Growing up in Scotland: overweight and obesity at age 10
The report uses data from the Growing Up in Scotland study to investigate trajectories of overweight and obesity during the primary school years and identify key risk factors.
5. Variations in overweight and obesity at age 10 by other factors
5.1. Introduction
The causes of childhood obesity are known to be many and complex (Obesity Action Scotland, 2017). They range from features of early life such as birth weight and early nutrition, to parental behaviours and characteristics such as eating habits and maternal BMI. Children's diet, along with their levels of physical activity and sedentary behaviour, is also known to be important.
The comprehensive nature of topics included in GUS data collection permits an exploration of the relationship between some of these related factors and child overweight and obesity at age 10. In this chapter we therefore examine associations between overweight and obesity and various child, parent and family circumstances and experiences from birth to age 10, though focused mainly on the period between ages 6 and 10.
Note that where statistically significant associations are found, these do not prove a causal relationship.
5.2. Key findings
- Children whose mothers are overweight or obese are significantly more likely to be overweight including obese at age 10 than children whose mothers have a healthy BMI. For example, 29-32% of children whose mother was obese were also obese compared with 11% of children whose mother was a healthy weight.
- Longer typical screen time and irregular breakfast habits were associated with overweight/obesity. For example, 31% of children who always ate breakfast were overweight including obese compared with 44% of those who only occasionally ate breakfast. Both factors also varied considerably by social background with children in more disadvantaged circumstances more likely to have higher screen time and irregular breakfast habits.
- Children with a television in their bedroom were more likely to be overweight including obese than those without – 38% compared with 26%. Having less than the recommended amount of sleep was also associated with overweight/obesity.
- Neither child longstanding illness, frequency of unhealthy snacking for children or parents, level of physical activity at age 6, nor participation in sport were statistically significantly associated with child overweight/obesity at age 10.
- Thirty-five percent of parents whose children were obese and 88% of those whose children were overweight perceived them to be of normal weight. Sixty-three percent of children who were obese and 78% of those who were overweight perceived themselves to be 'about the right size'.
- Children who were obese were less likely to be very happy about the way they looked than healthy weight children (53% compared with 62%).
- Analysis to explore which factors were most closely associated with being overweight or obese at age 10 when all factors of interest were taken into account found relationships with being overweight or obese at age 6, having a mother who was obese, an average weekly screen time of 14 hours or more, only occasionally eating breakfast and having a TV in the child's bedroom. Of these, BMI status at age 6 was by far the strongest predictor of overweight/obesity at age 10.
5.3. Child health, birth weight and maternal BMI
Differences in children's BMI status at age 10 was examined according to variations in birth weight, maternal BMI and child health.
Table 5‑1 Children's BMI classification at age 10 by birth weight
| Birth weight | ||||||
|---|---|---|---|---|---|---|
| <2.5kg | 2.5 to <3kg | 3 to <3.5 kg | 3.5 to <4 kg | 4 to <4.5 kg | 4.5 kg or above | |
| % | % | % | % | % | % | |
| BMI age 10 | ||||||
| Underweight | 5 | 4 | 2 | 1 | - | - |
| Healthy weight | 69 | 64 | 67 | 63 | 56 | 64 |
| Overweight | 12 | 15 | 13 | 17 | 19 | 18 |
| Obese | 14 | 17 | 18 | 19 | 25 | 18 |
| Unweighted bases | 157 | 378 | 995 | 840 | 319 | 63 |
Birth weight was reported by parents during the first sweep of data collection when the child was aged 10 months. Data was collected in both imperial and metric units, with imperial weights converted to create a single variable indicating weight ranges from < 2.5kg to >= 4.5kg. Results are shown in Table 5‑1.
Children with a low birth weight (of less than 2.5kg) are less likely to be overweight or obese at age 10 than children with higher birth weights (Table 5-2). Likelihood of being overweight or obese generally increases with birth weight with children who weighed between 4 and 4.5kg at birth being considerably more likely to be overweight or obese than those with lower birth weights.
