NHS Scotland Global Citizenship Doing It Well
The Guide provides advice and guidance for NHS Scotland Health Boards and staff about how to get involved in Global Citizenship at home and overseas. This includes guidance on risk assessments, safeguarding and building sustainable partnerships and relationships.
Section 2 – Getting Involved
Active Global Citizenship
Everyone can get involved in active global citizenship by making the connections between our day-to-day decisions at home and the potential impact these choices have on people who live in low- and middle-income countries. This awareness enables us, as individuals, to do what we can to promote social justice.
Case Study: Emily Broadis, Consultant in Public Health Medicine, NHS Ayrshire and Arran, Active Global Citizen
Living and working in Malawi opened my eyes to inequality, resourcefulness and living in the present, and the friendships I made mean that poverty is no longer faceless. I think for me, active global citizenship is the explicit recognition that the way I live, through consumer and lifestyle choices, work and volunteering, can make a difference to those who are disadvantaged, and it brings a hope that both peoples’ lives, and planetary health, can be made fairer and healthier.
Traditionally global health work, has been considered through the lens of overseas volunteering. However, staff from across the NHS contribute to global health in multiple and innovative ways including:
- mentoring healthcare staff from low- and middle-income countries who come to work in NHS Scotland to develop new skills and learning
- providing remote support including: virtual learning, clinical networks, coaching and mentoring using a wide range of technology from Scotland to staff in low- and middle-income countries
- providing additional cover and support when a team memberis volunteering overseas
- fundraising to support local and global initiatives
- voluntary work within Scotland to support refugees/asylum seekers
- supporting healthcare system development in a low- and middle-income country with skills, experience and tools in areas such as project management, financial management and quality improvement
For further information please see the Active Global Citizenship resources which includes thinking about our everyday choices and the impact these may have on others.
Environmental Sustainability, Climate Change and Global Health
One of the natural consequences of becoming a Global Citizen is being someone who makes an active contribution to local and global sustainability.
But what do we mean by ‘sustainability’, especially as it seems to mean different things to different people and organisations? Being sustainable simply means that things can be maintained at an agreed level or rate, usually of a given resource or resources. So, financial sustainability means that we are seeking to maintain the use of funding at an agreed level or rate, staffing sustainability means that we are training and recruiting the staff necessary to maintain services, and environmental sustainability means that we are using environmental resources in a way that maintains the integrity of our environment. When we consider global health, we are usually considering the ways in which we actively support the development of health and healthcare systems in a sustainable way.
Sustainable development has been described by the United Nations as:
“development that meets the needs of the present without compromising the ability of future generations to meet their own needs.”
Source: UN. The Sustainable Development Agenda
Linked to this overarching commitment are seventeen sustainable development goals (SDG) that make clear the actions that are necessary. When it comes to environmental sustainability and climate change in the context of global health, the necessary actions encompass:
SDG 12 Responsible consumption and production: ensure sustainable consumption and production patterns
SDG 13 Climate Action: take urgent action to combat climate change and its impacts
SDG 14 Life below water: conserve and sustainably use the oceans, seas and marine resources
SDG 15 Life on land: sustainably manage forests, combat the spread of deserts, halt and reverse land degradation, and halt biodiversity loss
For those involved in developing and delivering Scotland’s global health response, it can be hard to see how such goals can be delivered practically. Even in Scotland, they can seem very distant from what we are all doing on a day to day basis. But this is why being a Global Citizen is so important.
In Scotland we are fortunate that our national performance framework, which sets out how Scotland will make the SDGs locally relevant, has sustainability as one of the outcomes. This means that by supporting what the NHS is doing locally in relation to sustainability, you are becoming a Global Citizen in Scotland. But more importantly, by becoming aware of, and acting to take forward the NHS Scotland Sustainability Action programme locally, you will be developing the practical day to day skills that mean you will be practicing in a more sustainable way when working as part of a global health initiative.
