A National Clinical Strategy for Scotland
The Strategy makes proposals for how clinical services need to change in order to provide sustainable health and social care services fit for the future.
2. Introduction: Why Do We Need to Change ?
The current direction of travel for NHSScotland has been set out by two documents.
The Healthcare Quality Strategy for NHSScotland, set out an ambitious approach to ensure that the National Health Service in Scotland could become one of the best health services in the world, with a world leading approach to patient safety, and more recently, a determined approach to deliver person centred care. The aspirations of the Quality Strategy remain central to the day to day work of the Health Service.
More recently, the Scottish Government set out the 2020 Vision, a high level description of the direction to be taken by the NHS in Scotland.
Our vision is that by 2020 everyone is able to live longer healthier lives at home or in a homely setting. We will have a healthcare system where we have integrated health and social care, a focus on prevention, anticipation and supported self-management. When hospital treatment is required and cannot be provided in a community setting, day case treatment will be the norm. Whatever the setting, care will be provided to the highest standards of quality and safety, with the person at the centre of all decisions. There will be a focus on ensuring that people get back to their home or community environment as soon as appropriate, with minimal risk of re-admission.
"The 2020 Vision." Scottish Government 2010
While this remains the central vision for the Health Service in Scotland, we need to change so our health and care system can deliver it, adapting to changing demands and opportunities, and ensuring sustainability. Without adapting and improving we will not be able to realise the potential of providing world-class care. The challenges we face are seen throughout much of the developed world, and countries are trying to adapt healthcare services so that they maintain a comprehensive supply of high quality healthcare in the face of steadily increasing demand. The ability to sustain services that are able to meet the increased demand effectively will be a key challenge for maintaining the delivery of high quality healthcare in the future.
Although this strategy argues the case for change, it considers only the delivery of clinical services and how they can be planned to deliver the best possible outcomes for patients. It is acknowledged that there is a need to improve the health of the Scottish population, by the development of a range of measures designed to address the determinants of poor health - lifestyle, educational, economic, employment, environmental determinants. The absence of discussion of these approaches does not reduce in any way the need for continuing the progress that has been made in recent years.
In setting out a National Clinical Strategy it is acknowledged that there are many challenges facing healthcare services in Scotland. These challenges are substantial, and thus it is essential that any Clinical Strategy is ambitious and visionary and sets out challenging but deliverable aspirations for a transformed future health service.
There are multiple reasons why we need to evolve and adapt in the face of changing circumstances. For any organisation, failure to adapt successfully to both external and internal challenges will result in an increased risk of failing to comprehensively meet the objectives of that organisation. The main drivers for change are discussed in this section. It is important to detail these at some length as a failure to understand the drivers for change will mean that change, which is always difficult, will not come about, and we will fail to be a world-class health service.
The main drivers for change are:
a) Demographic changes in our population
b) The changing patterns of illness and disability
c) The relatively poor health of the population and persisting inequalities in health
d) The need to balance health and social care according to need
e) The need to manage the skilled workforce in a way that makes best uses of their skills, allows further changes in roles, and provides sustainable services despite the current recruitment challenges
f) Financial considerations
g) Developments of new treatments
h) Remote and rural challenges
i) Opportunities from increasing, better, and more joined up use of Information Technology
j) Reducing waste, avoidable harm and variations in treatment.
In discussing these drivers it is important to recognise, above all, the overriding need to maintain and enhance the quality of care, and the outcomes that care provides for our population.
A. Demographic Changes in Our Population
Although Scotland lags behind some other European countries, life expectancy has been steadily increasing. This is of course welcome, and is a measure of both healthier lifestyles and improved clinical care. However, the significant consequence is that the average age of the population and the percentage of older people is increasing, and looks likely to continue to do so until at least 2030.
Current projections suggest that the population of Scotland will rise to 5.78 million by 2037, and that the population will age significantly, with the number of people aged 65 and over increasing by 59%, from 0.93 million to 1.47 million. The number of households headed by people aged 65 and over is projected to increase by almost 54% between 2012 and 2037. In contrast, households headed by someone aged under 65 are projected to increase by just 3%. The number of households headed by someone aged 85 and over is projected to more than double over the same period, from 77,400 to just over 200,000.
Estimated and projected age structure of the Scottish population, mid-2012 and mid-2037
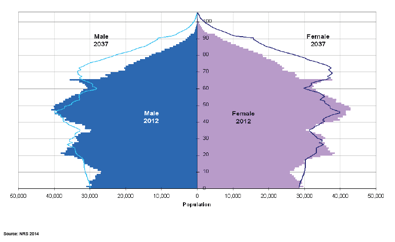
Whilst an older population will require more healthcare, it is possible to point to recent changes that have altered the rates of need for treatment. For example the rate of hip fracture per thousand of the population over 65 seems to be decreasing, although because of the absolute increase in the population over the age of 65, the actual number of hip fractures is increasing and is likely to continue to do so. Likewise the rate of bed day use per 1,000 of the population over the age of 75 has decreased significantly (primarily due to reduced average length of stay) from 5,421 in 2009/10 to 4,815 in 2013/14 - a reduction of 11%. Inevitably, however, this falling rate is challenged by the increasing absolute number of the population over the age of 75.
The impact of the increasing age of the population can be demonstrated by considering two particular conditions: dementia and cancer.
Dementia
The increasing prevalence of dementia in an older population will have considerable consequences for the volume and type of health and social care that is required for the future. People with dementia have the greatest likelihood of using high cost unscheduled hospital care for extended periods of time.
A recent estimate carried out by Alzheimer Scotland suggests that there were 89,000 people with dementia in Scotland in 2013. Of that number, between 50-65% have a formal diagnosis (depending on which prevalence model is applied). Approximately 3,200 are under the age of 65. The rates of dementia are strongly related to age. There is evidence that the true prevalence, rather than the number of cases actually identified and diagnosed, at age 65-69 is around 1.8% in men and 1.4% in women. The prevalence increases rapidly so that 20.9% of men aged 85-89 have dementia, with around 28.5% of women of the same age having the condition. While the majority of people with dementia manage to live at home, with input from relatives and informal carers, the disease is steadily progressive and it is almost inevitable that health and social services will require to provide significant input as the illness progresses. The figures above indicate how the scale of the problem will increase as the proportion of older people in the population increases.
Cancer
Over the last ten years, age-standardised incidence rates of cancer in Scotland have fallen by 4% in males but increased by 7% in females. However, excluding non-melanoma skin cancers, the actual number of cancers diagnosed in Scotland has increased over the last 10 years from 27,095 cases in 2003 to 31,013 in 2013. This is likely to be largely due to an ageing population.
It is estimated that up to one in two people in Scotland will be diagnosed with some form of cancer during their lifetime. This does however include cancers that will have no detrimental impact on life expectancy, such as indolent prostate tumours. It is estimated that there are 176,000 people in Scotland who have been diagnosed with cancer over the last 20 years and who are still alive. This is approximately 3% of the population of Scotland.