Maternal (biological mother's) BMI was measured when the child was aged 6. As with cohort children, the height and weight of mothers was measured by survey interviewers during the household visit. BMI was then calculated and grouped into standard classifications. For most adults, a BMI of 18.5 to 24.9 kg/m2 is considered healthy, 25.0 to 29.9 kg/m2 is overweight and over 30 kg/m2 is obese.
As shown in Figure 5‑1, child and maternal BMI are closely related. Children whose mothers are overweight or obese are significantly more likely to be overweight or obese themselves at age 10 than children whose parents have a healthy BMI. For example, 29% of children whose mother was obese and 32% whose mother was severely obese were also obese compared with 11% of children whose mother was a healthy weight.
Figure 5‑1 Children's BMI classification at age 10 by maternal BMI*
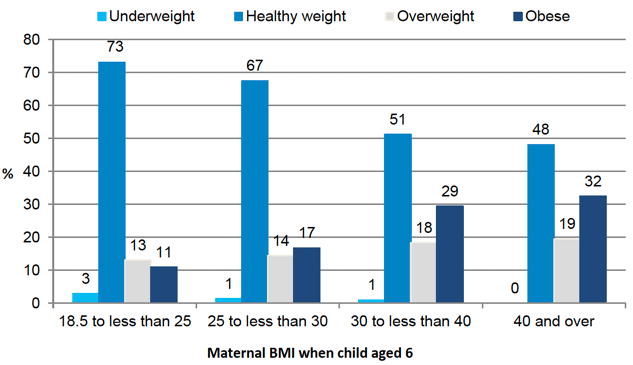
*Note mothers with BMI < 18.5 kg/m2 were excluded due to low base sizes
The relationship between child health and BMI at age 10 was explored using a measure of child longstanding illness. At each sweep of data collection, parents are asked whether the child has an illness or disability that has troubled or is likely to trouble him/her over a period of time. Responses given when the child was aged 6, 8 and 10 were combined to create a variable indicating whether the child was reported to have an illness at age 10, at ages 6 or 8 but not 10, or at none of these ages. There was no statistically significant relationship between child longstanding illness and child overweight/obesity at age 10.
5.4. Eating habits
Two measures of the child's eating habits at age 10 were selected for analysis. The first combines data from three questions on how often the child ate sweets or chocolates, crisps, and drank sugary drinks into a summary measure of unhealthy snacking. The second asked how often the child ate breakfast.
Frequency of unhealthy snacking was not statistically significantly associated with overweight/obesity at age 10. This is perhaps not surprising given that the questions do not provide information on portion sizes nor wider eating habits (such as the nutritional content of main meals).
Figure 5‑2 Children's BMI classification at age 10 by how often eats breakfast
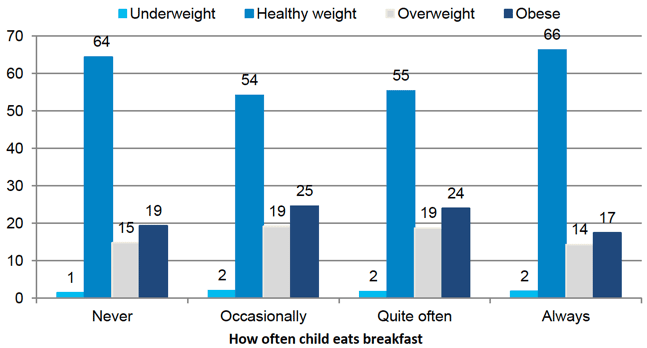
Eating breakfast was related to BMI at age 10. As shown in Figure 5‑2, children who always ate breakfast were more likely to be a healthy weight and less likely to be overweight or obese than children who ate breakfast occasionally or quite often[17]. Among children who always ate breakfast, 31% were overweight or obese compared with 44% of those who only occasionally ate breakfast.
This relationship may be driven by socio-economic variations in how often children eat breakfast. In general, children from more disadvantaged backgrounds – who are also more likely to be overweight or obese – were more likely than those from more advantaged backgrounds to have breakfast only occasionally or quite often. For example, 17% and 13% of children in the lowest income group had breakfast occasionally or quite often compared with 3% and 5% in the highest income group. In contrast, 91% of children in the highest income group always had breakfast compared with 66% in the lowest income group.
