Prescription for Excellence - the future of pharmaceutical care: vision and plan
A vision and action plan for the future of NHS pharmaceutical care in Scotland through integrated partnerships and innovation.
Chapter 1 The Vision
1.1 The Vision
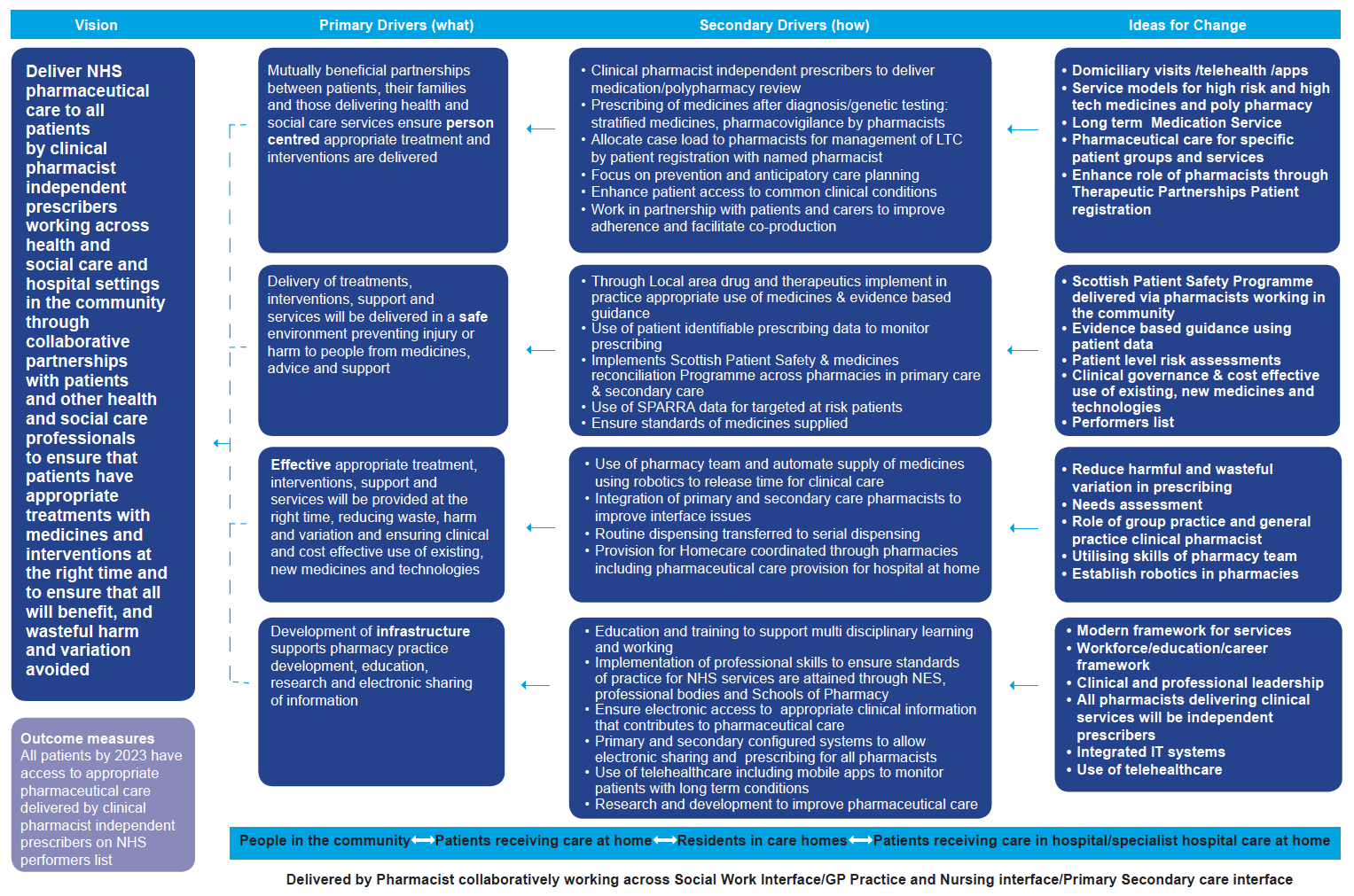
1.1.1Our Vision as set out in the driver diagram (Figure 1) identifies four key patient populations, each with specific pharmaceutical care needs: people in the community; patients receiving care at home; residents in care homes; and patients receiving care in hospital / specialist hospital care at home. It focuses not on the physical registered pharmacy premises, but rather on the clinical capability of pharmacists working in a variety of environments to meet those care needs in partnership with other medical and social care professionals.
