A Fairer Scotland for Older People: framework for action
This framework has been developed to challenge the inequalities older people face as they age and to celebrate older people in Scotland.
Accessing public and other services
Older people want action to ensure they have access to:
- the public services they need
- adequate numbers of care sector workers in the wake of Brexit
- the health and social care services they require, including mental health
- opportunities to influence how health and social care integration is organised and delivered.
Supporting positive engagement – what government and stakeholders are doing, and will do
When we speak of services in this chapter, we refer to services in their widest sense – so not just central and local government services, but also those accessible from the voluntary and private sectors that have been identified as priorities by older people, such as banking and healthcare.
Supporting community facilities
Keeping connected with communities and everyday activities is one of the means by which health and wellbeing can be supported. Older people speak of their concerns about community facilities – things like libraries, parks, local shops, meeting places, and banking services – being reduced or removed.
The Scottish Government’s A Connected Scotland[31] strategy for tackling social isolation and loneliness and building stronger social connections recognises the importance of libraries to communities. That’s why we’re investing in the Public Library Improvement Fund to support innovative ways for people to use public libraries, and are also taking forward implementation of the first strategy for public libraries in Scotland. We will work to ensure our approach to increasing access includes hard-to-reach groups and considers further how to build on what libraries already offer as community hubs.
We Will
Engage with key partners on Ambition & Opportunity: a strategy for public libraries in Scotland 2015–202032 in recognition of libraries as vital public spaces for older people.
Older people, particularly (but not exclusively) those in rural areas, have expressed great concern about the closure of local bank services as banking moves increasingly to online platforms (similar issues arise in other services, such as post offices). The Scottish Government shares concerns on this issue and has lobbied strongly for bank closure reversals, but as regulation of the financial system remains a matter reserved to the UK Parliament in Westminster, our influence in this area is limited. We will nevertheless continue to support action for a more diverse banking sector and raise issues of local bank branch closures with senior executives in the sector.
We Will
Continue to highlight the damaging impact of financial services reductions in local services to banks and post offices to the UK Government.
Continue to work with the financial services sector to mitigate the impact of service reform on older people.
For those who experience reduced mobility in older age and require support with, for example, accessing toilet facilities, the Scottish Government is fully committed to the continuing provision of Changing Places toilets. This is an important part of the A Fairer Scotland for Disabled People: delivery plan[33], particularly in supporting our ambition that “places should be accessible to everyone.”
On 20 February 2019, the Scottish Government announced funding of £45,000 for PAMIS (Promoting a More Inclusive Society) to design and build a second mobile Changing Places Toilet to support individuals and families to be able to get out and experience what Scotland has to offer, particularly in more remote regions.
We also recognise that good health and wellbeing and the ability to access health services are vitally important to older people. We want to ensure that person-centred care planning is enabled, and documentation of anticipatory care plans ensured.
We Will
Continue to implement the new GP Contract by transferring services so that GPs can focus on the work only they can do. This will allow for longer consultations for patients where they are needed, particularly for complex care of patients with multi-morbidity, including comorbidity of physical and mental health issues.
Revise and update the Palliative Care Direct Enhanced Service, which resources practices to learn from and improve the palliative care they provide, from April 2019.
Through our National Primary Care Workforce Plan, we have set out how we will assist primary care services effectively to respond to the changing and growing needs of the ageing population and the anticipated changes in the way services will be developed to meet these needs.
We Will
Strengthen multidisciplinary teams to deliver an enhanced and sustainable workforce to improve patient outcomes in primary care settings.
Work with partners to ensure that better-quality and more timely data is developed to drive effective local and national workforce planning for primary care.
We know demand on primary care services inevitably will rise, given increasing levels of multi-morbidity among an ageing population and our strategic goal of shifting care from hospitals to community and home or homely settings. This requires a GP workforce that is both sufficient to meet demand and flexible enough to address changing needs.
We Will
Increase the number of GPs working in Scotland by at least 800 by 2028 through our recruitment and marketing campaign that will launch this year.
Continue to invest in training and education of general practice nurses, providing nursing care across the life cycle. This includes supporting the management of long-term conditions and supporting people with complex conditions or who are frail as part of integrated community teams.
