The Penrose Inquiry recommendation
Short-life working group report on the Penrose Inquiry recommendation on infection of people with Hepatitis C from NHS treatment.
5 Background
5.1 Hepatitis C: Key facts
5.1.1 General
- Between 100 and 200 million people worldwide are infected with Hepatitis C. In the EU the figure is around 6 million; in the UK 214,000 and in Scotland 37,000.
- In resource-rich countries, injecting drug use is the principal route of Hepatitis C transmission while in resource-poor ones, sub-optimal infection control associated with healthcare procedures is the main cause.
- 8-16% of people infected with Hepatitis C for 20 years have cirrhosis of the liver. Disease progression is accelerated by, in particular, excessive alcohol consumption and HIV co-infection. People who acquired their HCV through blood transfusion, generally, have a disease progression rate at the lower end of the spectrum, probably because they tend to have less liver disease co-morbidities such as excessive alcohol consumption.
- Hepatitis C's role in causing serious illness and death from cancer or liver failure is well recognised but infection is also associated with non-liver related disease and psycho-social morbidity.
- Prevention of Hepatitis C is dependent on interrupting routes of transmission. A vaccine is unavailable and is unlikely to become available in the near future.
- Diagnosis of Hepatitis C is imperative to allow people to be assessed for treatment but also provides an opportunity to drive home behavioural change messages in terms of preventing onward transmission of infection (especially among people who inject drugs) and reducing the risk of disease progression (e.g. warnings about the dangers of excessive alcohol consumption).
- The efficacy of antiviral treatments which eradicate HCV infection has increased dramatically over the last 20 years; oral safe, short duration therapies with cure rates of over 90% will be available for all major genotypes in 2016.
5.1.2 Scotland: Estimates for Scotland's HCV Chronic Population
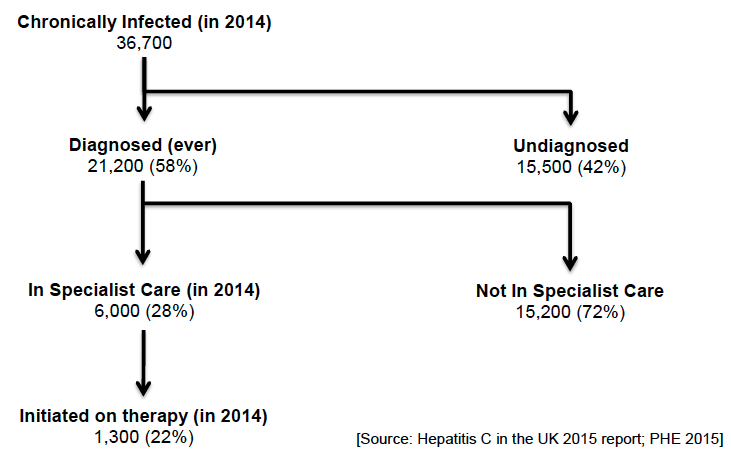
5.2 Scottish Government Response to Hepatitis C
2006: Launch of Scotland's Hepatitis C Action Plan Phase I: Development of a case for investment in Hepatitis C service provision.
2008: Launch of Scotland's Hepatitis C Action Plan Phase II:
Investment of £43 million for Hepatitis C prevention,
diagnosis and care services during
2008-11.
2011: Launch of Scotland's Sexual Health & Bloodborne Virus Framework (Phase I) incorporating continued investment in Hepatitis C services and adopting an outcome indicator approach to monitoring the impact of the investment.
2014: The establishment of Scotland's HCV Treatment & Therapies Group to generate guiding principles for service providers and users in the era of new highly effective antiviral therapies.
2015 Launch of Scotland's Sexual Health & Bloodborne Virus Framework (Phase II) incorporating continued Hepatitis C service investment, the employment of which is to be steered by the principles generated by the Hepatitis C Treatment & Therapies Group.
5.3 Impact of Scotland's Response to Hepatitis C and the Challenges Ahead
During 2006/ 0 7-2014/15:
- An estimated 50% reduction in the annual number of new HCV infections from 1,500 to 750.
- An increase in the proportion of the total estimated infected population who are diagnosed, from 38% to nearly 60%.
- A four-fold increase in the number of new initiates onto antiviral therapy annually from 450 to approximately 1600.
- An overall reduction in the estimated number of people
infected from 38,000 to near 36,000; the figure probably would
have been around 42,000 if there had been no response since 2006.
However, very considerable challenges exist:
- The annual number of new presentations of HCV-related liver failure/hepatocellular carcinoma ( HCC) increased from 100 to 190; approximately 40% occurred in people who had been HCV diagnosed within five years of presentation.
- 15,500 infected people, a high proportion of whom are older, former people who inject drugs ( PWID) with moderate or severe liver disease, remain undiagnosed.
- Most (near 75%) diagnosed HCV infected people are not in specialist care.
- Near 10,000 infected people likely have either cirrhosis of the liver (stage F4) or are in the pre-cirrhotic stage (F3) and, thus, are in urgent need of therapy; most are undiagnosed or are not in specialist care.
- Optimal therapies, while highly cost-effective for those with F3/F4 liver disease, are costly, particularly in the context of large numbers of such individuals being eligible for therapy now.
Contact
Email: Robert Girvan, robert.girvan@gov.scot