National ophthalmology workstream: hospital eye services
How we plan and manage the delivery of hospital eyecare services to provide timely care for patients.
5. What Good Really Looks Like
5.1 Clinical Condition Pathways
At all sites in Scotland there is evidence of good practice and overall there are many areas where Scottish services excel. Adoption, adaption and consolidation of these proven approaches should therefore form the basis of each Board's way forward and detailed local action plan. It is also acknowledged that in Scotland we already have the elements of a blueprint and an evidence base of what works and what gains are realistically achievable - with accepted local variation. A number of high impact developments have been identified as being significant e.g. nurse injectors delivering intra-vitreal anti VEGF treatment for Age Related Macular Degeneration. The Peer Review process too, has created significant momentum, for change and improvement.
The vision for NHS Scotland is to achieve a Target Operating Model for Eye Services across primary and secondary care. The intention is to design and deliver a world class service, in state of the art facilities which is person centred, safe and effective. Measurable outputs are essential to this approach so that we can continuously challenge our decisions, our systems and processes so that all services work to the top of their scope with comparable efficacy and outputs. This may also mean that not all services will be provided in all places so that we can streamline provision and location so that every patient is seen in the right place, at the right time, by the right professional. The six keystone considerations revolve around managing the whole system and recognising that high volume surgical conditions and Long Term Conditions need to be dealt with differently and effectively.
5.1.1 High volume surgical condition - Cataracts - issues and achievable benefits still to be realised
Figure 2: Keystone consideration 1: cataracts
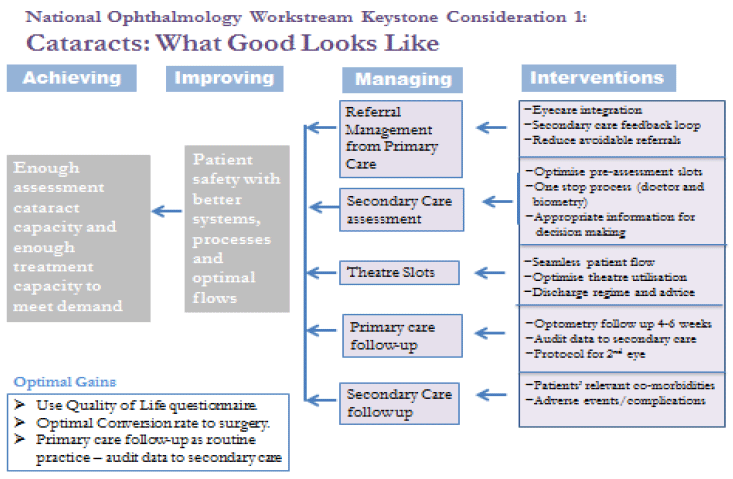
Referral Management: The overall objective is to create sufficient assessment and surgical capacity to meet demand. The ophthalmology peer review visits revealed that there is variation across Boards with regard to the numbers of patient referred for cataract surgery and those actually progressing to surgical intervention. This 'conversion rate' from referral from primary care to cataract surgery ranges from 50-90%. This, in part, may be a consequence of Boards being at different stages with the roll out of electronic referrals which allows standard proforma to be completed and sent to secondary care. Presently with non-electronic referrals there is variation in the information received via optometry practices. Ongoing training of optometrists, development of clear pathways and communication between primary and secondary care is in hand to ensure that patients are referred for surgery at the right time with all the necessary information. False positive referrals - those patients who either do not need or wish for surgery - are a poor use of both the patients and hospital time.
Recommendation: Adequate training of primary care practitioners - optometry and general practice - to ensure that those referred for cataract surgery are suitable candidates for surgery. Monitoring of conversion rate to surgery is essential in order to capture appropriate referral patterns.
As a consequence of the variation of conversion rates to cataract surgery, the Director of Optometry at NHS Education Scotland, is developing an e-learning package, supported by webinars and it is anticipated this will rolled out in the middle of 2017.
