Living and Dying Well: Building on Progress
Living and Dying Well: Building on Progress records the progress which has been made towards achieving the aims of Living and Dying Well, and sets out the next phase of actions required by NHS Boards working with stakeholders.
1 Introduction
1 The launch of Living and Dying Well: A national action plan for palliative and end of life care in Scotland1 in October 2008 followed the Scottish Government's acceptance, in its December 2007 action plan for health and wellbeing Better Health Better Care2, of the recommendations made in the Scottish Partnership for Palliative Care ( SPPC)'s May 2007 report Palliative and end of life care in Scotland: the case for a cohesive approach3. Two years on, there is widespread evidence that the cohesive national approach outlined in Living and Dying Well1 is well on the way to ensuring the provision of consistent and equitable palliative and end of life care for all people and their families across Scotland who need it.
2 Key to the success of Living and Dying Well1 is its dual emphasis on a person-centred approach to care and care planning and on the importance of communication, collaboration and continuity of care across all sectors and at all stages of the patient journey. Those values also form the basis of the Scottish Government's Healthcare Quality Strategy for NHSScotland4, launched in May 2010. The Quality Strategy4 recognises the importance of anticipatory approaches and advance care planning, based on mutually empathic dialogue between patients, families and all of the individual professionals involved, as a key component of person-centred care. Living and Dying Well1 outlines this process as follows:
- early identification of palliative care needs
- holistic assessment, with the patient and carer, of their physical, social, emotional, cultural, religious and spiritual care needs and other relevant life circumstances
- planning, co-ordination and delivery of appropriate care based on the needs identified
- appropriate sharing and communication across all care settings of the needs and plans identified and actions taken
- regular review and repetition of the assessment and planning cycle.
3 This approach is now firmly embedded in Scottish Government healthcare policy, and underpins workstreams such as the Long Term Conditions Collaborative5, Scotland's National Dementia Strategy6, Reshaping Care for Older People7, and Getting it Right for Every Child8. Its particular significance in palliative and end of life care is highlighted by the 2009 data from Information Services Division ( ISD) (figures 1-2) for hospital admissions and bed days during the last five years of life. These figures demonstrate the reality of a population living longer with multiple long term and life threatening conditions and show that, in the five years before death, people are admitted to hospital more and more frequently, often on an emergency basis, and remain there for increasing lengths of time. These admissions also represent an increasing proportion of all hospital admissions. Figures produced by ISD for the Scottish Government show that those in the final year of life accounted for around 30% of all bed days.
4 Living and Dying Well1 advocated a comprehensive and cohesive approach to the planning and improving of palliative and end of life care. It describes palliative and end of life care as integral aspects of the care delivered by any health or social care professional, focusing on the person, not the disease, and applying a holistic approach to meet the physical, practical, functional, social, emotional and spiritual needs of patients and carers facing progressive illness and bereavement. It is essential that NHS Boards, with key stakeholders, including, for example, the voluntary sector and social care partners, work together in order for the aims of Living and Dying Well1 to be fully realised.
5 The collaboration and continuity of care is significant for patients and carers with palliative and end of life care needs. It is important to note the patients and their carers within other sectors particularly care homes and people at home. For example, there are approximately 38,000 beds in care homes for older people and 55,000 people over 65 years receiving home care. Whilst these figures do not specifically relate to palliative care need, they do reflect a population of older people who may require palliative care and who may wish for support to be provided within that setting.