To help you get started, your local NHS intranet should be able to guide you to your local Sustainability Action contacts.
Minimising the environmental effects of global health work
There can be a real conflict within global health partnerships between working towards improving the health of our populations, and contributing to the climate emergency by flying people across the world.
This topic is explored in more detail in our second eLearning module, Global Health Work: good quality, ethical and effective. The main recommendations from the discourse around the carbon footprint of partnerships are:
- avoid premium class travel: travelling in business class generates roughly three times the carbon of travelling in economy class, and in first class roughly four times. It is important to minimise the carbon generation of our global health travel (as climate change is disproportionately affecting low-and middle-income countries)
- prioritise telehealth and virtual education: clearly it’s better for the planet if we don’t need air travel at all. Many partnerships are now using a hybrid model where some teaching and other support is done remotely using the internet. This has been much easier since the Covid-19 pandemic
- avoid short trips: the carbon impact of an international trip is reduced (per day) as the trip gets longer. Therefore the recommendation is that longer visits and placements are better than short (less than around two weeks) ones
- develop partnerships closer to home: less air travel is better for the planet, and therefore developing partnerships closer to home will reduce the air miles. In addition, supporting South-South partnerships and addressing health inequalities in your own country or area is another way to minimise air travel
Reference: Can J Anaesth. 2023 Jan 20;70(3):327–334.
Building Collaborative Health Partnerships
Health partnerships are a model for improving health and health services based on ideas of co-development between people and institutions from different countries. The partnerships are long-term but not permanent and are based on ideas of reciprocal learning and mutual benefits.
Whether you decide to volunteer with a charity or as part of a health partnership, your input should be based on collaborative working and follow the principles of Global Health Partnerships (GHP) – Principles of Partnership.
Health partnerships take many forms; they can be an arrangement between friends, colleagues, organisations, charities or NHS Boards. However, fundamental to any partnership is that they have been developed collaboratively and are based on need.
NHS Scotland recommends that all NHS staff engaged in health partnerships embrace Global Health Partnerships’ Principles of Partnership. This can be done prior to establishing a partnership, or established partnerships can be reviewed regularly to check that these principles are embedded in everything that they do.
Global Health Partnerships’ Principles of Partnership:
1.Strategic: Health Partnerships have a shared vision, have long-term aims and measurable plans for achieving them and work within a jointly-agreed framework of priorities and direction.
2.Harmonised and Aligned: Health Partnerships’ work is consistent with local and national plans and complements the activities of other development partners.
3.Effective and Sustainable: Health Partnerships operate in a way that delivers high-quality projects that meet targets and achieves long term results.
4.Respectful and Reciprocal: Health Partnerships listen to one another and plan, implement and learn together.
5.Organised and Accountable: Health Partnerships are well-structured, well-managed and efficient and have clear and transparent decision making processes.
6.Responsible: Health Partnerships conduct their activities with integrity and cultivate trust in their interactions with stakeholders.
7.Flexible, Resourceful & Innovative: Health Partnerships proactively adapt and respond to altered circumstances and embrace change.
8.Committed to joint learning: Health Partnerships monitor, evaluate and reflect on their activities and results, articulate lessons learned and share knowledge with others.
9.Embed equity and inclusion: Health Partnerships consider unequal power relations and inequalities experienced by individuals as a result of their social identities and take action to ensure equity and inclusion are embedded in their work.
10.Committed to Climate Action: Health Partnerships proactively contribute to climate change adaptation and mitigation.
Source: GHP’s Principles of Partnership
Case Study: Niall Campbell, Consultant Liaison Psychiatrist, NHS Borders reflects on the NHS Borders Health Partnership with St Francis Hospital, Katete, Zambia
As Chairman of Logie Legacy, I visited St Francis Hospital in Katete, Zambia, to review our ongoing work there. As a Psychiatrist and a GP, I was interested in the interplay between physical and mental health. I witnessed first-hand the scale of unmet mental health need, limited access to treatment, and the wider challenges of inequality, rising gender-based violence, and teenage pregnancies, and continued stigma around mental health. These pressures place significant strain on already limited health services. One of our aims is to enable mental health care not just within hospital but bringing it into communities reiterating the message ‘no health without mental health’.
