Non-sexual violence in Scotland: report
Findings on the most up to date, complementary statistics on non-sexual violence in Scotland.
Part of
9.1 Annex 1 – Case Study – NHS Lothian Assault Injury Surveillance
Background
Over a number of years, NHS Lothian has established and refined a local approach to Emergency Department Assault Injury Surveillance. This was based on the ‘Cardiff Model’, developed by J. Shepherd and colleagues in Wales (see Sivarajasingham et al, 2016)[42]. The programme uses routinely collected clinical data to identify occasions where an individual’s attendance at an emergency department is identifiable as resulting from interpersonal violence[43]. These data are extracted from locally-held electronic patient records, cleaned and anonymised. Brief reports of the anonymised data are regularly shared with community safety partners to inform local decision making. Comparisons between these and police reported data have demonstrated that more than half of cases presenting to emergency departments related to incidents not reported to the police[44]. The following brief overview of some available data demonstrates how Assault Injury Surveillance can help inform the intelligence picture to support violence prevention.
Findings
In 2018 a total of 2,506 people attended NHS Lothian Emergency Departments with a violence-related injury. This represents a 17% reduction since surveillance began in 2013 when there were 3,009 attendances. In keeping with national findings, this demonstrates a downward trend over this period (Figure 20).
Figure 20: Number of attendances at NHS Lothian Emergency Departments with a violence-related injury, by year and sex
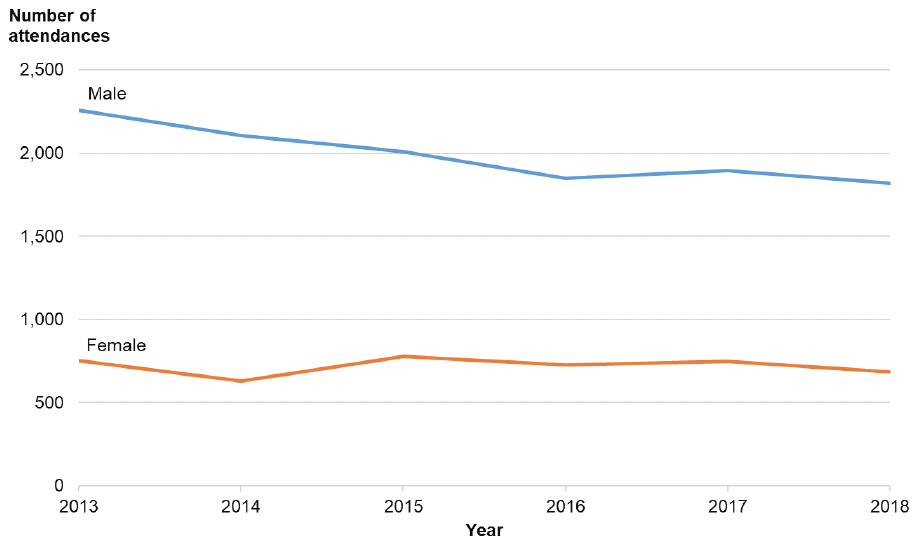
In 2018, males were more than two and a half times as likely as females to attend an emergency department as a result of violence (males = 4.7 per 1,000 population; females = 1.7 per 1,000 population – Figure 21). Rates of attendance in males have shown a strong downward trend with a reduction of 24% between 2013 and 2018. In females the changes in rates of attendance have been less consistent although, overall, there is a modest downward trend. These findings are broadly in keeping with national trends for non-sexual violence among males and females. It is interesting to note the persistence of a gap between rates of attendance for males and females at Lothian emergency departments. This pattern is consistent with trends seen in national emergency hospital admissions for assault; where reductions over time have been driven largely by males; but where males persist in constituting the majority of admissions (see Section 4.1.2).
