Managing Health at Work Partnership Information Network (PIN) Guideline
This Guideline emphasises the need for employers to promote and support employee health and wellbeing and includes sections on issues that affect the health and safety of staff in their everyday work.
MANAGING HEALTH AT WORK
Guideline 8 Biological and chemical hazards
8.1 Introduction
It is acknowledged that in the healthcare environment unpredictable and unforeseen exposure to chemical and biological hazards will inevitably occur. However, through a programme of hazard identification, risk assessment, control implementation and monitoring all reasonably practicable steps will be taken to minimise the risks to healthcare staff.
8.2 The legislative framework
Legislation related to chemical and biological hazards includes:
Health and Safety at Work Act (1974)
Management of Health and Safety at Work Regulations (1999)
Control of Substances Hazardous to Health (COSHH) Regulations (1999)
Chemical (Hazard, Information & Packaging for Supply) Regulations (1994) - CHIP
Food Safety Act (1990)
Food Safety (General Food Hygiene) Regulations (1995)
Reporting of Injuries, Diseases & Dangerous Occurrence Regulations (RIDDOR) (1995)
Data Protection Act (1998)
Requirements of the regulations
Staff must not carry out any work which could involve being exposed to a hazardous substance unless a suitable assessment of the health risks has been carried out and the necessary steps taken to adequately control the risk.
An employer's first duty is to eliminate the use of a dangerous substance ( see 8.4) or to substitute it with a less dangerous one. Only when this is not reasonably practical should employers consider other control measures.
Controls should, as far as reasonably practicable, involve protection other than providing personal protective equipment (PPE). Employers must keep to the specific legal standards relating to the control measures for carcinogenic substances and biological agents.
8.3 Employers main duties
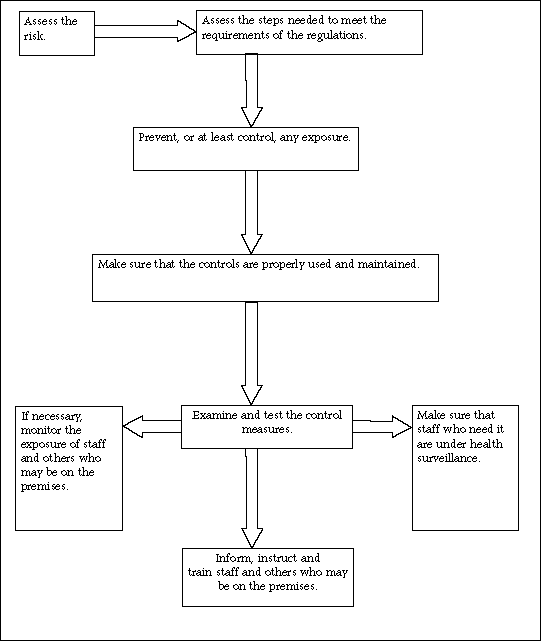
8.4 Recommended approach
The term 'substance hazardous to health' covers virtually all substances which can cause adverse health effects or diseases arising from work activities. However, lead and asbestos are covered by separate regulations. The COSHH regulations deal with chemical and biological hazards, although employers will need to consider all substances used in order to keep to these regulations in the healthcare setting. Some of the more common dangers (which may need their own policy) are shown below.
8.4.1 Legionella
Legionella bacteria have the potential to cause Legionnaire's Disease, a potentially fatal pneumonia. Breathing in small droplets of water contaminated by legionella bacteria causes infection. Outbreaks have been associated with cooling towers and hot- and cold-water services.
NHSScotland organisations should carry out risk assessments to identify potential sources and prepare a scheme for controlling the risks.
8.4.2 Respiratory sensitisers
Respiratory sensitisers can cause asthma. Some of the more common respiratory sensitisers in the healthcare setting include glutaraldehyde, formaldehyde, laboratory animals, latex proteins and certain drugs including penicillin, tetracycline and methyldopa.
Treating occupational asthma involves removing the sensitised subject. This may mean a change of job or even speciality or profession.
8.4.3 Skin sensitisers
Skin sensitisers can cause allergic contact dermatitis. In the healthcare setting many agents are used which can cause skin sensitisation. However, the commonest skin sensitisers include accelerators and antioxidants in latex products, formaldehyde, certain anti-microbial agents and some pharmaceutical products. Treating someone who has become sensitised may involve removing them from further exposure.