We must create the conditions that facilitate more meaningful conversations between people and their healthcare professionals, and create the conditions that help people make informed choices about their treatment and care options, based on what matters most to them. The shared vision for Scotland is that:
‘By 2025, everyone who provides healthcare in Scotland will demonstrate their professionalism through the approaches, behaviours and attitudes of Realistic Medicine.’
Dr Catherine Calderwood,
Chief Medical Officer for Scotland[34]
Realistic medicine is about:
- listening to and understanding patients’ problems and preferences
- sharing decisions between healthcare professionals and their patients
- ensuring that patients have all the understandable information they need to make an informed choice
- moving away from the ‘doctor knows best’ culture to ensure a more equal partnership with people
- supporting healthcare professionals to be innovative, to pursue continuous quality improvement and to manage risk better
- reducing the harm and waste caused by both over-provision and under-provision of care
- identifying and tackling unwarranted variation in clinical practice.
Professionals and patients sharing decisions will ensure people have the information they need to make an informed choice about their treatment and care, meaning they will receive care they really value. Shared decision-making can also reduce the harm and waste caused by overtreatment and help redirect wasted resources to more appropriate care.
In October and November 2018, we held Scotland’s first ever Citizens’ Jury, a recognised tool for public engagement, on a health topic. Over three weekends, the Jury considered the question: ‘What should shared decision-making look like and what needs to be done for this to happen?’
The Jury presented recommendations to the Chief Medical Officer in February 2019 on what needs to be done to support professionals and the public to practise shared decision-making[35]. The Scottish Government committed at the outset to carefully consider the recommendations and reply to all, either with a commitment to action or an explanation of why any recommendations cannot be taken forward.
We Will
Develop an action plan to take forward the Citizens’ Jury recommendations to help promote and support shared decision-making to help ensure people receive healthcare they really value.
Promoting transport links
Transport is a key area in which the Government and partners have been able to take positive action to promote older people’s engagement with, and contributions to, communities.
We are committed to providing free bus travel to older and disabled people, helping them to lead more connected, healthier and happier lives. Since the scheme began in 2006–2007, we have provided budgets of over £2 billion to fund concessionary travel. The average benefit per year is about £260 for a person eligible to use the Scotland-wide Free Bus Travel Scheme for Older and Disabled People. There are close to 1.4 million cardholders in Scotland, of whom 90% hold a pass on the basis of age. The scheme as a whole was responsible for around 141.8 million journeys in 2017–2018.
We consulted in 2017 on how to ensure the sustainability of concessionary travel. The scheme is greatly valued and works well for cardholders for a number of reasons, including making financial savings, reducing isolation, engendering a sense of greater independence and increasing confidence in their own ability to travel. Cardholders see the scheme as having improved their mental and physical wellbeing. Additional journeys are being made by cardholders that would not otherwise have been made. Respondents with a disabled or visual impairment card cited greater independence as a key benefit.
Community transport plays an important role in providing flexible and accessible community-led solutions in response to unmet local transport needs, and often represents the only means of transport for many vulnerable and isolated people, often older people or people with disabilities. Typically, community transport includes voluntary car schemes, community bus services, school transport, hospital transport, dial-a-ride, wheels to work and group hire services. Most community transport initiatives are demand-responsive, taking people from door to door, but a growing number are scheduled services along fixed routes where conventional bus services aren’t available.
These types of services help people access the services they need, particularly in rural areas where public transport can be limited. They are of particular benefit to older and disabled people who have difficulty accessing conventional bus services. Our research tells us that community transport offers health benefits, including enabling access to health services and ensuring fewer missed appointments, and also that it has wider economic benefits for local communities, providing jobs and supporting volunteering and training opportunities.
Bus usage was highest for people aged 60 to 79; in rural areas, however, older people were less likely to have used a bus in the previous month
Percentage who had travelled by bus in the previous month by urban/rural classification
15% of people aged 50 to 79 living in remote rural areas had used a bus in the past month
In contrast, about 70% of people aged 60 to 79 living in large urban areas had used a bus
Source: Transport and Travel in Scotland 2013–17
Funding is provided to local authorities for community transport and demand-responsive transport services, and local authorities allocate the funding to best meet local needs and circumstances. We are supporting community transport through funding to the Community Transport Association in Scotland to develop the sector and provide a minibus driver and instructor training programme in Scotland.