Using similar questions on sweets, crisps and sugary drinks, a measure of parental unhealthy snacking – again measured when the child was aged 10 - was also derived. This was not statistically significantly associated with child BMI at age 10 nor was it associated with maternal BMI when the child was aged 6.
5.5. Child activities
Measures of child activity considered include levels of physical activity and participation in sport, sedentary behaviour, unsupervised time and sleep.
5.5.1. Physical activity and organised sport
Levels of physical activity were measured using the approach applied in the Scottish Health Survey. When the child was aged 6, parents were asked about their child's participation in four types of physical activity (for at least 5 minutes) in the past week. For activities outside school, these included walking, organised sports or exercise activities such as swimming lessons or a gymnastics class, and other active behaviour such as running about, riding a bicycle or kicking a ball around. Mothers were also asked whether their child had taken part in walking, sports, exercise or other active things when the child was at school.
For each of these different types of physical activity, mothers were asked for the number of weekdays and the number of weekend days on which their child had engaged in the activity, and for the duration of each type of activity on both a weekday and a weekend day in the past week. Average duration was recorded using a 10-point scale, running from (1) at least 5 minutes but under 15 minutes to (10) 4 hours or more. This information was used to estimate typical total physical activity time per week and to classify children into three groups:
- those active for 60 minutes or more on all seven days
- those active for between 30 and 59 minutes on all seven days
- those with lower levels of activity
Excluding activity at school, the vast majority of children (84%) were reported as having been active for 60 minutes or more on every day in the past week. Just 8% had been active for between 30 and 59 minutes on each day and 8% less so. When activity at school is included, 86% had been active for 60 minutes or more every day. Whether including or excluding activity at school, level of physical activity at age 6 was not associated with overweight or obesity at age 10.
When the child was aged 6 and 8, parents were also asked whether the child regularly participated in out-of-school activities including organised team and individual sports.
Data from both time points was combined to create a variable indicating whether the child participated in organised sport at ages 6 and 8, at one or other age, or at neither age. Fifty-six percent of children were regularly participating in sport at each age[18], 25% only at either 6 or 8 years and 19% at neither age. This was not statistically significantly associated with overweight or obesity at age 10.
5.5.2. Sedentary behaviour
Screen time was used as a measure of sedentary behaviour. When the child was aged 6, 8 and 10, parents were asked how long their child spent watching television (including DVDs and videos), and how long they spent using a computer or games console, on a typical weekday and a typical Saturday. Duration was recorded in hours, or fractions of hours. Weekly hours of screen time were calculated for each age and then averaged over the three ages.
Almost one-third (29%) of children were reported to have less than 14 hours of screen time per week with a similar, though slightly larger proportion, having between 14 and 21 hours (36%). Twenty-two percent spent between 21 and 28 hours per week on screen-based activity and 14% 28 hours or more (equating to 4 or more hours per day).
Weekly screen time was associated with BMI at age 10, with children with higher typical screen time more likely to be overweight or obese than those with lower screen time. As shown in Figure 5‑3, 40-41% of children with over 21 hours per week of screen time were overweight or obese compared with 34% of children with between 14 and 21 hours, and 25% of children with less than 14 hours.
Socio-economic variations are again notable here, and they may be driving some of the differences in rates of overweight and obesity. Children in lower income groups were considerably more likely to have higher weekly screen time than children in higher income groups. For example, 49% of children in the lowest income group were reported to have 21 hours or more of screen time per week compared with 24% of children in the highest income group.`
Figure 5‑3 Children's BMI classification at age 10 by typical weekly screen time
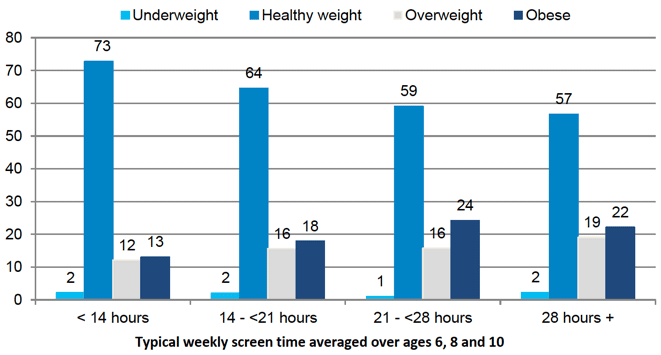
A factor which may influence levels of screen time and thus overweight and obesity, is whether or not a child has a television in their bedroom. The analysis found that children with a television in their bedroom were more likely to be overweight or obese than those without (Figure 5-4).