Figure 1
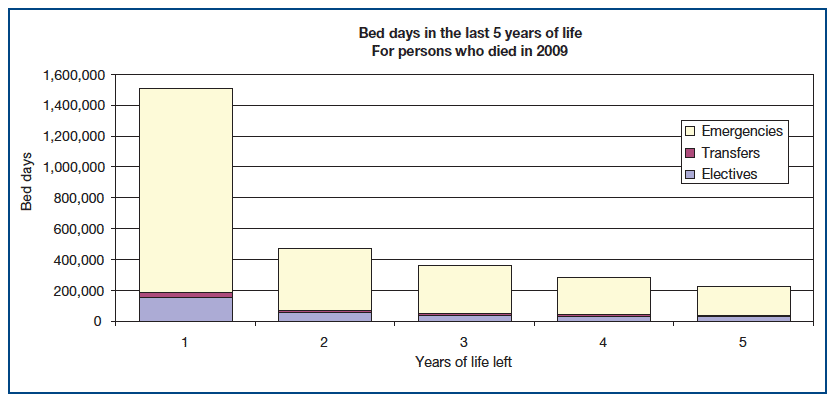
Figure 2
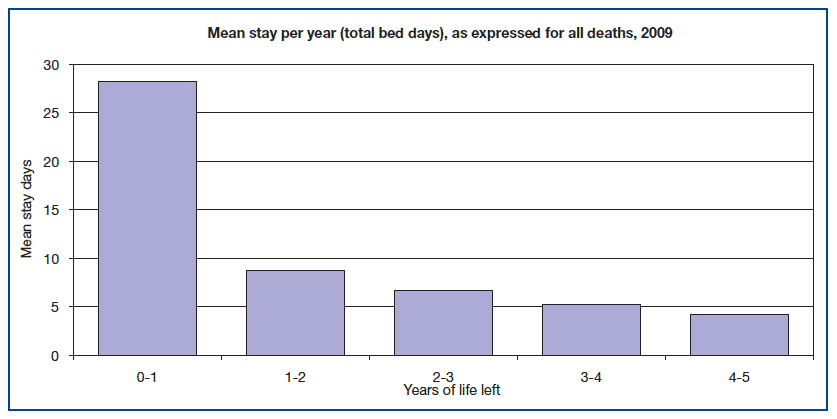
6 These figures do not signify any failing in the approach which supports Shifting the Balance of Care9 and related strategies. The hospital admissions reported in Figure 1 will frequently, but not always, represent the right care in the right place and at the right time for a particular patient and his/her family. However, we know from the findings of the National Patient Experience Programme 10, that additional support for patients and carers is required around the times of entering and leaving hospital. Planning ahead with patients and families while the patient is in the community, for example, at home or in a care home setting, according to the philosophy of advance/anticipatory care planning, is crucial in ensuring that care provided is appropriate and in accordance with the patient's wishes, and key to improving patients' and carers' experience of care.
7 The cycle of hospital admission and discharge evident in the last five years of life means that the entire health and social care system, including the interfaces for example, between primary care, acute care, care at home, care homes and out of hours care, is necessarily involved on a 24/7 basis in delivering and ensuring the quality of palliative and end of life care. Much of the Living and Dying Well1 development work described below has been devoted to this area, and there is now widespread recognition of the complexity involved. The Scottish Patient Safety Programme11 emphasises the particular importance of timely and effective communication at the time of transfers of care while the recently published General Medical Council guidance Treatment and care towards the end of life: good practice in decision making12 advises:
" As treatment and care towards the end of life are delivered by multi-disciplinary teams often working across local health, social care and voluntary sector services, you must plan ahead as much as possible to ensure timely access to safe, effective care and continuity in its delivery to meet the patient's needs."
(paragraph 50)
8 Getting this right will go a long way towards bringing about the improvements required to achieve the Quality Ambitions 4 of NHSScotland, as well as the aims of Living and Dying Well1.
9 Those aims were ambitious and wide-reaching, but Living and Dying Well1 did not claim to have all the answers. Since October 2008 it has been the catalyst for a huge amount of collaborative and development work across a range of areas. These include the short life working groups established following its launch to explore specific issues and make recommendations to the Living and Dying Well1 National Advisory Group, as well as a number of parallel initiatives and developments relevant to its aims. The resulting outputs and recommendations, outlined below, are testament to the enormous level of engagement and commitment which have characterised the contributions of individuals and organisations across all sectors of health and social care. This document records the very substantial progress which has been made by all concerned towards achieving the aims of Living and Dying Well1, and sets out the next phase of actions required in order to continue building upon that progress.
Progress to date includes:
- robust ongoing governance and leadership to support improvement
- ongoing national roll out of the electronic palliative care summary ( ePCS)
- the publication of the NHSScotland Do Not Attempt Cardiopulmonary Resuscitation ( DNACPR) policy13
- the publication of the NHSScotland Resuscitation Policy for Children and Young People14
- the commitment and support of organisations including NHS Quality Improvement Scotland, NHS Education for Scotland and the Scottish Partnership for Palliative Care
- strong links across national strategies and policies including the Healthcare Quality Strategy4
- the development of palliative care guidelines
- recommendations on palliative care assessment tools
- the development of NHSScotland referral criteria to specialist palliative care and
- publication of guidance on advance care planning.