New cancer registrations in Scotland, 1989-2013: number of cases and age standardised rate (European Age Standardised Rate - using ESP20132)
Figure 3. New cancer1 registrations in Scotland, 1989-2013: number of cases and age standardised rate2 (European Age Standardised Rate - using ESP20132)
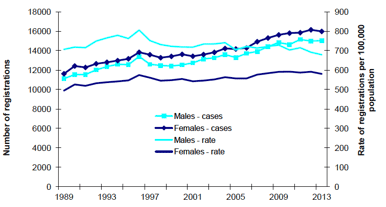
Source: Scottish Cancer Registry
1 All cancers excluding non-melanoma skin cancers (ICD-10 C00-C97 excl C44)
2 The European Standard Population (ESP), which was first used in 1976, was revised in 2013. Figures using ESP1976 and ESP2013 are not comparable. The European Age Standardised Rate (EASR) is calculated using ESP2013 and 5 year age groups 0-4, 5-9 up to an upper age group of 90+.
This increased incidence, and increased prevalence, will have a very significant impact on the services that we will be required to deliver in the future. Medical technology has developed significantly, and recurrences of cancer are now treated more aggressively (and more successfully) than before. These increases in demand, along with the rapidly changing range of investigations and treatments as we develop greater understanding of cancer treatment, means that we must have a service that is able to adapt promptly to developing technology. The careful scrutiny of treatment developments, the development of an evidence base, and the need to adapt to changing treatments requires ongoing planning of cancer services across the population. The next steps will be outlined in a cancer plan to be published in Spring 2016.
These two examples indicate how we will need to build capacity in both our social care and healthcare services to meet the increasing demands that will develop as our population grows older. These changes will require us to adapt current health and care services so that they are aligned to address the burden of ill-health in our population. We will need to focus on preventing illness, delaying progression or exacerbations, supporting self-management where appropriate, and providing health and social care safely, effectively, equitably and sustainably, aiming to return people to a state of maximum health and independence for as long as possible.
B. The Changing Patterns of Illness and Disability
It has been recognised for at least the last 50 years that the pattern of illness experienced by the Scottish population has changed significantly from acute life-threatening illnesses, towards long-term conditions and disability.
In 2014, 46% of adults had one or more long-term conditions. The prevalence of long-term conditions increased with age, from a quarter (25%) of adults aged 16-24 to three-quarters (77%) of those aged 75 and over[1]. Long-term conditions are generally defined as conditions that have been present for at least 1 year and are unlikely to be cured. The significance of long-term conditions is that they are very likely to persist for the rest of the individual's life, resulting in ongoing need to manage the condition or conditions.
A significant number of long-term conditions are preventable with appropriate lifestyle choices, indicating the need in Scotland for continued work on influencing changes in lifestyle choices and thereby developing a healthier population for the future.
Long-term Conditions:
- People with long-term conditions are twice as likely to be admitted to hospital and will stay in hospital disproportionately longer than people without them.
- Account for over 60% of hospital bed days used.
- Most people who need long-term residential care have complex needs from multiple long-term conditions.
- People living with long-term conditions are also more likely to experience psychological problems.
- People living with a long-term condition are likely to be more disadvantaged across a range of social indicators, including employment, educational opportunities, home ownership and income. Someone living in a disadvantaged area is more than twice as likely to have a long-term condition as someone living in an affluent area, is more likely to be admitted to hospital because of their condition, and will be more likely to develop the long-term illness at an earlier age - a difference of as much as 10 years.
ISD
Longstanding illness by Scottish Index of Multiple Deprivation (SIMD) quintiles, 2014
| Type of longstanding illness | SIMD 2012 quintiles | ||||
|---|---|---|---|---|---|
| Least deprived | 2 | 3 | 4 | Most deprived | |
| Neoplasms & benign growths | 2% | 2% | 3% | 2% | 3% |
| Endocrine & metabolic | 9% | 7% | 11% | 10% | 11% |
| Mental disorder | 6% | 6% | 7% | 8% | 15% |
| Nervous System | 4% | 4% | 5% | 5% | 5% |
| Eye complaint | 2% | 1% | 2% | 3% | 2% |
| Ear complaint | 1% | 1% | 2% | 1% | 2% |
| Heart & circulatory system | 11% | 10% | 14% | 13% | 17% |
| Respiratory system | 7% | 7% | 8% | 10% | 11% |
| Digestive system | 4% | 5% | 6% | 6% | 8% |
| Genito-urinary system | 2% | 3% | 2% | 3% | 2% |
| Skin complaint | 1% | 2% | 3% | 2% | 2% |
| Musculoskeletal system | 15% | 14% | 17% | 20% | 23% |
| Infectious Disease | 0% | 0% | - | 0% | 0% |
| Blood & related organ | 1% | - | 1% | 1% | 1% |
| Other complaint | 0% | 1% | 0% | 1% | 0% |
| No longer present | - | 0% | 0% | - | - |
| Any longstanding illness | 42% | 41% | 46% | 50% | 55% |
Source: Scottish Health Survey
It should be recognised that although long-term conditions are often thought to be associated with older age, the absolute number of long-term conditions experienced by the under 65s in the population is greater. The clinical significance of long-term conditions is very varied, ranging from illness that can be considered more of a risk factor (such as hypertension and osteoporosis) to those that cause increasing disability (such as osteoarthritis, chronic obstructive pulmonary disease, heart failure, macular degeneration and hearing loss). While it is possible to provide secondary prevention to reduce the rate of progression of many long-term illnesses, and to decrease the episodes of exacerbations, the combined impact of multiple long-term conditions is to cause a progressive, cumulative disability that severely threatens the quality of life, and creates a need for greater and greater social support. While it is recognised that, overall, the majority of the support is provided by family and other carers, it is inevitable that there will be an increasing demand on health and social care services.
It is essential to recognise that the accumulation of long-term conditions and related disability results in increasing needs that may be complex, and may require social care and support more than clinical solutions. This has been one of the main drivers behind the recent integration of health and social care across Scotland - to ensure that people in need have appropriate help that addresses their needs - which may not be predominantly medical.
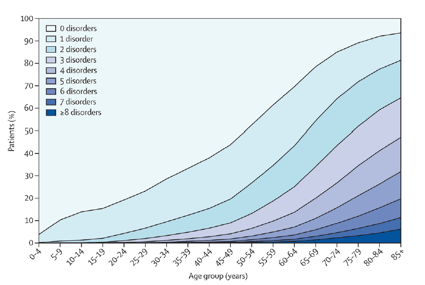
Source: Barnett et al, The Lancet 2012; 380: 37-43
The chart above shows how there are increasing numbers of long-term conditions found in older people. The accumulation of multiple long-term conditions results in progressive loss of independence and increasing need for social support.
