Neurological care and support: framework for action 2020-2025
The framework sets out a vision for driving improvement in the care and support for those with neurological conditions in Scotland.
Introduction
13. We have set out high level priorities until March 2021, and we are developing a five-year implementation plan with key delivery partners such as Scottish Government directorates, Integration Authorities, NHS Boards, the third sector and other organisations.
14. The Scottish Government aims to help people sustain and improve their health, independence and wellbeing.[19]
15. In 2003, it was estimated that there were about one million people in Scotland living with a neurological condition, of whom at least 10% were disabled as a result[20]. Neurological conditions account for between 10% and 20% of acute medical admissions[21] and 10% of the overall burden of disease in Scotland, as measured by disability-adjusted life years[22]. This Framework and commitments are not condition specific. We have maintained a broad view of neurological conditions, in recognition that it is unrealistic to list every condition in which neurological symptoms might be expressed.
What are neurological conditions?
16. We use ‘neurological conditions’ to include a wide range of conditions, disorders and syndromes affecting the brain, spinal cord, nerves and muscles. The Scottish Government recognises the World Health Organisation’s (WHO) definition of neurological conditions[23] (Annex B). However, while the WHO definition provides examples of conditions – this framework is not limited to those specifically mentioned and is also intended to cover the population of people who have rare, complex or uncertain neurological conditions not referred to, as well as diagnoses contained within ICD-10 classification Chapter VI[24]. In addition, although not explicit within the WHO definition, we acknowledge that Functional Neurological Disorders (FND) are common, disabling, poorly understood[25] and included within our definition of neurological conditions.
17. Neurological conditions range from the common to the very rare, and are caused by a range of diverse pathologies. These may be congenital, hereditary/genetic, neoplastic, degenerative or infective, however, the cause of many conditions remains uncertain.
Impact of neurological conditions
18. Neurological conditions may occur as an abrupt ‘one off’ event with life changing consequences, or they may evolve over many years, either in a relapsing remitting manner or in a relentlessly progressive way. Some neurological conditions are more readily identified and defined than others, and some generic headings mask enormous variation in how symptoms affect people’s lives.
19. We know that the diagnosis of a neurological condition is life changing and, for some, can affect the person’s ability to live independently, achieve personal ambitions, sustain their personal identity or life roles, work, or drive. For others, their condition may affect their ability to communicate, walk, think, swallow or breathe and may result in premature death.
20. Diagnosis of a neurological condition can have a range of mental health impacts, from emotional wellbeing to requiring specialist psychological and psychiatric support. In supporting someone to live with a neurological condition, it is important that a holistic approach is taken to understand and respond to their individual needs, including their mental health. Timely access to psychological and psychiatric assessment, treatment and support for individuals with neurological conditions, where needed, is an important part of the care pathway given the link between neurological conditions, mental health and quality of life.
Approach
21. During consultation, people told us that they want to be able to live well and play a key role in making decisions about their care and support. People asked for appropriate advice and support for them and their carers so that they could do this on their own terms. Some people feel treatment is ‘done to them’ rather than being partners in their care.
22. This requires support, both for health and social care professionals and individuals, to be able to shift the balance of power to a more equal relationship, enhance communication and improve how care and support are delivered and developed.
23. In order to facilitate better conversations between people and their health and social care professionals, we must create the conditions that help people make informed choices and express their views about their treatment and care options, based on what matters most to them. The shared vision for Scotland is that:
‘By 2025, everyone who provides healthcare in Scotland will demonstrate their professionalism through the approaches, behaviours and attitudes of Realistic Medicine.[26]’
Dr Catherine Calderwood,
Chief Medical Officer for Scotland
24. Realistic medicine means:
- listening to and understanding people’s problems and preferences;
- sharing decisions between people and health and social care professionals;
- ensuring that people have all the information they need to make an informed choice;
- moving away from the ‘doctor knows best’ culture to ensure a more equal partnership with people;
- supporting health and social care professionals to be innovative, to pursue continuous quality improvement and to manage risk better;
- reducing the harm and waste caused by both over-provision and under-provision of care; and
- identifying and tackling unwarranted variation in clinical practice.