8.4.4 Controlling infection and communicable disease
Infections and communicable disease may not be obvious or diagnosed at the time of patient contact. As a result, staff must use standard (previously known as 'universal') precautions at all times to protect their patients and themselves.
Employers need to carefully assess waste generated from healthcare activities to make sure that items which could cause 'sharps' accidents or cross-infection are disposed of appropriately.
Biological dangers in healthcare extend beyond clinical and laboratory settings to other areas. For example, poor practices when handling food can lead to contamination, food-borne illness and food poisoning.
8.4.5 Mercury
Mercury is a poisonous substance and direct exposure to the vapour by inhalation, through the skin or orally or nasally is a health risk. Employers should have a policy to get rid of products containing mercury but, in the meantime, have a spillage policy and make sure that equipment and trained staff are available to deal with any mercury spills. Appropriate waste disposal procedures should also be in place.
8.4.6 Pharmacy products
This covers a wide range of items which can affect health. Employers should control the use of anaesthetic gases and monitor air to make sure that standards are being met. Where cytotoxic drugs are given and disposed of, there should be a policy that protects staff and visitors. Unused 'prescription only medicines' (POMs) must be disposed of as special waste through the pharmacy.
8.4.7 Immunisation and post exposure prophylaxis
Employers should offer staff immunisation against infectious diseases caught at work which are appropriate to their occupational risk. There is also a duty of care to patients in reducing the risk of transmitting infectious agents from staff to patients.
If a staff member suffers a needlestick or contamination incident, their manager must carry out an immediate assessment and take necessary follow-up action including providing HIV post-exposure prophylaxis if appropriate.
8.5 Responsibilities for putting policies and procedures into practice
It is important that the responsibilities both at a strategic and local level are clearly defined. Procedures must identify who is responsible for the following functions within the organisation.
8.5.1 Identifying hazards
In this context a hazard is a substance that could cause harm. A system should be in place to identify all dangerous substances used.
8.5.2 Risk assessment
A risk is the likelihood of a hazard occurring. Employers should keep documents for the procedures for carrying out assessments to meet the requirements of the regulations and keep these as simple as possible. The assessment process should take into account specific risks posed, for example, to new and expectant mothers and young people.
8.5.3 Putting control measures in place
Employers should identify suitable control measures which satisfactorily control the risk. In descending order of priority, control measures are:
getting rid of the risk;
substituting the agent causing the risk;
working in a totally enclosed system;
providing local exhaust ventilation;
providing a safe system of work; and
providing personal protective equipment.
Employers must use all control measures that are identified as necessary at all times. They must also maintain, examine, test and review control measures regularly to make sure that they stay fit for purpose.
8.5.4 Monitoring exposure
If necessary, health surveillance and environmental and personal exposure monitoring should be carried out at appropriate intervals. This should be agreed by consulting with the Occupational Health Service (OHS).
8.5.5 Keeping records
It is a good idea to have an agreed assessment form to support a consistent approach towards assessment. Employers and staff must make sure that all information is recorded in an accurate and timely way. All written records should be legible, signed and dated.
Under the regulations, employers must be able to produce the following records.
The assessments of risks to health caused by exposure. This should include a list of hazardous substances, the control measures provided and the training provided for staff.
The examination, testing and maintenance of control measures. Employers must keep these records for at least five years.
Records of monitoring environmental exposure. Employers must keep these for at least five years.
Employers should keep records of individual dosimetry monitoring and health surveillance for staff for at least 40 years from the date of last entry.
8.5.6 Monitoring and review
All procedures should give details of the method of the review and how often it is carried out. Employers must review assessments in particular when there is reason to think they are no longer valid or there has been a significant change in the work to which the assessment relates.
8.5.7 Communication
At induction and during employment all staff should know about the measures in place to protect them from chemical and biological hazards relevant to their roles. Employers should update this information regularly.
Staff should have access to copies of all COSHH risk assessments which are relevant to their area of work.
8.5.8 Training
Procedures should be in place to make sure that assessors are given enough training to carry out their roles. Employers should also provide information, instruction and training to staff on:
the risks to health created by being exposed to the substances they are working with; and
the measures in place to control the risk and their own responsibilities.
It is particularly important that employers provide this information at induction and regularly after this, and also when any change is made to working practice or the working environment.
