Personalising Realistic Medicine: Chief Medical Officer for Scotland's Annual Report 2017-2018
The Chief Medical Officer's fourth annual report on Realistic Medicine, with a focus here on the principle of Building a Personalised Approach to Care.
Chapter 4 Personalising Realistic Medicine Across Our Principles
My report has explored the ways in which we can build a personalised approach to care – both for our patients and for our workforce. But, to deliver our 2025 vision, we need to go further and consider the other Realistic Medicine principles too. In this chapter, we explore the synergies between each principle and the personalised approach to care.
Changing Our Style to Shared Decision-Making
Of all principles, shared decision-making is the one with the most obvious links to building a personalised approach to care. Put simply, it is hard to conceive of how one could be achieved without investing time and skills in developing the other. In 2018, the Scottish Government conducted a mixed-methods study investigating good practice in shared decision-making and consent.[31] The work consisted of 3 phases: a literature review on current policy and guidance; a group consultation with the Person-Centred Stakeholder Group; and an online survey for NHS Board Medical Directors and Clinical Governance Leads. The key finding was that all healthcare professionals should adopt a personalised approach within their practice. The report’s main recommendation was to ‘bring the conversation back to the room’ – to allow a rich and meaningful dialogue built on partnership and placed at the heart of every interaction between those giving and receiving care. The study suggests that we:
- Provide more guidance on effective ways of communication to enable health professionals to clearly explain risks, benefits, outcomes and alternative treatments;
- Develop a national standardised repository of validated evidence-based information about treatments and procedures and the associated risks;
- Provide clear guidance on the appropriate use of, and better access to, high quality decision-making aids for healthcare professionals and patients;
- Provide staff with education and adequate skills to communicate information clearly to the patient and ensure the patient has understood it (‘teach-back’ technique); and,
- Provide staff with training on how to build a more supportive relationship with the patient to enhance person-centred consultations.
It is interesting to reflect on how closely several of these findings match the recommendations of the Citizens’ Jury (Chapter 2), and we must act on them.[14] In January 2019, with support from the Scottish Government, NHS Education for Scotland appointed a lead for Realistic Medicine. Their role will be critical in supporting training programmes on shared decision-making and value-based healthcare to help us practise Realistic Medicine and deliver more personalised care. As part of this work, we will also promote training and resources that exist already, such as Effective Communication for Healthcare (EC4H) workshops, available in many NHS Boards.[32] These communication workshops have been designed for a range of different professionals and cover topics including anticipatory care planning, shared decision-making and challenging communication scenarios.
Reducing Harm and Waste
‘Personalised healthcare and population healthcare are two sides of the same coin’.
Muir Gray
Realistic Medicine is responding to the twin threats of harm and waste in healthcare by focusing on the concept of value. In Realising Realistic Medicine, I explored the relationship between value for a population and value for an individual using this graph from Muir Gray (see Figure 1).[2]
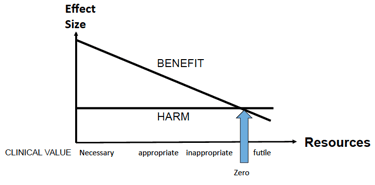
Figure 1: Donabedian-style graph of the relationship at an individual level between healthcare benefits and harms, and increasing resources
It shows that, when there is only enough resource to make interventions available to a few, they are offered to people who have most to gain and who are more willing to accept risk – in these circumstances, it is more likely that we are delivering high value healthcare. However, as investment increases, interventions are offered to people who are less severely affected, so the maximum benefit that this person can expect is less but the probability and magnitude of harm remains the same. This can produce low or even negative value healthcare. By building a personalised approach to care, we are better placed not only to communicate these concepts to our patients, but also to understand what benefit and risk means in the specific context of their lives.
A personalised approach to care can reduce harm in other ways too. An adverse event is a situation where a person experiences an outcome of treatment or care that is unexpected and unwelcome. There can be lasting psychological and emotional consequences for those affected directly and for the staff involved. In Scotland, Being Open provides a best practice framework for all healthcare organisations in such a situation.[33] It creates an environment where patients and their families feel supported and where healthcare professionals and managers have the confidence to act appropriately. Psychological harm to families following an adverse event is reduced when they experience compassionate care, when their perspective on the event is valued and when they are central to the review of care.
