A National Telehealth and Telecare Delivery Plan for Scotland to 2016: Driving Improvement, Integration and Innovation
A joint National Delivery Plan from the Scottish Government, CoSLA and NHS Scotland, it sets out the vision and direction for a Scotland in which the use of technology, which plays an increasing role in our everyday lives, will be integrated into service development and delivery, transforming access to and availability of services in our homes and communities and more acute settings.
This Delivery Plan sets out 6 workstreams, each with specific actions to be delivered by 2015.
3.0 New Opportunties
Investing in our Digital Infrastructure
Scotland's Digital Future - Infrastructure Action Plan sets out plans for delivering a world-class and future-proofed digital infrastructure by 2020. The Step Change 2015 programme12 will enable more people across Scotland to access the internet and use telehealth and telecare. The Plan will support the increase in take-up, stimulate demand for digital access, and help the population to be at ease with digital technologies accessible through next generation broadband infrastructure(NGBi) and 3/4G mobile coverage.
Through the Choose Digital First programme we are working with a broad range of public, private and third sector partners to ensure that everyone has access to and can make best use of digital technologies. The efforts on demand stimulation will help improve the commercial case for investment in our digital infrastructure. Working with Scottish Enterprise, Highlands and Islands Enterprise and Business Gateway to provide business support and ICT advisory services to upskill staff and encourage businesses to make better use of broadband services is also a core component of Choose Digital First.
The South of Scotland Alliance (SoSA) is a strategic partnership between Dumfries & Galloway Council, Scottish Borders, NHS Borders, NHS Dumfries & Galloway, and Scottish Enterprise. SoSA have produced a South of Scotland Local Broadband Plan (LBP) which aims to reach at least 90% of the population across the South of Scotland by 2015. "The rural nature of the Borders with some towns located a considerable distance from health and care premises make the use of Telecare and Telehealth equipment vital for many service users but is dependant upon the right infrastructure being in place."
Scottish Borders Council
Reshaping Care and Integration
Our Reshaping Care for Older People Programme and the related Change Fund, which is one of the Scottish Government's key preventative spend funds (£300 million of the overall £500 million preventative spend budget), drive the transformation of service design needed to achieve the vision that public services must increasingly be built around the assets and potential of our people and communities rather than being dictated by organisational structures and boundaries.
The Change Fund represents the start of a fundamental shift away from reactive, institutional care and toward more preventative and anticipatory care that enables older people to remain safe and well in their own homes. It actively encourages the local Change Fund Partnerships - consisting of NHS Boards, Local Authorities and Third and Independent Sector representatives across the 32 community planning partnerships - to redesign health and social care services to support older people to remain independent in their own homes, thereby reducing hospital admissions, aiding discharge after a crisis and promoting the concepts of community capacity building and co-production of services between providers and users. It provides a catalyst for the development of innovative new service models that deliver treatment at home or in the community for even the most challenging of situations in a true local partnership. There are clear opportunities to utilise technology as a transformational change agent within this wider agenda.
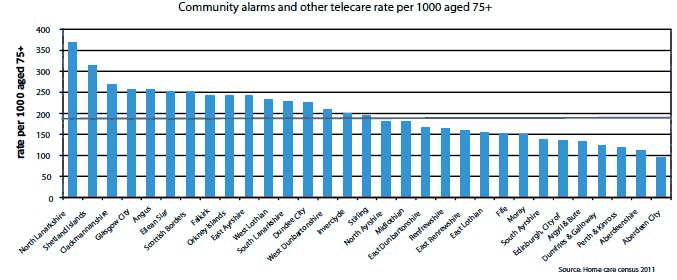
Home Care statistical data from March 2011 estimated that 162,000 people in Scotland received a telecare service but illustrates significant variation in provision across Scotland. While local circumstances should be taken into account, analysis to understand the drivers and extent of variation in practice and in service provision should be an area of shared focus for commissioners, practitioners and providers. The JIT and SCTT are supporting partnerships to redesign local pathways of care and to use their Change Fund and the Integrated Resource Framework to shift investment towards community and preventative interventions, including telehealth and telecare.
Self Directed Support (SDS) and Self Management
The principle of individuals having a greater say in how public resources are used - including how services are provided - is central to public service reform, and the Christie Commission recognised self-directed support as a means to achieving this.
Self-directed support represents a step change in the provision of social care in Scotland for the benefit of people who receive social care and support and their carers. Our Bill, which is currently before Parliament, will enshrine in law for the first time the principle of the right to choose for everyone eligible for social care.
The Bill sets out the full spectrum of options from which people can choose and, critically, it provides that the choices people make must be given effect to by local authorities. It empowers individuals to be the commissioners and lead partner in managing their care and support. Telecare and telehealth can, and should, be at the heart of both SDS and self management approaches. Emerging good practice in early adopters of SDS will be captured and shared. The Health and Social Care Alliance administer and report on the impact of the Self Management Fund for Scotland.