25. Legislation mandating full involvement in decision-making is already in place within social care through the Social Care (Self-directed Support) (Scotland) Act 2013[27]. Under this legislation, people are supported to decide what matters to them (their personal outcomes), how their social care support is delivered and by whom within the available budget. The Scottish Government funds independent support and advice for people navigating social care through Support in the Right Direction funding.
26. We recognise that many people do not need, or want access to hospital based care and support. The actions detailed later in this Framework are considered to be based on a pyramid of support (Figure 1), which defines levels of support and care dependent on the needs and choices of the individual.
Figure 1.
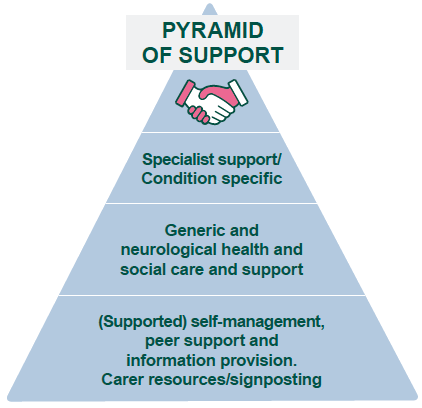
27. In the first (largest) tier of the pyramid, people living with neurological conditions are self-managing their condition effectively within their communities, accessing resources to promote self-management.
28. In the second tier, people have a need for generic as well as neurological care and support that covers all neurological conditions delivered within the local community (e.g. paid care workers from the local authority or a social care provider, personal assistants, social workers, speech, occupational or physiotherapy).
29. In the smallest tier are people who require specialist, often condition specific support, available locally but also frequently regionally or nationally. Such individuals may require complex, highly tailored packages of care and support.
30. People may move between these tiers, or access all tiers at the same time, depending on their needs and may at times be out with services. Social care delivered in any tier will be accessed through self-directed support, Scotland’s mainstream approach to social care. This ensures that support is personalised, and allows people to take control of their support.
A: Ensure people with neurological conditions are partners in their care and support
31. People told us they wanted to focus on personal outcomes and to be partners in their care and support. Some people gave good examples of personalised care from clinical nurse specialists, therapists and their GP. Others found helpful information and support from charities, online or described receiving excellent support from paid care workers.
32. Data from the Lived Experience Project and consultation responses showed that while some feel listened to, others perceived a lack of understanding on the part of clinicians, practitioners and other staff. People described there is a lack of understanding of their condition (in some cases reporting a perception that their symptoms were not believed), a lack of information on what care and support is available, and a lack of consideration of what matters most to them.
33. Improving communication between people and health and social care professionals is a priority for the Scottish Government. We are working to spread the What Matters to You?[28] approach. This encourages staff to focus on what is important to the people they are caring for and supporting. It is based on the principle that by talking to people about what is important to them, listening to the answers and taking action on what we hear, we can provide the care and support that people really need and want. Our ambition is that conversations about what matters becomes a core part of how health and care services are delivered across Scotland, every day. Where a person has lost their voice or has difficulty speaking, the legislative duty to provide or secure communication equipment and support in using that equipment will ensure those needs are met.
34. To facilitate this approach we have developed Making it Easier – Scotland’s Health Literacy Action Plan[29] to improve health literacy. This aims to ensure we all have the skills, confidence, knowledge and understanding to navigate complex health and social care systems. We have also recently revised the Charter of Patients’ Rights and Responsibilities[30] to ensure people know what they are entitled to when using NHS services and receive NHS care in Scotland.
Commitment 1
We will support shared decision making and personalised models of care and support, including access to supported self-management where appropriate.
Commitment 2
We will work with stakeholders to raise awareness of the information and resources available on neurological conditions.