Figure 5‑4 Children's BMI classification at age 10 by whether has a TV in bedroom
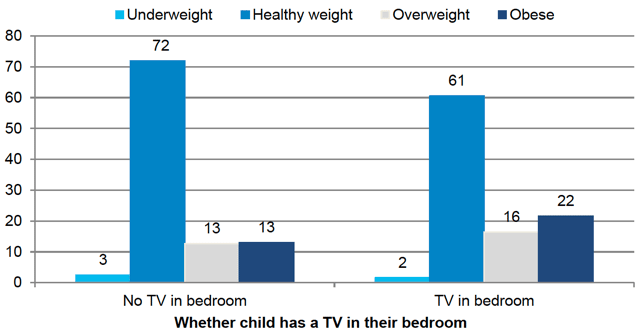
Children in more disadvantaged circumstances were significantly more likely than those in more advantaged circumstances to have a television in their bedroom which may be affecting the relationship with BMI. Four out of five children (82%) in the lowest income households had a television in their bedroom compared with just over two out of five (44%) children in the highest income households.
5.5.3. Unsupervised time
Differences in BMI were also analysed according to a measure of parental supervision. The hypothesis is that parents who report higher levels of supervision generally may extend that level of regulation to aspects of their child's life associated with their health, including overweight and obesity – for example their diet and levels of physical activity.
To measure level of supervision, parents were asked how often the child spent time with his/her friends, but without adults, doing things like playing in the park, going to the shops or just hanging around after school. There was no association between frequency of unsupervised time and BMI at age 10.
5.5.4. Sleep
A number of research studies have found an association between lack of sleep and obesity (Reilly et al, 2005; Taveras et al, 2008). In GUS, sleep duration is measured by asking parents what time the child is typically in bed and ready to sleep and what time the child wakes up on a school day. Duration of sleep was measured at ages 6, 8 and 10 and compared with the recommended sleeping time for children at these ages[19]. A variable was created which indicated whether or not the child was reported to have less than the recommended amount of sleep for at least two out of the three age points.
Children who were reported to have had less than the recommended amount of sleep were a little more likely to be overweight or obese than those who did get the recommended amount of sleep (Figure 5‑5). Of those who had less than the recommended amount of sleep at two or three ages, 37% were overweight or obese at age 10 compared with 32% of those who had the recommended amount of sleep.
Figure 5‑5 Children's BMI classification at age 10 by whether child gets enough sleep
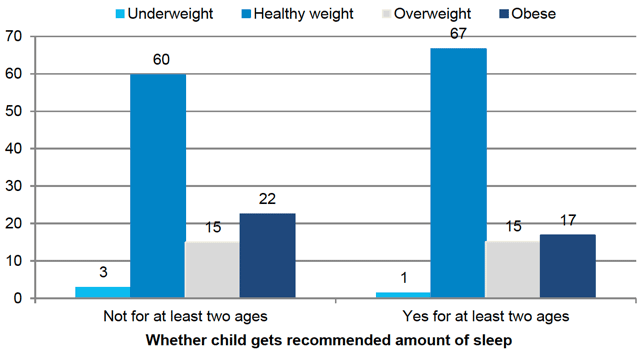
Variations in whether children got less than the recommended amount of sleep by social background may be influencing the relationship with BMI. Forty percent of children in the lowest income group were reported to have had less than the recommended amount of sleep compared with 30% of those in the highest income group.
5.6. Perceived body size and body image
5.6.1. Parent and child perceptions of weight
A parent's perception of their child's weight status and recognising the potential health risks from being overweight or obese is important in influencing the facilitation or 'modelling' of healthy behaviours (i.e. when parents themselves undertake health promoting activities and behaviour). Similarly, if children themselves do not recognise that they are overweight or obese they may be less inclined to take action to reduce their weight or prevent further increases in BMI.