Our partnership with St Francis Hospital has demonstrated the value of true bidirectional learning, with shared ideas, mutual support, and renewed motivation for UK staff who have felt demoralised or demotivated. The engagement with Zambia has brought a renewed sense of purpose and perspective for staff, which has included staff from catering, admin and clinical staff. The collaboration reinforces how global partnerships strengthen both local care and professional development.
This visit reinforced key lessons: mental health remains under-resourced globally, health is shaped by social determinants, and long-term global partnerships deliver meaningful, shared impact for patients, staff, and systems alike. There is strength in partnership and we continue to make a difference.
Brave Muleya, Clinical Officer in Psychiatry at St Francis Hospital, reflects on the partnership’s impact: “The support we receive from Logie Legacy allows us to feel confident in seeing and treating the most vulnerable patients in our community. The partnership has allowed mental health to be visible, and has broken down barriers to access and reduced stigma. It means so much to us.”
Engaging with a Health Partnership
If you are looking to get involved in global citizenship, as a first step, you can get in touch with your NHS Board’s Global Citizenship Lead Champion who will endeavour to guide you to further information and local staff involved in global health work. This can be helpful in thinking about the different ways you could contribute and also if there are any opportunities locally to get involved in your Board (to find out who your Lead Champion is, email ScottishGHCU@gov.scot).
You can also search the Health Partnership Map which will give you an idea of the different health partnerships that are underway and an idea of what is involved and how your skills and interests could contribute. Many of the partnerships on our website also have links to their own websites and publications which can also help you to familiarise yourself with their work.
If a local partnership is involved in work outside of your field, it can still be worth having a conversation with the partnership leads. Many partnerships evolve as a result of local interest and expertise as well as the needs expressed by host organisations.
Health Partnership Toolkits
Global Health Partnerships has several excellent resources that could help you as an individual in setting up governance arrangements for your new partnership:
- Principles of Partnership
- International Health Links Manual
- Example Memorandum of Understanding
- Students in Partnerships
- Duty of Care Guidance for health partnerships also includes advice on insurance, indemnity and visas etc.
Health Partnership Programme
In July 2025, reflecting its ongoing commitment to global health equity, the Scottish Government launched its flagship new Health Partnership Programme, funded from the Scottish Government International Development Fund. This programme builds on Scotland’s 20-year legacy of international development, drawing on the Scottish Government’s strengths in health and education and deep-rooted relationships with partner countries to drive equitable, sustainable improvements in healthcare.
Always aligned with, and building on the success of the NHS Scotland Global Citizenship Programme, this Scottish Government initiative will, through partnership working:
- support health partnerships between health institutions in Scotland, Malawi, Rwanda and Zambia – promoting bidirectional learning, mutual benefit and the exchange of skills and knowledge
- mobilise the power of international collaboration to strengthen health systems across Malawi, Rwanda, Zambia and Scotland
- provide opportunities for healthcare professionals to share skills, experience and knowledge across borders — improving health for all
Global Health Partnerships were appointed in 2025 as Fund Managers for the first phase of this new Programme, taking forward funding calls for proposals and managing the grants, working closely with the Scottish Government international development team. More information to be found on this webpage: Introducing the Scottish Government Health Partnership Programme (SGHPP) – Global Health Partnerships.
Measuring the effectiveness of what you are doing
Working out what you will have achieved in what you do is really important. Have I ‘made a difference’? Before you start, think about how you could measure what you do and have some plans in place beforehand. This should be kept very simple – large evaluations of programmes have their place but they are difficult to do and expensive.