35. People told us that staff were sometimes reluctant to share information with families and carers, and that their carers were not given the information or help they needed. People and their carers asked for training in using equipment and carrying out technical interventions. We understand for non-NHS employees there are considerations about responsibility and potential liability relating to the training of equipment use and interventions, with the need for appropriate governance arrangements to ensure safety.
36. We acknowledge the key role of unpaid carers and the need to support their health and wellbeing. In particular:
- All carers have the right to a personalised plan to identify what is important to them.
- Carers have the right to support to meet their own needs. For example, this may include training in specific techniques to help the person they look after. Local authorities must consider whether support should include a break from caring.
- Every area must have a local carer strategy and an information and advice service for carers.
- Carers also have the right to be involved in assessing the needs of the cared-for person and in decisions about discharging the cared-for person from hospital.
Commitment 3
We will work with the third sector and carer organisations to help ensure:
- Carers of people with neurological conditions are aware of their rights under the Carers Act[31]; and
- Local carer information and advice services know how to access the most relevant information and training for carers of people with neurological conditions.
Early Priorities for Aim A
We will ensure people and their carers are partners in their care and support by:
- Facilitating engagement events to involve the neurological community in co-production of the implementation Plan.
- Promoting organisations/systems that can enable this aim including Self Directed Support (SDS) advocacy, A Local Information System for Scotland (ALISS), Care Information Scotland and contactSCOTLAND (the video relay service for people with a sensory impairment).
- Supporting a review of neurological condition content on NHS Inform.
- Identifying areas of best practice supporting personalised models of care including Self-Management Projects.
B: Improve the provision of co-ordinated health and social care and support for people with neurological conditions
37. We know that the current model of primary, secondary and tertiary care works for many people living with neurological conditions.
38. For some, however the current structure creates barriers to accessing care and support when and where they need it. Whether due to a lack of awareness about some conditions, lack of access to appropriate services, lengthy waiting times, the need to travel long distances, the nature of their condition, or differences between referral and prioritisation criteria for housing adaptations, respite care, and provision of specialist, personalised equipment.
Commitment 4
We will ensure that the legislation, policy and guidance that Integration Authorities and the NHS use when planning and commissioning services
are designed to support consistent, timely and appropriate provision of care and support for people with neurological conditions.
39. We recognise that transition periods in the provision of care and support such as when young people move into adult care, adults move from their own home to residential or nursing care or become users of care and support for older people, are times of increased risk.
40. Through the Lived Experience project and the national engagement events, we heard that some people experienced a lack of ‘joined up’ care. People described a lack of co-ordination between teams, and disjointed care between care providers, statutory, third and independent sectors. There was a clear message that we should improve communication amongst care and support professionals and between professionals and others.
41. Getting it right for every child (GIRFEC)[32] already exists to support families with making sure children and young people receive the right help, at the right time, from the right people. The Children and Young People Scotland Act (2014)[33] is also relevant as it too supports improved planning, co-ordination and delivery of personalised care that is rights based and takes account of people’s experiences and choices. The feedback from young adults with neurological conditions, and their families, focused on the difficulties experienced when moving/transitioning from care and support
for children and young people to that for adults. We also heard examples of less frequent review appointments, lack of access to therapy,
and the need to establish relationships with a new care team.
Commitment 5
We will work with key partners across sectors, to embed the Principles of Good Transitions[34], as a good practice framework for transitions for people living with neurological conditions.
42. Our Framework for Action on Palliative and End of Life Care, already sets out our aim that by 2021 everyone in Scotland who needs palliative care will have access to it. To achieve this aim it is essential we create the right conditions nationally to support local communities in their planning and delivery of palliative and end of life care services and supports.
43. More generally, people have expressed concerns about moving into a suitable care home, as residential care for people with a complex neurological condition may not always be available locally. In these and other cases many people might benefit from the approach adopted for palliative care across health, social care and community settings that would be more responsive to the changing preferences and priorities of people living with advanced neurological illnesses and those of their families.
