NHSScotland Chief Executive's annual report 2015-16
Presents an assessment of the performance of NHSScotland from 2015 to 2016 and describes key achievements and outcomes.
Chapter 3 - Improving the Health of the Population
'The greater recent challenges to our public health have come from … lifestyle behaviours, changing societal expectations and a new urban and suburban environment.'
Marie, who has the support of a Links Worker. You can read more about Marie's story and hear from her directly at www.nhsscotannualreport.com
Scotland has effective and mature public health systems which are the match, and in some aspects superior, to those across the developed world. Health protection arrangements have been tested in recent times through the outbreak of Legionella in Edinburgh in 2012, a patient with Crimean Congo Haemorrhagic Fever in Glasgow in 2013 and Ebola at the end of 2015. On all three occasions, the systems worked well and limited the risk to the public's health. Equally effective are our vaccination programmes (in childhood, for elderly people and for at risk groups). Uptake rates in most cases are higher than in other comparable countries and our programmes achieve and often exceed the level of immunity amongst the general population which means the unvaccinated population has a degree of protection (often referred to as herd immunity).
But, in common with all developed societies, the greater recent challenges to our public health have come from non-communicable diseases. These are largely created through lifestyle behaviours, changing societal expectations and a new urban and suburban environment which reduces individuals' opportunities to be physically active.
Tackling Inequalities and Strengthening Community Participation
One way of addressing the challenges that our urban and suburban environment place on us, whether as communities or individuals, is through use of the newly developed Place Standard.
The Place Standard derives from a commitment made in Scotland's architecture policy Creating Places [110] , and a recommendation arising from Good Places, Better Health [111] , the Scottish Government's strategy on health and the environment. Delivery of the Place Standard is integral to the Government's agenda on tackling inequalities and strengthening community participation. Launched in December 2015, the aim of the Place Standard is to support the delivery of high quality places in Scotland and to maximise the potential of the physical and social environment in supporting health, wellbeing and a high quality of life. Research shows that the quality of a place can have a direct impact on a community's quality of life, particularly in relation to health and wellbeing outcomes.
The Place Standard is an easy-to-use tool, framed around a set of 14 key questions that are central to the delivery of successful, sustainable places. Each question has been informed by the evidence base on the impacts of the physical and social environment on quality of life, and in particular, health outcomes.
| Theme | Question: In my place… |
|---|---|
| Moving around | can I easily walk and cycle around using good quality routes? |
| Public transport | does public transport meet my needs? |
| Facilities and amenities | do facilities and amenities meet my needs? |
| Natural space | can I regularly experience good quality natural space? |
| Play and recreation | do I have access to a range of spaces and opportunities for play and recreation? |
| Housing and community | does housing support the needs of the community and contribute to a positive environment? |
| Traffic and parking | do traffic and parking arrangements allow people to move around safely and also meet the community's needs? |
| Streets and spaces | do buildings, streets and public spaces create at attractive place that is easy to get around? |
| Identity and belonging | does this place have a positive identity and do I feel I belong? |
| Social interaction | is there a range of spaces and opportunities to meet people? |
| Influence and sense of control | do I feel able to participate in decisions and help change things for the better? |
| Care and maintenance | are buildings and spaces well cared for? |
| Feeling safe |
do I feel safe? |
| Work and local economy | is there an active local economy and the opportunity to access good quality work? |
The tool does not deliver a numerical outcome or overall 'score'. Instead the results are represented in a radar diagram format or 'place compass', as shown in Chart 1.
