Mental health and wellbeing strategy
Strategy laying out our approach to improving mental health for everyone in Scotland.
9. A whole system approach to improving mental health and wellbeing
This model on the following page shows what we think an empowered, effective and accessible support system should look like.
As we were developing this Strategy, people told us that a whole person approach was important to them. We have defined a whole person approach in the context of mental health as:
"When a whole person approach to mental health is proactively considered, embedded and applied in all policy and practice, planning and decisions, we will make the changes required to improve life circumstances."
People's needs for mental health care vary enormously. Some people may be able to manage their mental health conditions themselves, especially with support from family members, peer support groups, faith-based organisations or community providers. Many others will need formal interventions to support their mental health conditions, typically offered through a range of daytime services.
In most areas, mental health support is accessible at out-of-hours primary care centres or via NHS 24. Some people will experience acute symptoms that require short-term care and treatment in hospital with follow-up support and care in the community.
Many people experiencing mental health conditions also require help accessing key social services such as housing, employment, education and welfare. Effective community-based mental health support, care and treatment includes consistency and co-ordination, as well as a careful mix of services and support that are responsive to the person's needs.
Only rarely do people experience conditions that require highly specialised or longer-term care, including within specialised mental health hospitals or residential facilities. People with complex mental health needs have the right to the same support and services as people with complex physical health needs. Anyone with mental health conditions may need different types of support and services at different points in their lives.
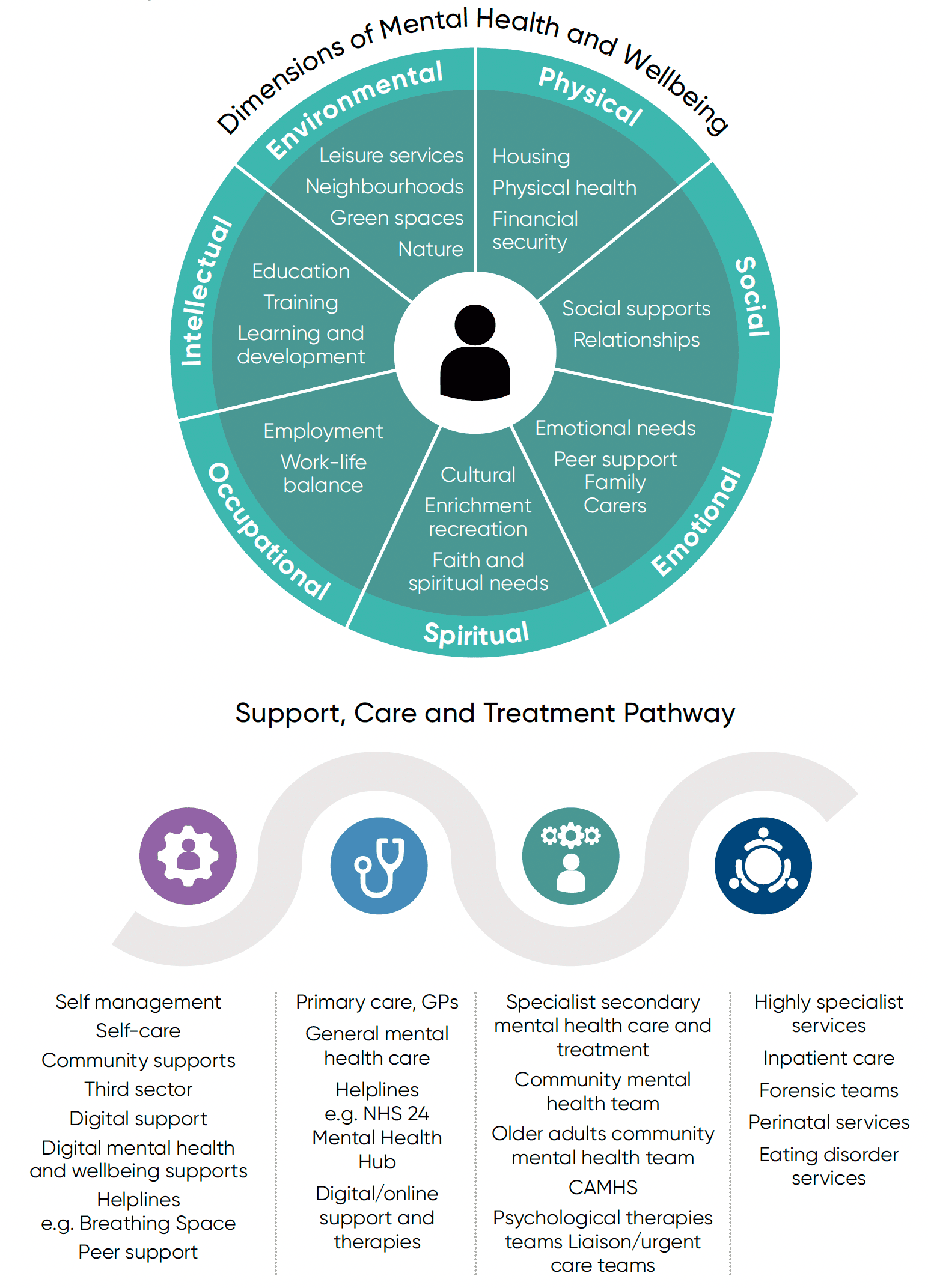
Graphic text below:
Dimensions of Mental Health and Wellbeing
Environmental
Leisure services Neighbourhoods Green spaces Nature
Intellectual
Education Training Learning and development
Occupational
Employment Work-life balance
Spiritual
Cultural Enrichment recreation Faith and spiritual needs
Emotional
Emotional needs Peer support Family Carers
Social
Social supports Relationships
Physical
Housing Physical health Financial security
Support, Care and Treatment Pathway
Self management Self-care Community supports Third sector Digital support Digital mental health and wellbeing supports
Helplines e.g. Breathing Space Peer support
Primary care, GPs
General mental health care
Helplines e.g. NHS 24 Mental Health Hub
Digital/online support and therapies
Specialist secondary mental health care and treatment
Community mental health team
Older adults community mental health team CAMHS
Psychological therapies teams Liaison/urgent care teams
Highly specialist services
Inpatient care
Forensic teams