8.5.9 Evaluation
Measurements used include the following.
Reactive:
using the 'Reporting of Injuries, Diseases & Dangerous Occurrence Regulations (RIDDOR) 1995';
providing the minimum dataset needed under 'Towards a Safer Healthier Workplace';
recording incidents including needlestick injuries; and
uptake and DNA (did not attend) rates for immunisation programmes.
Proactive:
setting targets for reducing injuries and illness in line with national and NHS strategies;
carrying out a health and safety audit;
creating action plans for putting improvements in place to control risks;
evaluating staff awareness of policies and procedures;
sending regular summary reports to Executive Directors; and
producing an annual report for the organisational Board.
8.6 Blood-borne viruses
8.6.1 Blood-borne viruses include HIV, hepatitis B (HBV) and hepatitis C (HCV). There are many other blood-borne viral infections of which we know little about how infectious they are or the long-term outcomes. Infected people may show no signs or symptoms of blood-borne infections that may be acquired or transmitted at any age from birth to retirement.
As a result, it is essential that all healthcare workers take routine or 'standard precautions' every day to make sure that good practices become a way of life rather than an 'add-on'. See section 8.7 for more information about standard precautions.
Most precautions taken to prevent blood-borne infections are simple and do not need expensive equipment or major changes to existing advice. For example, covering any cuts and abrasions with a waterproof dressing before going to work should be routine practice.
8.6.2 A blood-borne viruses policy should also include and link with the following topics:
8.6.2.1 Preventing transmission at work
This includes:
immunisation before people start work;
safe working procedures including standard precautions;
reporting near misses;
a health and safety culture; and
providing enough staff.
There should be local procedures in each area to take account of the particular challenges of the client groups and workload.
Specialist areas such as laboratories, maternity units and surgical theatres will need routine and major incident and emergency policies and plans. Paramedics, staff working in mental health services, accident and emergency staff and resuscitation teams face both predictable and unknown hazards. Plans and procedures should anticipate risks and prepare staff to protect themselves. Employers should encourage healthcare workers to get help if they are not sure that they can carry out an activity or treatment safely.
8.6.2.2 Preventing transmission
This includes:
pre-employment screening for staff who carry out 'exposure-prone procedures' (this includes those staff working in body cavities where fingers cannot been seen, for example, dentists, surgeons and midwives);
support and advice from OHS for staff with skin conditions which might expose them to risk;
non-invasive techniques;
redesigning procedures to reduce manual input as far as possible, for example in cleaning;
single-use-only equipment; and
retraining or support for staff to change career if they become infected and can no longer work in their previous role.
8.6.2.3 Treating needlestick injury
This includes:
providing appropriate first aid (all staff need training);
a fast-track risk assessment in Accident and Emergency or a designated unit;
providing appropriate antibiotic or anti-viral therapy if necessary;
storing baseline blood samples for any later testing; and
reviewing incidents with the staff member and management to assess if a similar incident could be prevented and making sure documents are correct and complete.
8.7 'Standard precautions'
To reduce the risk of transmitting blood-borne viruses from infected patients to healthcare workers, and vice versa, staff should do the following 1:
Use good basic hygiene with regular hand washing, before and after contact with each patient, and before putting on and removing gloves. Change gloves between patients.
For all clinical procedures, cover existing wounds and breaks in exposed skin with waterproof dressings, or with gloves if the hands are widely affected.
Healthcare workers with chronic skin disease such as eczema should avoid invasive procedures which involve sharp instruments or needles when there are extensive breaks in the skin surface. Broken skin provides a potential route for blood-borne virus transmission, and blood-skin contact is common through holes in gloves which may not be seen.
Use protective clothing as appropriate, including protecting the mucous membrane of eyes, mouth and nose from blood and body fluid splashes. Avoid wearing open footwear in situations where blood may be spilt or where sharp instruments or needles are handled.
Prevent puncture wounds, cuts and abrasions and if they are present, make sure that they are not exposed.
Avoid using sharps wherever possible and consider using other instruments, cutting diathermy and laser.
If sharps have to be used, be particularly careful handling them. Follow approved procedures and use approved sharps disposal containers.
Clear up spillages of blood and other body fluids promptly, and disinfect surfaces.