Chart 1: Sample Place Compass
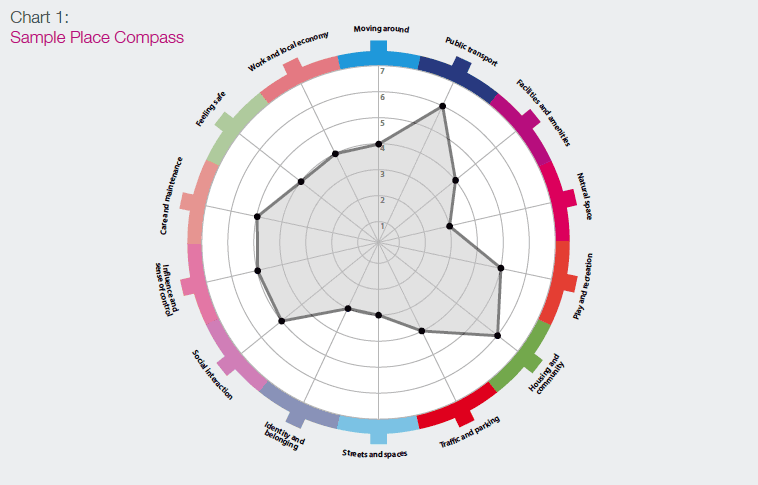
This represents an assets map of the assessment area, as identified by those carrying out the evaluation. Space within the tool is provided for comments, priorities and potential actions to be included. It has been designed so that communities and individuals can easily use the tool, but it is also useful to professional audiences.
The Place Standard produces visual outputs in diagram and text format. Its purpose is to instigate structured conversations on issues that are linked to improving quality of life and reducing inequalities. These conversations can generate positive and collaborative relationships, potentially leading to more informed decision-making, co-production projects and participative processes.
As an example, in East Dunbartonshire, a joint project led by the Community Planning Partnership with support from NHS Health Scotland and Keep Scotland Beautiful is implementing the Place Standard tool as part of planning for local improvement. Surveys, participatory workshops and one-to-one sessions will all use the tool as a central method to gather the views of communities about their local places, with a focus on localities within the council area that have a relatively high percentage of the population living in income deprivation. This approach is already having an impact in preparing for the production of the Local Outcome Improvement Plan.
There are several other parts of the country such as within Fife, Inverclyde, Shetland and South Queensferry (within the City of Edinburgh Council area) where the place standard tool has already been used, or is being used, to collect and collate local knowledge about a specific place in a consistent format; with the resultant data informing plans for action, change or development. The Place Standard Implementation Group is supporting work to build on early experiences and share good practice across all Local Authorities in Scotland.
As we develop measures to help communities come together and help shape their living spaces we also continue to focus our efforts on the individuals and families living in those communities to help them make healthier choices.
Chart 2: European Age-standardised Mortality Rates per 100,000 for People Aged Under 75 in Scotland
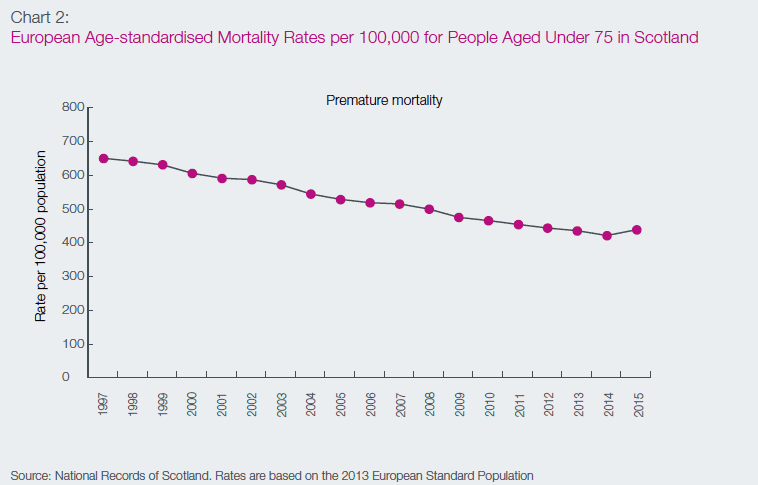
Source: National Records of Scotland. Rates are based on the 2013 European Standard Population
Reducing Premature Mortality
As a result of improved treatments and a greater focus on prevention, premature mortality (deaths among those aged under 75 years) has reduced substantially, down 17 per cent since 2005 to a death rate of 440.5 deaths per 100,000 population in 2015 (see Chart 2). Early deaths due to cancer - the leading cause of death - have reduced by 13 per cent over the last decade. Deaths due to heart disease and cerebrovascular disease are down by 41 per cent and 37 per cent respectively, while deaths due to diseases of the respiratory system have reduced by 11 per cent [112] . The increase by 4 per cent in premature mortality between 2014 and 2015 is likely to be due to the impact of the specific flu strain prevalent over the winter period. Older people were particularly affected by the flu strain, which also ran for a longer period of time than usual. Similar patterns were seen in a number of other European countries.