1.1.2 Our success in delivering the Vision will be measured through the delivery of the following main outcomes through a series of work programmes which will be delivered over the next 10 years.
- Pharmacists in the NHS would be recognised as clinicians responsible for the provision of NHS pharmaceutical care.
- Releasing capacity of pharmacists to deliver pharmaceutical care would be facilitated by full utilisation of pharmacy technicians, support staff and increased use of robotics in dispensing to improve safety and efficiency.
- All patients would have access to NHS pharmaceutical care by NHS accredited clinical pharmacist independent prescribers in all settings.
- Pharmacists in secondary care and in primary care work together in an integrated way which would be supported by a common clinical pharmacy career structure.
- Patients have a close relationship with an individual pharmacist, ensuring greater continuity and consistency of care for patients - introducing the concept of the named pharmacist and patient registration with NHS Board listed pharmacists which will underpin professional relationship with patients and local clinical governance systems.
- NHS Boards to have a direct relationship with individual pharmacists providing services in their areas regardless of setting.
- Pharmacists work closely with GPs, primary care, community teams and secondary care sharing information for the benefit of the patient. These pharmacists would be known as the general practice pharmacists.
- Pharmacists work in groups to deliver NHS Pharmaceutical care to patients in all care settings, especially for those with complex or long term conditions with allocation of caseloads.
- Pharmaceutical care for specific patient groups is provided under a national frame work and to nationally determined NHS standards. A national framework and NHS standards for the pharmaceutical care of residents of care homes and people receiving care and support at home would be prioritised.
- NHS Board Pharmaceutical Care Services Plans with needs assessments to enhance local healthcare planning which would include equitable access to services in deprived areas as well as specific public health needs driving a new contractual framework for premises and pharmaceutical care, removing any perverse incentives.
- The Scottish Government will work with patients, dispensing doctors and appropriate stakeholders to explore how rural communities can be further supported in terms of pharmaceutical care.
- Pharmacists undertake an enhanced role in preventing ill-health, co-production and minimising health inequalities.
- Pharmacists and the wider pharmacy workforce are trained appropriately to their enhanced role, both pre and post qualification.
- NHS boards would provide professional and clinical leadership for all pharmacists providing NHS pharmaceutical care services.
Drivers for Change and Evidence
1.1.3 Some of the additional drivers for change are listed in Appendix 1. Alongside the Wilson and Barber Review[5], a number of other key documents, reports and pilots have provided evidence for the development of the Vision. They are listed in Appendix 2. Appendix 3 acknowledges the achievements through The Right Medicine[6].
Patient Journey in 2020
For me the way I look after my health has changed over the last 5 years. Last year I went into hospital after a heart attack. I had suffered for 3 years previously with angina and also more recently had problems with my breathing which had started a couple of winters ago after a chest infection. My GP told me I had chronic obstructive airways disease (COPD) which had been caused by my years of smoking and that it could get worse if I didn't stop smoking. I had been a smoker for over 40 years and at the age of 63 I felt too old to be breaking old habits! My GP had asked me to see the pharmacist who worked closely with my GP for a review of my breathing after a chest infection. Before this I had only seen my pharmacist for advice for winter ailments as I was on a list of medications. The pharmacist gave me a self-management plan for my breathing and showed me how to monitor my treatment, I felt much more in control and knew I could ask for help when needed. After this one weekend I felt my chest was flaring up and after getting advice from the pharmacist started to take my antibiotics that she had prescribed as a standby. It was wonderful as normally I am ill for weeks afterwards as I normally wait until I am really poorly before I make an appointment to see my GP. After this the pharmacist provided me with support and prescribed treatment to help me stop smoking. It took me a while but she was very supportive and helped talk though all the issues that I had. Its six months since I quit and I am less breathless. My breathlessness score is better and I have not had so many chest infections.