Figure 21: Rate of attendance at NHS Lothian Emergency Departments with a violence-related injury per 1,000 population, by year and sex
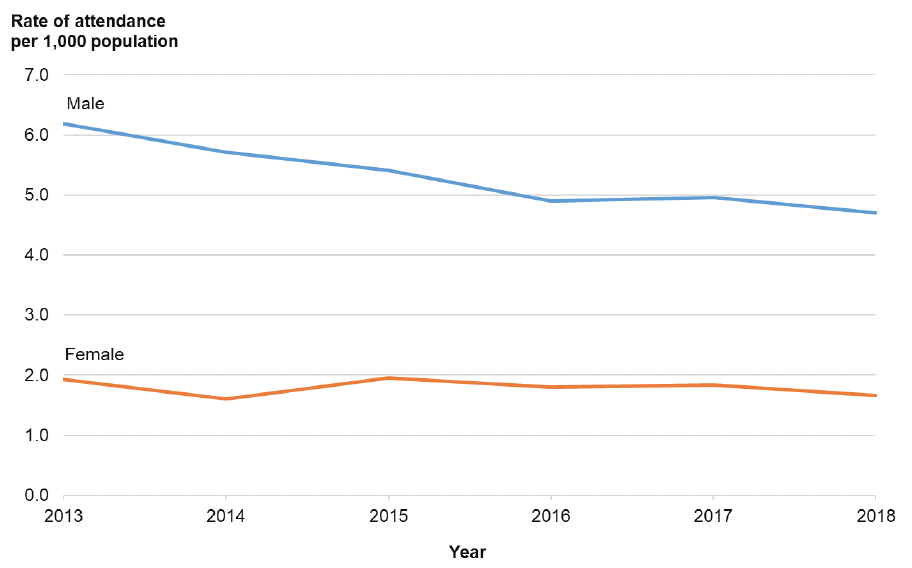
The majority of the decline in attendance appears to be driven by reductions in attendance by males aged: 10–19, 20–29 and 30–39 years (Figure 22). Within these three age categories there were 453 fewer attendances in 2018 when compared with 2013; a reduction of 24%. This is broadly consistent with analysis of the victims of certain more serious crimes (attempted murder and serious assault) in Police Recorded Crime records (see Table 2: Attempted murder & Serious assault victims by age group, 2008-09 & 2017-18.). The largest change in female attendance was seen in women aged 20–29 years with 64 fewer attendances; a reduction of 23% (Figure 23). Please note, due to small numbers we have excluded patients aged 0–9 years from this case study.
Figure 22: Rate of attendance at NHS Lothian Emergency Departments with a violence-related injury per 1,000 population by age group – males.
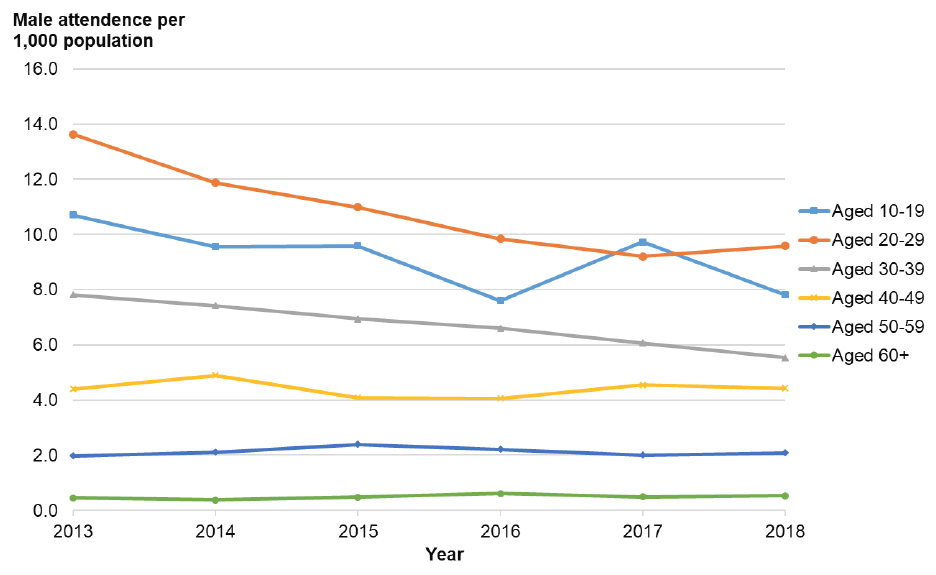
Figure 23: Rate of attendance at NHS Lothian Emergency Departments with a violence-related injury per 1,000 population by age group – females.