When children were aged 10, parents were asked how they would describe their child's weight from four categories: underweight, normal weight, somewhat overweight or very overweight. Similarly, children were themselves asked whether they thought their body was much too thin, a bit too thin, about the right size, a bit too fat or much too fat.
The results in Table 5‑2 show that whilst many parents accurately classify their child's weight, a significant proportion whose children are overweight or obese tend to think their children are a normal weight. For example, 35% of parents whose children were obese and 88% of those whose children were overweight perceived them to be of normal weight.
Table 5‑2 Parental perception of child's weight by BMI classification at age 10
| BMI classification at age 10 | |||||
|---|---|---|---|---|---|
| Underweight | Healthy weight | Overweight | Obese | All | |
| % | % | % | % | % | |
| Parent's perception of child's weight | |||||
| Underweight | 29 | 7 | - | - | 5 |
| Normal weight | 71 | 92 | 88 | 35 | 80 |
| Somewhat overweight | - | 1 | 12 | 63 | 14 |
| Very overweight | - | - | - | 2 | <1 |
| Unweighted bases | 50 | 1813 | 408 | 476 | 2806 |
As shown in Table 5‑3, 63% of children who were obese and 78% of those who were overweight perceived themselves to be 'about the right size'. This may suggest that a sizeable proportion of children who may be at risk of poorer health outcomes due to overweight or obesity may not be aware of this. 16% of healthy weight children thought they were either a bit or much too thin.
Table 5‑3 Child's perception of his/her weight by BMI classification at age 10
| BMI classification at age 10 | |||||
|---|---|---|---|---|---|
| Underweight | Healthy weight | Overweight | Obese | All | |
| % | % | % | % | % | |
| Child's perception of weight | |||||
| Much too thin | 10 | 4 | 1 | 1 | 3 |
| A bit too thin | 36 | 12 | 2 | 1 | 9 |
| About the right size | 54 | 80 | 78 | 63 | 76 |
| A bit too fat | - | 4 | 18 | 30 | 11 |
| Much too fat | - | 1 | 5 | 1 | |
| Unweighted bases | 49 | 1803 | 407 | 472 | 2770 |
Parents' perceptions of their child's weight were compared with the child's view (Table 5-4). Other than for healthy weight, there was no overwhelming correspondence between what parents and children reported. Whilst for 80% of cases where a parent perceived their child to be normal weight the child also deemed themselves to be about the right size, only in 40% of cases where a parent perceived the child to be overweight did the child deem themselves too fat.
Table 5‑4 Child's perception of his/her weight by parent's perception of child's weight
| Parent's perception of child's weight | |||
|---|---|---|---|
| Underweight | Normal weight | Overweight | |
| % | % | % | |
| Child's perception of weight | |||
| Too thin | 43 | 12 | 1 |
| About the right size | 56 | 80 | 59 |
| Too fat | 1 | 8 | 40 |
| Unweighted bases | 144 | 2241 | 378 |
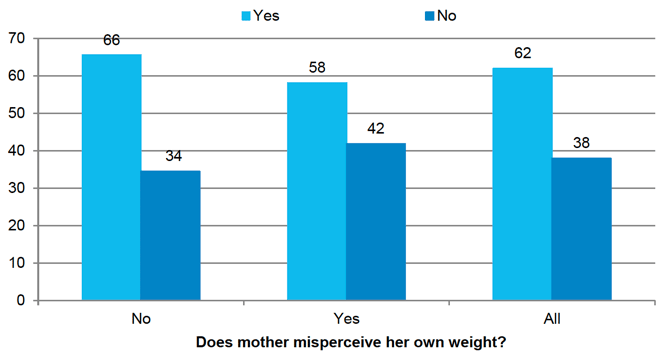
Further analysis was conducted to examine whether mothers who misperceived their own weight were more likely than those who correctly perceived their own weight to misperceive their child's weight (Figure 5-6). The majority of mothers correctly identified their child's weight status at age 10, 62% having done so. Even amongst mothers who incorrectly perceived their own weight status, most (58%) accurately identified their child's status. However, those mothers who misperceived their own weight were more likely than those who correctly perceived their own weight to judge their child's weight incorrectly. Forty-two percent of mothers who were incorrect about their own weight were also incorrect about their child's weight compared with 34% of mothers who were correct about their own weight.