Anyway, when I was admitted to hospital, the pharmacist gave the pharmacist in hospital a list of my tablets that I was taking. Just as well as in the shock of it all, I had forgotten the new one I had been started on. After my heart attack, I was put onto some additional medicines and the dose of others was increased. The pharmacist in the hospital had sent all my medication changes to my pharmacist who reviewed all my medication and then ran through the changes with me. I couldn't understand why I was taking a higher strength of my cholesterol tablets and also why I needed a new tablet for my heart as my blood pressure was fine. The pharmacist working with my GP sees me every six months to manage my COPD and heart conditions and I see the GP when I need to.
They record everything on one system so the GP and pharmacist both seem to know what's going on with my care. It seems like a great team effort.
Figure 1: Vision For Future NHS Pharmaceutical Care Of Patients In Scotland
1.2 The Future
1.2.1 This Action Plan provides a vehicle to deliver pharmaceutical care of NHS patients fit for the 21st century. Pharmacists are highly qualified and skilled healthcare professionals who make a significant contribution to healthcare in Scotland, however their full potential is yet to be fully utilised within NHS Scotland to help deliver the 2020 Vision for health and social care.
1.2.2 The Government's manifesto contains a commitment "to further enhance the role of pharmacists, building on the introduction of the Chronic Medication Service, and encourage even closer joint working between GPs, pharmacists and other community services …"
1.2.3 This Action Plan recognises the important traditional role of the supply of medicines from registered pharmacies located in high streets across Scotland. Scottish Government Health and Social Care Directorates will continue to work with pharmacy owners and NHS Boards to ensure an efficient and cost effective pharmacy network for the supply and dispensing of NHS prescriptions and other aspects of NHS pharmaceutical services which are best delivered from registered pharmacy premises.
However, integrated delivery of care, as set out in the 2020 route map, will require the delivery of NHS pharmaceutical care to consider new and innovative models to facilitate professional independence of pharmacists working in partnership with other health and social care professionals and the third sector. These new and innovative models will explore, for example, the concept of clinical pharmacist group practices to complement the traditional pharmacy network.
A Clinical pharmacist provides patient care that optimises care and use of medicines for patients in all settings often collaborating with medical and other healthcare professionals. Clinical pharmacists are regarded as the experts in therapeutic use of medicines
1.2.4 In the future, pharmacists delivering NHS pharmaceutical care should be clinical pharmacist independent prescribers, who may have allocated workloads to target their clinical skills to patients who would most benefit from the continuity of care provided, by working in partnership with the medical profession to optimise the use of medication which would include monitoring and adjusting treatment.
1.2.5 The Vision also builds on the pharmacist's role in encouraging and supporting the individual patient to manage their own condition(s) which is central to the concept of Co-production. Co-production is the process of active dialogue and engagement between people who use services and those that provide them, putting the service user on the same level as service provider. Co-production recognises that each of us has skills and knowledge, and the ability to develop these. It also recognises that access to support from family, neighbourhood and community allows for greater independence.
Co-production designs support and services around what people can do for themselves, rather than seeking to make them more dependent. It offers the potential to enhance both quality of life and longevity through focusing on the assets that promote the self-esteem and coping abilities of individuals and communities.
1.2.6 Pharmacists have a role in the healthcare team to monitor the adverse effects of medicines as well as their clinical performance to optimise their safe and effective use. This is known as pharmacovigilence. Monitoring patient outcomes when treated with new medicines presents opportunities for closer working between the medical and pharmaceutical professions and the pharmaceutical industry.
1.2.7 The Wilson and Barber Review[7] highlighted that patients would generally welcome greater continuity around the pharmacist providing their pharmaceutical care. In addition, evaluation of the smoking cessation component of the community pharmacy Public Health Service[8] found that outcomes were often better for patients when they regularly saw the same member of pharmacy staff.
Scottish Government believes that more needs to be done to provide consistency and continuity and the concept of the named pharmacist will be explored when considering the delivery of NHS pharmaceutical care.
