Living and Dying Well: Building on Progress
Living and Dying Well: Building on Progress records the progress which has been made towards achieving the aims of Living and Dying Well, and sets out the next phase of actions required by NHS Boards working with stakeholders.
3 National developments
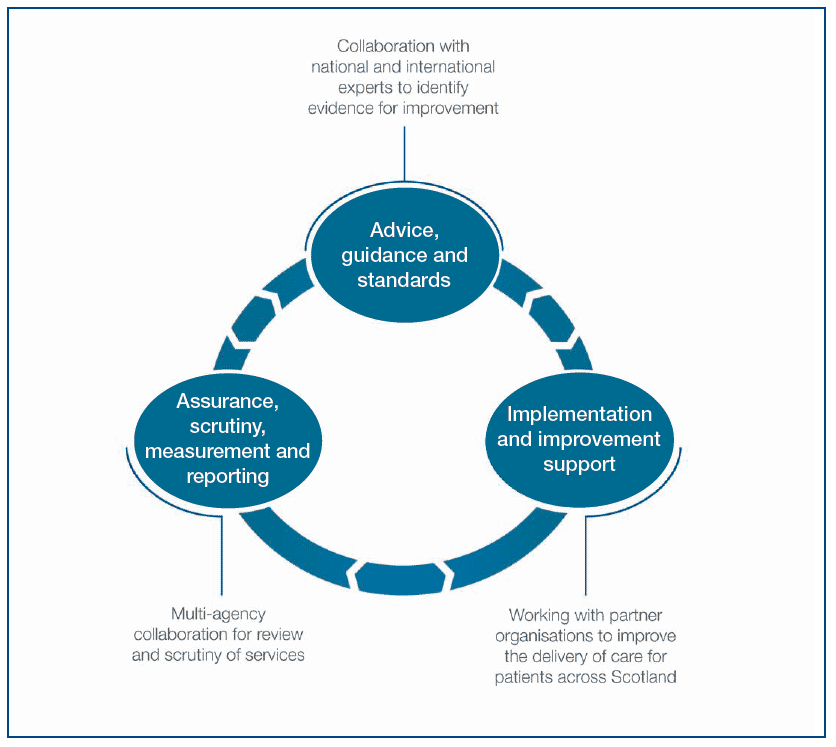
16 The Scottish Government is committed to an integrated approach to its key policies and strategies. The recently launched Healthcare Quality Strategy for NHSScotland4 provides the opportunity to bring together all aspects of patient care in a new quality improvement model (figure 3) which will ensure a unified approach to ensuring the best quality care for every patient every time at every stage of their lives.
17 NHS Quality Improvement Scotland has agreed that palliative and end of life care, and the continuing implementation of Living and Dying Well1 and Living and Dying Well: Building on Progress should be included as one of the integrated work programmes through which it will support implementation of the Healthcare Quality Strategy4.
18 The NHSQIS approach is based on an integrated cycle of improvement incorporating:
- advice and guidance
- implementation and improvement support
- assessment, monitoring and reporting.
Figure 3
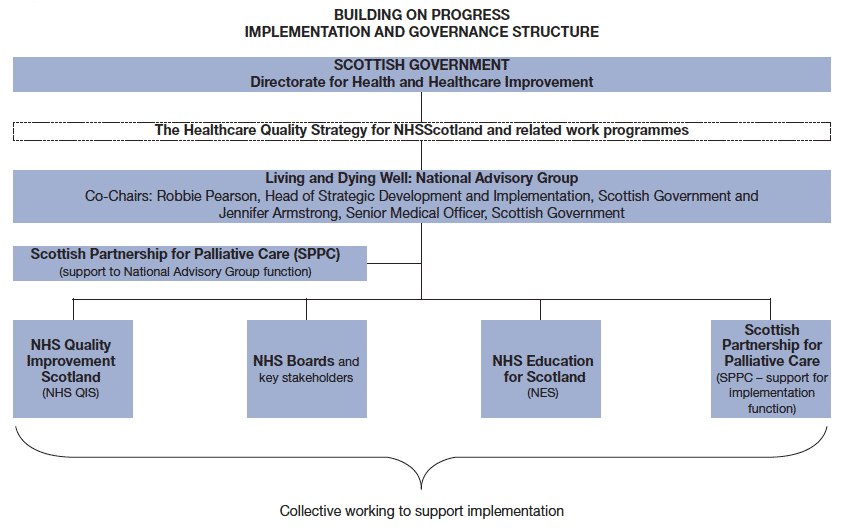
19 In its role of supporting continuous quality improvement within palliative and end of life care, NHSQIS will work closely with the Scottish Government, with NHS Boards, Special Health Boards such as NHS Education for Scotland, the Scottish Partnership for Palliative Care and other partner organisations to promote integration and alignment of national initiatives and programmes of work. It will liaise closely with NHS Boards regarding further priority areas of activity and will ensure that any future developments are taken forward in partnership with SPPC and NES through the Living and Dying Well1 National Advisory Group (see figure 4). The strengths of NHSQIS (quality improvement), NES (education and workforce development) and SPPC (innovation, setting the agenda (leadership) and sharing beyond traditional palliative settings) will collectively maintain the development of palliative and end of life care which will bring together best practice and support improvement in a continuous cycle.