If you are teaching, for example, could you use ‘process measures’? Getting formal feedback on your teaching and assessing knowledge change before and after are easy to do. Assessing changes in practice (for better or worse) in the group you are working with is something that will allow you to further develop or to modify what you are doing. Online questionnaires such as Survey Monkey can be really helpful – but you need to really encourage people to complete them.
Think about how the work you do could be replicated over a longer period. Keeping any good intervention going over a period time or repeating it on a regular basis is bound to be more effective than something that is one-off.
Helpful Tips
- explore the current local data which is owned by the Ministry of Health in the partner country and ask questions about: what data is collected (patients/services/procedures/outcomes)? Who collects the data? How is it stored and used?
- consider the monitoring and evaluation plan prior to setting up the project or partnership. Can data which is already being collected contribute to this? Will your hosts be able to use currently collected data to evaluate this project? Try to avoid establishing parallel data capturing methods but rather consider how this project might strengthen current strategies in place
- if appropriate, consider offering support to build professional capabilityin the field of data capture
Quality Improvement Zone
In planning the sustainability of the health partnership you are involved in, the Quality Improvement Zone provides information and resources to support people with experience at all levels of quality improvement to develop their knowledge.
In the QI Zone you will find:
- information on what is quality improvement, the improvement journey and related quality improvement tools and topics
- a range of educational resources, including eLearning modules, guides and frameworks
- information on the different levels of experience in quality improvement and associated learning programmes
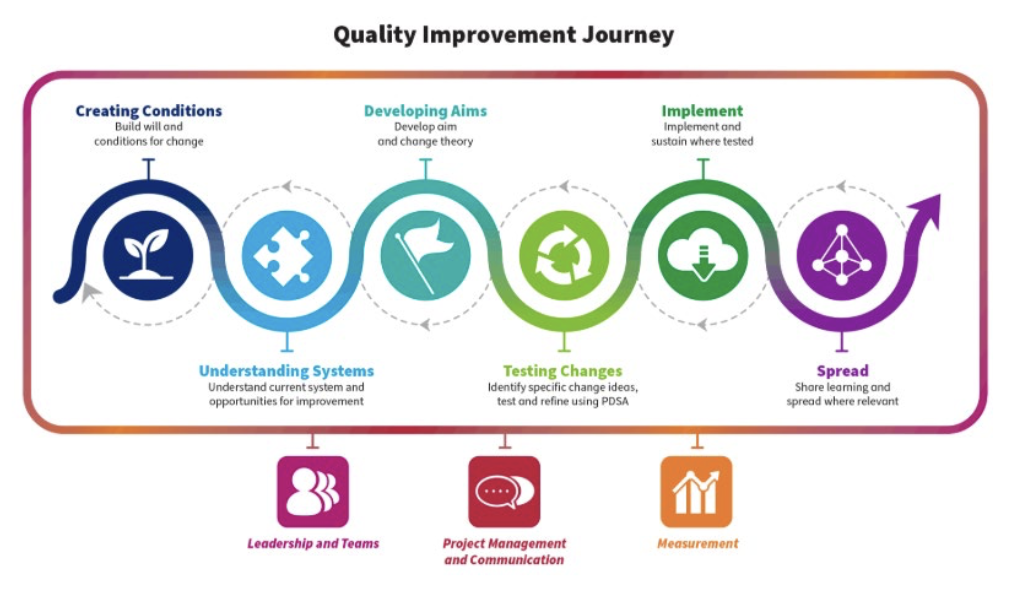
Quality Improvement Journey
Creating Conditions: build will and conditions for change
Understanding Systems: understand current systems and opportunities for improvement
Developing Aims: develop aim and change theory
Testing Changes: identify specific change ideas, test and refine using PDSA (Plan, Do, Study, Act)
Implement: implement and sustain where tested
Spread: Share learning and spread where relevant
There are three overarching themes you need to think about throughout the quality improvement Journey. They are leadership and teams; project management and communication; and measurement.