Commitment 6
We will continue working together with others to deliver a national programme to support local reform of adult social care support. The full implementation of self-directed support is integral to the programme for adult social care reform.
44. We also heard about the need to share information between members of care teams, and the importance of anticipatory care plans for some people with neurological conditions. A national programme delivered by Healthcare Improvement Scotland supported the implementation of anticipatory care planning and the development of supporting infrastructure concluded in June 2018. An anticipatory care planning approach is now spread through a range of programmes delivered by Healthcare Improvement Scotland’s ihub.
Commitment 7
We will work with Healthcare Improvement Scotland, Integration Authorities and the NHS to promote the implementation of anticipatory care planning, to ensure these plans are widely available and adopted by the services and people with neurological conditions.
45. We recognise the need to harness digital technology as a means of improving communication and overall care for people with neurological conditions. This ranges from better use of technology for care and support, to improving the availability of information for people with neurological conditions, their families and carers. There has been significant progress in the development and roll-out of innovative approaches to video-appointment and out-patient booking systems that allow people to book an appointment at a time that suits them. We want to encourage the extension of these approaches for people with neurological conditions.
Commitment 8
We will work to improve the use of digital technology to ensure that integrated services seamlessly meet the needs of people with neurological conditions and those who provide care and support to them.
46. Many people with neurological conditions experience deterioration in their condition over time. There is a need for a more proactive approach to offering information, care, support and rehabilitation that enables them to maintain their independence, health and wellbeing. There is also a need to develop and test different community based neurological rehabilitation models, that can proactively provide care and support to people with a wide range of neurological conditions. Models may include generic neurology keyworkers, as well as clinicians, social workers and practitioners with advanced skills, and would need to be tested in both rural and urban settings.
47. We value the role of third and independent sectors as key partners in developing, delivering and trialling new care and providing ongoing support and look to actively create a sustainable environment for this, particularly in areas where these organisations may be best placed to deliver.
48. Some neurological symptoms (e.g. headache, tingling hands/feet, dizziness) are extremely common and rarely caused by serious underlying disease. Yet they cause concern and anxiety for people and their clinicians, and represent a significant proportion of primary to secondary care referrals, either routinely or urgently. It is questionable whether this is the best way to support people with these symptoms, and so we propose to test projects that assess and support people with common neurological symptoms.
Commitment 9
We will support Integration Authorities and the NHS to improve services and support, with a commitment to evaluate and test generic/neurology community based multi-disciplinary team models and to test innovative ways of delivering health and social care, including new roles and new arrangements for co-ordinating care and support for people with neurological conditions.
49. There is potential to explore whether existing community based models of care and support such as those used in some specialist neurological services, acquired brain injury, stroke and dementia could be enhanced and extended to those with other neurological conditions.
Commitment 10
We will work with the Neurological Alliance of Scotland and other stakeholders to explore the potential of national care frameworks and how these can inform neurological care and support.
Early Priorities for Aim B
We will improve the provision of co-ordinated health and social care by:
- Embedding support for the Framework with COSLA, local and national organisations and Integration Authorities.
- Exploring opportunities through the new GP contract (community treatment and care) to design community based multi-disciplinary teams that can support GPs (as expert medical generalists) to focus on complex health needs.
- Working with Integration Authorities and NHS Boards to encourage them to develop a specific plan within the suite of plans underpinning their strategic plan that demonstrates how care and support will be provided for those with specific complex care needs including neurological conditions.
- Inviting proposals from across Integration Authorities, NHS Boards and third sector organisations to test innovative projects.
- Exploring the potential of national care frameworks to provide signposts to neurological care and support.
- Improving the use of advancing technologies in health and social care services, including shared records, person-held records or other initiatives to improve communication.
- Mapping innovative projects planned or underway across all sectors in Scotland to test new models of care and support for neurological conditions, and their outcomes – to identify gaps and identify opportunities for shared learning.
