My Health, My Care, My Home - healthcare framework for adults living in care homes: summary
Framework providing a series of recommendations that aims to transform the healthcare for people living in care homes.
5. Urgent and Emergency Care
Accessing appropriate urgent and emergency care in a safe and timely way is extremely important. This is particularly so at weekends and during the out of hours period.
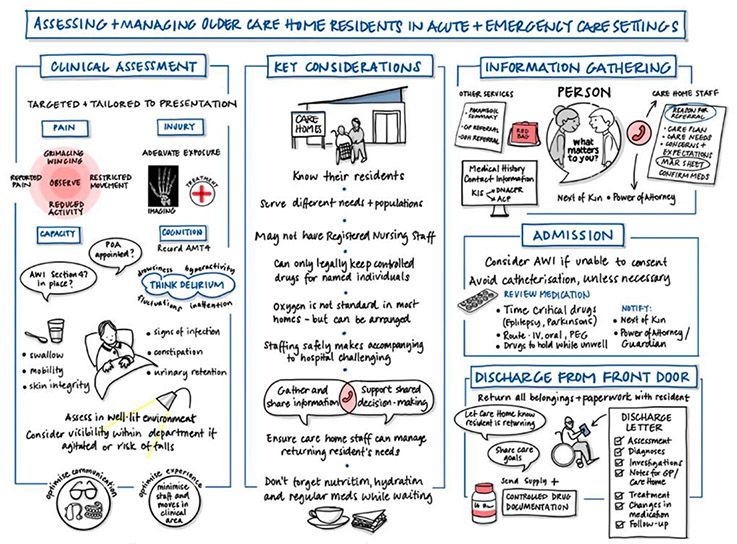
People living in care homes can become unexpectedly unwell, requiring urgent care and attention. At times it can prove difficult to establish the cause of sudden deterioration due to complex issues, for example cognitive decline or reduced physical function. It is also more difficult for people living in care homes to access services that have been set up for urgent care (e.g. an urgent optometry or dental appointment, a community pharmacy or a hospital minor injuries unit). Many of the urgent care services developed as part of the General Practice (GP) contract, such as advanced practitioners, will only see people who are able to attend the GP surgery.
Access to services out of hours can be challenging for care home staff and response times may be lengthy. There are many different ways to obtain urgent and emergency care across Scotland outwith normal working hours (out of hours services, professional lines, NHS 24/ 111, or 999), many of which do not provide an immediate service for vulnerable people living in care homes. A consistent approach is needed. As is a multidisciplianry approach for professionals working together. The sector has made clear their desire for direct professional to professional communication channels, such as dedicated phone lines, to ensure staff in care homes have 24/7 support in making decisions for a person who has become unwell. Having direct access to help during the out of hours period will aid seamless and timely access to health and care support and response 24/7. This is particularly important in managing symptom control for people approaching the end of life.
However, people living in care homes are at risk of developing delirium and deconditioning from an admission to hospital. A shared decision should be made about whether transfer to hospital is appropriate, taking into account the individual's care plan, carer and relatives' wishes and clinical assessment.
Alternatives to hospital admission including community-facing specialty teams (e.g. hospital@home) should be considered to allow individuals to receive hospital-level care within the care home when appropriate.
Recommendations
5.1 Support and empower care home staff by providing and encouraging participation in training opportunities and enabling all staff to have the tools to assess and communicate in acute and emergency situations using the SBAR format.
5.2 People living in care homes should have timely access to members of their MDT, 24/7 when urgent or unscheduled care is required.
5.3 HSCPs should consider developing dedicated community healthcare teams comprising advanced practitioners who can respond quickly and visit people in care homes requiring urgent unscheduled assessments, with support and advice being easily available from the GP by phone. These services should cover both weekdays and weekends.
5.4 Both care home staff and healthcare staff should be familiar with the SBAR format when discussing urgent or emergency care, and consider using a structured proforma for these conversations.
5.5 Care home staff should be able to contact healthcare professionals during an urgent or emergency situation in a consistent and timely manner - this includes exploring possibilities for dedicated professional to professional communication channels.
5.6 Scoping work should take place to explore the use of near patient and point of care testing within care homes, taking into account Realistic Medicine principles.
5.7 Health boards should develop Hospital@Home services that support people living in care homes to receive hospital-level care within the care home.
5.8 Further work is required across Scotland to improve the accessibility and provision of medicines during an urgent situation. This includes exploring mechanisms to enable care homes to hold a stock of certain drugs within the home.
5.9 People living in care homes should never be denied admission to hospital solely on the basis of living in a care home, and at point of admission older people should be assessed by a senior clinical decision maker with experience in caring for frail older adults.
5.10 Timely and safe transfers to and from hospital for older people in care homes should be optimised.
5.11 Digital access to an individual's health records, and clinical outcomes should be timely and accessible to all parts of the system.
Contact
Email: carehomeshealthcare@gov.scot