Figure 5‑6 Whether mother correctly classified child's weight at age 10 by mother's classification of her own weight
5.6.2. Child's satisfaction with body image
The relationship between body satisfaction and increasing weight status has been demonstrated in a number of research studies. In GUS, body satisfaction was measured by asking children how they felt about the way they look. A four-point response set was used ranging from 'very happy' to 'not at all happy'.
The vast majority of children were either very (59%) or quite (34%) happy with the way they looked. There were no statistically significant differences by sex, with similar proportions of boys and girls being happy and unhappy with how they look.
Figure 5‑7 Children's BMI classification at age 10 by body satisfaction
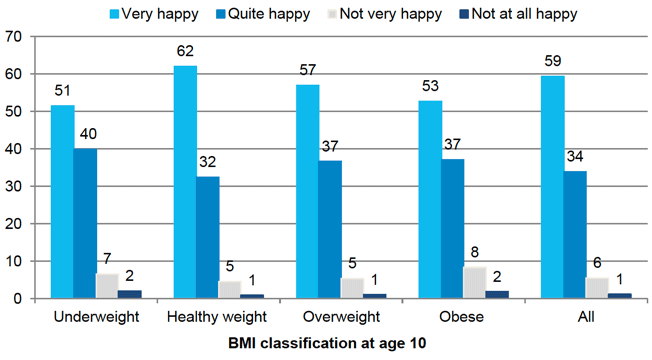
Table 5‑5 Body satisfaction by child's BMI status and sex
| Child's BMI classification at age 10 | ||||
|---|---|---|---|---|
| Underweight | Healthy weight | Overweight | Obese | |
| % | % | % | % | |
| Body satisfaction - boys | ||||
| Very happy | * | 60 | 55 | 57 |
| Quite happy | * | 35 | 38 | 33 |
| Not very happy | * | 5 | 6 | 8 |
| Not at all happy | * | 1 | - | 1 |
| Body satisfaction - girls | ||||
| Very happy | * | 64 | 59 | 48 |
| Quite happy | * | 30 | 35 | 41 |
| Not very happy | * | 4 | 5 | 8 |
| Not at all happy | * | 1 | 2 | 2 |
| Unweighted bases – boys | 27 | 901 | 210 | 247 |
| Unweighted bases - girls | 22 | 901 | 199 | 226 |
*Base sizes are too small to report.
However, body satisfaction did vary by weight status. As shown in Figure 5‑7, most children across all BMI groups were happy with how they looked. However, children who were obese were less likely to be very happy and more likely to be not very happy than healthy weight children (53% compared with 62% and 8% compared with 5% respectively). Differences in body satisfaction between children who were overweight and healthy weight were not statistically significant.
There was no statistically significant difference in the relationship between weight status and body satisfaction between boys and girls (Table 5-5). For both groups, most children were happy with how they looked across each weight classification. The data suggests that girls who are obese may be less likely to be very happy with how they look than boys who are obese (48% compared with 57%); however the difference is not statistically significant. Almost identical proportions of obese boys and girls were not happy with how they looked (9% and 10%).
5.7. Multivariable analysis of factors predicting overweight or obesity at age 10
Analysis in the previous sections has shown relationships between a range of children's characteristics, circumstances and experiences and their weight status at age 10. In particular, section 4 demonstrated the considerable socio-economic differences in levels of overweight and obesity. The subsequent analysis of other factors – such as how often children eat breakfast - suggested that it may be the underlying variations in these factors by social background which is driving the relationship with overweight and obesity. In other words the association between eating breakfast and weight status exists because those children who eat breakfast less often tend to be from more disadvantaged backgrounds, the same children who are more likely to be overweight or obese.
To control for these inter-connected relationships between social background characteristics and other factors, multivariable logistic regression analysis was undertaken. This allows some insight into those factors which are independently associated with overweight and obesity at age 10.