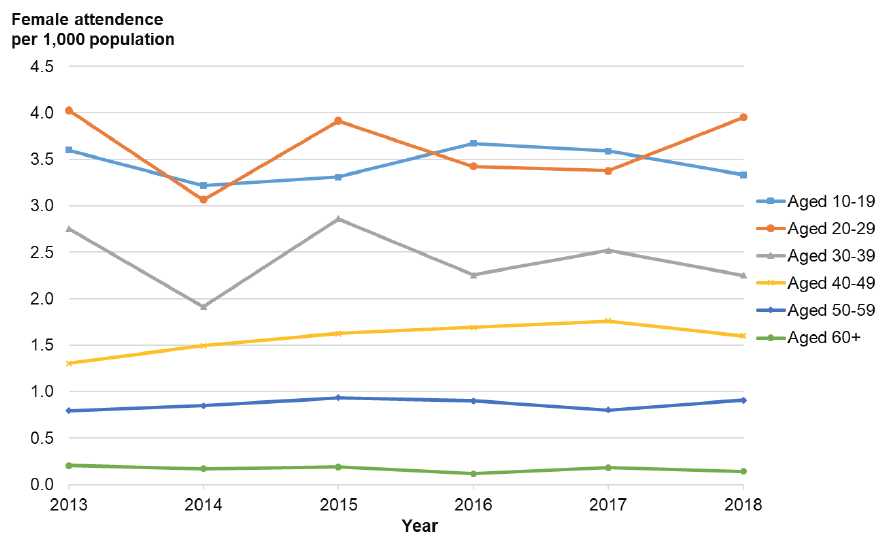
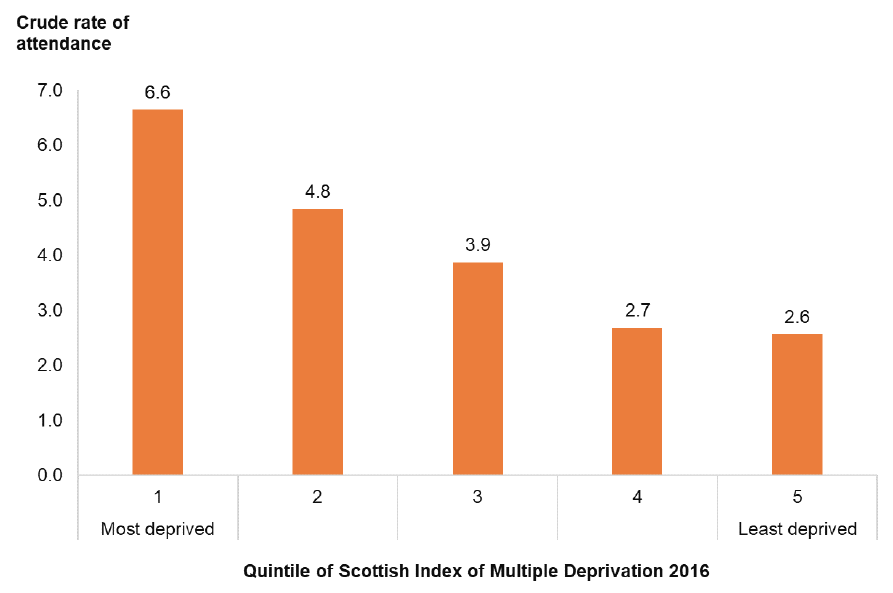
In Figure 24, attendance rates in 2017 are estimated for each quintile (20% group) of Scottish Index of Multiple Deprivation (SIMD 2016). This shows an association between an area measure of multiple deprivation and the estimated rate of experiencing a violence-related injury. In keeping with the findings of the SCJS and Police Recorded Crime data (see Section 4.1.4), a disproportionate burden of violence is seen to fall on those from more deprived areas. These Lothian data also demonstrate a clear gradient across all deprivation quintiles reinforcing the need for population-wide approaches to violence prevention which are proportionate to need.