‘I think patients and families find it very positive, which is bizarre when it can be something very negative that’s happened to them. But from my experience, they don’t expect you to be so honest and open with them and when you are, I think they truly value that, and I think they trust you more because they feel you’re not hiding anything from them’.
Midwife trained in Being Open
‘The best endorsement is we have come out the other side happily...we were so well supported. The lasting benefit is that I don’t really think about it at all now...’
Parent receiving Being Open care
Future harm is reduced when staff engage with the learning and improvement generated from the adverse event review reports. In maternity services in NHS Lothian, staff realised that families were not being involved consistently in the reviews of care that followed adverse events. With Being Open, staff have worked to overcome barriers in communication with families, so that they are able to engage soon after an event in an open and transparent manner and elicit their concerns effectively. These concerns are then incorporated into the review and families are supported as feedback is shared from the review report. Families now report greater trust and confidence in the service and the NHS Board. Staff feel more confident about building relationships with the families and more confident about being able to provide personalised care.
Tackling Unwarranted Variation in Practice and Outcomes
Variation in healthcare exists because health systems are complex and the population has differing needs. Unwarranted variation is variation in healthcare that cannot be explained by need, or by explicit patient or population preferences.[34] Persistent unwarranted variation is of concern because it affects health and social care funding, equity of access to healthcare, and can cause hidden harm. Identifying and addressing this is essential to improving outcomes and to delivering Realistic Medicine.
In earlier Realistic Medicine reports, I outlined our plans to support clinicians to tackle unwarranted variation through our Value-Based Healthcare (VBH) work program. Over the past year we have made great progress, appointing Realistic Medicine Clinical and Finance Leads across Scotland, training them and 120 others in the principles of VBH and awarding funding to support 11 VBH improvement projects. In September 2018, we published the beginnings of a Scottish Atlas of Healthcare Variation and have added new maps on a regular basis, with plans for continued expansion in the months and years to come.[35] The Atlas is publically available and highlights geographical variation in the provision of health and care services and associated health outcomes across Scotland. Each map is accompanied by an explanatory narrative to support public understanding and interpretation of the Atlas. Box 7 displays our Atlas map for cholecystectomy (surgical removal of the gallbladder).
As discussed in Realising Realistic Medicine, the Atlas does not set out to explain this variation or provide a measure of performance. It does not say what the ‘correct’ rate of a procedure or treatment is or indicate that high or low is bad and average is ideal. Instead, it is a tool which provides informative and easily accessible data to allow clinical teams to question, debate and explore the variations demonstrated, and use these conversations to promote quality improvement. It is hoped that the Atlas will help to identify over- and under-treatment across Scotland and support healthcare teams to generate solutions to reduce waste and harm.
Box 7 – How to use the Scottish Atlas of Healthcare Variation
Prior to publication, we tested the Atlas with healthcare professionals, the public and policy makers. We used their feedback to refine and improve the Atlas, and continue to encourage users to let us know how they are using the Atlas and how we can make it better. Information Services Division (ISD) Scotland have created several user guides, videos and Frequently Asked Questions to assist clinicians in understanding and interpreting the data, and will be hosting Webex training sessions to increase understanding.
The Atlas is interactive. It allows the user to choose how to display the data and gives a demonstration of geographical variation and variation over time.
The images below demonstrate rates of cholecystectomy across Scotland:
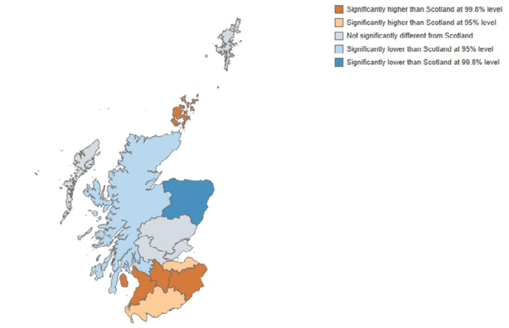
Maps – the map highlights each NHS Board in a colour indicating how significantly different the standardised rate is from the Scotland value, and in which direction. Significance is based on whether the Scotland value falls within the confidence interval of the value for the NHS Board, at two confidence levels: 95% and 99.8%.
