Open with Care – supporting people in adult care homes to have meaningful contact with others: progress report
This report summarises progress with the implementation of Open with Care - supporting meaningful contact in care homes guidance since publication. The report recognises the excellent progress and identifies key actions where care homes and partners can improve and embed good quality, meaningful contact as the norm.
Progress with resuming meaningful contact
This section considers the level to which indoor visiting has restarted and been sustained since publication of Open with Care, the reasons for indoor visiting not being supported (where that was reported), and changes to the frequency and quality of contact for residents.
Restarting visiting
Before lockdown came into force on 5 January 2021, just over half of adult care homes that submitted data on 21 December 2020 supported indoor visiting. After lockdown and as recommended in national guidance, this percentage fell to 4.0 per cent on 11 January 2021 (the next reporting date), and further to 2.7 per cent (under 30 homes) by 22 February. At this point, the majority of homes supported outdoor and essential visits only (61 per cent) or essential visits only (36 per cent).
Background on the Turas Care Home Management Tool
The Turas Tool has around 1,070 adult care homes registered and around 1,040 homes that have submitted data in a 30-day period. The tool has been developed to enable a consistent approach during the pandemic to early escalation as well as timely local and national care home support, information, intervention and governance with, for example, COVID-19 outbreaks. Data in the tool is self-reported by care homes. Care home visiting status data is published fortnightly as at the most recent Monday (previously published weekly). Care homes supporting indoor visiting is shown as a percentage of all homes on Turas that submitted data on that day (unless otherwise stated). Weekday response rates are high with just under 1,000 homes submitting data. Data is accessible to local oversight arrangements and the Care Inspectorate who use this to contact homes and support them to implement indoor visiting. It enables targeted improvement with care homes or providers.
Just before the guidance was published (22 February), the percentage of adult care homes that supported indoor visiting was 2.7 per cent. Since then, there has been a consistent and sustained increase in the support for indoor visiting. The largest increases were seen in March (62 per cent on 8 March, 82 per cent on 15 March) to reach over 90 per cent by the end of the month. In April, increases slowed as the final care homes moved to support indoor visiting. As at 14 June, the percentage of adult care homes supporting indoor visiting was 97 per cent. At the same time, the number of confirmed outbreaks in care homes has fallen.
For older adult care homes, the percentage of homes supporting indoor visiting, as at 14 June 2021, was 97 per cent and 93 per cent for other type of care homes.
Care home type
Care home type is based on Care Inspectorate registration. Registration type does not necessarily mean that this is the only type of resident in that care home. Care homes not registered as for older adults: Alcohol & Drug Misuse; Blood Borne Virus; Children & Young People; Learning Disabilities; Mental Health Problems; Physical and Sensory Impairment; and Respite Care and Short Breaks.