Figure 24: Crude rate of attendance at NHS Lothian Emergency Departments in 2017 with a violence-related injury per 1,000 population by Scottish Index of Multiple Deprivation (2016) quintile
In 2018, the item the person was attacked with was recorded as ‘other’ or ‘unknown’ in 44% of cases. In the remaining cases where the item which injured the patient was specified, the injury was due to: body part, 82.7%; blunt object, 5.5%; bottle, 5.0%; knife, 4.8%; and glass, 2.1%. Due to large and varying proportions of patients where the item was recorded as ‘other’ and ‘unknown’ over time, it is not currently possible to comment on trends.
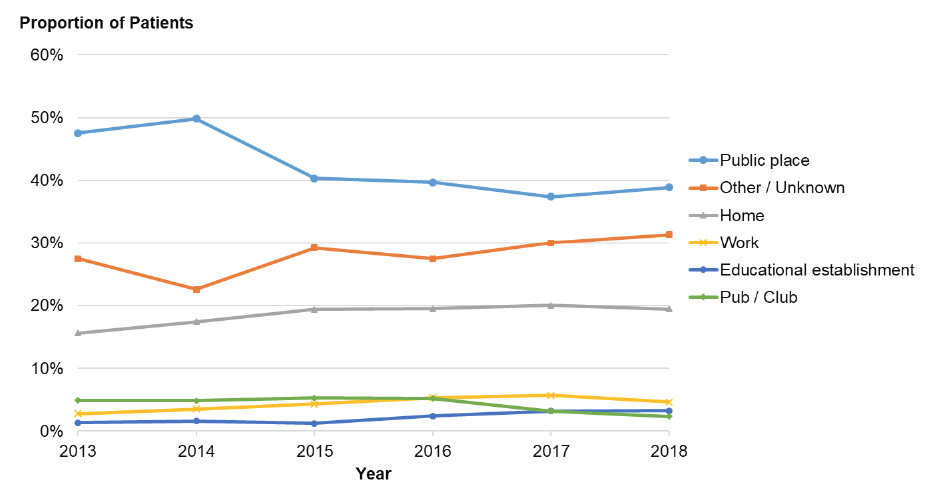
In keeping with the above issues around unknown data, around a third of patients did not have a location of injury recorded and this proportion has increased slightly in recent years (see Figure 25). Hence caution is advised when interpreting any apparent trends in these data but they may give some sense of where violence-related injuries are happening. For example in 2018, a large proportion of injuries occurred in a ‘public place’ (39%), followed by ‘other / unknown’ (31%) and home (19%). Again, these more common locations are consistent with national findings (Section 3.4).
Figure 25: Proportion of patients attending NHS Lothian Emergency Departments with a violence-related injury by year and location of injury.
NOTES: Data for patients aged 0–9 years have been excluded from this case study due to small numbers. A more detailed analysis of the wider NHS Lothian Assault Injury Surveillance data set is planned and will be published in due course
Acknowledgements: with thanks to NHS Lothian Emergency Department staff for gathering data, Mette Tranter for running the Surveillance programme and Caitlin Fox and Robyn Pascoe for analytical support.
Contact: Philip Conaglen, Consultant in Public Health Medicine, NHS Lothian Department of Public Health and Health Policy, philip.conaglen@nhslothian.scot.nhs.uk
June 2018
Contact
Email: Frances.warren@gov.scot