Secondary Care Assessment: There are different pre-assessment models across the country. In NHS Ayrshire and Arran 75% of patients undergo a rigorous assessment by optometrists and are pre-assessed by nursing staff via telephone - biometry and consent are undertaken on the day of surgery. This is a model that has been in use for many years and is wholly dependent on training of specific optometrists for the role which is on-going and relies on local relationships. It is acknowledged though, that surgeons meeting patients on the day of surgery runs the risk of an increased cancellation rate.
The workforce involved in pre-operative assessment is also variable across the country. In NHS Highland, nurses and hospital optometrists pre-assess patients and consent is taken by the optometrist at the pre-assessment visit. However, in NHS Dumfries and Galloway one nurse undertakes all aspects of the pre-assessment appointment resulting in fewer patients being reviewed within each session; while in NHS Tayside and at the Golden Jubilee consultants review each patient at the pre-assessment clinic prior to being listed for a surgical procedure. Overall the average number of patients pre-assessed in one dedicated cataract session ranges from 3-14 patients. Some HES do not have cataract only pre-assessment slots and assess all ophthalmology patients referred for ophthalmic surgeries in mixed pre-assessment clinics.
Recommendation: Pre-assessment slots should be optimised in a dedicated one stop process to prevent unnecessary hospital visits. The clinics should be streamlined to optimise numbers assessed with adequate space and staff.
Cataract Theatre Throughput: The national monthly management information for the HES has identified significant variation in the number of cataracts undertaken in a 3.5 hours' theatre session. The majority of cataract surgery is not undertaken on dedicated cataract theatre lists, but on mixed case lists (i.e. with other ophthalmic surgical procedures). On those lists that are 'cataract only' the overall numbers vary from three to seven per session. It was recommended in Action on Cataracts, 2001 that one cataract should be undertaken every 30 minutes - including turn-around time and this was re-iterated in the Monitor Report. Some Health Boards use a scoring system which outlines the number of cataracts that can be added to a theatre session depending on the degree of surgical difficulty ( DSD). This scoring system developed by Dr Patrick Kearns and colleagues in NHS Fife, now adopted at the GJNH, can be found at appendix 2.
Recommendation: Cataract theatre lists should aim to undertake one case every half hour.
Turn-around Time
The turn-around time is the critical rate limiting step in cataract surgery theatre utilisation. Departments indicated that generally the limitation in numbers performed was due to lack of support staff (adequate porters, health care assistants, scrub nurses etc.) or because of the geography of the building - leading to delays caused by slow lifts or long distances to travel. The National Ophthalmology Workstream is working with Health Boards to mitigate rate limiting steps and reduce turn-around time.
Making a difference
The MMI has been revised to reflect the fewer number of cataract only sessions undertaken - many cataract surgeries are undertaken as part of a mixed theatre list and consequently the first seven months of data which focussed on the number of cataract surgeries undertaken in a 3.5 hours' theatre session appeared fewer as a consequence of being diluted within mixed theatre lists. The Golden Jubilee National Hospital is exploring ways to reduce their turn-around time through double scrub theatre lists. Currently this sits at 8 minutes - measured form speculum to skin and accounted by:
- 1 minute for writing up the case
- 2 minutes surgeon de-gowning, scrubbing and re-gowning
- 2 minutes prepping patient
- 2 minutes draping
- 1 minute final pre-op check (surgical pause)
If the hospital can delegate prepping and draping to other members of the multi-disciplinary team, there is scope to reduce this time from 8 to 4 minutes. The GJNH is also working towards supporting the training junior surgeons.
There is anecdotal evidence to suggest that some Boards are having difficulty in 'pulling' information from existing theatre systems and require to manually count the number of procedures undertaken for specific sub-specialties. Systems and processes should be able to capture and measure procedures undertaken in an allocated timeframe to ascertain the time taken to undertake cataract procedures in mixed theatre sessions and to benchmark variations across Health Boards and consequently ensure best practices are shared between colleagues.
Recommendation: Explore processes and ensure that turn-around time is as short as possible.
Potential to increase cataract throughput: In November 2016, across NHSScotland, 666 ophthalmology theatre sessions were undertaken. 278 of these sessions were cataract only sessions and 1689 cataracts were performed. Although this equates to an average of 6 cataracts per session, there is still widespread variation ranging from 4-9 cataracts undertaken in a 210 minute theatre session.