Chart 1 shows the percentage of care homes supporting indoor visiting between December 2020 and mid-June 2021, based on self-reported data, alongside the number of confirmed COVID-19 outbreaks in adult care homes.
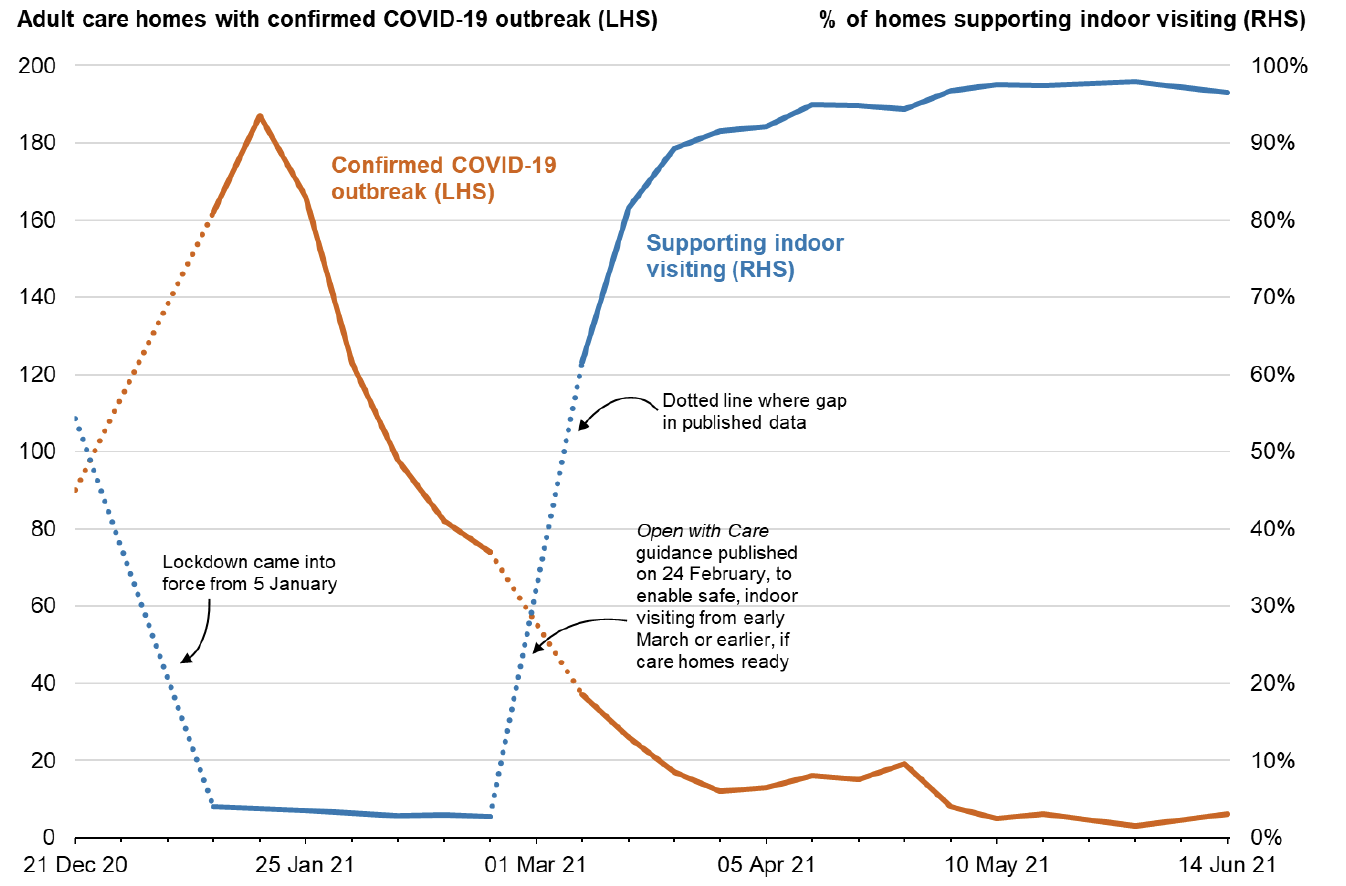
Note: '% care homes supporting indoor visiting' shown as percentage of all homes that submitted data on that day
Source: Turas Care Home Management Tool
In relation to the level of uptake, a number of care homes indicated lower than expected levels of visiting by friends and relatives. For some relatives and friends, the perceived risks of catching or passing on COVID-19 meant they stayed away from the care home. Some relatives reported having developed new routines during the COVID-19 restrictions, and now visiting less regularly than before.
Practical challenges to increasing people coming into care homes alongside COVID-19 protections have been reported by care homes and member organisations, mainly due to staff capacity and logistics. These include the additional demands associated with more testing of visitors. To ease this burden, care homes have asked for discretion to be able to allow visitors to test at home. This has to date not been possible due to the Medicines and Healthcare products Regulatory Agency (MHRA) advice around the use of LFD test kits that are currently supplied to care homes in Scotland. A small proportion reported issues with relatives' complying with protections in the care home (such as distancing or group size).
Care homes have also reported taking a range of actions to resume residents' contact, with some taking a very structured approach with dedicated time slots or areas. Some have put dedicated staffing in place (visiting coordinators) using the COVID-19: financial support arrangements for social care providers. While a more structured approach was supported within Open with Care as care homes initially resumed visiting, feedback from inspections indicates variation in how the guidance has been implemented. While some care homes have implemented Open with Care flexibly, there are reports that others are doing so more rigidly or inflexibly, creating additional burden for care homes and constraining good quality contact for residents as a result.
Where homes are not resuming indoor visiting
In Turas, care homes were asked to provide a reason where support for indoor visiting was not indicated. The most frequent reasons were:
- making preparations to resume indoor contact;
- care home's outbreak status;
- where indoor visiting is not routine practice or needed due to the type of care home service.
Respite services, particularly for people with a learning disability, would be an example of the last. In these, residents stay for a short stay and there is no reported demand for indoor visiting (although systems should be in place to support this, if desired, and essential visits also should always be supported).
Several other reasons were given by a very small number of homes including:
- guidance from local health protection teams
- waiting on 1st or 2nd vaccination dose
- non-COVID-19 related reasons (for example, diarrhoea and vomiting outbreaks), and
- staff members testing COVID-19 positive.
The vast majority of homes, however, have moved to support indoor visiting and, where not supported, the main reasons now are outbreak status and not currently applicable to the type of service.