The analysis was conducted in a series of steps:
- First, a regression model was run which included only demographic (sex, ethnicity) and socio-economic variables (household income, parental educational qualifications, social class and area deprivation)
- Second, weight status at age 6 was added to a model containing only significant variables from amongst the demographic and socio-economic variables
- Third, a separate model was run including those other factors found to be statistically significantly associated with weight status in the cross-sectional analysis conducted earlier in section 5 (birth weight, maternal BMI, frequency at which breakfast eaten, screen time, TV in bedroom, sleep).
- Finally, a combined model was then run including the statistically significant variables from the first three steps.
In all models, the outcome variable was whether or not the child was overweight or obese at age 10.
Table 5‑6 Factors predicting overweight/obesity at age 10 – SES and demographic variables – summary results[20]
| Sig. | Odds ratio | |
|---|---|---|
| Highest parental educational qualification (ref: degree level) | < .001 | |
| No qualification | 1.822 | |
| Lower level Standard Grades and Vocational qualifications / other qualifications | 2.238 | |
| Upper level Standard Grades and Intermediate Vocational qualifications | 1.397 | |
| Higher grades and Upper level vocational qualifications | 1.562 | |
| Area deprivation – quintiles (ref: 1 - least deprived 20% of areas) | < .05 | |
| 2 | 1.168 | |
| 3 | 1.411 | |
| 4 | 1.571 | |
| 5 Most deprived | 1.515 | |
| Child sex (ref: female) | NS | |
| Child ethnicity (ref: White) | NS | |
| Household annual equivalised income (ref: Top quintile >=£39,216) | NS | |
| Socio-economic classification (ref: Managerial and professional) | NS |
Pseudo R squared = .04
A summary of results from the first step are provided in Table 5‑6. Of the various demographic and socio-economic variables considered, only two - parent's level of education and area deprivation - remained significant after controlling for differences in the other variables. The findings indicate that, after controlling for other demographic and socio-economic differences, compared with children whose parents were degree-educated, those whose parents had lower qualifications were more likely to be overweight or obese at age 10. Similarly, compared with children living in the 20% least deprived areas, those living in the three most deprived quintiles were more likely to be overweight or obese.
Table 5‑7 provides a summary of the results of the regression analysis from step two when BMI at age 6 is added alongside parent's level of education and area deprivation.
Table 5‑7 Factors predicting overweight/obesity at age 10 – combined age 6 weight status and SES variables – summary results[21]
| Sig. | Odds ratio | |
|---|---|---|
| Child's BMI classification at age 6 (ref: underweight/healthy weight) | < .001 | |
| 1.00 Missing | 3.045 | |
| 3.00 Overweight | 8.307 | |
| 4.00 Obese | 44.692 | |
| Highest parental educational qualification (ref: degree level) | < .05 | |
| No qualification | 1.632 | |
| Lower level Standard Grades and Vocational qualifications / other qualifications | 2.071 | |
| Upper level Standard Grades and Intermediate Vocational qualifications | 1.352 | |
| Higher grades and Upper level vocational qualifications | 1.314 | |
| Area deprivation – quintiles (ref: 1 - least deprived 20% of areas) | < .05 | |
| 2 | 1.128 | |
| 3 | 1.362 | |
| 4 | 1.461 | |
| 5 Most deprived | 1.585 |
Pseudo R squared = .36
Being overweight, and in particular, being obese, is very strongly associated with being overweight or obese at age 10 after controlling for differences in social background. For children who were overweight at age 6 and for those who were obese, the odds of being overweight/obese at age 10 were 8 and 45 times higher than those for children who were a healthy weight or underweight at age 6.
Even after controlling for weight status at age 6, social background remained an important predictor of overweight or obesity at age 10. Lower parental qualifications and higher area deprivation were each associated with overweight or obesity at age 10.
