3. Universal journey for all children in Scotland
3.1 The universal journey
The universal journey defines the aspiration for all women, children and families in Scotland to access safe, effective and person and family-centred care and services. The aspiration of professionals is to support them through that journey, tailoring the intensity of support to meet need.
The universal journey is supported by the GIRFEC National Practice Model (Figure 1), Pathways for Maternity Care - Keeping Childbirth Natural and Dynamic ( KCND), Health for all Children (Hall 4) and the Personal Child Health Record.
Figure 1. GIRFEC National Practice Model
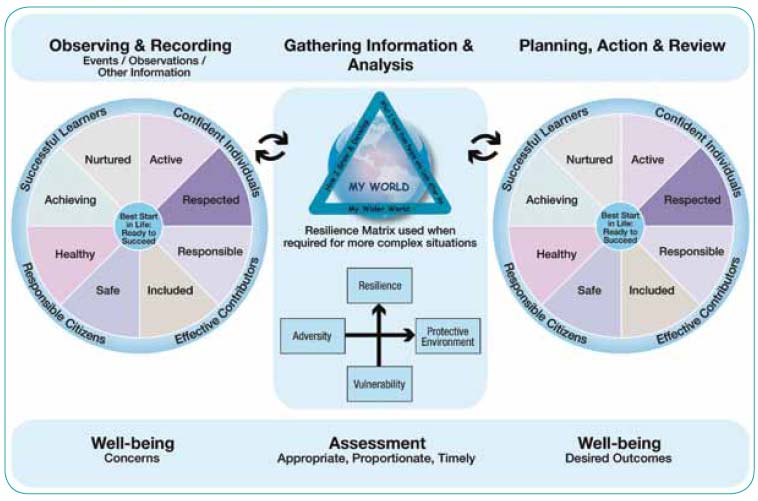
3.2 Universal pathway of core contacts
The universal pathway of core contacts has been included in this guidance at the request of practitioners and agencies. It provides a visual representation of how all children and families can expect to receive equitable support from health services.
Table 1. Universal Pathway pre-conception to 3
Time |
Interaction |
Pre-conception |
Up to 12 months before conception |
There is currently no universal approach to managing pre-conceptual health. However, Improving Maternal and Infant Nutrition - a Framework for Action18 and A Refreshed Framework for Maternity Care in Scotland19 highlight areas of concern that can contribute to poor health outcomes for mother and baby, such as poor nutrition and obesity. |
Antenatal - unborn baby |
First point of contact |
- Sensitive enquiry as to whether or not the woman is accessing any other services such as substance misuse, social work and psychiatric services, and any history of domestic violence.
- Information provided, scheduling of screening tests 20 and contacts, parent education sessions, locally available services to support pregnancy, birth and postnatal care and specialist services to support healthy lifestyle choices.
- Families who wish termination of pregnancy are offered appropriate information and counselling.
|
10-13 weeks |
- Maternity record updated (Scottish Women-Held Maternity Record ( SWHMR)).
- Care is planned with named midwife to meet identified needs.
- Information given: Ready Steady Baby. 21
- The named midwife undertakes to support the maternal and family journey throughout the antenatal period using guidance from the KCNDPathways for Maternity Care. 22
|
15-16 weeks |
- Maternity record updated, refreshed and needs are recorded.
- Consider engaging with the public health nurse/health visitor, family and other key professionals to allocate the Health Plan Indicator ( HPI) antenatally. 23
|
18-21 weeks |
|
22-41 weeks |
- Maternity record is refreshed and needs are recorded.
- Screening tests for height of uterus, blood pressure and urinalysis, oedema, fetal heartbeat, fetal movement and emotional well-being discussed and documented.
|
BIRTH |
Within first 24 hours |
- Maternity record is refreshed and identified needs are recorded to reflect needs of parent and baby using guidance from Pathways for Maternity Care in relation to physical/mental health and well-being, including emotional attachment.
- Infant feeding support is initiated and information on general care of baby is discussed.
- Full neonatal examination is performed within 72 hours.
- Within three days, screening tests of mother's mental health and well-being, blood pressure, temperature, respiratory rate, bladder and bowel function, perineum and pelvic examination/exercise are performed.
- If appropriate, anti-D and any relevant blood tests are performed.
|
Around 10-14 days (within 28 days) |
- The antenatal assessment and care plan, alongside what antenatal pathway of support has been followed, is discussed between the named midwife and the named public health nurse/health visitor.
The first visit (notification visit) is conducted by the public health nurse/health visitor, assessment of child and family circumstances is refreshed and the care plan updated.
- Information is provided on registration of the child with a GP, general child health surveillance and immunisation programmes and locally available services.
- The personal child health record 24 is given to the family, if it has not already been issued.
- The child is weighed.
- Newborn hearing screening test is performed.
|
6-8 weeks after birth |
- The public health nurse/health visitor record is refreshed and care plan updated.
- The first physical health and development check, including weight for child, is performed.
- The Edinburgh Postnatal Depression Score for maternal mental well-being is calculated.
|
3, 4, 12 and 13 months |
- "Childsmile" dental assessment is conducted.
- Weight check and immunisation performed.
- The Health Plan indicator ( HPI) 25 is allocated by the public health nurse/health visitor.
|
24-30 months |
- The 24-30 month review should cover the following as a minimum and may need to be expanded, depending on child and family circumstances and professional concerns: 26
- speech, language and communication
- personal, social and emotional development (including behavioural issues)
- nutrition, growth and weight
- immunisations
- parental concerns and issues
- vision, hearing and oral health
- physical activity and play.
|
