Management of chronic pain in children and young people: summary
A summary of the available evidence, combined with a consensus group agreement on key recommendations and suggested patient pathways.
1. Introduction
Patient View
“From a patient perspective I feel these recommendations should be adhered to, to improve patient experience within paediatric chronic pain services. Highlighting the positive experiences of other patients can have an effect on how willing the patient is to cooperate with the multi-disciplinary team.
Drawing from my own experience, it is important that all professionals are delivering the same advice to the patients and families. At present, many patients feel there are discrepancies amongst the different professionals and the advice they have received.
I personally believe these guidelines will play an important role in the improvement of paediatric pain services, and will be an important resource for those experiencing chronic pain.”
The International Association for the Study of Pain ( IASP) defines pain as "an unpleasant sensory and emotional experience associated with actual or perceived tissue damage or described in terms of such damage" [1]. Pain can be described as acute, where it is of recent onset, or chronic, which is commonly defined as longer than three months. However, in reality there is often no clear dividing line between acute and chronic pain. Epidemiological studies indicate a prevalence of chronic and recurrent pain in children of 15-30%, with 8% of children reported as having severe and frequent pain [2-4]. In a systematic review of the epidemiology of chronic pain in children and adolescents the prevalence rates varied. Generally pain prevalence rates were higher in girls and increased with age for the majority of pain types. In addition, lower socioeconomic status was correlated with higher pain prevalence, particularly in headache conditions [5].
Most chronic pain in children can be effectively managed in primary care, with appropriate investigations to exclude treatable causes. There should be an early emphasis on the biopsychosocial nature of pain with access to reliable information and self-management resources for the child and family. There is a significant minority of children where chronic pain can be severely debilitating, affecting all aspects of the child’s life and that of their parents and family members. The impact of pain is wide-ranging affecting school attendance, participation in sports or social activities as well as increased healthcare seeking and medication use. The deleterious effects of untreated pain in children can extend into adulthood [6]. It has also been shown that chronic pain can have a serious negative impact on financial wellbeing. In a cost of illness study in this population, the financial burden of adolescent chronic pain on the UK economy in one year was calculated to be £3840 million [7]. In a study of 149 young adults (aged 10-17) presenting at interdisciplinary pain services in the US it was found that the average cost of care per patient was $11,787 annually [8]. The total cost of moderate to severe chronic pain in the US was estimated to be $19.5 billion a year. The long-term effects of chronic pain on pain processing are not well understood, but it is likely that changes occur leading to excess sensitivity and altered signalling in the nervous system, even without any ongoing tissue damage or injury.
Specialist chronic pain services for children and young people are patchy and have developed through the enthusiasm and commitment of a small number of clinicians. There is very limited access to multidisciplinary pain management and this can be particularly difficult for teenage young people, falling into a gap between children's and adult services or not having an organised transition from one to the other [9, 10]. It is essential that there should be more healthcare professional and public education and resources to effectively manage pain. This is in keeping with the gold standard that care is responsive, and personalised care incorporates a multidimensional pain assessment. Any management plan should address these dimensions of a child or young person’s pain experience, taking account of challenges such as geographical limitations to accessing this care.
The Scottish Intercollegiate Guidelines Network ( SIGN) guideline on the Management of Chronic Pain in Primary Care ( SIGN 136) did not include paediatric pain in remit as the limited evidence base was thought to be insufficient for a full SIGN Guideline [11]. During the development of SIGN Guideline 136, there was feedback from key stakeholders that there is a need for expert guidance on managing paediatric chronic pain [12]. While recognising that in many areas, there is limited high quality evidence, this working group has drawn together multidisciplinary expertise to review the available evidence, and to reach consensus on areas where evidence is limited. Wider consultation out with this group has also been sought.
Delivery of good quality, timely care underpinned by the best available evidence is important. Moreover, routine and accurate assessments of pain must consider the child’s developmental stage, experiences and communication abilities. Thus, this guideline aims to provide a useful practical resource, improving quality of life and reducing the risks of longer term harms for children and young people with chronic pain.