When running the third step, all variables except the child's sleep duration were found to be statistically significantly associated with overweight/obesity at age 10 (Table 5-8). These included: a birthweight of 4kg or more (compared with a birthweight of 3 to 3.499kg); having a mother who was overweight or obese; eating breakfast less often than 'always'; screen time of 14 hours or more (compared with less than 14 hours) and a having a TV in the child's bedroom. Of the factors considered, having a mother who was obese had the strongest association with the child being overweight or obese at age 10. Notably, having missing data on screen time was also strongly associated with overweight/obesity. Whilst this may suggest that those who did not provide a response to this question are perhaps more likely to have children with high screen time durations, only a relatively small number of cases (n = 46) in the model fell into this category. Therefore any such interpretation should be treated with caution.
After the statistically significant socio-economic and other factors were combined into a single model along with age 6 weight status, neither area deprivation, parental level of education nor birthweight were associated with overweight/obesity at age 10. The remaining variables all showed some independent association with overweight/obesity, as shown in Table 5-9.
Table 5‑8 Factors predicting overweight/obesity at age 10 – Other variables – summary results[22]
| Sig. | Odds ratio | |
|---|---|---|
| Birth weight (ref: 3 to 3.499kg) | < .05 | |
| < 2.5 kg (low birth weight) | .631 | |
| 2.5 - <3kg | .996 | |
| 3.5 - <4 kg | 1.145 | |
| 4 kg or above | 1.484 | |
| Maternal BMI (ref: less than 25) | < .001 | |
| Missing | 2.109 | |
| 25 to less than 30 | 1.375 | |
| 30 and over | 2.772 | |
| How often child eats breakfast (ref: always) | < .05 | |
| Never | .888 | |
| Occasionally | 1.476 | |
| Quite often | 1.376 | |
| Average weekly screen time (ref: less than 14 hours) | < .001 | |
| Missing | 3.377 | |
| 14 - <21 hours | 1.340 | |
| 21 - <28 hours | 1.753 | |
| 28 hours or more | 1.665 | |
| Whether child has TV in bedroom (ref: No) | < .001 | |
| Yes | 1.397 | |
| Whether child gets recommended amount of sleep | NS |
Pseudo R squared = 0.10
Table 5‑9 Factors predicting overweight/obesity at age 10 – combined age 6 BMI, SES, demographic and other variables – summary results[23]
| Sig. | Odds ratio | |
|---|---|---|
| Child's BMI classification at age 6 (ref: underweight/healthy weight) | < .001 | |
| 1.00 Missing | 2.609 | |
| 3.00 Overweight | 8.099 | |
| 4.00 Obese | 43.231 | |
| Maternal BMI (ref: less than 25) | < .001 | |
| Missing | 1.647 | |
| 25 to less than 30 | 1.240 | |
| 30 and over | 2.297 | |
| How often child eats breakfast (ref: always) | < .05 | |
| Never | 0.956 | |
| Occasionally | 1.533 | |
| Quite often | 1.552 | |
| Average weekly screen time (ref: less than 14 hours) | < .001 | |
| Missing | 4.088 | |
| 14 - <21 hours | 1.329 | |
| 21 - <28 hours | 1.638 | |
| 28 hours or more | 1.661 | |
| Whether child has TV in bedroom (ref: No) | < .01 | |
| Yes | 1.303 | |
| Highest parental educational qualification (ref: degree level) | NS | |
| Area deprivation – quintiles (ref: 1 - least deprived 20% of areas) | NS | |
| Birth weight (ref: 3 to 3.499kg) | NS |
Pseudo R squared = 0.40
Weight status at age 6 remains the strongest predictor of overweight/obesity at age 10 with odds ratios similar to those noted in Table 5‑7. Having a mother who was obese when the child was aged 6 was the next strongest predictor. After controlling for weight status at age 6 and social background, the odds of children with an obese mother being overweight/obese at age 10 were 2.3 times higher than the odds for children whose mother was a healthy weight (or underweight, BMI < 25). Average weekly screen time, only occasionally eating breakfast, and whether the child had a TV in their bedroom all remained statistically significantly associated with overweight/obesity at age 10.
Overall, the explanatory power of the combined model was moderately strong with around 40% of the variance in overweight/obesity being explained. The majority of this is accounted for by weight status at age 6. The additional variables explain only a small additional amount of difference in children's levels of overweight/obesity.
Contact
Email: Ewan Patterson