More widely, care home provider groups' corporate visiting policies were previously seen to be a key barrier to the implementation of visiting guidance. Feedback suggests that these have become much more aligned to Open with Care, however challenges remain. These relate generally to more restrictive policies than recommended in Open with Care, for example in relation to visit length, enabling touch and wearing of PPE.
On publication of Open with Care, the Care Inspectorate published a position statement to the sector, outlining their expectation that providers implement visiting policy and practice, in line with the guidance. All care homes not doing so are contacted by the Care Inspectorate and support given to put this into place. Information is also shared with local oversight teams to support care homes' improvement in putting changes into place. Where homes do not make the necessary changes the Care Inspectorate will require them to do so in line with legislation.
Changes to the frequency and quality of meaningful contact
Turas asks care homes about the level of indoor visiting they are currently supporting. At 14 June, a growing number of care homes reported having increased indoor contact with residents beyond the starting point of two visitors per week, either to daily visits or group visits indoors. This equated to 155 homes (or 16 per cent) and 140 homes (or 14 per cent) respectively.
Whilst Open with Care was clear that two designated visitors per week should be seen as the minimum starting point, feedback has indicated this has been interpreted by some care homes as the maximum level. The data suggests that slow progress has been made towards increases in frequency, duration or number of people.
The quality of residents' contact with others is not currently collected via Turas. However feedback from a range of other sources provides some understanding of the nature of issues experienced by residents and relatives, where these occur. The Care Inspectorate look at relatives' experience and views including visiting at inspection but this is for purpose of inspection and not to collect national routine information.
Data from the Action on Rights team provide some insight into the quality of contact. Since their launch on 24 February and to 14 May 2021, they have supported 114 cases. The service reports many positive experiences around meaningful contact with friends and relatives which has positively impacted on everyone's wellbeing. However, progress reports from Action on Rights show several broad issues preventing meaningful contact for relatives:
- Variation in the interpretation and implementation of Open with Care. At times, this involved a local visiting policy different to the guidance, such as visiting in dedicated rooms rather than residents' rooms; time limits on visiting or a lack of support to visits out of the care home. High levels of anxiety, distress and confusion around visiting were reported among people contacting the service. In the first few weeks post publication, a lack of family confidence around using the guidance in conversations was reported; this was not reported by May. However there remained a hesitancy around direct contact with the care home for some, either by relatives or by Action on Rights, often because of fears about repercussions for their relatives.
- Another issue reported in May was a 'one size fits all' approach to risk assessments within the care home, preventing consideration of individual needs and preferences.
TIDE also reported family and care home staff concerns around others' perceptions of them as contact with loved ones resumed. Family members reported people thinking they were unimportant, inconvenient, 'just a visitor' or intent on causing trouble.
One family member stated: "I have been made to feel like my relationship with my mum doesn't matter".
In turn, staff reported feeling that people viewed them as controlling, or prison guards – or deliberately keeping families apart, including in negative media portrayals, with one staff member saying:
"There is a lot of abuse and allegations made on social media which are not true. In the press all you see is negative stories about care homes – it is not a balanced approach to the story (…) it doesn't talk about the effect it has had on us and all the time and work it takes to makes sure all the procedures and guidance are followed."
TIDE also reported that many relatives reported good experiences of care homes and of staff being caring, supportive and helpful, with one saying:
"Thank you for being there for my mum, I appreciate you so much. I look forward to the day when I can return as normal and help you out in return."
Feedback from the CPAG Engagement subgroup and Care Home Relatives Scotland members highlighted issues in the following areas:
- visit length;
- number of visits a week being limited (to the minimum of two weekly);
- visit location (in a public area not someone's room);
- lack of outdoor visits alongside indoor visits;
- residents' ability to leave the home;
- additional PPE and IPC requirements (e.g. being asked to wear gloves or touch being prevented);
- inability of staff and visitors to test at home;
- inconsistent advice to care homes from oversight teams/public health
- staffing levels;
- essential visits not being supported in all homes.
Since late March to 27 May, 28 concerns have been raised with the Care Inspectorate about Open with Care's implementation. These related to the quality of visits both indoor and outdoor, concerns around timings and length of visits that some services had put in place; lack of understanding and knowledge around what the guidance means, from a relative and friends' perspective; confusion among some care home relatives over what is an essential visit; relatives being refused entry by some care home services.
The Care Inspectorate has supported relatives by seeking resolution to their visiting concerns through mediation with the provider/care home. In most cases this approach has been successful; in the remainder formal complaints have been investigated and where these have been upheld, requirements for changes to visiting have been put in place to align with Open with Care.