- Working with Healthcare Improvement Scotland’s Improvement Hub to review neurological rehabilitation care and support across Scotland, identifying needs gaps and unwarranted variation, aspects of good practice and integrated models of care.
- Identifying and learning from transition models of care within neurology and other relevant areas that are good practice and those supported by Principles of Good Transition.
- Working with the Disabled Children and Young People Advisory Group to look at possible areas of good practice and support with implementation
- Understanding systematic approaches to mental health including collaborative relationships of neurology, psychiatry, neuropsychology and community models of care and identifying gaps in provision.
- Exploring mechanisms to support alignment of this Framework with coexisting strategies and models of care, such as those for stroke, dementia, learning disabilities, mental health and Augmentative and Alternative Communication (AAC). To build on complimentary issues, commonality in priorities or areas of improvement; to identify gaps and enable good practice and maximise implementation actions and outcomes.
- Linking in with other key emerging areas of activity such as Brain Health Scotland to support the implementation of personalised prevention plans and produce specific knowledge and understanding amongst targeted groups.
C: Ensure high standards of effective, person-centred, and safe care and support
50. Scotland’s Health and Social Care Standards[35] set out what everyone can expect when using health, social care or social work services in Scotland. The standards seek to provide better outcomes for everyone, and we have developed our approach in accordance with the principles of Dignity and Respect, Compassion, Inclusion, Responsive Care and Support, and Wellbeing.
51. We have worked closely with Healthcare Improvement Scotland on the revision of its General Standards of Neurological Care and Support 2019[36], with a shared ethos to bring the greatest benefit to all people living with neurological conditions.
52. These neurological standards complement the Health and Social Care Standards by articulating what people with neurological conditions should expect to receive in terms of high quality care from the health and social care organisations that support them, regardless of their condition, geographical location or individual circumstances. Organisations will use the standards to demonstrate that they are delivering high quality care and support.
53. As neurological conditions affect everyone in different ways, and also cause differences over time, it is difficult to find a way of measuring what type of treatment, care and support works best. We know the use of meaningful outcome measures is paramount to everyone so that they can decide what treatment, care and support will work best for them. The choice of measures for monitoring the outcomes of the implementation of the neurological standards is similarly complex.
Commitment 11
We will promote and support the implementation of the Health and Social Care Standards 2018 and Healthcare Improvement Scotland General Standards for Neurological Care and Support 2019.
54. The Scottish Burden of Disease project ranked neurological conditions as fifth in terms of years lost owing to early death or living in less than ideal health (disability-adjusted life years, DALYs), representing 10% of the overall DALY score in Scotland.
55. We have a series of prevalence estimates for some (but not all) conditions, some more accurate than others; we do not underestimate the challenge we face regarding basic epidemiological data. More consistent and comprehensive recording of neurological conditions in people’s health and care records would help ensure that they were visible to appropriate services. It would also support more accurate population-level prevalence estimates and other data analysis to inform service planning and development.
56. The development of linked data to support Integration Authorities is a key focus for NHS Information Services Division. Improved data collection will enable better understanding of people’s access to care and support. This will inform future planning based on need, and provide a way of measuring performance and outcomes.
Commitment 12
We will work with NHS Information Services Division and others to ensure a cohesive approach to capturing the needs of people with a neurological condition that will:
- improve the recording of neurological conditions in people’s routine health and care records, so that they are visible to appropriate services;
- enable more accurate population-level estimates of the prevalence of neurological conditions to inform other data analysis; and
- support the development of systems and processes for service planning and workforce development, based on these improved prevalence estimates.
57. Health and social care and support needs to be effective. Ensuring effectiveness implies a willingness to learn from user feedback and service reviews, participation in development and improvement activities, a willingness to consider new paradigms, and apply new findings from research. Scotland has a proud history of research, and we wish to encourage ongoing research within the Neurological Community, alongside other development and improvement activities.
