National ophthalmology workstream: hospital eye services
How we plan and manage the delivery of hospital eyecare services to provide timely care for patients.
4. Delivering the Aims
A systematic approach has been employed to deliver of the aims of this work -
- Initially a scoping exercise to identify possible opportunities for the development of new models of care in individual departments was performed;
- These were supported and evaluated through a Test of Change process;
- Next each was considered for national roll out, based on 6 keystone considerations;
- National strategy symposium and workshop to discuss methods to embed best practice;
- Latterly peer review visits to every ophthalmic department in Scotland.
The fundamental priorities for Workstream have been addressed throughout:
- Using data to inform booking processes;
- Promoting novel pathways to deliver care - in primary and secondary care;
- Recognising workforce deficiencies and identifying how these can be met by
- attractive recruitment measures to meet the shortage of consultant ophthalmologists and
- reviewing the roles of and upskilling the HCP workforce;
- Exploring the role of technology.
4.1 Tests of Change
Since 2014, a focus has been placed on offering support to each Board in testing initiatives that have been shown to work in some settings and to understand whether they may translate to local eye services by adapting existing knowledge. To support this improvement, each Board was asked to measure the success of each test and gauge the outputs/benefits of their improvements to evidence their impact that may therefore be replicated elsewhere. These measurements may, for example, reflect an increase in activity by streamlining pathways and/or processes, or by releasing capacity. Common areas of focus are in line with the aims of the NOW and include all elements of the workstream:
- Using data to inform, support and improve booking practices to ensure that patients are booked safely and that reflects capacity within the service;
- Promoting novel pathways to deliver care;
- Reviewing roles of and upskilling the HCP workforce -training HCPs to undertake procedures previously performed by medical staff, releasing doctors to perform high level decision making tasks or procedures only they can do;
- Working across the primary secondary care interface - strengthening working relationships to develop and manage non-medical professionals' skills to manage low risk patients safely in the community;
- Exploring the role of technology - using tele-consultations and the development of virtual clinics.
There have been numerous ' Tests of Change' sponsored by The National Ophthalmology Workstream over the past two years. Table 2 below highlights one test from each Health Board . Please note, this list is far from exhaustive.
Table 2: Examples of 'Tests of Change.'
| NHS Health Board | Examples of Test of change |
|---|---|
| Ayrshire and Arran | Scoping and developing a technical solution to allow two way electronic communication and sharing of images with community optometrists for a shared care initiative. |
| Borders | Education - up-skilling workforce. |
| Dumfries and Galloway | Information to sub-specialty level for capacity planning. |
| Fife | Integration of the management of acute anterior uveitis between primary care optometrists and the hospital eye service. |
| Forth Valley | Advice only session for community optometrists. |
| Golden Jubilee National Hospital | Information video for patients undergoing cataract surgery to standardise information. Video conferencing to assess patients travelling to GJNH for cataract surgery. |
| Grampian | 'App' to host optometry guidelines for community optometrists. |
| Greater Glasgow and Clyde | Proof of concept with Open Eyes, dovetailing with existing systems to develop an Electronic Patient Record. |
| Highland | Realignment of systems and processes to streamline the cataract pathway. |
| Lanarkshire | Planned review list ( PRL) for medical retina. |
| Lothian | Glaucoma stratification regarding complexity of a patient's condition and subsequent follow-up location. |
| Tayside | Innovative development of virtual macular clinics to change expectation and flows. |
Some Tests of Change are being led nationally e.g. from a training and continuing professional development perspective, sponsoring the development of ophthalmology educational modules for nurses with 20 places per academic year, delivered at and accredited by Caledonian University. The first cohort of students graduated from the course in January 2017.
4.2 What Good Looks Like
Focus has been placed on adapting, adopting and embedding these 'Tests of Change' to make permanent change as part of the day-to-day operation of the system. The clinical and managerial community working across Hospital Eye Services have been key partners in confirming 'What Good Looks Like' articulated as the Six Keystone Considerations that reflect the NOW elements, illustrated in Figure 1.