The Bus Service Operators Grant scheme is a discretionary grant that subsidises commercial and community bus routes. This is an annual subsidy of over £50 million comprising a core payment and an incentive for the operation of green, environmentally-friendly buses. The Grant contributes to the maintenance of the nation’s bus networks for the benefit of passengers. The core payment aims to support operators to keep fares at affordable levels and provide networks more extensive than would otherwise be the case.
We currently are reviewing the National Transport Strategy. The new National Transport Strategy will be published by the end of 2019 and will set out a compelling vision for transport for the next 20 years. As part of the review, national working groups involving a range of key stakeholders were convened to examine significant themes relating to transport. One of these groups, of which Age Scotland and the Mobility and Access Committee for Scotland were members, looked at the theme of ‘Tackling Inequality’, and covered a range of concerns expressed by older people (among others) around accessibility to public transport and affordability. The group submitted a report with suggested policies to underpin the new National Transport Strategy, and these suggested policies are currently being assessed for fitness to be included in a formal public consultation on the new strategy commencing May 2019.
In addition to the report from the working group, extensive stakeholder engagement with older people took place in 2018 on the National Transport Strategy review. Workshops convened jointly by Transport Scotland and Age Scotland were held throughout Scotland to explore the specific concerns, opportunities and challenges faced by older people in relation to transport. Feedback from these workshops will help to inform thinking around the production of the draft strategy.
We Will
Engage directly with the Older People’s Strategic Action Forum to shape the next National Transport Strategy as part of our consultation process.
Promoting self-directed support
The Social Care (Self-directed Support) (Scotland) Act 2013 enshrines in law that people who are eligible for social care support must be involved in decisions about what their support looks like and how it is delivered. This re-balancing of power between services and the individual seeks to ensure that the supported person can direct their care in a way that focuses on the aspects of life that matter to them.
The National Self-directed Support Strategy 2010–2020[36] is a joint Scottish Government and Convention of Scottish Local Authorities (COSLA) 10-year plan dedicated to driving forward the personalisation of social care in Scotland. COSLA and the Government jointly approved the 2016–2018 self-directed support implementation plan to help with the changes needed to introduce, use and roll-out the approach in full across Scotland, and to support people to get the choice and control set out in the legislation. The full implementation of self-directed support is integral to the developing programme of adult social care reform.
We Will
Publish a national implementation plan (2019– 2021) to embed self-directed support in social care nationally and locally, so that older people can make the decisions that matter to them in terms of being supported to maintain their social connections.
Under the Support in the Right Direction 2021 (SiRD2021) programme[37], we are funding 31 projects delivering direct and local independent support across 31 local authority areas. These projects will help older people and their carers make informed decisions and plans for their social care and work towards maximising their choice, control and flexibility over those arrangements. Over £7.2 million will be invested in projects from October 2018 to March 2021, with work with relevant local authorities ensuring that more people across Scotland who require social care are engaged, informed, included and empowered to make choices about their support.
Integrating health and social care
A number of innovative ways of delivering healthcare in rural areas are being developed and tested with Scottish Government support. Working with NHS boards, we are developing networks between rural and urban hospitals to support doctors working in rural areas to maintain and develop their skills, ensuring that patients can access and receive safe care. Access to health and care services is also being enhanced through technological means, including the Attend Anywhere browser-based video consultation tool, which allows access to routine appointments from home or anywhere through a smartphone/tablet.
Free Personal Care for people aged 65 and over in Scotland currently benefits around 76,000 older adults. In 2016–2017, just under 46,000 older people received personal care in their own homes and just over 30,000 in residential care homes. The Scottish Government has been working with the Convention of Scottish Local Authorities and other partners to improve the fairness and consistency of charging for social care, and Free Personal Care will be available to those under 65 who are assessed as requiring it by 1 April 2019.[38]
Prevention programmes for improving health in later life, particularly for those with lower health status, will be vital to enabling people to live in good health and wellbeing in older age. Shortening the amount of ill health in later life is clearly possible,[39] not only through measures in the health and social care sector alone, but also by a wide range of sectors – education, housing, transport, work and pensions, benefits and leisure sectors, for instance – coming together with health and social care to put in place the opportunities and supports people need to keep well and avoid ill health.