Commitment 13
We will support the neurological research agenda by:
- promoting the work of the Chief Scientist Office, third sector organisations’ research and Scottish neurological research networks;
- encouraging opportunities for people with neurological conditions to become involved in research trials; and
- highlighting the need for further qualitative research on the impact of living with a neurological condition, and on the identification of outcome measures that are meaningful to people who use care and support across the Neurological Community.
Early Priorities for Aim C
We will ensure high standards of effective, person-centred and safe care and support by:
- Exploring the feasibility of developing a national reporting framework with HIS that includes key performance indicators to measure improvements in care and support, effective measures of experience and outcome of person-centred care and support.
- Partnering with HIS to support organisations to conduct regular, open and honest self-evaluation using the Quality Framework and associated organisational self-evaluation tools and ensure that outputs are aligned through collaborative working and diligent information sharing that feeds into the wider neurological agenda.
- Developing our population data with ISD. through publication of the Scottish Burden of Disease statistics in 2020.
D: Ensure equitable and timely access to care and support across Scotland
58. Over the past 10 years there has been increasing demand on hospitals for neurology, neurophysiology, neuro-rehabilitation, neuropsychology and therapy care and support. There is also significant demand on care and support that Integration Authorities plan and commission the Health and Social Care Partnerships to deliver.
59. Over the past 10 years there has been a 13% increase in the total number of residents in a care home for disabled adults, against a backdrop of a slight reduction in registered care home places. This increase may be due to the fact that as people live longer their needs may be more complex. It also could suggest that there are significant challenges in providing care and support for people with physical disabilities, many of whom will have a neurological condition, particularly in terms of enabling them to remain in their own home.
60. The Scottish Access Collaborative Programme is working to sustainably improve waiting times for non-emergency procedures and will shape the way care and support is provided in the future.
61. Neurology is a speciality being explored through the Scottish Access Collaborative, and this work, in conjunction with the Modernising Patient Pathways Programme, should lead to better referral guidelines and care and support pathways for people with neurological symptoms across Scotland.
Commitment 14
We will seek to improve access to healthcare and support by working with the Scottish Access Collaborative for Neurology and other partners to develop nationally agreed, regionally and locally applied guidelines for health services and referral pathways for neurological conditions.
62. Mapping Neurological Services in Scotland 2017/18 confirmed considerable variation in access to care and support depending upon local services, pathways and geography. We also heard from people with neurological conditions that the care and support they received varied depending on the condition they had, and the availability of care and support in their local area. Some people reported that they received excellent care. Others reported long periods of anxiety while waiting for a diagnosis and access to care and support, and a lack of support for managing their symptoms following diagnosis. (For some conditions people feel there is no care and support available to them).
63. The Scottish Atlas of Variation aims to highlight geographical variation in Scotland’s population health, the provision of health services and associated health outcomes. The Atlas will facilitate discussion and raise questions about why differences exist and help to promote quality improvement through conversation. In time, the Scottish Atlas of Variation will be an important tool to help identify and eliminate unwarranted variation, and to support the reduction of harm and waste within healthcare.
64. Variation in care and support is not confined to health. We heard about care and support not being accessible to people in neighbouring localities because of partnership boundaries, of differences in funding essential equipment, such as communication equipment, and of lack of access to therapy services due to place of residence. We need to remove barriers to improve access to care and support so that people can move easily to access the care and support appropriate to their needs, and at the right time.
Commitment 15
We will work with stakeholders to develop proposals for maps on Neurological Conditions to be included in the Scottish Atlas of Healthcare Variation.
Early Priorities for Aim D
Ensure equitable and timely access to health and social care and support across Scotland by:
- Identifying key priorities from Scottish Access Collaborative and Healthcare Improvement Scotland neurological streams and support
their development through alignment with this Framework. - Encourage NHS Boards and Integration Authorities to consider introducing/strengthening current provision for commonly accessed services including: open access clinics and rapid access clinics.
- Identify what outcome measurements are currently reported and support development of tools to measure impact of models of care.