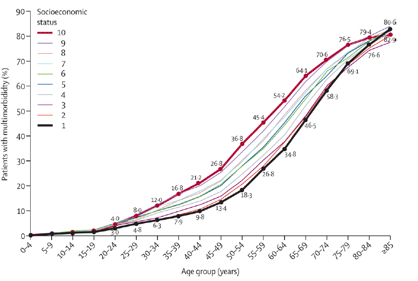
Source: Barnett et al, The Lancet 2012; 380: 37-43
This chart shows how the population that is most deprived develops long-term conditions at an earlier age - developing long-term conditions up to 10 years earlier than the least deprived.
In conclusion, the increasing prevalence of long-term conditions, and the complex needs that arise from multiple long-terms conditions will drive increasing demand for health and social care for the foreseeable future. The fact that there will be more people with multiple conditions in future means that clinicians will increasingly need to work in teams across specialisms and will need to be supported in that by improved information exchange and clinical decision support systems.
C. The Relatively Poor Health of the Population and Persisting Inequalities in Health
While the health of the Scottish population is improving, and life expectancy has also improved, we lag behind some other European countries across a wide range of population health measures, including dental and oral health. This alone makes the case for renewed efforts to have a comprehensive public health approach across all sectors of Government (and the third sector) as many of the long-term conditions described above can be significantly reduced by improvements in lifestyle, education, wealth, employment, environment, social cohesion and mental wellbeing.
This clinical strategy does not focus on the prevention of ill-health, but that does not in any way indicate a lack of importance of public health initiatives. As well as the obvious benefits to individuals, they can be shown to effectively reduce demand for healthcare. This has been evidenced, for example, by the significant improvements brought about already by the nursery school tooth brushing campaign, which has substantially reduced dental decay and the need for fillings and extractions.
The use of the rotavirus immunisation in children has dramatically reduced the incidence of diarrhoea and vomiting, and thus reduced the number of admissions to hospital. The ban on smoking in public places is bringing about an increased reduction in the number of smokers, which will impact on the demand for many aspects of healthcare.
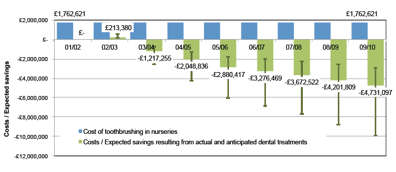
The chart above shows how the investment of £1.7 million annually on a toothbrushing campaign in Nursery Schools has led to a significant drop in the need for fillings and extractions - showing improvements for patients, and reduction in overall costs.
Although a relatively crude measure of health inequalities, the inequalities across Scotland can be demonstrated by consideration of life expectancy, and healthy life expectancy.
Life expectancy (LE) is an estimate of how many years a person might be expected to live, whereas healthy life expectancy (HLE) is an estimate of how many years they might live in a "healthy" state. HLE is a key summary measure of a population's health.
- The most recent annual estimates for Scotland are for boys born in 2013 to live 77.1 years on average, 60.8 of these in a "healthy" state. Girls born in 2013 would be expected to live 81.1 years on average, 61.9 of these years being "healthy".
- Underlying trends in both LE and HLE at birth show a general improvement in Scotland over recent years.
- The gap between LE and HLE (the years expected to be spent in a "not healthy" state during the average lifetime) has been fairly constant for females between 1980 and 2008, but tended to increase for males.
- There are considerable variations in LE and HLE at birth in Scotland among different geographical and socio-economic groupings. Men living in the most affluent parts of Scotland can expect to live 10 years longer than those in the most deprived areas. Differences in healthy life expectancy are even starker with a gap of 20 years for men living in the most and least deprived areas. As shown in the table below, even the most advantaged section of the population can anticipate a significant period of "Ill health" - with the most disadvantaged likely to experience approximately twice the number of years of ill health:
| |
Males - Least deprived | Males - Most deprived | Female - Least deprived | Female - Most deprived |
|---|---|---|---|---|
| Life Expectancy (years) | 81.7 | 71.3 | 84 | 77.2 |
| Healthy Life expectancy (years) | 69.1 | 48.3 | 71.9 | 51.5 |
| Expected years of "Ill health" | 12.6 | 23 | 12.1 | 25.7 |
Source: ISD
- LE is significantly worse (lower) in Scotland than in the UK as a whole, for both males and females. HLE is significantly worse (lower) in Scotland than in the UK for males, but similar for females.
- Scotland has one of the lowest LEs in Western Europe. International comparisons of HLE are hampered by the lack of consistent health measures. However, on the basis of a related indicator, healthy life years (HLY), it would appear that, in comparison with many European countries, Scotland fares badly for males but compares better for females[2].
D. The Need to Balance Health and Social Care According to Need
As referred to above, the development of multiple long-term conditions leads to increasing loss of independence, and the development of complex needs that cannot be met solely by health services. For many older people who have increased restrictions on their life, perhaps from combinations of multiple long-term conditions such as sensory loss, poor mobility, chronic pain, social isolation and mental health issues, the need for rehabilitation, social support and integration into local communities may have greater immediate importance to them than the provision of medical care. The implementation of Health and Social Care Integration will mean that we are better placed to ensure that there is an appropriate balance between health and social care services. This is important to prevent health services being used as the "default" when social support might be more appropriate (as happens with a number of avoidable hospital admissions, particularly in older people).
Admissions to hospital
Analysis of admission trends show that across most age groups, the rate of admission to hospital is relatively steady. However in the over 75s, and particularly in the over 85s, the number of admissions is driven by an increasing rate of admissions in those age groups, along with the increasing numbers of patients in these age groups. There is evidence from across health and social care that, for many of our older people, admission to an acute hospital is too often the fall-back option, when it is possible that their needs could have been satisfactorily met by enhanced support and care input within their home and community. This is important. Not only does avoidance of admission, where possible, provide a service that is preferable to most people, it can be associated with less unintended harm from treatment, less confusion and dependency, and, of course, less need to continue to increase capacity in our hospitals over the coming years.
| |
2011 | 2012 | 2013 | 2014 |
|---|---|---|---|---|
| Emergency inpatient discharge | 534,178 | 547,673 | 551,524 | 554,893 |
| Routine inpatient discharge | 447,989 | 448,263 | 469,543 | 518,743 |
| Day case discharge | 443,109 | 453,520 | 459,919 | 451,281 |
Source: ISD Scottish Hospital Activity
The steady rise in unscheduled admissions shown in the table above is likely to continue unless health and social care systems adapt. The rate of unscheduled admissions in the elderly population will increase most. Currently admissions in this group of patients are partially driven by a lack of health and care services in the community that are able to rapidly escalate the levels of care during an exacerbation of illness to maintain them in their homes.