Developing a national programme to support local reform of adult social care
Together with the Convention of Scottish Local Authorities, we have been working with people who use social care support, carers, people who work in social work and social care, local and national organisations, health and social care partnerships, councils and other professional sectors to co-develop a national programme to support local reform of adult social care.
Scots are enjoying longer lives, which often are accompanied by more complex care needs. Demand for social care is growing faster than our traditional services were designed for. The programme is bringing together different perspectives, skills and experiences to agree what needs to change for people to be able to access the right support into the future and how to make those changes. It will raise awareness of the value of social care for individuals and our society and identify where and how national action can build on, and support, existing and planned work driven by local communities and health and social care partnerships.
The People-led Policy Panel is a new engagement framework consisting of 50 members, with a core group of 19 people who meet on a more regular basis. The diverse group members all have lived experience of adult social care support, including carers. They have experience of different kinds of social care for different purposes and are from a spread of areas across Scotland. The Panel will be engaging with other citizen-led groups and forums to get more in-depth insights on specific perspectives or issues. The views and experiences of older people will be directly involved in this work.
We Will
Work with the People-led Policy Panel to shape what the national programme to support local reform of adult social care will focus on, and the projects and activities within it.
The Adult Support and Protection (Scotland) Act 2007 gives local authorities powers to intervene to prevent harm and abuse to adults who may be vulnerable. The Act places duties on local authorities, health boards, police and others to cooperate to protect adults to reduce and prevent the risk of harm. It covers all types of harm, physical, psychological and sexual abuse, neglect and self-harm. An inspection of six adult support and protection partnerships by the Care Inspectorate and Her Majesty’s Inspectorate of Constabulary in Scotland in 2018 found strengths and areas for improvement.
We are developing an improvement plan to strengthen adult support and protection across Scotland, with the work to be delivered over the next three years.
We Will
Formally engage with the Older People’s Strategic Action Forum in 2019 so that the experiences of older people are reflected in and inform our improvement programme for adult support and protection.
In partnership with the Convention of Scottish Local Authorities, care providers, integration authorities and the Care Inspectorate, we will be undertaking work looking at the future role of care homes in the context of health and social care integration. This will be taken forward as part of the national programme to support local reform of adult social care.
Safeguarding against the effects of Brexit on health and social care services
The Scottish Government shares older people’s concerns about the effects of the UK exiting the European Union (EU) (Brexit) on recruitment and retention of staff in the health and care sector. While the long-term implications of Brexit cannot be predicted precisely, very real impacts have already been felt, with the Nursing and Midwifery Council reporting a massive decline in the number of registration applications from nurses and midwives from the European Economic Area and Switzerland over the year immediately following the EU referendum. Our National Health and Social Care Workforce Plan: part three[40] sets out approaches to ensuring we have the workforce Scotland needs across health and social care, and these approaches will seek to mitigate the impacts of Brexit as these emerge. The next iteration of the workforce plan will be the publication of the Integrated Health and Social Care Workforce Plan this year.
What we do know for sure is that Scotland’s health and social care sector benefits enormously from the contribution of staff from across the EU. Around 13,000 citizens from other EU nations currently work in health and social care in Scotland, comprising 3.5% of the sector’s overall workforce. In social care alone, 7.3% of registered nurses and 5.5% of adult social care staff come from non-UK EU nations.
We greatly value EU citizens and their wider contribution to our society, and we are working to ensure their rights and place in our nation are protected. This means we need to retain our ability to recruit staff from inside and outside the EU, with cross-border mobility and freedom of movement being essential components. To this end, we are absolutely committed to supporting EU nationals to continue to live and work in Scotland.
Addressing mental health issues in older age
Mental health is an absolute priority for this government, reflected in the appointment of a specific minister for mental health. Our new 10-year Mental Health Strategy 2017–2027[41] has a strong focus on equalities, recognising the enormous impact mental health can have on health, wellbeing and quality of life in older age.