Tackling Alcohol-related Harm
Scotland is also seen as a world-leader in addressing alcohol-related harm. It was recognised several years ago that Scotland's relationship with alcohol had become unbalanced, and bold action has been taken to tackle alcohol misuse.
A whole-population approach is at the heart of Scotland's alcohol strategy, Changing Scotland's Relationship with Alcohol: A Framework for Action [113] , which includes a package of over 40 measures to reduce alcohol-related harm by helping to prevent problems arising in the first place. It also addresses improving support and treatment for those who are already experiencing problems.
Alcohol-related harm has an impact not only on individuals, but also on families and communities. Alcohol Brief Interventions ( ABIs) play an important preventative role in tackling this as part of a wider strategic approach to addressing problem alcohol use. The ABI Programme has focused delivery on three priority settings: Primary Care, A&E and antenatal services. In 2015/16, 97,245 ABIs were carried out, exceeding the target of 61,081 by 59 per cent [114] . The target has continued into 2016/17 to support the long-term aim of embedding ABI delivery into routine practice, with broadened delivery opportunities in wider community settings to increase coverage of harder-to-reach groups. If people feel better supported to live well within their community and to self-manage, they are more likely to avoid reaching crisis point, which can mean ending up in hospital.
Reducing Smoking and Tackling its Harmful Effects
Tobacco remains the primary preventable cause of ill health and premature death. It is associated with 127,000 hospital admissions and over 10,000 deaths each year in Scotland - around a fifth of all annual deaths. Annual costs to NHSScotland associated with tobacco-related illness are estimated to exceed £500 million per year [115] .
Reducing the number of people who take up smoking, supporting those who do smoke to quit and protecting people from second-hand smoke have long been clear public health priorities. The Scottish Government's Tobacco Control Strategy - Creating a Tobacco-free Generation [116] was published in 2013. This sets a bold and ambitious target to reduce smoking rates to 5 per cent or lower by 2034. The Scottish Health Survey for 2015 published in September 2016 reveals encouraging progress towards achieving this goal. It shows that 21 per cent of adults now smoke - one in five adults in Scotland. There was also a significant decrease from 2014 to 2015 in the proportion of children who were exposed to second-hand smoke in the home (11 per cent to 6 per cent) [117] .
NHSScotland continues to play a key role in tobacco control efforts. NHSScotland succeeded in achieving the Scottish Government's target of supporting at least 7,279 people to quit for at least three months in the most deprived areas between April 2015 and March 2016. Recently-published figures show that NHSScotland achieved 109 per cent of the target (7,047 successful three-month quits). This is despite the fact that the number of quit attempts made through NHS smoking cessation services in Scotland has fallen by 47 per cent since 2011/12 [118] .
This is likely to be due to a number of factors, including the rise in the popularity of e-cigarettes as a means of stopping smoking. Supporting people in deprived communities to stop smoking, particularly given the high smoking prevalence in this group, remains a challenge but will continue to be a priority for tobacco control activity.
It is not just people who smoke who are affected by the health impact of tobacco. Second-hand smoke also affects children who are exposed to it. Recent Scottish research shows that harmful chemicals from tobacco can linger in a room for up to five hours [119] . NHSScotland rolled out a nation-wide smoke-free policy for all its outdoor grounds as of April 2015. This built on the range of policies already in place across NHS Boards to deliver one Scotland-wide approach, and was supported by a national campaign that recognised the efforts of people who smoke in trying to comply with the policy. The Scottish Government included powers for Ministers to set perimeters around hospital buildings in legislation passed in April 2016. This will make it an offence to smoke within defined perimeters in hospital grounds. This will support implementation of smoke-free grounds.
In addition, the Scottish Government's Take it Right Outside campaign, launched in 2014, was developed with the support of NHS Boards to raise awareness of the risks of smoking indoors and supports people to not smoke in the homes of children. Help continues to be provided for those who want to quit. GPs provide expert advice and will direct people to a range of local services on their doorstep. Pharmacists have become a convenient frontline smoking cessation service for many people, providing smoking cessation products to help people quit with ongoing advice and follow-up support. Further information and advice is also provided through services such as Smokeline (0800 84 84 84) and the Take it Right Outside campaign.