There is evidence from a range of settings that it is possible to treat a proportion of these people in their homes, and provide similar outcomes, with a better experience, and less impact on their independence than if they are admitted to hospital.
Hospital discharge
The ability to discharge people from hospital can be delayed by an inability to promptly organise suitable support packages for them, resulting in a worse experience for the individual, the potential for further loss(es) of function, delays in admitting other patients, pressures within hospital systems and increased but potentially avoidable use of resources within acute hospitals.
We are committed in Scotland to tackling delays in discharging people from acute hospital beds - a key driver for integrating health and social care. Delayed discharges in this context are defined as patients who are still in hospital more than two weeks after they have been declared medically fit for discharge. In the census in October 2015 there were approximately 1,280 such patients. This figure is a reduction of 7% from the same time the preceding year. However the Information Services Division notes that in September 2015, a total of 48,000 bed days were used by patients whose discharge had been delayed. Again this is an improvement on the situation from the preceding year, with an 8% drop. However, this figure suggests that on average, 1,578 beds across Scotland are occupied by patients who are clinically ready to leave hospital. This figure suggests that there is very considerable potential to relieve pressure on hospitals by continuing the improvement in addressing discharge delay. It must be considered an urgent priority to ensure that any barriers to discharge for these patients are removed and support provided for them to leave hospital. This improves their experience of healthcare, and also potentially frees up resources (beds and staff) for use by other patients in need.
We also know that the vast majority of people, if asked, declare a desire to die at home. Currently in Scotland over 50% of deaths occur in hospital, and people may (though by no means always) experience a depersonalised death that is distressing for them and their relatives. We need to ensure that we have the capacity to support individuals and their families to stay in their own homes, or return to them when this is their explicit wish.
The conclusion from this section is that we know it is better for people to be supported to stay in their own homes and communities for as long as possible, as independently as possible. We also know that demand for inpatient hospital care will increase significantly to an unsustainable level unless we fundamentally shift the balance of care from acute hospital services to comprehensive and responsive primary, community and social care services, along with comprehensive approaches to improving public health and the ability of patients to self-manage their long-term conditions.
There is a need to prioritise investment carefully to optimise the effectiveness of services. In order to improve outcomes and reduce the pressure of unscheduled admissions to hospital, it will be necessary to appropriately prioritise investment in primary health and social care to allow alternatives to admission to be developed where it is clinically appropriate to do so. This may include investment in hospital-based services that could reach out to communities - such as community facing geriatricians.
However, the increased proportion of older persons in the population will result in an increase in the need for a range of procedures - especially those that are age-related, such as cataract removal and joint replacement. Demand assessment for these operations has been carried out, as a result of which the Scottish Government has allocated £200 million over the next 5 years to increase elective capacity across the country, particularly where population projections suggest most need. Evidence from the Golden Jubilee National Hospital shows that a concentration of high volume procedures results in lower complication rates, reduced length of stay, and effective, standardised care.
E. Workforce Issues
A sustainable health workforce which is motivated, adaptable and highly trained is crucial to delivering high quality healthcare in the changing health landscape and to meet our vision for health and social care by 2020 and beyond.
While the total NHS workforce has grown to an all-time high of 161,000[3](138,000 WTE), that in itself will not meet the challenges we face such as increasing demand for healthcare. We need to do more to maximise the contribution from the whole healthcare workforce, and be prepared to change the way we deliver services.
We do not underestimate the challenge these changes will mean for our workforce. Through Everyone Matters[4] the Scottish Government set out a clear workforce vision and plan which was co-produced with NHS staff. We will support our workforce to make those changes through the priority areas identified in that plan. These are:
- Healthy organisational culture
- Sustainable workforce
- Capable workforce
- Workforce to deliver integrated service
- Effective leadership management.
Alongside the strong partnership working approach that is well established in NHSScotland, this collaborative approach will be vital in creating the sustainable workforce we need for the future.
Challenges
In common with many healthcare systems in the developed world, NHSScotland faces a challenge in maintaining a suitably trained workforce over the next 5-10 years. For certain professions and in certain regions, it can be extremely difficult to recruit the right staff in the right quantities. International shortages of key specialties are by their nature difficult to address in a Scottish context alone. Adding to these challenges are the differing roles played by Scottish Government and NHS Boards; the complex interactions around workforce planning; and individual circumstances applying to professional groups, service plans and policy development. We also need to bear in mind that the medical workforce in particular has an older age profile than most other employment sectors, and it is likely that a higher proportion of those over 55 may choose to retire over the next few years.
Self-evidently, gaps in the medical training establishment and workforce are likely to adversely affect the quality and sustainability of services provided to patients. Within the medical workforce, gaps in particular specialties and in particular areas could create risk to the sustainability of services. Using expensive alternatives such as locums can help address the current needs of the service, but in a way that is unsustainable, and a poor use of resources. It also demonstrates the need to better match our workforce capacity to overall demand in a sustainable and affordable way which anticipates the challenges for healthcare in the future.
In addition gaps in the workforce among care workers make it difficult to start care packages timeously, with the result that patients remain in hospital after they have been determined to be fit to be discharged from hospital. As we move to integration of health and social care, it is important that we plan for the wider workforce employed across health and social care, ensuring that the important contribution of care staff is recognised, and that these roles are as attractive as possible for potential care workers.
Achieving the right balance
Securing the right workforce within the clinical environment, and balancing this against the diverse needs of patients can be extremely difficult. Complex illnesses, and the pace of change in technology may mean patients require specialised staff who can provide the highest quality high technology care available when such specialised intervention is required. However, patients with multiple conditions may need clinicians with broader based skills who can provide more generalist care.
This complex and almost infinitely variable clinical environment means that there is no one solution to the challenge of sustainability. However we do know that too much medical specialisation has often led to disjointed, disease-focussed care for patients with multiple conditions, often provided within hospital rather than community settings, and frequently requiring referral to multiple specialists. The tension between specialist and generalist approaches applies particularly to doctors (and was recognised by the Greenaway Report on the training of doctors in the UK[5]).
It is right that Scotland should make a full contribution to UK-wide developments on medical training. But we also seek to achieve an optimum balance for Scotland - though broadly in favour of more generalist approaches - through the Shape of Training Transitions Group, which is best placed to respond to challenges of sustainability - if necessary, by making adjustments to medical training intakes.
Although there is a demonstrable need for doctors of all roles to have a wider generalist approach (to match the multiple combinations of illnesses in their patients) we argue in this strategy for services to be planned across populations, with specialised centres for complex interventions, staffed by clinicians with specialist skills. There will be considerable planning and judgement required to develop a sustainable balance of medical, and wider clinical, workforce to provide the best possible outcomes across all ranges of complexity.
