Neurological care and support: framework for action 2020-2025
The framework sets out a vision for driving improvement in the care and support for those with neurological conditions in Scotland.
Early Priorities until March 2021
The following priorities will be targeted until 2021 and by achieving these, we will have put in place the infrastructure required to support delivery of the commitments over the remaining period of this five-year Framework. We are also developing an implementation Plan with stakeholders that will
set out detailed actions against each commitment.
This Framework operates within the context of key Scottish Government strategies such as the National Clinical Strategy [39], Realistic Medicine
and Health and Social Care Delivery[40]. Neurology is also included as a targeted specialty within the Scottish Access Collaborative Programme, Modernising Patient Pathways Programme and the Waiting Times Improvement Plan[41].
Successful delivery of this framework will be dependent on leadership. A foundation of person centeredness, working across boundaries and
in co-production with the Neurological Community.
An early priority is the creation of clear leadership and governance arrangements that will be achieved by:
- agreement between Scottish Government Directorates about the ownership and input to specific framework commitments;
- continuing with the review of membership for the National Advisory Committee for Neurological Conditions to ensure there is relevant expert oversight; and
- investing in regional and local networks including a national network of Regional and Local Implementation Leads working across Integration Authorities, NHS and the third sector to support delivery of this framework and implementation across Scotland.
Feedback provided to us throughout development of this Framework has highlighted the disconnect experienced by people with neurological conditions when there are unnecessary boundaries and barriers between sectors.
A key priority will be to develop relationships that enable organisations to co-design care and support through cross organisational approaches and that are co-produced with people with lived experience of neurological conditions.
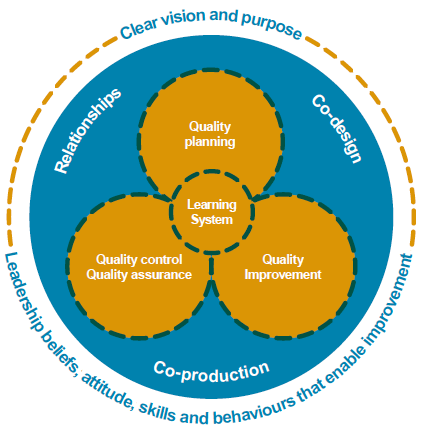
To ensure that implementation and improvement actions and support are informed by the elements that form part of effective quality management systems – specifically quality planning, control, assurance and improvement that is linked to leadership, learning systems and processes that promote collaboration with staff and people involved with services.
Early Priorities by Aims
Aim A: We will ensure people and their carers are partners in their care and support by:
- Facilitating engagement events to involve the neurological community in co-production of the implementation Plan.
- Promoting organisations/systems that can enable this aim including Self Directed Support (SDS) advocacy, A Local Information System for Scotland (ALISS), Care Information Scotland and contactSCOTLAND (the video relay service for people with a sensory impairment).
- Supporting a review of neurological condition content on NHS Inform.
- Identifying areas of best practice supporting personalised models of care including Self-Management Projects.
Aim B: We will improve the provision of co-ordinated health and social care by:
- Embedding support for the Framework with COSLA, local and national organisations and Integration Authorities.
- Exploring opportunities through the new GP contract (community treatment and care) to design community based multi-disciplinary teams that can support GPs (as expert medical generalists) to focus on complex health needs.
- Working with Integration Authorities and NHS Boards to encourage them to develop a specific plan within the suite of plans underpinning their strategic plan that demonstrates how care and support will be provided for those with specific complex care needs including neurological conditions.
- Inviting proposals from across Integration Authorities, NHS Boards and third sector organisations to test innovative projects.
- Exploring the potential of national care frameworks to provide signposts to neurological care and support.
- Improving the use of advancing technologies in health and social care services, including shared records, person-held records or other initiatives to improve communication.
- Mapping innovative projects planned or underway across all sectors in Scotland to test new models of care and support for neurological conditions, and their outcomes – to identify gaps and identify opportunities for shared learning.
- Working with Healthcare Improvement Scotland’s Improvement Hub to review neurological rehabilitation care and support across Scotland, identifying needs gaps and unwarranted variation, aspects of good practice and integrated models of care.
- Identifying and learning from transition models of care within neurology and other relevant areas that are best practice and those supported by Principles of Good Transition.
- Working with the Disabled Children and Young People Advisory Group to look at possible areas of good practice and support with implementation
- Understanding systematic approaches to mental health including collaborative relationships of neurology, psychiatry, neuropsychology and community models of care and identifying gaps in provision.
- Exploring mechanisms to support alignment of this Framework with coexisting strategies and models of care, such as those for stroke, dementia, learning disabilities, mental health and Augmentative and Alternative Communication (AAC). To build on complimentary issues, commonality in priorities or areas of improvement; to identify gaps and enable best practice and maximise implementation actions and outcomes.
- Linking in with other key emerging areas of activity such as Brain Health Scotland to support the implementation of personalised prevention plans and produce specific knowledge and understandings amongst targeted groups.
Aim C: We will ensure high standards of effective, person-centred and safe care and support by:
- Exploring the feasibility of developing a national reporting framework with HIS that includes key performance indicators to measure improvements in care and support, effective measures of experience and outcome of person-centred care and support.
- Partnering with HIS to support organisations to conduct regular, open and honest self-evaluation using the Quality Framework and associated organisational self-evaluation tools and ensure that outputs are aligned through collaborative working and diligent information sharing that feeds into the wider neurological agenda.
- Developing our population data with ISD through publication of the Scottish Burden of Disease statistics in 2020.
Aim D: Ensure equitable and timely access to health and social care and support across Scotland by:
- Identifying key priorities from Scottish Access Collaborative and Healthcare Improvement Scotland neurological streams and support
their development through alignment with this Framework. - Encourage NHS Boards and Integration Authorities to consider introducing/strengthening current provision for commonly accessed services including: open access clinics and rapid access clinics.
- Identify what outcome measurements are currently reported and support development of tools to measure impact of models of care.
- Producing an Atlas of Variation proposal to create maps with a narrative to identify and tackle unwarranted variation to support improvement in outcomes.
Aim E: Build a sustainable neurological workforce for the future by:
- Establishing immediate, medium and long term priorities and the reasons for gaps in services and shortfalls where they exist.
- Identifying opportunities to improve recruitment into hard to fill posts including medical, clinical and support posts in neurology, neurophysiology, neuroradiology and neuro-rehabilitation.
- Examining the value of potential roles played by nurses, allied health professionals, general neurology keyworkers and healthcare scientists. As this work matures, we will use findings to refine workforce planning across neurological specialists and the wider health and social care workforce involved in delivering neurological services.
- Developing a longer term approach to workforce planning, consistent with the approach set out in the national Integrated Workforce Plan to be published later this year, that considers the range and complexity of medical, clinical and support roles involved in providing high quality neurological services.
Contact
Email: Clinical_Priorities@gov.scot