Tackling Overweight and Obesity
Obesity rates in Scotland are among the highest in the developed world, with current projections suggesting obesity rates could be over 40 per cent by 2030 [120] . The Scottish Health Survey Results 2015 showed almost two-thirds of adults (65 per cent) in Scotland are overweight or obese, with 29 per cent classified as obese.
The proportion of boys of healthy weight (73 per cent in 2015) has increased year on year since 2011 (63 per cent) and is comparable to the level seen in 1998 (70 per cent). The proportion of girls who were a healthy weight in 2015 was 70 per cent, a level that has remained relatively steady since 1998. Just over one in four (28 per cent) children were at risk of being overweight in 2015, with no significant difference existing between boys and girls (26 per cent of boys and 29 per cent of girls). In 2015, 15 per cent of boys and 14 per cent of girls were at risk of obesity, figures which were identical to those in 1998. Compared with a child with parents of a healthy weight, a child with an obese parent was significantly more likely to be at risk of being overweight, including obesity (40 per cent compared with 22 per cent), or at risk of obesity (23 per cent compared with 11 per cent) [121] .
The Scottish Government's strategy, Preventing Overweight and Obesity in Scotland: A Route Map Towards Healthy Weight [122] , focuses on prevention. The Route Map sets out both national and local governments' respective long-term commitment to tackling overweight and obesity. It focuses on reducing energy consumption, increasing energy expenditure with a particular focus on those in early years and with people of a working age. Work continues to support a series of healthy weight interventions, including supporting adult and child healthy weight interventions in NHS Boards.
Football Fans In Training
Losing weight is difficult but keeping it off is even harder. Most people who lose weight are back at their original weight three to five years later. One promising programme in Scotland is Football Fans In Training ( FFIT), run by the Scottish Professional Football League ( SPFL) Trust. Developed by a Scottish research team led by the University of Glasgow, a randomised controlled trial in 2011/12 found that 12 months after starting FFIT, men who took part in the programme lost 5.56 kg, or 4.96 per cent of their baseline weight [123] .
The programme was also cost-effective. With funding from Scottish Government, the SPFL Trust has continued to deliver the programme in 32 football clubs across Scotland: now almost 3,000 men have taken part in FFIT [124] . The research team has now followed up the original participants in the trial to see if they managed to keep the weight they lost off three-and-a-half years after starting the programme. The research will be published in early 2017. Football Fans In Training is now internationally-recognised. It has been transferred to the English Leagues with clubs such as Southampton, Middlesbrough and Blackburn Rovers and lower league clubs such as Torquay actively involved. Work is also in place to start to transfer the programme to the German Bundesliga.
Supporting Wellbeing in Pregnancy and Parenthood in Young People
March 2016 saw the publication of the Pregnancy and Parenthood in Young People Strategy [125] . The strategy supports Scotland's young people and young parents, and aims to drive actions that will address the cycle of deprivation associated with pregnancy in young people aged under 18.
Whilst rates of pregnancy in young people have fallen in recent years, the gap in inequality is increasing. Young women aged under 20 living in Scotland's most deprived areas are five times more likely to experience a pregnancy as someone living in the least deprived. In order to address this gap in equality, the Strategy aims to increase the opportunities available to young people to support their wellbeing and prosperity across the life course. Multiple agencies have been tasked with working toward achieving the aims of the strategy, working together across NHSScotland, Local Authorities and the third sector with the support of a national lead.
Promoting Healthier Behaviours
NHSScotland has a key responsibility for promoting health and wellbeing in the population it serves, but it has recognised in recent years that it should also be seen as an organisation that values and promotes health among its workforce and those that engage with the service. This is being realised through the Health Promoting Health Service.
Health Promoting Health Service is about promoting healthier behaviours and discouraging detrimental ones in NHSScotland, and is aimed at staff and anyone visiting NHS premises in Scotland. It seeks to achieve this by ensuring that healthier choices are readily available and that appropriate support and encouragement is in place to help people make better choices. With its person-centred approach, Health Promoting Health Service goes further, seeking to connect people with sources of support for non-medical issues that may be impacting on their health - such as money worries and housing issues - so that those at risk of poverty and inequality achieve the best possible health outcomes.