What we expect
Our expectations in Scotland are that, regardless of which profession is delivering high quality services in our NHS, it should:
- Combine generalist as well as specialist skills
- Work effectively in teams
- Value the contribution of all disciplines to addressing patient needs
- Have excellent generic skills, such as listening, communication, leadership and improvement skills
- Engage in life-long learning, recognising the pace of change in health and social care
- Remain flexible, able to adapt to changing technology and patient need.
Building our approach to sustainability and risk
To deliver a sustainable workforce supply we need to ensure sufficient supply into training, maintain those numbers through the pathway of training and retain a high proportion of those qualified staff within NHSScotland, as well as attracting high quality staff from elsewhere.
Even relatively few gaps in supply can create significant service challenges for Boards, particularly if compounded by difficulties in recruiting suitably skilled short-term locum cover. So maintaining that supply, and using the supply in the most effective ways, is a key area of focus for now and the future to mitigate those risks.
At the same time, making fundamental changes to ensure the delivery of high quality services in future, will mean using our understanding of risk to improve and develop more sensitive models of supply and demand, with gap analysis providing risk-based intelligence which informs recruitment decisions and education requirements.
Much positive work is already being done with NHS Boards and others to obtain better intelligence about why and where vacancies occur in order to improve consistency in Board reporting of vacancies, which will:
- inform more effective workforce planning
- further develop and use mandated workload and workforce planning tools
- improve data in areas such as midwifery, neonatal nursing and community nursing
- aid profiling the GP and consultant workforces so there is a consistent evidence base to underpin decisions on future numbers.
We are extending this work into health and social care integration to develop common datasets where that is appropriate, to ensure Integration Joint Boards are fully equipped to plan and provide integrated services across Scotland.
While we need to accelerate this work, we are not starting from a zero baseline. In medicine, supply and demand issues in the education and training pathway are particularly complex and planning for future service need is challenging given the duration of medical training (a minimum of 10 years for GPs and 15 years for hospital specialists). We are developing an increasingly sophisticated understanding of supply and demand issues and other factors influencing the choices made by medical undergraduates and junior doctors, which is enabling us to target increases for particular specialties. We recently announced an increase of 100 in GP specialty training places and an enhancement of the GP returners scheme to encourage GPs who are not currently working in NHSScotland back into the service. In addition we are working with our universities on a number of actions that will increase the number of medical undergraduates and broaden the range of people entering medical education to ensure that all of our young people have the opportunity to develop their skills through a career in NHSScotland.
Transforming roles
As demand for health services increases, we need to ensure future models of service delivery and workforce configuration are optimal. Ensuring a sustainable workforce means maximising the contribution of all healthcare professions, so that our staff work at the top of their professional capability, but without adding to a loss of continuity of care or increasing the complexity of care. It means further investment in a mixed economy workforce, and crucially, it means transforming roles so they are of more direct benefit to Scotland's NHS patients in different healthcare settings. For example, further training allows experienced nurses to deliver advanced practice; pharmacists with extended roles can provide care, especially for patients with long-term conditions; allied health professionals can develop increased skills to deliver professional care autonomously; and physician associates are a recent and welcome addition to multidisciplinary clinical teams. The primary care workforce is the one which we most need to develop and grow in order to achieve the capacity and workforce transformation that is required, and specific reference is made to that later in this chapter.
Our ultimate aim remains to have sufficient numbers of the right staff in the right location with appropriate skills, delivering patient care of the highest possible quality. Much excellent healthcare is already delivered by multidisciplinary teams. This has been shown to be highly productive and delivers safe and effective care with improved outcomes for patients. We will continue to build on this model going forward.
General practice
The number of GP vacancies within independent contractor practices is difficult to define precisely, though ISD collects data on numbers of GPs, and the biennial Primary Care Workforce Survey is underway. There is however considerable evidence of a significant recruitment challenge in general practice across Scotland, with some areas finding it more difficult to recruit than others. This has had multiple impacts, including a number of practices relinquishing their contracts, requiring Health Boards to deliver a directly managed GP service for a period of time until new arrangements are put in place.
The sustainability of the GP workforce continues to be affected by the existing short-fall in GP numbers, the trend towards flexible working, the high proportion of GPs over the age of 55 who are likely to retire in the next five years and the fact that GP specialty training places are difficult to fill. These issues are common across the whole UK.
The Scottish Government is taking measures to increase the supply of newly trained GPs, with the recent announcement of an extra 100 GP training posts across Scotland from August 2016. This potential increase in capacity is accompanied by renegotiation of the GMS (GP) contract (due to be implemented from April 2017) which will provide a role and career structure that is more attractive.
Concerted action is also needed to make GP careers more attractive, and there are a number of actions which are being considered or are already in train to address this. These include giving medical students the opportunity to spend more of their training in primary and community care settings, presenting a more positive view of general practice, and extending the range of career opportunities for GPs. Such opportunities include the new one year GP fellowship to provide them with the enhanced skills to work in the new community-based models.
The renegotiation of the GP contract is a key enabler to increase the attractiveness of the profession, removing bureaucracy and enabling GPs to spend more time on the type of patient care that provides the greatest benefits to patients, whilst providing higher levels of job satisfaction to the doctors.
For the future, general practice will require a different approach. The role of the GP will evolve to be the expert medical generalist, working with larger teams, and supported by a wider multi-professional team able to deliver much greater clinical care, working in a way that utilises their particular skills. The impact of the clinical team will be enhanced by collaborative working with social care staff, and increasingly by signposting patients to third sector organisations that provide significant community-based support for patients.
The development of the wider primary care team will be trialled in a number of areas through new ways of working. Important issues to be determined by the trialling of newer models will include how continuity of care for patients can be optimised in wider teams, and how the increased range of professionals can be integrated to work with the existing practice-based structure of primary care.
The development of a highly skilled and effective mix of professionals in primary care will require development of targeted training for nurses, pharmacists and allied health care professionals, so that they are able to develop the extended roles that will be required to practice more autonomously in the primary/community care services of the future.
It will be important for primary care professionals to be prepared to offer some basic training to relevant social care staff, with particular emphasis on what developments with a client should prompt contact with a healthcare professional.
The provision of an appropriate level of support for patients in the community (aiming to help rehabilitation and re-enablement) requires a continuing expansion of the primary care workforce. This will be a central role of the newly formed Integration Joint Boards. However, given the resource constraints, it is likely that a shift from investing in hospital care will be required, with a more significant move to investment in primary and community care.
Conclusions
Healthcare will increasingly be delivered by teams of professionals united by common professional values, with effective clinical leadership.
Recognising the current and future challenges in recruitment of highly skilled staff, we need to continue planning of training and recruitment for all types of clinicians to ensure that we can have the capacity to deliver the services that will be required in the future. Enhanced capacity has to be planned early to deliver the health and social care workforce that will be required in the future, particularly given that training for some professionals takes years. A new GP contract must provide a professionally satisfying career path to attract a greater proportion of doctors into primary care.