Recommendations:
- Each Health Board should review causes for reduced cataract numbers per list to improve throughput.
- Consideration should be given to cataract only lists - alternating with other surgical lists alternate weeks.
Primary care follow-up post-cataract: Across NHSScotland patients are followed up in a variety of different ways. Some clinicians discharge all patients directly to community optometry following both first and second eye surgery, others restrict discharge to those undergoing second eye surgery only and some review all post-operative cataracts in the HES (usually by in house optometrists, nurses or orthoptists). Patients with other ocular pathology or complicated surgery are not suitable for post-operative review in the community and clear, shared communication channels need to be active for all discharged patients.
NHS Highland has discharged all cataracts directly into the community for more than 10 years - recognised communication channels to the hospital for the patient and the optometrist are in place.
Alongside this, it would seem that the General Ophthalmic Contract has been interpreted differently across Health Board areas with some community optometrists requesting remuneration unless the patient has been discharged by the hospital - therefore first eye cataract cases are all seen in the HES. The peer review visits revealed around 60-70% of patients have cataract surgery on both eyes.
Recommendation: Suitable patients, who have no other ocular morbidity - including complicated surgery - should be considered for discharge to community optometrists for post-operative review and refraction, ensuring that audit forms are returned to secondary care. First and second eyes should be considered and booking processes for those patients that have been deemed clinically appropriate to progress to second eye cataract surgery should be in place.
5.1.2 Out-patient clinics - Long Term Conditions - issues and achievable benefits still to be realised.
Figure 3: Keystone consideration 2: Long Term conditions management
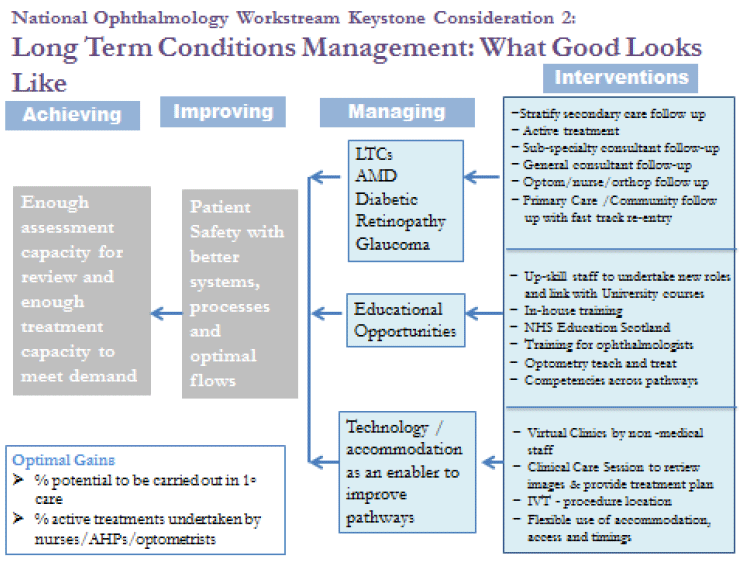
It is recognised that long term ophthalmology conditions require lifelong monitoring and often intervention to prevent deterioration of sight threatening conditions.
Intra-vitreal anti VEGF injections: Pharmacological agents (anti- VEGFs) to treat, previously untreatable, medical retinal conditions such as age-related macular degeneration, diabetic maculopathy and retinal vascular disease are now commonplace. These conditions also require regular diagnostic tests to monitor the effectiveness of the treatment. Previously, injections were administered by medical staff, however, following changes in governance, it has been possible for non-medical Health Care Practitioners - usually nurses - to deliver these treatments following a period of training.
Treatment Regimes: The number of injections that patients receive will depend on their response to treatment, although all patients will routinely receive three loading doses of the drug via intra-vitreal injections. The number of injections any one patient requires can be as few as three but it is clinically appropriate for some patients to require and receive life-long treatment. The number of IVT injections undertaken across the country is extrapolated from different sources: some Boards record this data on hospital systems and in others this information is captured by pharmacy - number of drug vials used.