Follow approved procedures for sterilising and disinfecting instruments and equipment. Wear gloves when cleaning equipment before sterilisation or disinfection, when handling chemical disinfectant and when cleaning up spills.
Follow approved procedures to get rid of contaminated waste safely.
1From UK Health Department's Protecting Health Care Workers and Patients from Hepatitis B: Recommendations of the Advisory Group on Hepatitis 1993, ' AIDS/HIV Infected Health Care Workers 1998 and Guidance for Clinical Health Care Workers: Protection against Blood Borne Viruses 1998.
APPENDIX 8.A
Model Policy for Conrolling Substances Hazardous to Health (COSHH)
1 Introduction
The COSHH Regulations (1999) protect staff and others against risks to their health. They apply to hazardous substances which arise in connection with work under our control or carried out on our behalf. The substances can be solid, liquid, gas, fume, dust, vapour or even micro-organisms and can endanger health by being absorbed or injected through the skin or mucous membranes, inhaled or ingested.
2 Hazardous substances
These include:
a substance which is listed in part 1 of the approved supply list as hazardous for supply within the meaning of the Chemicals (Hazard Information and Packaging) Regulations 1994. It has been specified as dangerous in part V of that list and is very toxic, harmful, corrosive or an irritant;
a substance for which the Health and Safety Commission has approved a maximum exposure limit (MEL) or an occupational exposure standard (OES);
biological agents;
dust of any kind, when there is a high concentration in air; and
a substance which creates a danger to the health of any person which is comparable with the hazards created by substances mentioned in those subparagraphs.
Not all substances which can be hazardous to health are covered by the COSHH regulations, either because they fall outside the definitions given above or are covered by other specific regulations. Among these are the Control of Asbestos at Work, the Control of Lead at Work, the Ionising Radiation Regulations and medicines given to patients.
3 The requirements of COSHH
Employers are responsible for:
assessing the risk to health arising from work and what precautions are needed;
introducing appropriate measures to prevent or control the risk;
making sure that control measures are used and that equipment is properly maintained and procedures observed;
monitoring the exposure of the workers and carrying out the appropriate form of surveillance of their health; and
instructing and training staff about the risks and the precautions to be taken.
4 Prevention and control
Clinical Directors and heads of department must make sure that staff are not exposed to dangerous substances or, if that is not reasonably practicable, that they are reasonably controlled.
Adequate control is achieved if employers meet the following criteria.
If the level of exposure of a substance which could be inhaled and has a MEL is reduced as far as is reasonably practicable (and in any case below the MEL).
If the level of exposure of a substance which could be inhaled and has an OES is reduced to the OES. If the level of exposure is more than the OES, employers must identify the reason and take action to sort out the problem as soon as is reasonably practicable.
A substance which could be inhaled and which does not have a MEL or an OES does not mean that it is safe. Employers should control the level of exposure to that which most of the population could be exposed to repeatedly without any effect on their health.
Employers should control exposure to any substance which can be dangerous if swallowed, absorbed through the skin or mucous membranes or which comes into contact with the skin or mucous members (chemical burns, dermatitis and microbial infection) to a standard where most of the population could be exposed repeatedly to it without any effect on their health.
Employers should always prevent exposure to carcinogens if this is reasonably practicable, or must at least control it to as low a level as is reasonably practicable.
Preventing exposure is the main aim. Measures that employers can consider for controlling exposure include the following.
1 Prevention - eliminate the hazardous substance or substitute it for a less dangerous form of the substance.
2 Control - clean to remove solid or liquid contaminants which contain any dangerous substance.
3 Dispose - get rid of dangerous substances safely.
4 Enclose - place the substance in a suitable container.
5 Exclude - non-essential personnel from the contaminated area.
6 Minimise - create or use as little of the dangerous substance as possible.
7 Provide:
suitable personal protective equipment (PPE);
suitable respiratory protective equipment (RPE); and
adequate facilities for washing, resting, changing and storing clothing, food or drink.
8 Prohibit - do not allow eating or drinking in contaminated areas.
9 Reduce - reduce the number of staff exposed or the period they are exposed for.
10 Store - store dangerous substances safely.
11 Remove - eliminate contaminants carried in the air.
12 Ventilate - provide ventilation to remove contaminants carried in the air.
Employers should prevent exposure in ways other than just providing PPE except to a carcinogen or a biological agent. Employers should always introduce process, engineering, procedural and personal controls before PPE if this is reasonably practicable.