However, increasing the numbers of staff alone will be insufficient. We have the potential to deliver care in different, and potentially better ways, by fully utilising the many skills found across the wide range of disciplines (supported in some settings by innovative use of digital technology). NHSScotland has already invested significantly in a mixed economy workforce and recognises the benefit of new roles in the healthcare setting but also recognises the need to do more.
The workforce challenges we describe are not exclusive to NHSScotland and dealing with them requires action by individuals, Health Boards and other bodies and Government. This should reflect our particular circumstances and build on our well established models of collaboration and partnership working.
F. Financial considerations
This is a clinical strategy which provides the rationale for change in the delivery of high quality and sustainable clinical services. To be successful it must also be underpinned by a sustainable financial strategy, with a primary focus on the value of healthcare services.
Value-based healthcare is an established approach to improving healthcare systems across the world - the central argument is that higher value healthcare is not necessarily provided by higher inputs. What matters more is that care is provided early in disease to prevent progression (avoiding the added patient burden of more intensive interventions), it is provided safely to avoid harm, it is proportionate to the patient's needs (avoiding the waste of providing outcomes that are not relevant to the patient), it is provided consistently and reliably (avoiding unwarranted variation).
Looking ahead, there are various issues that will specifically impact on the health resources available:
- The estimated annual percentage change in the volume of demand for healthcare (and cost) as a result of anticipated demographic changes over the period to 2030, and increased life expectancy, is projected to be at least one per cent per annum. In the absence of change, this equates to an increase of up to £120 million per year.
- The projections for increased costs of medicines suggest a further 5-10% increase on current spending per year.
- Staff costs are approximately 65% of total costs, and are projected to continue to rise as a result of pay structures, National Insurance and Pension changes.
This all requires to be delivered within the context of the toughest public expenditure conditions we have faced. The Scottish Government's discretionary budget will be around 12% lower in real terms in 2019-20 than it was in 2010-11. Despite this pressure, health spending continues to be protected, with health resource spending in Scotland set to rise to a record level of £12.4 billion in 2016-17.
Scottish Government Health Resource Spending
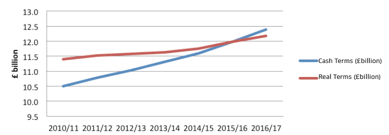
Source: Scotland's Spending Plans and Draft Budget 2016-17, Scottish Government, December 2015
Investments in 2016-17 include: £250 million investment to be directed to health and social care partnerships, to ensure improved outcomes in social care; £45 million improvements to primary and community care, to support the development of new models of care; and £200 million over the next five years for the development of a new network of diagnostic and treatment centres, enabling faster treatment and addressing demographic pressures.
This strategy is primarily about improving the value delivered by, and from, health services. Improving value by providing reliable care that is proportionate to need, is safe, effective, person centred and sustainable will increase value for patients, and is likely to stabilise costs.
Evidence shows that the relationship between healthcare expenditure and health outcomes is non-linear. If it were, any additional euro spent on healthcare would result in a corresponding improvement in the population's health status (measured, for instance, in terms of healthy life expectancy). In reality, the greater the expenditure, the lower the marginal improvement in health status as a result of its increase.
Countries also vary significantly in their ability to translate a similar level of resources into health outcomes.
International comparisons show that the same amount of per capita healthcare expenditure can be associated with very different health outcomes even after taking into account the differences in lifestyle and socio-economic realities among countries. It is not only how much money is spent, but also how it is spent, that determines a country's health status. Present budget constraints should therefore be used as an opportunity to improve the value and effectiveness of healthcare spending.
"Investing in health" European Commission Staff Working Document: Feb 2013
G. Changes in the Range of Possible Medical Treatments
The pace of change as a result of medical advances is considerable. It is not just the change in the actual treatment that will alter the services that we can offer, it is change in the way that services are delivered, and challenges to accepted practice. For example, 10 years ago it was considered normal and acceptable for patients to remain in hospital for up to 10 days after hip replacement. Since then, work has been done to reduce the physiological impact of anaesthesia and operation, and speed recovery. Progressive work has shown that better outcomes can be obtained with a concerted effort to reduce length of stay, and it is now not unusual for patients to be discharged within 48 hours of hip replacement. Likewise there has been a continuing increase in the amount of day-case surgery, and, especially in gynaecology, a significant move to provide traditional day-case care in outpatient clinics - improving the service to patients, maintaining or improving outcomes and providing a higher value service at less cost.
Scientific advances will continue to provide the means to improve outcomes, but many of these advances will come with considerable cost and complexity, and may require more total resource than the treatments they displace. We will need to ensure that we have a health service that assesses improvements in outcomes against increases in resource input, and is as efficient as possible, otherwise our ability to invest in future treatments may be constrained. There is evidence that some advances are only very slowly taken up across the Health Service. This natural conservatism with respect to new treatments can have benefits as there are examples of treatments that have been withdrawn after early experience has revealed previously unsuspected safety issues or unpredicted harms. However we need to ensure that new advances are taken up promptly across the whole of Scotland, especially if they result in significant increases in the value of treatment to patients, and improved outcomes, or reduced costs. The role that Healthcare Improvement Scotland has taken in this respect has ensured that cost-effective and proportionate use is made of new technology (for example, the consortium formed to advise on the use of the novel anti-coagulant agents) but there are further opportunities to improve decision making and treatments.
In summary, we need to ensure that any new developments in Scotland deliver proportionate improvement in value in relation to their costs. That value should always be related to patient experience and outcomes.
We should focus as much on different and better ways of delivering current services as we should on new technology and medicines. Medical and technical advances can be marginal in their impact; service improvement can be transformational.
We require a continuing national approach to support service improvements - as has been seen with the increased understanding of improvement science with the Scottish Patient Safety Programme. We require to support widespread clinical leadership - from multiple professions - to ensure that we have a Health Service that is rapidly able to adapt to changing technology, and better ways of delivering current services.
H. Remote and Rural Challenges to High Quality Healthcare
Scotland has a population of just over five million, and covers a vast area, much of which is sparsely populated. Rural Scotland accounts for 98% of the land mass and approximately 20% of our population live there[6]. A significant proportion of areas are remote from centres of significant population and thus physical access to services. Rural populations continue to grow at a faster rate than the rest of Scotland and have higher levels of older people, which increases demand for core services. Furthermore many rural households suffer from deprivation with "extreme fuel poor" rates around double of those elsewhere in Scotland.
The co-ordination and delivery of health and social care in remote and rural areas presents very significant challenges. There are insufficient populations to sustain specialist hospital services and distances and limited public transport links to acute hospital care can result in long travel times. This can lead to difficulties in providing high quality emergency care - issues which have been significantly addressed by the establishment of the flight based medical retrieval services.