The MMI highlights that the number of injections carried out in a standard session varies from 12-18 procedures. This, in part, can be explained by newly trained non-medical HCPs who are starting to undertake these procedures. Nurse specialists who have been up-skilled for the past few years are delivering the same number of injections as their medical colleagues with excellent patient satisfaction. As this workforce continues to undertake these procedures, parity in the number of injections undertaken in each session will expect to be similar across Health Boards.
One of the limiting factors with administration of IVT injections has been highlighted as appropriate accommodation. A clean room is necessary to ensure, as far as possible, a sterile environment in which to undertake the procedure. Otherwise, some NHS Boards have resorted to utilising theatre capacity to ensure patient safety. This will have a compounding effect on the number of surgical procedures undertaken, and is a clear rate limiting factor.
Recommendation: Ensure appropriate accommodation is available to prevent theatre capacity being utilised for procedures that require clean room status. Injections should be carried out in a clean room rather than in theatrae
Recommendation: to optimise use of clinical time, anti VEGF injections should be routinely performed by non-medical HCPs - usually, but not exclusively nurses.
Stratified risk of patients: Once firm diagnosis has been determined, patients with chronic ophthalmic conditions should be stratified into low risk, medium risk or high risk in order to determine the optimum mechanism of follow up - which may be face to face with a consultant or an HCP or in a virtual format.
Virtual consultations using technology: Virtual clinics are being used more frequently for long term conditions such as AMD and glaucoma to enable patients to attend for clinical assessment and imaging - which, in the virtual clinic situation - can be undertaken by non-medical HCPs. Images and clinical information are then reviewed by an ophthalmologist remotely, enabling the clinician to review many more patients than they could have done by assessing each patient in person. Only those patients in which there is a change in their clinical condition or who require a decision regarding further treatment require to be reviewed directly by the ophthalmologist.
Recommendation: HCPs should be trained to perform clinical assessment and imaging on low risk patients to help facilitate virtual clinics, where feasible, using appropriate IT and connectivity.
Injection protocols
Not only do patients require to attend for injections, they also require diagnostic tests ( OCTs) to assess the effectiveness of the treatment as well as out-patient review by ophthalmologists and/or virtual assessment. In order to utilise all available slots per session, some Boards have chosen to implement a combination of booked with 'see and treat' - one stop appointments. For example, NHS Forth Valley appoints those patients requiring a loading injection (required as initial treatment) at the beginning of a session. This prevents the lag time at the start of a see and treat clinic, especially if the first patients reviewed do not require an IVT injection.
Recommendation: To ensure maximum utilisation of injection slots, consider a mixture of booked and 'see and treat - one stop' slots. This will reduce the number of hospital attendances by patients allowing diagnostic tests, treatments and review to be undertaken in as few appointments as possible to manage the patient's condition as clinically indicated.
Remote and Rural: In remote and rural areas it can be challenging for patients to attend regional centres for review, appropriate patients could be reviewed by a high street optometrist in conjunction with secondary care through the use of technology. This is currently being explored by NHS Ayrshire and Arran who are undertaking a scoping exercise supported by the National Ophthalmology Workstream.
5.2 Enablers - mechanisms to deliver the changes
5.2.1 Health Intelligence - issues and achievable benefits still to be realised
Figure 4: keystone consideration Health Intelligence
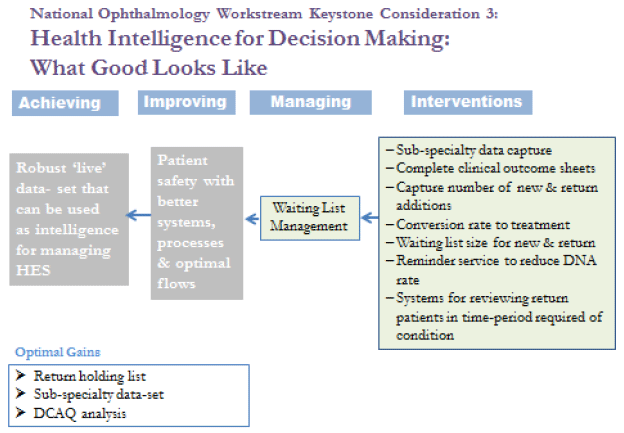
Information for decision making: Presently, there are limited data to inform capacity planning and what limited data are available are only at general ophthalmology level and not at sub-specialty level or, more specifically at diagnostic level. Such data are essential in order to plan services and manage change in a positive way.
