Primary care: national monitoring and evaluation strategy
Our approach to Scotland's national monitoring and evaluation of primary care reform up to 2028.
Background: Primary Care Policy in Scotland
There is clear international evidence that strong primary care systems are positively associated with better health and better health equity. Figure 1 illustrates how the Scottish Government’s six Primary Care Outcomes align to the National Health and Wellbeing Outcomes[2] and the National Performance Framework.[3] Tackling inequalities runs as a thread through the Primary Care Outcomes and associated actions to deliver them.
Figure 1: Scottish Government Primary Care Outcomes[4]
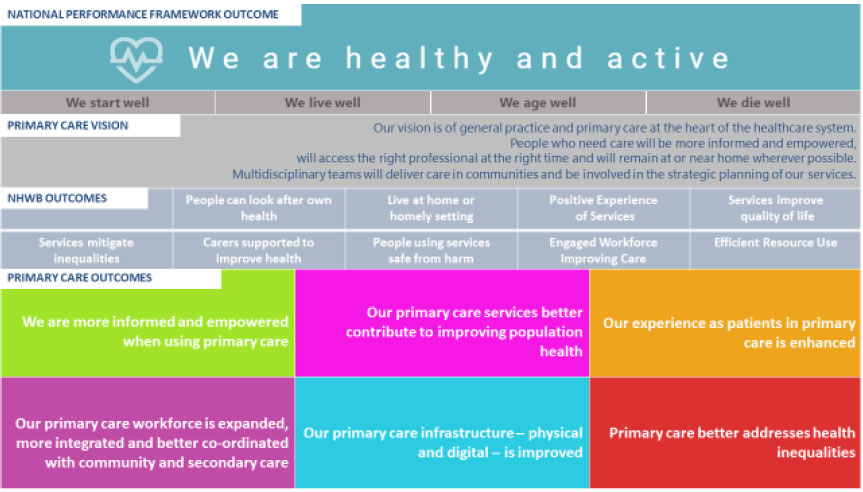
As set out in “The Health and Social Care Delivery Plan”,[5] the Scottish Government’s vision for the future of primary care is for enhanced and expanded multi-disciplinary teams, made up of a variety of roles across health, social and community services, each contributing their unique skills to improving outcomes for individuals and local communities. This will help deliver our aspiration of care being provided at home or in a homely setting, and help ensure rewarding, well-supported careers for our healthcare workforce. Getting primary and community care right is an essential component in ensuring the health and social care system is sustainable, helping achieve the Delivery Plan’s “triple aim” of better care, better health and better value.[6]
With our local and national partners, we have embarked on an ambitious programme to support and develop primary and community care. The First Minister announced in October 2016 an increase in funding for primary care of £500 million by the end of the current Parliament. This investment will see at least half of frontline NHS spending going to community health services and will enable us to expand the primary care workforce to deliver improved patient care. Our commitments to significantly develop and expand the primary care multidisciplinary team (MDT) are set out in our national primary care workforce plan.[7]
The next three years will see significant reform in primary care that will provide the bedrock for what we do in the years beyond 2021. The General Medical Services Contract for GPs[8] establishes a refocused role for all GPs as Expert Medical Generalists (EMGs) and as the senior clinical decision maker in the community. The Memorandum of Understanding (MoU)[9] between Integration Authorities, the British Medical Association, NHS Boards and the Scottish Government supports the delivery of the EMG role through service redesign and the expansion of the multidisciplinary workforce. The MoU sets out agreed principles of service reconfiguration (including patient safety and person-centred care), ring-fenced resources to enable the changes to happen, new national and local oversight arrangements, and agreed priorities over the 3-year period 2018-2021. Locally agreed Primary Care Improvement Plans (PCIPs), produced for the first time in summer 2018, outline how Integration Authorities, working with their partners, will deliver the aims of the MoU.
These changes are part of wider ongoing reforms to primary care in Scotland. This includes the removal of the Quality and Outcome Framework (QOF) and the establishment of Improving Together,[10] a national quality improvement framework to support the work of GP Clusters. The Transforming Roles Programme[11] is ensuring nationally consistent, sustainable and progressive roles, education and career pathways for nurses, supported by investment in additional training and continuous professional development. There has been considerable investment in testing new models of care and improvement in every territorial Health Board in Scotland, with the Scottish School of Primary Care (SSPC) tasked with capturing key learning from tests funded by the Scottish Government. Innovative models are also being tested in our national boards (particularly the Scottish Ambulance Service and NHS24) to improve patient outcomes. Developing the analytical, digital and physical infrastructure in primary care to help facilitate wider reforms continues to be a key long-term strategic priority.
Recently, “The Review of Progress with Integration of Health and Social Care”,[12] conducted under the auspices of the Ministerial Strategic Group for Health and Community Care, was published on 4 February 2019. It includes a commitment to develop a framework for community-based health and social care integrated services, including primary care services. The framework will be key in identifying and promoting best practice in local systems to clearly illustrate what “good” looks like in community settings, with a firm focus on improving outcomes for people. The Scottish Government and COSLA will lead this work, involving Chief Officers and other partnership staff to inform the framework.
All these developments sit within a dynamic context of: Health and Social Care Integration and the 2020 Vision to shift the balance of care from secondary to primary and community care settings;[13] “The National Clinical Strategy”[14] and Realistic Medicine;[15] Scotland’s “Digital Health and Care Strategy”;[16] continued public sector financial challenges; increased demand arising from demographic change and more complex clinical cases; workforce pressures; and evolving clinical practice. It is also essential to see the reform of primary care within the context of “the Scottish Approach” to designing and delivering public policy and services.
Contact
Email: socialresearch@gov.scot