There are other key ingredients to the provision of effective emergency care - the ability of well-trained local clinicians suitably equipped to respond rapidly to emergencies, and the ability to transport selected patients rapidly to definitive care. Due to the low rate of emergencies in sparsely populated remote locations, clinicians there may infrequently be called upon to provide emergency care, leading to reduction of any skills that have been acquired. For this reason, it is necessary to consider further development of remote clinician support from specialists so advice can be obtained rapidly via phone or internet, given the much broader range of skills required of clinicians in rural areas. This may augment the broad range of service initiatives that are found across rural Scotland - often based on local solutions using local resources and skilled healthcare professionals.
A number of innovative ways of delivering healthcare in rural areas are being developed and tested with Scottish Government support. Working with NHS Boards we are developing networks between rural and urban hospitals. These networks will support doctors working in rural areas to maintain and develop their skills - ensuring that patients receive safe care. In some areas this will involve rotating staff between rural and urban hospitals to ensure that we continue to provide services close to communities. This work has already delivered early success in supporting the delivery of general surgical services in Fort William's Belford Hospital. Working with NHS Highland, a network between Caithness General Hospital and Raigmore Hospital in Inverness is being put in place which will involve rotating staff between the two hospitals. This will support the delivery of the majority of surgical care and all out-patient care close to the community in Wick. The Scottish Government is also supporting an enhanced training programme for GPs who will be able to support the general medical services delivered in Caithness General.
Another initiative implemented by NHS Highland with SG support is 'Being Here', (2013-2016). This programme has explored new healthcare approaches to tackle challenges of primary care delivery in rural and remote areas. New multi-practice models for GP provision are being tested in West Lochaber, Isle of Islay, Mid Argyll and in Campbeltown for 24/7 care by the community hospital, local GPs and the Scottish Ambulance Service working together.
Remote rural practices face particular difficulties with mobile phone coverage and broadband connectivity - important given that there are more branch surgeries in rural areas. However, new technologies can create real opportunities in both treatments and access to services. Installing telehealth facilities in the 'Small Isles' Medical Practice on Eigg - with links with other islands being developed too - is enabling patients to access improved virtual face-to-face consultations remotely with their GPs. Support to encourage improved connectivity in rural areas has been identified as a priority by the Rural Parliament and is important, not just because of the potential improvements in the provision of healthcare, but because of the wider issues for more remote communities relating to education, business and social integration.
Delivering routine health, dental and social care, can be difficult due to the challenges of recruiting and retaining clinicians and care professionals to rural communities. Potential barriers include: social and professional isolation, limited spouse employment opportunities, reduced educational opportunities for children, the demands of providing very broad emergency and non-acute services, increased on-call duties, lack of suitable housing, and difficulties in obtaining continuous professional development.
The ability to attract young professionals of all disciplines to more remote and rural environments is a more general issue - suggesting that to be successful, recruitment campaigns should be multi-faceted and relate to more general community development as well as considering opportunities for multi-professional working across communities.
To tackle the barriers to recruitment and retention of staff, including GPs, the 'Being Here' programme has helped deliver an ambitious and creative recruitment exercise aimed at attracting health professionals to live and work in remote and rural areas. With a new micro-site and targeted advertising campaign, a number of successful appointments have been made.
The benefits of adopting community resilience models are also being realised, with the appointment of local residents to posts of rural health and care support worker and first responders. The importance of using all community assets, and developing care that anticipates and reduces the risk of acute illness, is particularly acute in rural areas, where arguably there is the greatest need. In the Small Isles the benefits of adopting community resilience models are being realised, with the appointment of local residents to posts of rural health and care support workers and first responders.
I. Opportunities from Increasing Information Technology (e-health)
Modern clinical IT systems can help to make care more efficient, safer, more person-centred, and more cost-effective. They offer considerable potential to redesign and standardise healthcare processes to meet healthcare practitioner and patient needs. When applied in the right settings IT systems can deliver efficiencies and free up much needed resources for frontline services.
The last 10 years have seen an acceleration in innovation in IT with increased connectivity and mobile communication, and massively more powerful data capture, storage and processing capacity. As a result, clinicians are increasingly reliant on IT systems and technology in their daily work and ensuring that IT infrastructure is resilient, secure and meets their needs is essential.
There have been some notable successes within the NHS in Scotland as a result of investment in IT systems, with direct positive impacts on the working conditions for staff and the quality of care for patients. For example Scotland was amongst the first countries in Europe to establish a national PACS (Picture Archiving System) which means that digital x-ray and scan images can readily be viewed at a distance on any computer that is connected to the network. There has been significant effort in digitising and back scanning records to ensure that these are available electronically. Clinical portal development has facilitated electronic information sharing across hospitals within NHS Boards providing staff with easy access to essential patient information and history, and is increasingly being made accessible to GPs and staff in the community. The electronic patient management system (PMS) optimises patient flow through hospitals by automating processes helping to make our hospitals more efficient and reduce unnecessary discharge delays. Transitions and referrals are managed electronically. Electronic discharge information is sent automatically to GPs allowing them to plan transitions back home or to a community setting with patients and their families using the most up to date information. Electronic referrals help to reduce the time patients wait to meet with a specialist. Application of the latest IT innovations mean that our newest hospitals are paper-light; pharmacy and laboratory services, which have previously been bottlenecks in the system, are fully automated and the latest technologies are being used in diagnosis and treatment where appropriate. Within community and GP services, the national procurement and implementation of two IT systems for general practice across the whole country has led to a dramatic improvement not only in the support for GPs but also in the sharing of summary patient data from primary care with the wider health service in particular providing essential medications and allergy information to the emergency and unscheduled care services. Scotland has a country-wide network to connect all points of care which has recently been expanded to support more integrated health and social care working across public and third sector partners. The secure email system - nhs.net - has allowed extremely effective email communication within the service. The introduction of real-time management information systems have made performance management and financial management much more effective and have helped NHS Boards to manage capacity and resource across the service.
Yet the adoption of some clinical IT systems across the NHS has been variable and has not kept pace with clinicians' expectations. We are not planning to develop a single comprehensive electronic patient record in the short to medium term, however more work is required to digitise paper records and case notes, share summary information between services and partners, and manage workflow across boundaries. The current limited use of electronic hospital prescribing and administration systems needs to be extended to replace existing paper based systems to ensure patient safety; and work is in hand to do so. Electronic reconciliation of medication records is required between hospitals, GP systems, and community pharmacists to ensure that a common up to date electronic medication view is available. Improved electronic information sharing is required between health and social care providers and their third sector partners to ensure that the patient receives the right level of care based on all the information available. Electronic systems will increasingly need to support cross boundary working as we concentrate and integrate resources to deliver the best available care, and support mobile access to meet patient and clinicians' needs. All developments will require greater interoperability between systems, common standards for recording and sharing information and local data sharing agreements based on the nationally agreed SASPI (Scottish Accord on the Sharing of Personal Information).