Remit of guideline
The current evidence for the key areas identified has been reviewed with the support of SIGN, using their methodology [13]. Chronic pain was defined as pain lasting longer than three months, or beyond the expected time of wound healing. Neither acute nor cancer pain were included. As chronic pain is caused by many underlying conditions, it was not the focus of this guideline to target specific conditions. The impact of chronic pain is wide-ranging which suggests that the data can be extrapolated to chronic pain as a whole.
The main guideline summarises available evidence, combined with consensus group agreement on key recommendations and suggested patient pathways. We have followed the methodology of SIGN 136 and hope that this guideline will facilitate the transition to adult services. Our aim is that this will ensure all health professionals are delivering a consistent, evidence-based approach. Research gaps have not been specifically listed, as these are clear from the key recommendations and current level of evidence associated with these.
The guideline’s definition of ‘child’ is derived from the UN Convention of the Right of a Child ( UNCRC): termed as a person under 18 years of age. At the national level, the Children and Young People (Scotland) Act 2014 similarly define a child as an individual who has not yet attained 18 years of age [14].
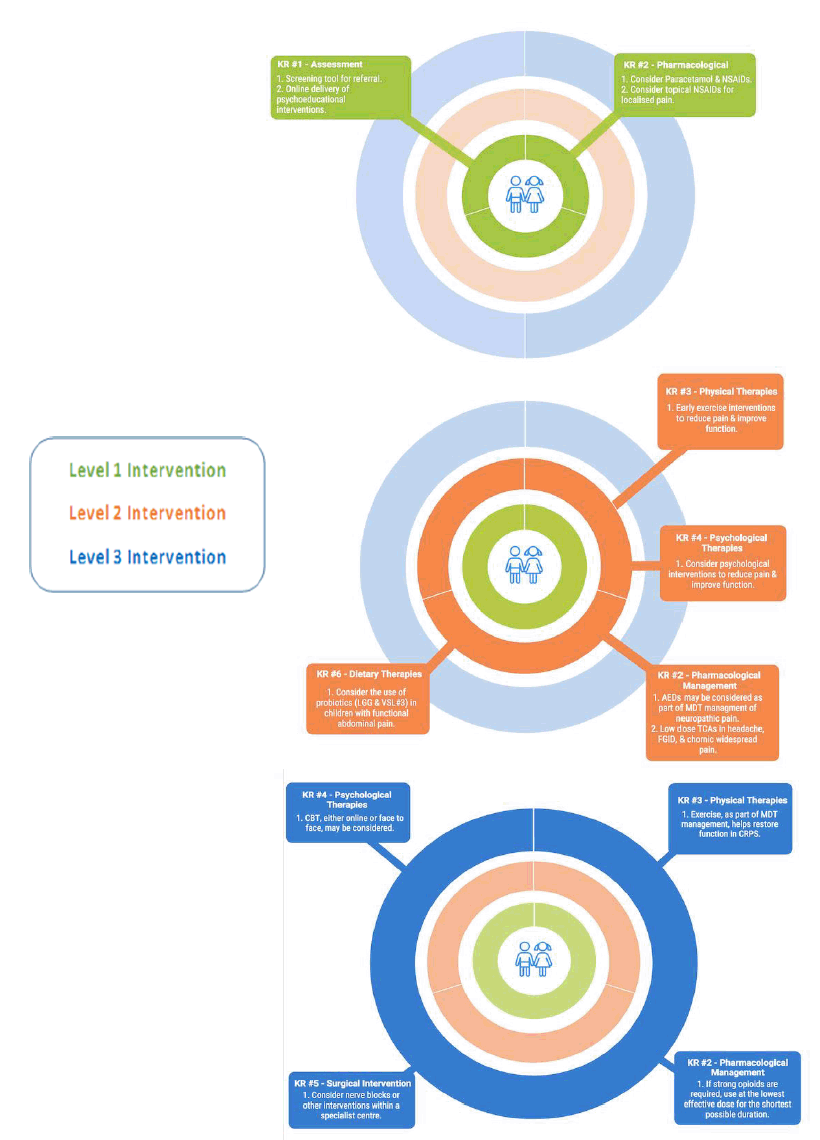
Treatment Pathways
Figure 1 overleaf represents a Paediatric Pain Pathway, which can be utilised by both clinicians and patients to guide management.