Our vision for the strategy is of a Scotland where people can get the right help at the right time, expect recovery, and fully enjoy their rights, free from discrimination and stigma. Our annual Mental Health Forum, the next of which is due in December 2019, provides an opportunity for stakeholders to track progress on the actions in the strategy and to help develop new actions in future years to help meet our ambitions.
A major part of mental health services in Scotland is enabling access to psychological therapies, a range of interventions designed to help people understand and make changes to their thinking, behaviour and relationships to relieve distress and improve functioning. The strategy commits the Scottish Government to offer national support to NHS boards to ensure no unwarranted variation across the country to mental health and psychological therapy services, and no lower levels of access to psychological therapies for people over the age of 65, numbers of which are now included in quarterly waiting times reports for psychological therapies from integrated joint boards.
We Will
Work closely with NHS boards throughout 2019 to improve provision of, and access to, mental health services, including psychological therapy for people over the age of 65.
Supporting people with dementia and their carers
There is an estimated number of up to 90,000 people living with dementia in Scotland, the vast majority of whom are over 65. Since 2007, we have taken priority action on dementia, with our third National Dementia Strategy 2017–2020 published in 2017[42]. Many people are developing dementia into very old age when they are already living with long-term or chronic conditions. The integration of health and social care in Scotland is designed to enable more older people with multiple conditions to stay living well in their own homes for longer and retain an active part in their communities as far as possible. Ongoing national work on dementia will include engagement with this framework’s agenda.
We Will
Coordinate national work on dementia and this framework to ensure that older people with dementia retain a visible and active part in their communities.
Engage with the Older People’s Strategic Action Forum on our ongoing national work on dementia to ensure older people’s representative groups are linked in to the current dementia strategy.
Planning the delivery of integrated services
Health and social care have been integrated to change the way key services can be accessed and delivered, with greater emphasis on supporting people in their own homes and communities and less inappropriate use of hospitals and care homes. The people most affected by these developments, and for whom the greatest improvements can be achieved, are older people.
The Public Bodies (Joint Working) (Scotland) Act 2014 provides the framework under which health and social care integration is taken forward. Integration authorities are required to engage and consult with a range of stakeholders and work with local communities and professionals to improve outcomes and sustainability.
A key element of the Act is that integration authorities are required to engage and consult with a range of stakeholders, working with local communities and professionals to improve outcomes and sustainability. It is important that the voices of those in communities, including older people’s, are heard on matters relating to health and social care integration. This takes place primarily at locality and strategic planning group level, but improvements in how engagement and consultation are taken forward are important in supporting the appropriate redesign and delivery of services that will meet older people’s, and others’, needs within their communities.
At national level, the Ministerial Strategic Group for Health and Community Care has proposed a look at how local systems undertake meaningful and sustained engagement to ensure this is the central pillar of how services are planned and delivered.
We Will
Engage with the Older People’s Strategic Action Forum in 2019 on matters relating to health and social care integration, and the current engagement and consultation practices of local partnerships.
Produce revised statutory guidance on local community engagement and participation based on existing good practice, which will apply across health and social care bodies. This will ensure engagement is central to achieving the scale of change and reform required via health and social care integration, and is an ongoing process that is not undertaken only when service change is proposed. The guidance will be published by the end of 2019.
Ensure carers and representatives of people using health and social care services are supported by their local partnerships to enable meaningful engagement with their constituencies. This would include, for example, receipt of integration joint board papers with enough time for meaningful engagement and allowing people using services time to respond to issues raised. It would also include paying reasonable expenses for attending meetings.
Supporting people with sensory impairment
The Scottish Government is committed to supporting children and adults who have deafness, sight loss and dual sensory loss to access the health and social care they need through its See Hear strategy.[43]
The term sensory impairment can apply to several different conditions. The strategy reflects this and works across a wide spectrum of categorisations and all age groups, supporting people who identify with, or who have a diagnosis of, auditory, visual or dual sensory loss.