Figure 4
20 In addition, the Analytical Services Division of the Scottish Government has identified a senior statistician to work with the Living and Dying Well1 National Advisory Group and appropriate policy leads to develop local and national indicators and appropriate targets aligned with the potential quality outcome measures identified in the Healthcare Quality Strategy4.
21 Significant quality improvements in palliative and end of life care have already been achieved through a number of national developments arising out of the implementation of Living and Dying Well1, in particular the Palliative Care Directed Enhanced Service in Scotland, the electronic Palliative Care Summary ( ePCS) and the NHSScotland Do Not Attempt Cardiopulmonary Resuscitation ( DNACPR) Integrated Adult Policy13.
22 The Scottish Government introduced its Palliative Care Directed Enhanced Service ( DES) in Scotland in November 2008 as part of its cohesive and integrated approach to meeting the palliative and end of life care needs of patients and families on the basis of clinical need rather than diagnosis or prognosis, and to addressing the need for effective communication at times of transfer and transition of care. Continued funding has been agreed for the year(s) 2010-2012, and reporting systems were reviewed between April and June 2010 by representatives of the GP community across Scotland to take account of feedback received. Alignment with the ePCS has also been assured. Revised guidance will be issued shortly to reflect developments arising from the implementation of Living and Dying Well1 and to support practices in:
- ensuring that they identify appropriate patients for the palliative care register
- sharing assessed needs through anticipatory care plans with patients, those close to them and with health and social care professionals who provide care both on hours and out of hours - especially when needs change
- determining a patient's preferred place of end of life care and seeking to meet this wish where possible.
23 In order to sustain the continued progress in palliative and end of life care a collaborative approach to support improvement is required. The experience and expertise of organisations such as, NHS Quality Improvement Scotland, NHS Education for Scotland and the Scottish Partnership for Palliative Care will collectively support quality assurance and quality improvement in palliative and end of life care.
24 The support to NHS Boards and key stakeholders will be further defined through the specific actions within this document and through further exploration with NHS Boards. In general terms, and summarised as Action 1, NHS Quality Improvement Scotland, will provide support in line with the integrated cycle of improvement illustrated in Figure 3, NHS Education for Scotland will provide the education focus to the listed priorities and the Scottish Partnership for Palliative Care will manage and review the progress against the actions of Living and Dying Well1 and Living and Dying Well: Building on Progress through which potential areas for future support and/or development will be identified.
Action 1
The Scottish Partnership for Palliative Care ( SPPC), NHS Education for Scotland ( NES) and NHS Quality Improvement Scotland ( NHSQIS) should work together to support NHS Boards and key stakeholders to implement the priorities and actions of Living and Dying Well1 and Living and Dying Well: Building on Progress, in line with the integrated improvement cycle illustrated in Figures 3 and 4, specifically:
NHSQIS will work with partner organisations and in collaboration with NHS Boards and key stakeholders to integrate quality improvement in the development of palliative and end of life care services.
- NES will continue to develop education solutions in line with the priorities and aims of Living and Dying Well1 and Living and Dying Well: Building on Progress
- SPPC will support NHS Boards and key stakeholders to implement the priorities and actions of Living and Dying Well1 and Living and Dying Well: Building on Progress through the specific identified actions.
In addition, SPPC will support the National Advisory Group ( NAG), fulfilling the roles outlined below:
- produce regular reports on implementation to NAG (based on intelligence gathering through SPPC networks and NHS board returns). It is suggested that a baseline report be developed. Thereafter exception reporting and taking periodic focus on specific actions could be employed
- identify common issues (e.g. which are not necessarily Board-specific) and escalate, as appropriate, to Members of the NAG
- in discussion with the NAG provide initiation of interventions to address common issues (where work at a national level offers appropriate solutions)
- ensure regular communication with stakeholders across sectors regarding activity, progress and good practice
- ensuring linkage between Living and Dying Well1 work and work ongoing in relation to other national work streams (e.g. Long Term Conditions, Dementia, Older People)
- provide the secretariat to the NAG.