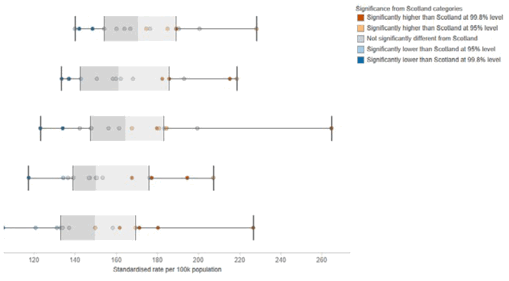
Boxplots – the boxplots show the standardised rates for NHS Boards in sequence from lowest to highest, for each financial year. A central ‘box’ indicates the inter-quartile range: that is, it extends from the 25th to the 75th percentiles (the middle 50% of data values), with the median indicated by a line. The ‘whiskers’ extend out to the minimum and maximum values. The fold-value is also shown under the financial year to allow quick comparison across the time period.
While there may be less overlap between tackling unwarranted variation at a population level and building a personalised approach to care, the two principles are not mutually exclusive. The Specialist Palliative Care Service in NHS Fife has developed an innovative model of best supportive care aligned to both principles.[36] The catalyst for change in Fife was the recognition by staff that many patients with advanced lung cancer were in their last weeks of life at diagnosis, with only a small window to benefit from best supportive care (i.e. palliative care when anti-cancer treatment is not possible). Some patients were receiving high quality care delivered by a range of professionals, often in primary care, but others received little or no support.
‘If somebody had explained to us, not necessarily what was going to happen, but what was available to us. You just felt…”into the abyss”’.
A patient before NHS Fife’s new model of best supportive care
This variation in experience was not accounted for by difference in need. Instead, it reflected variation in the system, with professionals describing ad hoc referral routes, lack of clarity around roles, inconsistent follow-up and suboptimal communication. The new model of care has tackled that unwarranted variation by ensuring that patients are consistently identified and all receive a personalised approach to care, including prompt multidisciplinary assessment, support and follow-up in a location that suits the person’s needs and preferences. Through shared decision-making, patients are supported to pursue only the follow-up that is likely to be of benefit. Routine hospital appointments, when deemed no longer necessary, are cancelled. Information about patient wishes is shared reliably across the health system. Feedback from patients, carers and staff has been overwhelmingly positive.
‘Everything they said they would put in place happened’.
A patient receiving NHS Fife’s new model of best supportive care
Managing Risk Better
Health and social care professionals are increasingly aware of the need to manage risk effectively but, for many, this can lead them to practise defensive rather than Realistic Medicine. In previous reports, we have discussed how communication failures are a common theme in most complaints, particularly those around consent. It is not just lack of communication but the nature, frequency and content of it. By building a personalised approach to care, we reduce this risk. We become more transparent in our conversations, more open and meaningful in our dialogue about the risks and benefits of different courses of action, and more aware of what matters most to the person. This leads to less criticism and fewer complaints rather than more.
‘One of our roles as professionals is to be leaders in openness and I include when things go wrong, as well as when things go well. When facing dilemmas, we must acknowledge them to the public that we serve, rather than try to overly finesse the information’.
Peter Homa
Adopting a personalised approach can also help us to manage risk at a system level. Human Factors and Ergonomics (HFE) is the scientific discipline concerned with understanding and improving the ‘fit’ between people and their working environment to ensure a safer, more productive and efficient workplace. It is about designing for people and supporting our workforce. Scotland is well-recognised internationally for its success in many fields of interest to HFE, such as non-technical skills training for surgeons and anaesthetists, clinical skills and simulation, the Scottish Patient Safety Programme, team working initiatives, safety culture assessment, significant event analysis and safety checklist design in primary care.
