
In 2012, 'Health and Wealth in Scotland: A Statement of Intent for Innovation in Health'[18] was launched. A blueprint for innovation this consolidates existing partnerships between NHS Scotland, academic institutions, industry and enterprise.
Some of the current work of Scottish life sciences and innovation companies is of potential relevance to rare diseases.
Health Technology Assessment
The Scottish Health Technologies Group (SHTG) provides clinical and cost-effectiveness advice on health-related technologies. This advice supports the planning and decisionmaking processes nationally and in NHS Boards. SHTG also provides early information on health technologies in development.
The SHTG links to European and international health technology networks and in common with developments in other health technology agencies is moving from the traditional health technology assessment to rapid reviews of evidence.
Telehealth and telecare technology
Telecare systems are becoming established in the community, offering support to and monitoring of elderly and disabled patients and those with long term conditions. Telecare also provides patients with support to self-manage health conditions and to live independently.
Telehealth is increasingly used to link patients to clinical expertise using video and other technologies. Clinician and patient may be some distance apart, but real-time video footage, diagnostic images and test results can be available to inform the consultation and resulting treatment.
As Scotland's health service buildings and facilities are refurbished or replaced, there is investment in the installation of modern health and communication technologies for use in screening, in diagnostics, in treatment, in monitoring and in follow-up.
A National Telehealth and Telecare Delivery Plan for Scotland to 2015 - Driving Improvement, Integration and Innovation[19] sets out actions to develop this provision to deliver a range of services as alternatives to traditional service delivery models.
Following the integration of health and social care and the focus on joint support to patients, shared information systems will be crucial in ensuring support to patients is effectively and efficiently co-ordinated across health, social care and partners.
Information systems, data and registers
Information systems, registers and the data within them are important in the efficient delivery of modern healthcare. With the integration of health and social care, patients with a rare disease will potentially be seen across a number of healthcare and social care settings, which may have different electronic clinical and care systems. The existing variation between systems, confidentiality and firewalls create difficulties in data sharing across NHS Board boundaries.
Through locality planning and joint working between health and social care professionals, information systems are being considered to improve data exchange and to facilitate positive outcomes for people across the spectrum of disease, including rare diseases. As clinical and social care pathways begin to be developed jointly they will need the support of robust IT platforms.
Work on IT developments in this area is covered by the Person-Centred e-Health Strategy[20]. In addition, NHS Boards are progressing the development of patient portals to give access to services in secondary care.
National Services Scotland (NSS) Public Health and Intelligence (PHI - formerly Information Services Division) has a role in developing data standards and coding, building on its well established work in these areas.
Electronic Health Data
Work is progressing well to have a pan-Scotland service available to support the use of routinely collected electronic health data. Through its participation in and co-ordination of the UK e-HIRC (E-Health Informatics Research Centre) network, Scotland is helping to deliver the goal of being able to combine the outputs of the UK datasets.
A Clinical Audit System was developed to provide databases for some conditions covered by National Managed Clinical Networks. This system is used to help health professionals work together in caring for patients.
PHI has considerable experience in linking patient records across healthcare settings. Although data linkage may be possible across different sectors, current variations in the recording of rare diseases and limitations in coding systems like ICD-10 makes it difficult at present to explicitly identify those patients with rare diseases.
PHI will have an important role in monitoring the development of ICD-11, the successor to ICD-10 and any subsequent roll-out across Scotland. As ICD-11 is still under development and may not be published until 2015 at the earliest, its introduction may not commence until 2016-17 or later. This means it cannot be relied on to identify rare diseases in the short term. Without the level of detail which may be available through ICD-11 when it is introduced, there may be limited examples of databases which appropriately record rare diseases. Account also needs to be taken of General Practice coding. In Scotland, the READ codes are used in General Practice. In England there is a planned move to a new system of coding by 2014.
In the main, NHS Boards determine the scope and rollout speed of their various e-Health approaches to suit their local circumstances. Progress is however monitored through the Scottish Government e-Health strategy.
Progress with patient portal developments is picked up during 6 monthly e-Health Plan reviews with each NHS Board.
Contact
Email: Paul Currie