The national ophthalmology workstream is collaborating with Information Services Scotland ( ISD) to deliver a solution to improve the dataset and to enable information on review patients - capable of capturing and monitoring the clinically indicated time of review - to be locally implemented and a national return collected. The recognition of the lack of capacity to manage review out-patients has been acknowledged nationally and to proactively manage the capacity required for service delivery, these data are essential. Presently, there is good evidence that patients are being reviewed in a timeframe significantly beyond that requested by the ophthalmologist due to insufficient capacity within existing Hospital Eye Services, and this was confirmed at Board level during the peer review process. This is exacerbated by the general separation of booking new patient appointments from return patient appointments. This indicates that there is an unmet need, but that need has not yet been quantified. The effectiveness of some treatments is dependent of being reviewed timeously, such that late (expensive) treatments could be wasted treatments, and therefore wasted resource, because the window of treatment opportunity has been missed.
Recommendation: data capture of review patient appointments and any delays to patients being seen in a clinically safe time is required.
From 2008 the number of new outpatients reviewed at Hospital Eye Services increased by 8.8% ( ISD). The total attendance at Hospital Eye Services (new and return patients) has increased from 406,609 attendances in 2008 to 438,358 in 2015. This 8% increase in overall attendances reflects the demographics of this patient cohort, along with the fact that individual patients require multiple attendances with a combination of diagnostic tests and, for example numerous intra-vitreal injections to treat conditions such as age-related macular degeneration.
Sub-specialty Tagging: As already highlighted, there is inadequate output of sub-specialty data for drill down. A few Boards are implementing this process although, to date, implementation is variable. As part of a test of change sponsored by the National Ophthalmology Workstream, NHS Lanarkshire has implemented a planned review list ( PRL) for their medical retina service which allows the service to appoint patients in the time critical period required of their condition; it also enables the service to quickly identify if extra capacity is necessary at specific times due to a fluctuation in demand/activity is required. NHS Dumfries and Galloway operates a 'hopper' system and has implemented sub-specialty planning across all ophthalmology sub-specialties; this originated via a retrospective data set and currently the Board can prospectively capture which patients require review in a particular timeframe. There is a threshold before and following the clinically indicated date of review that allows a degree of flexibility for booking staff - this period is relative to the length of the review date e.g. if the patients required to be reviewed in one month, there may be a week's flexibility either side of that date. For return appointments, for example, which require a 6 months' appointment this may extend to one month either side. This model ensures patient focussed care can be planned and in tandem with this, will forecast any increase in activity and allow Hospital Eye Services to plan accordingly. Ensuring that all interventions below are actioned will enable each HES to undertake Demand, Capacity, Activity Analysis which will enable patient focussed treatment.
Recommendation: Sub-specialty data capture is essential to make current and future plans - and to manage change intelligently.
5.2.2 Booking Processes / Management - issues and achievable benefits still to be realised.
Figure 5: Keystone consideration: Booking Processes
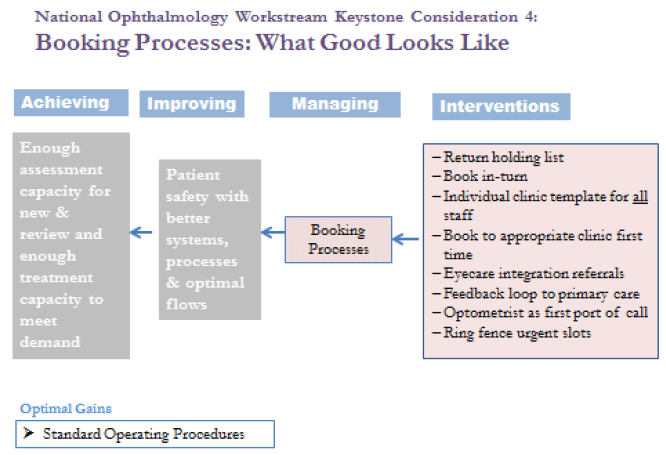
'The way that appointments are booked can have a profound effect on the efficiency of hospital processes and ultimately the delivery of safe and reliable services for patients.' (Effective Patient booking for NHSScotland).