- Utilising intelligence to inform capacity planning
- Booking Processes
- Workforce
- Primary / Secondary care interface
- Out-patient activity - management of long-term ophthalmic conditions - Age-related macular degeneration, diabetic retinopathy and glaucoma
- Management and flows of high volume surgical work - cataracts
Figure 1: Overarching workplan 'What Good Looks Like'
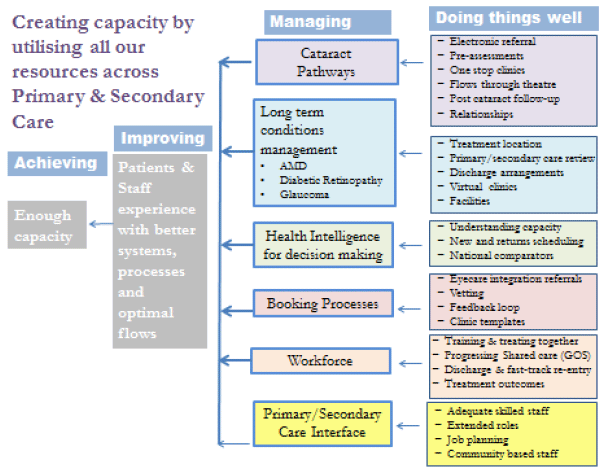
Using these keystone considerations, each Board assessed remaining gaps and opportunities, reviewing their priorities and options for standardised implementation across Scotland.
Some aspects of the keystone considerations are being sponsored and fast tracked nationally. Others depend on improvement methodology for their development. Significant cross-fertilisation continues with Boards communicating with each other and sharing ideas and driving common themes. Increasingly, organisations are working together to implement the changes created.
4.3 Embedding Best Practice - National symposium
The national ophthalmology event held in November 2015 showcased the positive improvements to ophthalmology services, gave delegates the chance to network and collaborate with their clinical and managerial colleagues and offered an important further catalyst for change. Benefits and value of the Tests of Change were considered and discussed around the 6 Keystone Considerations. Further useful work at the symposium included a debate about the design of optimal pathways to galvanise each Board's proposals to improve capacity and flows within their Eye Services.
These procedures and processes, once routinely harnessed, will make a cumulative positive impact to service delivery and enable each patient to be seen in the right place, by the right person. Continuing national emphasis is being placed on concentrating efforts across the Eye Care community to achieve maximum impact.
Such developments align well with the Monitor report (October 2015) which aims 'to help NHS providers make improvements in the productivity of elective care / in the two largest elective specialties - orthopaedics and ophthalmology.' The report recommends that 'focussing on five of nine good practices reviewed will realise most of the potential productivity gain.' For Ophthalmology, these five practices are:
- Stratifying patients by risk and creating low complexity pathways for lower-risk patients;
- Extending clinical roles to enable lower-grade staff to undertake routine tasks in theatre or out-patients usually performed by consultants;
- Increasing throughput in theatres by explicitly measuring, communicating and managing the number of patients per theatre session;
- Implementing enhanced and rapid recovery practices to reduce length of stay;
- Providing virtual follow-up for uncomplicated patients.
The Monitor report concluded that no service model or organisation appears to excel in all five aforementioned practices. Therefore by harnessing and embedding these practices across Health Boards, there remains scope to work differently in these specialties.
4.4 Peer Review Visits
Throughout May and June 2016, formal 'set piece' peer review visits were undertaken to all mainland Health Boards across NHSScotland, in order to focus on the key local issues which contributed to gaps, opportunities and variation.
These were led by Professor Carrie MacEwen and supported by clinicians and managers from other Health Board areas. The visits were viewed as positive and constructive and focussed on the Keystone Considerations that form the overarching workplan of the National Ophthalmology Workstream. Current initiatives, local limitations and recommendations for action and support were identified.
A department specific report was formulated based on each Board visit - highlighting the strengths of the department and identifying areas where support would benefit the service.
Each Health Board area was tasked with reinvigorating their local ophthalmology action plan to progress throughout 2016/17 - as highlighted, local Tests of Change have been used to implement Health Boards' action plans and have been, in part, supported by the National Ophthalmology Workstream for the past two years These local plans went further and set out Health Boards' further delivery intentions and their priorities for specific areas within the specialty which require detailed analysis locally in order to treat patients most appropriately. Practical support and partnership working are being used to drive rapid improvement, with emphasis on clear actions and timelines relating to implementation.
Contact
Email: Jacquie Dougall
Phone: 0300 244 4000 – Central Enquiry Unit
The Scottish Government
St Andrew's House
Regent Road
Edinburgh
EH1 3DG