The strategy’s recommendations are delivered through local partnerships involving local authority, health and third sector organisations who are responsible for identifying local priorities and developing workstreams, timescales and implementation plans based on local priorities and need.
There is an estimated 850,000 people with hearing loss in Scotland, one in six of the population, and of those, 70% are over 70. This figure is projected to increase by 50% by 2034.
Most services for those with hearing loss are provided from acute hospital settings, with only 15% of all activity classed as community-based provision. We are seeking to improve community provision of support for people who use hearing aids, delivering more accessible and integrated services and providing diagnostic services in premises closer to people’s homes. This is why we are establishing two pilots that will explore the delivery of enhanced community audiology services in a general practice setting. The pilots, which link with third sector providers, will be held in NHS Ayrshire and Arran and NHS Tayside and are set to commence early in 2019, running for 12 months.
We Will
Work with stakeholders to deliver enhanced community audiology services and testing.
Use evidence from pilots exploring the delivery of enhanced community audiology services in a general practice setting to inform next steps in provision of audiology services for older people.
We recognise the importance of good eyesight throughout life, and the Scottish Government is committed to continuing to provide free NHS-funded eye examinations for everyone. Monitoring for eye disease becomes more crucial as we age, and additional tests and assessments to identify early signs of sight-threatening conditions, especially glaucoma and age-related macular degeneration, are part of the Scottish eye examination for older people. We will continue to provide an NHS-funded eye examination service to support the early identification of sight-threatening disease.
Visual impairment increases dramatically with age. Loss of vision can have a devastating effect on a person’s physical and mental wellbeing. The appropriate provision of low-vision aids can support independence within the community and reduce reliance on support services.
We Will
Establish a community-based low-vision service, building on the groundwork that has already been conducted, to improve access to low-vision aids and appropriate signposting to other support services.
Introducing technology-enabled care
‘Globally, just over half (55%) of us believe that technological development has the capacity to improve age for a lot of people’
Ipsos-MORI/Centre for Ageing Better
The Perenials: the Future of Ageing, page 177
Scotland’s world-leading Technology-enabled Care Programme continues to support greater independent living and healthy ageing by delivering a step-change in how technology is used as a cost-effective support.This includes maximising the service redesign opportunities presented by the shift from analogue to digital telecare services.
Technology and technology-enabled care are providing new and exciting opportunities to identify people at risk before they have experienced harm. New technologies are emerging that can monitor our health, combining pioneering ‘predictive analytics’ with innovative wearable technology to identify the most vulnerable people in society.
Promoting digital participation
Eighty-five per cent of Scottish households reported having internet access at home in 2017, an increase from 42% in 2003. The groups most likely to remain disconnected are the older generations, people living in social housing, those who are unemployed, and people who have challenges accessing digital technology due to disabilities.
Average internet use decreases with age
Percentage who use the internet every day
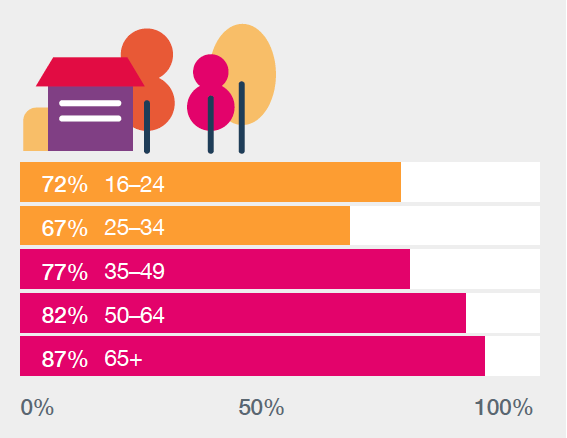
Source: Scottish Household Survey 2017
The Scottish Government is committed to increasing digital participation. A cross-sector movement throughout Scotland to ensure that everyone is able to realise the social, cultural and economic benefits of digital technologies now exists. This is shown in the continuing increase in digital participation, the number of signatories to the Digital Participation Charter, the number of projects supported by the Charter Fund and the increase in sector-specific digital champion networks.
Our Digital Participation Team has been looking at ways to increase digital inclusion for older adults. Research carried out with groups of older people with varying degrees of digital skills has shown that many older people prefer peer-to-peer learning from someone they know and identify with, over more formal training courses.