Patients should be booked in the clinically indicated timeframe to manage their condition and allow best outcomes of treatments. Staff working in booking areas, irrespective whether it is in a booking hub, or managed by an ophthalmology team, should be aware of the importance of ensuring that diagnostic tests and treatments should be closely aligned to prevent unnecessary duplication of attendances and improve the patient experience and ultimately the clinical outcome.
- Prior to making a referral, the referrer should use a booking fact sheet to discuss the process and purpose of referral with the patient;
- Staff within an NHS Board should work to standard operating procedures/protocols to ensure equity in appointing patients;
- A process should be established to promote booking in turn and to monitor booking processes;
- A standard vetting approach across all hospital sites to include agreement of sub-specialties/capacity categories;
- Continue to support the reduction of DNA/ CNA and cancelled clinics with less than 6 weeks' notice;
- Implement a Patient Reminder System to support utilisation of available capacity;
- Ongoing waiting list validation to ensure maximum clinic utilisation;
- Utilise clinic outcome data to support future service planning and review regularly to identify opportunities for improvements to pathways such as required to account for the variation in demand.
Along with this, Hospital Eye Services are, in the main, still using paper systems rather than electronic patient records ( EPR) which can be challenging especially when viewing images to assess a patient's disease process. In some areas images are stored as pdfs making the process of assessing images slow and consequently the patient pathway is protracted. A few Boards are introducing 'paper- lite' systems while a few others are using stand-alone modules for a single condition. Information and technology departments wish to ensure, that if specific systems are procured, there should connectivity with existing hospital systems to ensure all information relating to a patient's health/co-morbidities are housed in one area. A test of change is underway in Greater Glasgow and Clyde Health Board using a bespoke version of Open Eyes with existing systems and processes ( SCI Gateway, Trakcare and Clinical Portal) to ascertain if there is a gap with these existing systems and consequently if Open Eyes can bridge the gap and produce an Electronic Record that enables 3-D images to be viewed.
Recommendation: An electronic patient record system that meets the needs of ophthalmology should be introduced in order to permit electronic capture of clinical data, audit and follow up data. Where appropriate this will promote care across primary and secondary care through data sharing.
5.2.3 Workforce - issues and achievable benefits still to be realised
Figure 6: Keystone consideration 5: Workforce
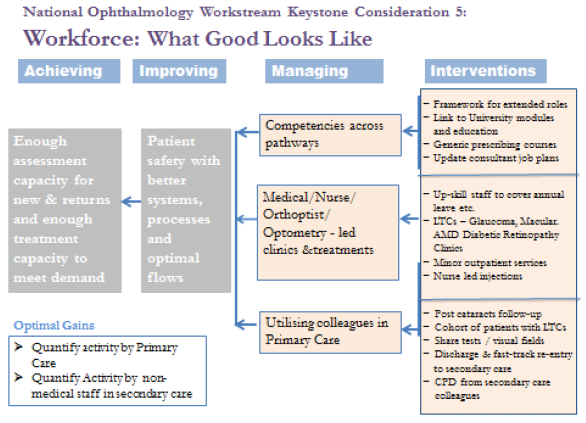
There are many good examples of staff roles being expanded and HCPs such as ophthalmic nurses, optometrists and orthoptists undergoing training to undertake further duties in conjunction with and on behalf of medical staff; freeing up ophthalmologists to make complex clinical decisions and to undertake treatments and surgical procedures. Increasingly, non-medical HCPs within the hospital service are being up-skilled to undertake IVT injections, perform minor surgical interventions, carry out pre-operative cataract assessments, review low risk or stable patients and carry out new and return out-patient clinics across a number of ophthalmology sub-specialties including glaucoma.
Although already staff are employed to undertake these duties and work at the top end of their competencies, there is often no backfill when they are on annual leave and consequently waiting lists accumulate and/or senior medical staff undertake these duties, or undertake extra clinics to ensure patients are reviewed in their clinically indicated timeframe. In order to overcome this issue, Greater Glasgow Clyde are in the process of up-skilling a number of nurse practitioners who will be able to undertake IVT injections on a sessional basis when necessary. Not only does this ensure succession planning, but also promotes continuing professional development. Junior doctors also work alongside non-medical staff as an adjunct to teaching and training by consultant colleagues to ensure that they achieve the competencies required, prior to undertaking many of these procedures autonomously.