Recommendations
Recommendations ( Section 2 and Figure 3) in this guideline are based on:
- a synthesis of the quality of the evidence;
and
- expert consensus opinion of the multidisciplinary guideline development group.
Where there is moderate to high quality evidence, this is highlighted with the recommendations. Due to the limitations in the evidence base, unless otherwise stated, the majority of recommendations are based on expert opinion (4), informed by current evidence.
Prior to any prescribing, the licensing status of a medication should be checked in the summary of product characteristics ( SPC). The prescriber must be competent, operate within the professional code of ethics of their statutory bodies and the prescribing practices of their employers [15].
Key to evidence statements
| Levels Of Evidence | |
|---|---|
| 1 ++ | High quality meta-analyses, systematic reviews of RCTs, or RCTs with a very low risk of bias |
| 1 + | Well conducted meta-analyses, systematic reviews of RCTs, or RCTs with a low risk of bias |
| 1 | Meta-analyses, systematic reviews of RCTs, or RCTs with a high risk of bias |
| 2 ++ | High quality systematic reviews of case control or cohort studies High quality case control or cohort studies with a very low risk of confounding or bias and a high probability that the relationship is causal |
| 2 + | Well conducted case control or cohort studies with a low risk of confounding or bias and a moderate probability that the relationship is causal |
| 2 | Case control or cohort studies with a high risk of confounding or bias and a significant risk that the relationship is not causal |
| 3 | Non-analytic studies, e.g. case reports, case series |
| 4 | Expert opinion |
Figure 1: Paediatric Pain Pathway [1]
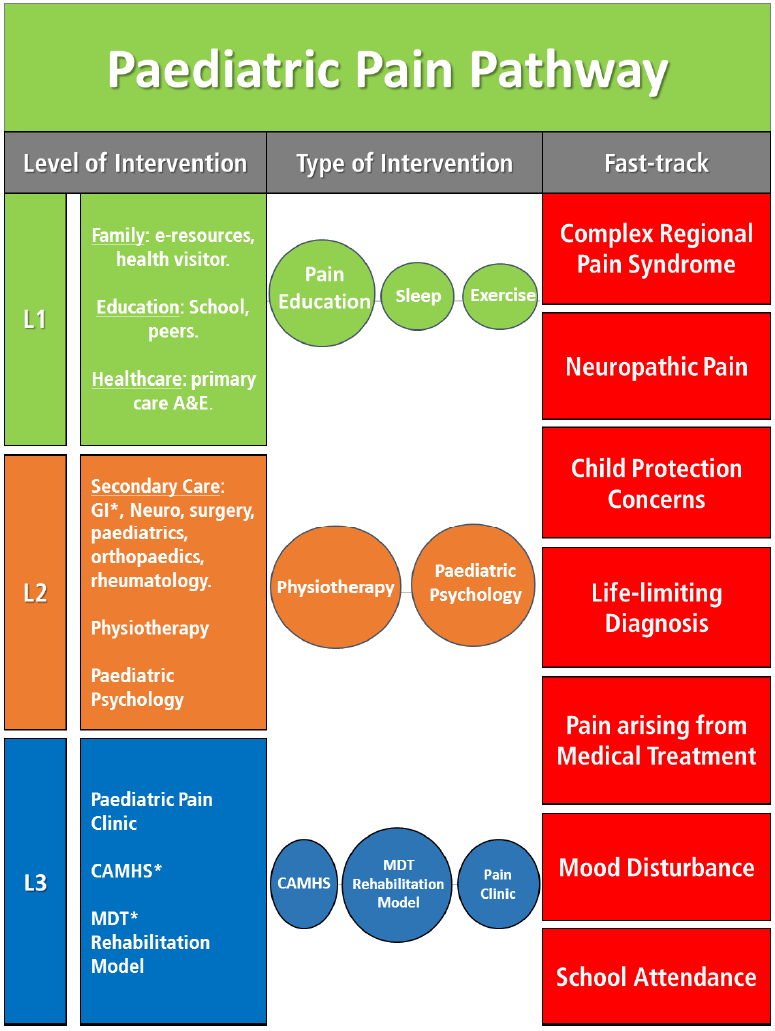
Figure 2: Key Recommendations ( KR)