Knowledge and Evidence
Encouraging evidence-based practice is a key part of quality improvement. HINARI is a global initiative which provides access to high quality, up-to-date health research evidence and decision-ready evidence summaries for use at point of care. These are free of charge to local and not-for-profit institutions in low- and middle-income countries. Training materials are available at research4life.
Volunteering with a Charity
Another way to volunteer overseas is to go with a charity. There is a list of organisations which provide volunteering opportunities on our . The Scottish Global Health Co-ordination Unit is not specifically recommending these organisations but rather providing you with a starting point to begin to explore the different opportunities that might be of interest to you.
If you are interested in volunteering with a charity or an organisation, we suggest that you research the organisation, the work and country that they are working in, and whether they have processes and support in place for collaborative partnership working, and ethical volunteering, including Safeguarding and Conduct.
If you choose to volunteer with a charity or organisation – here are some questions that you should consider:
- what is the vision of the organisation?
- is the work community led, i.e. based on the needs of the community?
- do the organisation’s values resonate with your own?
- is the organisation’s vision based on social justice or charity?
- how is the organisation funded and is this transparent?
- is there a safeguarding policy and is training available?
- who has overall accountability for the project?
Medical Equipment and Other Donations
If you are working as part of a health partnership, your host partners may identify medical devices and equipment that are needed. Medical equipment has become a fundamental part of modern healthcare delivery giving health professionals throughout low- and middle-income countries the tools they need to deliver quality care, enabling screening, prevention, diagnostics, treatment and palliative care.
Although most donations are made with good intentions, the donation of medical equipment is complex and dealing with donated goods comes with risks and difficulties to both the donor and the recipient. If poorly executed, donations can burden the recipient, wasting an enormous amount of money, human resources and time, with long term implications of crippled healthcare systems and amassing environmental burden, for example, the WHO estimates that up to 70% of donated equipment is non-operational.
The following main barriers to effective donations of medical equipment have been identified:
- lack of collaboration and understanding between donors and recipients
- poor alignment with local needs and infrastructure, including power supply and available consumables
- limited support for long-term use, such as training, maintenance, and integration
- inadequate documentation and language accessibility for equipment use and servicing
- weak coordination and accountability, with no tracking or impact assessment
If you or your partnership is considering donating equipment, follow the 10 Step Guide which has been designed to support you and your partner through the important considerations to making a safe and effective donation. There is also a checklist to support you to work through the Guide. Although the Guide focuses on the donation of medical equipment, the key messages are also applicable to other types of donated equipment, e.g. consumables, rehabilitation and therapeutic equipment.
The Scottish Global Health website signposts a range of good practice resources to help evaluate whether or not to donate and how to do so effectively from start to installation to ongoing support. There is a section in the eLearning module – Global Health Work – that covers safe medical equipment donations. To access it, sign up for a Turas account.
Do you know about Warp-it?
NHS Bodies and Charities can register for Warp-it where they can search for public sector bodies and connect with them to share unneeded resources, information and promotional tools, e.g. posters which you can use.
Humanitarian Support
For information on giving humanitarian aid in a crisis please see the Ready Scotland website.
Books and journals
Donations of books and journals should be carefully considered. Healthcare knowledge changes rapidly and needs to be appropriate to the context where it will be used.
Some key principles in selecting materials to send are:
- resources should be up to date – outdated information is often irrelevant and can be harmful. For books, 10 years is usually a maximum cut-off point, and for many aspects of healthcare the pace of change means that five years is more realistic
- resources should be relevant to the priorities and the context where they are to be used. Resources based on processes, systems and devices used principally in high-income countries are less likely to be useful in low- and middle-income countries
- digital access – printed journals date rapidly and are largely replaced now by digital access through resources such as HINARI – available free of charge to local, and not-for-profit institutions in low- and middle-income countries
- logistics – consider transportation methods, associated costs and assurance that resources will reach their intended destination
Contact
Email: ScottishGHCU@gov.scot