1.2.8 NHS Boards are responsible and accountable for the provision of pharmaceutical services in secondary and primary care sectors. Currently in primary care, NHS Boards make arrangements with pharmacy owners for the delivery of pharmaceutical services. The pharmacist delivering these services needs to ensure that their priorities are focused on the patient above all else. Perverse incentives such as targets and bonuses based on commercial retail priorities should not be allowed to adversely affect patient care.
Scottish Government will explore new and innovative models to facilitate the professional independence of the pharmacists delivering care to patients.
1.2.9 For an ageing population that has increasing multiple morbidities (more than one medical condition), delivery of NHS pharmaceutical care to all patients in all settings is essential. However, it requires a step change in establishing collaborative partnerships within an integrated health and social care system in order to achieve the best possible outcomes from medicines.
1.2.10 Medication is by far the most common form of healthcare intervention. Four out of five people aged over 75 years take a prescription medicine and 36 per cent are taking four or more[9]. However, it is suggested that up to 50 per cent of drugs are not taken as prescribed, many drugs in common use can cause problems and that adverse reactions to medicines are implicated in 5 - 17 per cent of hospital admissions[10].
1.2.11 Research has demonstrated that patients on multiple medications are more likely to suffer drug side effects and that this is more related to the number of multiple morbidities a patient has than age. There is a clear and steady increase in the number of people admitted to hospital with drug adverse effects[11]. Individuals admitted with one drug side effect are more than twice as likely to be admitted with another. This situation can be accentuated by altered pharmacodynamics and pharmacokinetics (changes in how the body deals with drugs) associated with either ageing or illness.
1.2.12 A top priority in pharmaceutical care is to prevent predictable side effects and optimise clinical outcomes with medication.
1.2.13 The Wilson and Barber Review highlighted particular concerns about the pharmaceutical care of both residents in care homes and those where care at home services are provided within social care arrangements.
This Action Plan prioritises these areas for early consideration with regard to new and innovative ways of service delivery. This will also include consideration of any issues which may adversely affect the care of patients in these environments.
1.2.14 The hospital sector is responsible for the provision of treatment of those patients living in their homes but still receiving specialist care by their hospital consultant. This is an expanding area of healthcare and presents opportunity to explore innovative pharmaceutical care provided through integrated working between the hospital, community pharmacists, medical practitioners and the pharmaceutical industry.
1.2.15 In some parts of rural Scotland, the NHS relies on dispensing doctors to provide dispensing services to their own patients who (through geography and demographics) are unable to secure the dispensing services of a community pharmacy. In these cases the dispensing doctor service plays a vital role in the provision of NHS medicines.
The Scottish Government will work with patients, dispensing doctors and appropriate stakeholders to explore how rural communities can be further supported in terms of pharmaceutical care.
1.2.16 Central to the future development of NHS pharmaceutical care is the importance of sharing of patient information between pharmacist delivering NHS services and other health and social care professionals in secure and confidential systems. This will be explored with patients, the medical and pharmaceutical professions, the NHS and other relevant key stakeholders.
1.2.17 The delivery of future innovative pharmaceutical care may require novel models for clinical practice and joint working which will create new demands on undergraduate and postgraduate education. These opportunities will be explored with NES, the professional bodies and the Schools of Pharmacy and Medical Schools in Scottish Universities.
1.2.18 The development of innovative pharmaceutical care will take place over the next 10 years and will focus on the three key Quality Ambitions, namely: person-centred, safe and effective care.
The Vision and Action Plan will be delivered through joint working between Scottish Government, NHS Scotland, health and social care professionals, patients and other appropriate key stakeholders.
Conclusions
Our Action Plan will build on the recommendations of the Wilson and Barber Review and related health and social care policy, and will clearly position the pharmacist's contribution to delivering measureable progress in support of the 2020 Vision and Route Map.
This work will be taken forward under a governance structure with the Scottish Government Health and Social Care Directorates to consider each of the areas identified for development, and to provide a detailed work programme and delivery plans. It will also take into account any additional requirements resulting from the implementation of the 2020 Vision.
Chapters 2-5 set out the Action Plan as the three main aims of the quality ambitions, person centred, safe and effective with the underpinning of the infrastructure that will be needed for delivery. At the end of each chapter we have set out the main areas to deliver the Vision.
Contact
Email: Martin Moffat