- Producing an Atlas of Variation proposal to create maps with a narrative to identify and tackle unwarranted variation to support improvement in outcomes.
E: Build a sustainable neurological workforce fit for the future
65. The delivery of joined up and holistic treatment, care and support requires us to think more widely about ‘workforce’ and those who support the independence, health and wellbeing of people with neurological conditions. Health and social care professionals are a huge asset, therefore it is important to support them in their current roles and in developing new roles. As staff move into new roles, we need to be able to model and predict the impact on the changing workforce and the availability of care and support.
66. There are challenges to address in this area. During the mapping exercise and engagement events, we heard of gaps in the provision of adequately trained staff to deliver care and treatment. We also know there are capacity issues for some medical, clinical and support posts in neurology, neurophysiology, neuroradiology and neuro-rehabilitation. To improve workforce planning for the wider neurological workforce, we need to build better intelligence about how and where clinical, professional and support roles across health and social care can most effectively combine to provide high quality neurological services to people who need them.
Medical Staffing
67. Medical training is managed at a UK level; the Shape of Training review proposed an important evolution in the development of specialties and their role within provision of healthcare, particularly in the acute sector.
68. Employers should work with medical staff to consider how recruitment and retention can be improved, recognising that job plans should reflect the needs of the individual as well as those of the service.
Wider workforce
69. It would be helpful for staff that do not provide specialist neurological care and support, such as other medical specialties, community teams, or staff based in care homes to receive training in understanding the specific needs that people with neurological conditions have.
70. We support the role of third sector and independent organisations in providing care, support and training. There needs to be consideration given to the sustainability of this workforce, while respecting the independence of the sector.
71. Feedback from the Neurological Community at our national engagement events identified a need to develop guidance on the use of equipment and interventions. Employers[37] are responsible for ensuring their staff have the skills and knowledge to carry out their roles. This responsibility is set out in the Codes of Practice for Social Service Workers and Employers and the Care Inspectorate use the codes in their inspections. The Health
and Social Care Standards are also relevant, in setting out what a person can expect from their service provider.
72. Part 2 of the National Health and Social Care Workforce Plan[38] proposes the development of a Framework for Practice in Social Care. This is led by the Scottish Social Services Council, and will work with stakeholders to consider how such a framework will contribute to ensuring clear routes are identified that reflect the development of appropriate expertise in the social services workforce, including management of specialist conditions.
73. The National Integrated Workforce Plan will set out our approach to integrated workforce planning across health and social care – covering many services and contexts. We will consider in more detail how neurological services can benefit from the recommendations in the Plan.
Commitment 16
We will test how national workforce planning solutions can help address capacity challenges for the neurological workforce. We will do this by improving workforce data, analysis, modelling and scenario planning to facilitate more effective and targeted recruitment into hard to fill posts in neurology, neurophysiology, neuroradiology and neuro-rehabilitation.
Commitment 17
Working with stakeholders, we will also examine how workforce planning for team-based approaches to neurological care – recognising many different roles played by nurses, allied health professionals, general neurology keyworkers, healthcare scientists and social care workers – can augment delivery, throughput and quality of services for people with neurology conditions.
Early Priorities for Aim E
Build a sustainable neurological workforce for the future by:
- Establishing immediate, medium and long term priorities and the reasons for gaps in services and shortfalls where they exist.
- Identifying opportunities to improve recruitment into hard to fill posts including medical, clinical and support posts in neurology, neurophysiology, neuroradiology and neuro-rehabilitation.
- Examining the value of potential roles played by nurses, allied health professionals, general neurology keyworkers and healthcare scientists. As this work matures, we will use findings to refine workforce planning across neurological specialists and the wider health and social care workforce involved in delivering neurological services.
- Developing a longer term approach to workforce planning, consistent with the approach set out in the national Integrated Workforce Plan that considers the range and complexity of medical, clinical and support roles involved in providing high quality neurological services.
Contact
Email: Clinical_Priorities@gov.scot