But substantial work still needs to be done in spreading and normalising HFE thinking and practices. Over the past two years, NHS Education for Scotland and the Royal College of Surgeons of Edinburgh have co-led ongoing national development work to plan how best to integrate HFE into everyday health and care delivery. The goal is to embed these concepts as seamlessly and successfully as in other safety-critical industries, such as energy and transport – sectors which are significantly less complex and risky than healthcare but paradoxically attract considerably more HFE-related attention. Working in partnership with over 150 colleagues from NHS Boards, universities and professional bodies, they have identified priority areas where HFE can potentially add value to existing efforts to improve care system performance (e.g. care safety, productivity, efficiency, reliability) and workforce wellbeing (e.g. health and safety, patient experience, staff welfare, work enjoyment). In this sense, valuing the person (patient or staff) is both the input and the output of the HFE process.
Becoming Improvers and Innovators in Healthcare
‘A desk is a dangerous place from which to view the world’.
John Le Carre
For our vision of Realistic Medicine to be realised, professionals need to feel empowered to embed its principles in to those parts of the system that they best understand. This requires each person to be at the forefront of improvement and innovation in their local area. To lead the change rather than be led.
Effective improvement and innovation is all about people. In his seminal work on quality management, Joseph Juran emphasises the importance of quality planning and understanding needs and assets from the customer’s perspective when setting priorities for improvement.[37] He also highlights the value of building relationships and supporting individuals to become equal partners in co-producing services. These principles have such strong relevance for health and social care that aspects of Juran’s quality framework have been adopted for use by Healthcare Improvement Scotland.[38]
It has been said that ‘people ignore design that ignores people’ so, when making improvements to the way we deliver healthcare, we must always engage with our patients, their families and our staff.[39]
A fantastic example of where this approach has been successful is in the redesign of the Emergency Department (ED) in Ninewells Hospital, NHS Tayside. Here, NHS staff, local medical students and design students from Duncan Jordanstone College of Art and Design at the University of Dundee collaborated with patients and families to improve people’s overall experience of the ED. The medical students shadowed patients through their journey and gathered information by questionnaire. Most people were very satisfied with their experience but were keen for more information about how long they would wait, who they would see and what might happen after they were seen.
The students then worked with colleagues in interior, graphic and product design to produce wall art that illustrated the process (see Figure 2). Patients were able to use this to follow the standard journey through the ED and learn more about the roles and responsibilities of staff wearing each type of uniform. Patient information cards were created to explain why there might be delays in being seen. These prototypes were then tested.
Figure 2: New Wall Art for Emergency Department in Ninewells Hospital, NHS Tayside
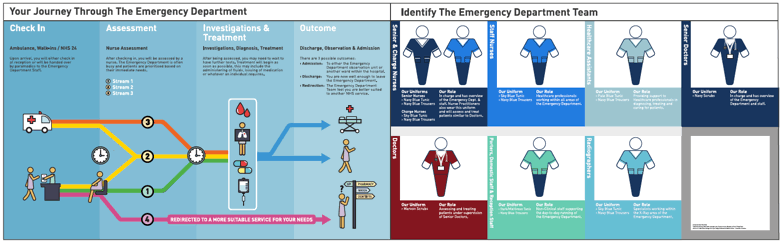
Before the introduction of these cards, 1 in 5 patients could identify different members of staff and their roles and 60% felt they knew why they were waiting and what the next step in their journey would be. After the design work, all patients were able to answer these questions. The department has now been redecorated accordingly.
Conclusion
I very much hope that my report has demonstrated that, while the principles of Realistic Medicine are presented visually as distinct entities, they are, in practice, inter-related and inter-dependent. I also hope that it is clear that building a personalised approach to care is the running motif throughout our Realistic Medicine vision and our most important objective.
In our first report in 2016, I asked ‘can we’ achieve these principles. Having witnessed the fantastic progress that’s been made over the last 3 years, it is clearly now time for this to change. I am convinced that, together, ‘we can’ build a personalised approach to care. And I believe wholeheartedly that we can deliver Realistic Medicine.
Contact
Email: stephen.fenning@gov.scot