Improvements in the hospital environment have been particularly evident over the last year, with healthier food choices on offer in staff canteens and visitor cafés, an increase in the number of sites with well-designed, usable green spaces for therapy and to encourage physical activity, and the ban on smoking in NHSScotland grounds.
NHS Boards achieved the Healthyliving Award Plus [126] in all 123 NHS-operated sites, with a further 60 in the third and private sector. The Healthyliving Award rewards caterers from across the length and breadth of Scotland for making it easier to eat healthily when eating out. Now retailers are required also to adopt healthier practice through the Healthcare Retail Standard [127] . Both sets of criteria are based on the general principles of a healthy balanced diet. They have been developed to reflect Scottish dietary targets, and so aim to ensure that healthier ingredients and cooking methods are used to keep fat, salt and sugar to a minimum, and options such as water, low-fat dairy products and fruit and vegetables are always available. NHS Boards are asked to ensure that all caterers (such as tea bars, restaurants and cafés) which sell food or drinks in healthcare premises work to maintain the Healthyliving Award Plus. To ensure a consistent approach among food service providers across NHSScotland, by 31 March 2017, 70 per cent of all food provision must meet Healthyliving criteria and have implemented the Healthcare Retail Standard.
Improving Oral Health
NHS Boards and their delivery of the Childsmile Programme have ensured that continued progress is made in improving the oral health of children. This is a crucial area, as dental decay is almost always entirely preventable, and by ensuring good oral health in children, we help safeguard the oral health of the future adult population. The latest results from the National Dental Inspection Programme ( NDIP) showed that 75 per cent of children in Scotland at Primary 7 had 'no obvious decay experience', compared with 59 per cent in 2007 [128] .
Despite the national success of the Childsmile Programme, health inequalities in oral health persist in Scotland. For example, 64 per cent of Primary 7 children in the most deprived areas have 'no obvious decay'; the equivalent figure for the least deprived areas is 85 per cent. This gap between least and most deprived needs to be further addressed and the Scottish Government's consultation on Scotland's Oral Health Plan is intended to achieve this [129] .
Protecting the Public Against Serious Diseases
After clean water, vaccines have had the greatest impact on people's health around the world. Vaccination programmes are one of the most effective ways of protecting the public against serious diseases and of reducing the spread of disease. Scotland has a number of well-established vaccination programmes for people across all ages and at various stages in their lives. Indeed, the Scottish routine childhood vaccination programme is one of the cornerstones of Scotland's efforts to protect public health, and the importance of this programme is clearly recognised by the public, as uptake rates in Scotland are enviably high. During 2015, two new meningitis vaccines were added to the routine childhood vaccination programme in order to help protect against particular strains of meningococcal disease (Men ACWY and Men B).
In August 2015, Scotland introduced an accelerated catch-up programme to vaccinate all 14-18 year olds with Men ACWY vaccine within one year to respond to an increase in cases of meningococcal group W (Men W) in the UK. The vaccine was also offered to students under the age of 25 attending university for the first time in autumn 2015. The Men ACWY vaccine now replaces the Men C vaccine given at around age 14 under the routine childhood vaccination schedule. While uptake figures for the Men ACWY catch up programme have not yet been published, it is almost certain that the uptake is likely to be very high, in line with other teenage booster vaccinations. Additionally, indications are that there has been a steady decline in cases of Men ACWY in the vaccinated age group, potentially suggesting early effectiveness of the programme.
In September 2015, Scotland became one of the first countries in the world to introduce a Men B vaccine. It is given alongside other routine immunisations at two and four months of age, with a booster dose at 12-13 months. Provisional vaccine uptake for the first routine cohort eligible for infant Men B vaccination is 95.7 per cent for one dose and 82.4 per cent for two doses by six months of age [130] . Such high uptake six months after introducing the vaccine demonstrates that the programme is working well and that inclusion of the Men B vaccine is acceptable to parents and guardians. Final uptake figures for Men B vaccination of children reaching 12 months of age between July to September 2016 will be published in December 2016. It is expected that the full impact of the Men B vaccine will become more apparent over time.