There are great opportunities for NHSScotland to put its valuable data resource to better use. Given that NHS IT systems are so comprehensive, there is the possibility of analysis of vast amounts of data to identify and study health and treatment trends in almost the entire population. Examples such as the Farr Institute are beginning to build capacity in health informatics research tapping into electronic health data and combining this with other forms of research and routinely collected data. If done in a way that respects data privacy and confidentiality, it should be possible to use NHS-held data much better to guide decision making in complex clinical and population health contexts. Growing evidence suggests that health informatics data can be particularly powerful when combined with a patient's own recorded information and clinical record to target treatment and achieve the best health outcomes. Further, presenting the combined data visually can support clinical co-management practice and sharing the anonymised information amongst interested professional and patient peer groups can support continuous improvement across services. The Scottish Government and NHSScotland are in the process of developing a Health & Social Care Information Strategy to ensure we take full advantage of existing and future opportunities in this respect.
Patient online access to their medical data is still only possible in Scotland in very limited circumstances, although patients have a legal entitlement to view their records if they wish. Most people are currently unable to access their notes online, book appointments electronically, view test results or order repeat prescriptions. This functionality exists with the current GP IT systems but requires local support and some change management within GP Practices to deliver. Good quality information can help patients and carers to achieve higher levels of self-management, and make realistic and informed choices about their healthcare that match their preferences. The provision of online information from accredited sources is in place with the development of digital resources such as NHSinform. However, the current range of public online health information resources needs to be consolidated and personalised. Telecare use is already well proven and is key to supporting patients in their own home but its use is variable and support is being provided to roll out best practice across Scotland. Telehealth is increasingly understood to be beneficial to patient self-management and assisted living when applied in the right circumstances and current work is focused on integrating solutions within a home based model of care. More advanced digital services including eConsultation, and home monitoring and video conferencing telehealth solutions could support GPs and enhance capacity within community hubs over time but will require greater commitment to change management and process redesign. Growth in this area will require a commitment to innovation and support for our local SME market. Scotland is ideally placed to lead in this fertile ground, given its already strong connections between industry, academia and service providers, and its track record in telecare and telehealth innovation. The Digital Health Institute was established to encourage and support market growth and ensure that we make the best use of locally grown innovation.
Plans are in place to significantly improve the situation with patient access in Scotland within the next few years through the creation of a patient portal. This will give access to a summary electronic patient record, personalised health information and digital services for every citizen in Scotland. As well as making the health service more accessible to those who are digitally literate, this IT development will be an important tool for health improvement, self-management and co-production of care plans by citizens. It is therefore a crucial element of realising our overall vision for increasing person-centred, integrated care in the community. Continued investment in IT improvement will be required to support transformed, more person-centred services, to enable better informed decision making, to ensure that clinical records are made readily accessible wherever people are treated and ensure that infrastructure remains resilient and secure.
There is a great opportunity to ensure IT systems are in place that will make the NHS safer, more efficient in delivery of services, more easily accessible and provide the ability to collect and analyse data to guide service planning and treatment decisions. These needs have been identified and a series of plans are in place to address them in the context of the Scottish eHealth Strategy.
J. A Need to Reduce Waste, Harm and Variation in Treatment
There is evidence of unmet need from undersupply or underuse of some services. However at the same time there is evidence of oversupply of some services or interventions, including some that are of limited value. The Academy of Medical Royal Colleges published a document[7] in November 2014 that suggested that '20% of mainstream clinical practice brings no benefit to the patient: Most waste in the NHS lies within clinical practice and models of care.'
There is some concern voiced by clinicians regarding the increased use of investigation and treatment. Their concerns centre on rapidly increasing levels of diagnostic tests, polypharmacy (the use of multiple drugs- this may be of benefit, but, especially in the older person, multiple drugs may give rise to excessive side-effects and drug-drug interactions), interventions at lower thresholds, and clinical variation that is not reasonably explained by patient need.
There are examples of poor understanding of risk by patients and clinicians alike that results in more treatment being used than a person would choose if fully informed and involved. This suggests that people are not always full partners in decision making, and so unable to choose treatment strategies based on complete information and their own preferences. If we are to support people having an increased voice in their treatment choices, and support them in self-management, we need to improve communications with patients, to increase health literacy (the understanding of health, healthcare interventions, and their likely impacts). Initial work has been developed by the Scottish Government on improving heath literacy, which needs to continued.
This must be addressed because of the harm that may result, along with stemming the waste of providing a service that is not desired. There is a need to develop targets that focus on outcomes rather than process, and use data on patient outcomes instead of biochemical or physiological measurement. The current clinical paradigm needs to adapt so that there is an increased focus on realistic and proportionate interventions (to maximise benefit and to minimise patient harm) and an even stronger participation of well-informed people in decisions about their care.
Summary of current challenges
Like many other health services, the NHS in Scotland is facing a series of challenges which can be summarised as:
- increasing need for support from an ageing population with increasing levels of multi-morbidity
- multi-morbidity arising approximately a decade earlier in areas of deprivation
- a need to improve care and outcomes via an expanded, multidisciplinary and integrated primary and community care sector, despite current workforce constraints
- a need to increase co-production with patients and carers, create high-quality anticipatory care plans and to support people in health improvement and self-management
- a need to embrace the changes required for effective integration of health and social care, and ensure that it makes a transformational change in the management of patients despite the current demand and supply challenges also faced by social services
- a need to reduce the avoidable admission of patients to hospital whenever alternatives could provide better outcomes and experiences
- a need to dramatically reduce the problem of discharge delay and thereby the risk of avoidable harm and adverse impact on the maintenance, or re-establishment of independent living
- a need to make better use of information and make better informed decisions about both individual and collective care
- a need to ensure that services become sustainable in the face of considerable workforce and financial constraints by giving careful consideration to planning of more highly specialist provisio
- a need to provide healthcare that is proportionate to people's needs and where possible preferences, avoiding over-treatment and over-medicalisation, and at the same time prevent undertreatment and improving access to services in others
- a need to provide services of greater individual value to patients
- a need to move to sustainable expenditure so that we maintain high quality services and can also avail ourselves of medical advances as they arise, and
- a need to integrate the use of technology into service redesign and to consider how IT could transform service delivery and help meet future challenges.
The NHS in Scotland is a highly valued public service that has significantly improved in recent years - as evidenced by falling death rates from heart disease, stroke and cancer. More people are being treated than ever before, and waiting times have dramatically decreased. The quality of healthcare in Scotland is high, and the work on patient safety, person-centred care and digital health has made us world leading in these areas. Despite the progress in improving quality, life expectancy in Scotland has not improved in line with other European countries, and significant health inequalities remain between the most affluent and the most disadvantaged communities.
Contact
Email: Karen MacNee