Recommendation: In order to deliver treatment(s) in the clinically indicated timeframe, ensure that there are sufficient members of the multi-disciplinary team who are up-skilled in order to provide cross-cover/back fill sessional work when required.
There is a shortage of consultant ophthalmologists in Scotland with a majority (73%) of departments reporting a vacancy and recognising the need for further recruitment in the next 2 years. This is impacting on all aspects of delivery of care including surgery, management of ophthalmic medical conditions and the leadership required to effect change. Imaginative options are essential to attract and retain an adequate highly trained ophthalmic consultant workforce in Scotland. Such options include - consultant appointments across different Boards to accommodate remote and rural issues and consideration of sharing out-of-hours care. Developing multi-disciplinary ophthalmic teams who work together to provide a sustainable service is essential for the current and predicted future demands.
Recommendation: Mechanisms to improve recruitment and retention of consultant ophthalmologists to be explored at national and regional level.
5.2.4 Primary Secondary Care Interface - issues and achievable benefits still to be realised
Figure 7: Keystone consideration 6: Primary Secondary Care Interface
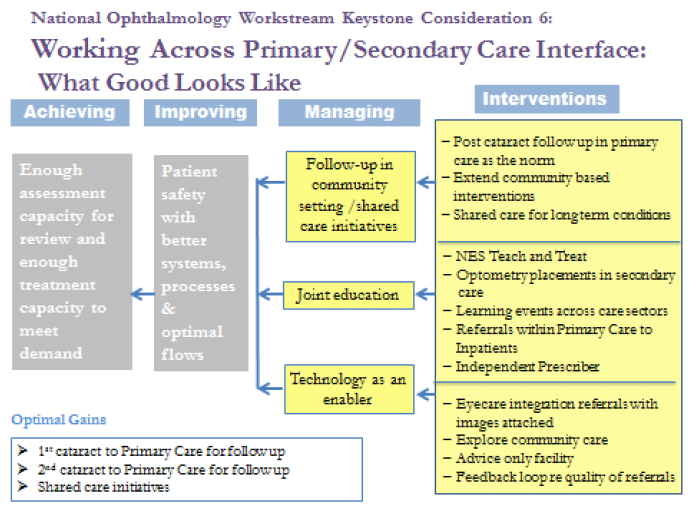
There remain a number of ways that the capacity in primary care optometry can be better used to assist delivery of care currently carried out in the HES as highlighted in section 5.1.1.
Increasingly in Scotland, the public recognise that high street optometry is the first port of call for ophthalmic primary care and are sign posted to their optometrist for the assessment of minor eye conditions. Whilst there are a number of independent prescribing optometrists across the country, some Boards work collaboratively with their GP colleagues regarding co-prescribing and therefore enabling prescribed treatments to be commenced in the community and/or to prevent patients attending for follow up appointments in secondary care, for conditions such as diagnosed ocular hypertension. NHS Tayside have discharged patients to the community for this patient group in line with the SIGN guidelines for glaucoma - with clear guidance about when patients should be re-referred.
The Community Eyecare Review has highlighted that "General Ophthalmic Services ( GOS): is to be seen as the core service which all optometrists provide, with the need to ensure that all have the required competencies and undertake mandatory and ongoing Continual Professional Development." This, in tandem with a view to registering patients with a named optometrist akin to being registered with a dental or medical practitioner, is being considered to promote continuity of care and patient safety. This is coupled with a need for training to accredited standards that meet NICE guidance for Glaucoma - and cataract and medical retina over the next two years as new NICE guidelines for these conditions are developed.
Recommendation: Continuing training for community optometrists remains a high priority. Identifying mechanisms to provide clinical training within the HES should be considered.
Contact
Email: Jacquie Dougall
Phone: 0300 244 4000 – Central Enquiry Unit
The Scottish Government
St Andrew's House
Regent Road
Edinburgh
EH1 3DG