We are now working with organisations such as the Scottish Council for Voluntary Organisations, Age Scotland, third sector community projects and housing associations to develop a network of digital champions for older people to aid digital inclusion and reduce social isolation and loneliness through the development of essential digital skills.
The Scottish Government funds the Scottish Council for Voluntary Organisations with £375,000 a year to support the Digital Participation Charter and the Digital Participation Charter Fund, ensuring there are robust links across sectors and that the Charter and Fund have as wide a reach as possible.
The aim of the Digital Participation Charter is to create a movement of support for the development of essential digital skills across Scotland. The Charter has secured commitment from over 600 public, private and third sector organisations to build the digital skills of their workforce, customers, volunteers and service users and to support each other to achieve that aim.
The Charter Fund was established in 2014 to support local projects to increase digital participation. It was a key action outlined in the Scottish Government’s Digital Participation: a national framework for local action strategy, published in 2014.[44]
The Fund’s aim is to provide funding for organisations to assist digitally excluded people to gain or improve their basic online skills. We have invested £1.5 million in the Fund, which has supported 169 local projects across Scotland to enable over 20,000 people to gain or improve their essential digital skills. Round 7 of the Charter Fund was launched on 30 January 2019 and is open to organisations from all sectors to support the development of basic digital skills. This round of funding focuses on two specific themes:
- supporting working-age people to increase financial capability, employment and other economic outcomes
- supporting older and disabled people to reduce social isolation and loneliness.
We Will
Work with the Ministerial Action Group on Digital Participation to increase digital inclusion of older people with the growing technologybased services sector.
Work with groups of older people to understand how digital technology can add value to their lives in a way that is meaningful to them, and link this to our ongoing work on delivering our digital strategy for Scotland.
Providing health and social care for older prisoners
Work on improving the provision of health and social care integration includes providing support to older prisoners with health and social care needs. The Scottish Parliament’s Health and Sport Committee report on healthcare in prisons, published in May 2017,[45] and the HM Inspectorate of Prisons for Scotland’s report Who Cares? The Lived Experience of Older Prisoners in Scotland’s Prisons, published in July 2017,[46] highlighted the urgent need to review the provision of health and social care due to the rise in older people in prison.
We established a national Health and Justice Collaboration Improvement Board in response, consisting of senior leaders from health and justice agencies, to explore how we can improve collaboration between health and justice and deliver benefits in practice. Under this Board, a Health and Social Care Integration in Prisons Workstream was established. This project is due for completion by March 2020.
The Workstream commissioned the University of Dundee to undertake a review of the current provision of social care in Scotland’s prisons, focusing on the human rights and equality of prisoners, and making recommendations on how to improve provision. The report is due to be published in spring 2019 and will inform the development of a new model for delivery of health and social care integration in prisons.
We Will
Respond to the recommendations made in the University of Dundee’s review of the current provision of social care in Scotland’s prisons when developing a model of delivery of integrated health and social care in Scotland’s prisons, taking into consideration the human rights and equality of care of older prisoners, including all of the protected characteristics.
Searching for people who §go missing
Older people in communities across Scotland are among those who go missing every year. The likelihood of an older person going missing is increased if they have a condition like dementia. In 2017–2018, Police Scotland made 22,966 investigations for people who were missing: 36% involved an adult (over 18 years) and 2% (538) involved an adult with dementia. Work in local authority areas has been developed to respond to this issue in ways that take account of local circumstances and support agencies in working together to locate those who have gone missing.
Police Scotland worked with partner organisations in 2015 to develop protocols for safeguarding and preventing people at risk of going missing, and of activating the appropriate response when they do go missing to ensure they are found as quickly as possible. A protocol for adults in care homes has been evaluated and is currently being reviewed with a view to identifying best practice and rolling-out the protocol through 2019–2020 to help safeguard older people who go missing.
We Will
Work with Police Scotland and partner organisations to develop and roll-out the adults in care settings pilot protocol to safeguard and prevent people at risk of going missing.
Contact
Email: karen.mechan@gov.scot