Case Study: Lochalsh and Skye Housing Association's Care and Repair Service
Lochalsh and Skye Housing Association's Care and Repair Service is working in partnership with NHS Highland and Highland Council to deliver telecare and telehealth monitoring devices cost-effectively to older people and disabled people in their homes. Telehealth devices are most commonly used to monitor long-term conditions such as Chronic Obstructive Pulmonary Disease, heart disease and certain mental health conditions. Daily test results are automatically sent to the Highland Hub Call Monitoring Centre, which generates an alert if any abnormality is identified. This increased monitoring reduces travel time for people in remote rural areas to and from hospital and has a corresponding reduction in stress levels. The Handyperson Service has also set up a demo/assessment room within Portree Hospital, which acts as a training facility for home carers, clients and community nurses to better understand the use and benefits of the devices.
Co-Production
People invariably have skills, talents and capabilities and are often looking for opportunities to 'contribute'. We need to support people to draw on these strengths and to support them to have more control over their own health and care, and in caring for others. "Co-production recognises that people have 'assets' such as knowledge, skills, characteristics, experience, friends, family, colleagues and communities. These assets can be brought to bear to support their health and wellbeing".13 We require to make both cultural and organisational shifts to embed asset-based approaches and co-production but it is clear this is a key driver for person-centred health and care and effective service delivery.
The 'Living it Up' Project in Forth Valley, Moray, Highland, Lothian and Western Isles is using co-production to shape the way that new technologies facilitate services, products, and information to support people to manage their Long Term Conditions and wellbeing. Community engagement work, led by Glasgow School of Art, the Health and Social Care Alliance and Carers Scotland brings together all partners to 'co-design' solutions by sharing their experience, skills and different perspectives. Partners include individuals, carers, local communities, third sector organisations, industry, enterprise and health, housing and care practitioners. This is all part of an 'at scale' initiative funded jointly by the Scottish Government and the Technology Strategy Board.
Innovation
Scotland has a long-established reputation and appetite for invention and innovation.14 Innovation, in all its forms, is already playing a key role in rethinking and changing the way we organise, finance, and deliver health, housing and care services. Our Statement of Intent for Innovation in Health aims to develop close working relationships with companies and NHSScotland to focus on future needs for technology and related products in health and healthcare.
There are considerable opportunities for academia, SME companies, third sector and global technology partners to be involved in testing, developing and implementing solutions to transform the design and delivery of health, care and wellbeing support in Scotland. Aligning and channelling these industry and academic resources and expertise appropriately could have a positive economic impact.
Case Study: A Digital Health & Care Innovation Centre
Scotland has outstanding resources in Digital Health and Care: world-leading medical research; world-leading Informatics research; outstanding health databases; recognised leadership in the delivery of telehealth and telecare; centres of excellence in design, organisational science, psychology, and evaluation of health systems. Partners from the Scottish Assisted Living Programme Board are seeking to establish a Digital Health and Care Innovation Centre to provide additional capacity to further develop the existing virtual network on digital health and care, and support integration.
This ambitious proposal has the potential to provide a focus for concerted action within an already vibrant digital health and care community. It would bring together academics, communities, practitioners and businesses, to focus and consolidate Scotland's leading position in Digital Health and Care innovation. It will enable 'Team Scotland' to challenge and transform health and care delivery and stimulate the creation of new products and services backed by experience and expertise from our expert communities.
Europe
Scotland is widely regarded in Europe as a country that has a mature approach to integrating telehealth and telecare in the delivery of services. The Scottish Centre for Telehealth and Telecare now represents Scotland in a range of European-funded projects aimed at realising the benefits from telehealth and telecare.
The European Commission is a powerful advocate for the use of information and communications technologies. It promotes their pivotal role in delivering a Triple Win for Europe:
- Improving health and quality of life;
- Supporting the long-term sustainability of health and social care systems;
- Growing and expanding opportunities for industry and the economy.
The Commission launched its European Innovation Partnership for Active and Healthy Ageing (EIPAHA) in 2011. This is a flagship development and has clear synergies with Scotland's priorities for 2020. The Scottish Government, as one of the leaders in Europe in this field, has been working directly with the Commission in the development and design of EIPAHA. This engagement offers mutually beneficial opportunities through knowledge exchange with other regions and access to funding opportunities in support of this high profile and transformational agenda.
The European Innovation Partnership (EIP) aims to increase by two the average number of healthy life years in the EU by 2020, by securing a triple win for Europe:
- Improving the health status and quality of life for European citizens, with a particular focus on older people;
- Supporting the long-term sustainability and efficiency of health and social care systems; and
- Enhancing the competitiveness of EU industry through an improved business environment providing the foundations for growth and expansion of new markets.
The EIP Steering Group has structured the programme around three pillars which reflect the life stages and the care pathway for the older person: Prevention, Screening & Early Diagnosis; Care and Cure; and Active Ageing and Independent Living.
Strategic implementation plan for EIP on Active and Healthy Ageing, Nov 2011
Contact
Email: Alistair Hodgson