5 Assessment
It is the responsibility of the Clinical Director or head of department to make sure that an assessment is carried out for each process involving hazardous substances. Employers must also assess substances released or produced as part of the process.
Even if the assessment is simple and obvious and can be explained at any time, it must still be recorded on the organisational assessment form ( see Annex 1). This must be signed by the assessor and by the manager or head of department. Managers should keep a copy of the assessment form in their department and send one to the Director of Facilities (or equivalent). The use of these forms will be audited.
Managers must review the assessment if there is reason to suspect it has become invalid or if there has been a significant change in the work previously assessed. Before any new substance is introduced to a workplace within the organisation, the manager must carry out an assessment. The manager must contact the Director of Facilities (or equivalent) about all additions and deletions to a department's inventory of hazardous substances.
The steps to follow in making an assessment are:
identify any hazardous substances which staff and others may be exposed to;
identify the route by which the substances might enter the body;
identify the resulting effects;
examine the working processes, practices and procedures which involve hazardous substances;
estimate the current exposure levels and those which might result from a planned or an unplanned event, such as an increase in levels if work or an accidental release;
compare the estimate against a valid exposure limit to allow to it to be controlled;
only use PPE when all other methods of control have proved inadequate; and
decide on other precautions to help control the substance and whether there is any need for monitoring the exposure.
In gathering information for an assessment, managers may need expert advice. More information is available from manufacturer's data sheets, from the substances database or the Health and Safety Adviser.
Adequate controls must include procedures for dealing with dangerous substances accidentally escaping.
PPE equipment must keep to the requirements of the International Standards Organisation, British or European Standards if these exist. Eye protection must follow the requirements of the Personal Protective Equipment at Work Regulations 1992 and with the current edition of BS2092. To keep to the COSHH Regulations, RPE must be suitable for the purpose and be of the type approved by the Health and Safety Executive or keep to their approved standard.
6 Examining and testing control measures
It is the responsibility of the Clinical Director or head of department to make sure that all control measures are kept in efficient working order and in good repair. Procedures may vary from weekly visual checks to thorough servicing schedules. Employers should examine local exhaust ventilation plant thoroughly and test it at least once every 14 months. Employers must also examine respirators and breathing apparatus frequently. A record of each examination should be kept and this should be available for inspection for at least five years from the date on which it was made.
Employers should provide enough information, instruction and training to allow staff to know the risks to health created by being exposed to hazardous substances and the precautions to be used, including decontamination, PPE and RPE.
7 Monitoring and reviewing
For the purpose of the regulations, monitoring involves using valid and suitable techniques to estimate the airborne exposure of staff to hazardous substances. The Clinical Director or head of department is responsible for making sure that this is being carried out by a competent person and that these activities are recorded.
Employers must monitor the exposure of staff if:
failure or deterioration of control could be a serious risk to health;
MELs, OES or any self-imposed working standards should not be exceeded; and
it is necessary to have an extra check of controls.
Employers must keep records of monitoring for 40 years if they record the personal exposure of identifiable staff. They should be kept for at least five years in all other cases. Records should provide enough information to decide:
when, where and under what conditions it took place;
what monitoring procedures were used and how long they took; and
whose exposure was monitored and what the results were.
8 Health surveillance
Health surveillance is appropriate when staff are exposed to substances in circumstances where:
an identifiable disease or negative health effect may be related to the exposure;
there is a reasonable likelihood that the disease or negative effect may occur under the particular conditions of the work;
valid techniques exist for detecting disease or effect.
This will involve the services of OHS who will be responsible for maintaining health records and carrying out the appropriate examinations, immunisations and investigation. Clinical Directors or heads of departments must act on any medical decision to restrict a staff member's work with a specific substance. Employers must keep staff health records for 40 years from the last date of entry. On receiving reasonable notice, any staff member must be allowed access to any health record which relates to them.
9 Informing staff
The Clinical Director or head of department must tell staff about the dangers and risks arising from their work, any precaution to be taken and, if carried out, the results of monitoring and the results of health surveillance. They must also provide training in using controls and RPE and PPE correctly.
10 Health and Safety Department
The Director of Facilities (or equivalent) will maintain the central records of assessments, controls and monitoring.