Perinatal services
Eating disorder services
Our whole systems model outlines that we must continue focusing on prevention and early intervention.
There is a key role for local support in the community. Support, care and treatment need to be delivered in a way that is as local as possible and as specialist as necessary. This requires a system that is responsive to local and individual needs.
However, we know that some mental health conditions are long-term or lifelong, resulting in people needing ongoing support for the rest of their lives. This requires ongoing access to a range of supports and services.
The principles of GIRFEC are already central to Children's Service Planning in Scotland and the delivery of CAMHS across the whole system.
A new way of person-centred working aimed at adults is being trialled called, Getting it Right for Everyone (GIRFE). This is a proposed multi-agency approach of support and services from young adulthood to end-of-life care. GIRFE will help inform whole system working and define the adult journey through individualised support and services. It will respect the role that everyone involved has in providing support. The principles of GIRFE are intended to be central to care planning, providing a whole person approach and more say, choice and control in accessing the help, support and care for all adults when needed. As a future practice model, it will place the person at the centre of decisions that affect them.
Case Study: Family First Approach
A request for assistance (RFA) process has been developed in Aberdeen City to provide clear pathways for children, young people and their families seeking early help for mental health and emotional wellbeing.
The RFA process is a single-entry point to a multi-agency support service, offering whole family support. The multidisciplinary team includes health visitors, family nurses, school nurses and representatives from CAMHS, Children 1st, Community Learning and Development, Social Work, Education, Alcohol & Drugs Partnership, and Creative Learning.
Requests can be made either by the individual, family member or professional. An RFA form gathers data on the needs, vulnerabilities and adverse childhood experiences of the child. The Fit Like hub team engage with the family in an initial conversation to understand their needs from their perspective and discuss this with representatives of the multi-agency partnership, holding the families' voices, needs and hopes at the centre of the discussion.
From these discussions, wrap-around support can be offered which comprehensively meets a whole family's unique needs. This support may come from multiple agencies, for example education support, trauma recovery support and financial support for a family. During their engagement with Fit Like, families can access more support at any time without re-referrals or bureaucratic processes.
Discussion may also lead to supportive and relational signposting to community services that may be better positioned to meet the family's needs. This reduces duplication of support, building capacity in the system by ensuring individuals and families receive the right support at the right time.