Distress Brief Intervention - under 18s elements: evaluation
This evaluation of the under 18s elements of Distress Brief Intervention (DBI) provides evidence of promising practice, and indications that DBI can be an effective intervention for use with young people.
Introduction
The Distress Brief Intervention (DBI) programme is a unique approach to supporting people in distress who present to frontline services. It brings the Scottish Government together with a DBI Central team, local NHS and voluntary sector DBI provider partnerships, national agencies and services including primary care, Police Scotland, Scottish Ambulance Service, emergency departments, NHS 24, third sector mental health organisations and academics from the University of Glasgow. Distress is defined by DBI as ‘an emotional pain for which the person sought, or was referred for, help and which does not require (further) emergency service response’. DBI consists of two levels of support. At Level 1, trained staff (e.g., police, A&E, ambulance, primary care and NHS 24) provide a compassionate response to individuals who present to them in distress. If a person is assessed as appropriate for DBI and would like further support, they are referred to the DBI Level 2 service with a promise of contact within 24 hours. At DBI Level 2, people are offered up to 14 days of community-based, person-centred support from trained staff. Support includes compassionate problem solving, wellness and distress management planning, supported connections and signposting on to other suitable services.
The DBI programme began in 2017 in response to the Scottish Government’s Mental Health Mental Health Strategy for Scotland: 2012-2015 and Suicide Prevention Strategies Suicide Prevention Strategy 2013-2016, which identified a need to improve support for adults in distress in Scotland. The programme has been led by the DBI Central Team in NHS Lanarkshire, with training developed and delivered by the University of Glasgow in consultation with the Scottish Government, DBI Central, mental health service users and stakeholders.
Since the programme began, there have been changes made to implementation and delivery of DBI. The Scottish Government’s Programme for Scotland 2018-2019 committed to extending DBI provision to children and young people aged under 18. After the DBI service was successfully extended to young people aged 16-17 years in the four original pilot areas (Aberdeen, Inverness, Lanarkshire and Scottish Borders), DBI was expanded in 2019 to support people aged 16 and over. As part of the Scottish Government’s COVID-19 pandemic response, a national pathway to DBI, via NHS 24, was also established in Spring 2020, offering support to people aged 16 or over across Scotland.
In 2019, the Children and Young People’s Mental Health Task Force made a number of recommendations focused around increasing the variety and availability of support to children and young people. In 2020 a scoping study (unpublished) was conducted to assess the appropriateness and practicability of lowering the DBI age range below 16. Following this, a limited and controlled test of change began in 2021 in a small number of schools sites in a limited number of local areas, in which DBI became available to 14- and 15-year-olds who present in distress and meet the criteria for DBI. This work is overseen by the DBI Children and Young People advisory group, comprising clinical and academic experts in children and young people’s (CYP) mental health, members of the DBI Central Team and leaders from education.
DBI has shown itself to be a highly effective intervention for over 16s in Scotland, with local provision across every Health and Social Care Partnership, which is complemented with 3 national pathways (Police Scotland contact centres, Scottish Ambulance Service contact centres, and NHS24). The effectiveness of DBI is supported through two independent evaluations:
- The evaluation of the DBI pilot phase, launched in 2017 for adults over 18, broadly endorsed the model and the Scottish Government’s commitment to expand it across all NHS Board areas. It found DBI effective in reducing distress, with one in ten participants indicating they might have attempted suicide or continued experiencing suicidal thoughts without DBI support.
- A separate evaluation of the NHS24 pathway to DBI—introduced in 2020 as part of the COVID-19 response and extended to those aged 16 and over—also confirmed DBI’s continued effectiveness in alleviating distress.
Clinical guidance highlighted within the scoping study is that DBI is unlikely to be suitable for under 14s in school year S2 or below in its current form but may be effective for 14- and 15-year-olds. The Scottish Government and DBI partners have been testing DBI’s effectiveness for children and young people from S3 up through small scale piloting via schools and CAMHS (age 14 to 18, later expanded to pupils aged 13 in S3 upwards), starting in 2021 in Lanarkshire (North and South) and Aberdeen City. This test-of-change progressed to include Inverness and West Dunbartonshire. As at August 2025, referrals to DBI CYP are now provided in 24 schools in these areas.
Additionally, Glasgow City and East Dunbartonshire Compassionate Distress Response Service (CDRS) became the DBI equivalent service for these areas in May 2023. The CDRS provides a DBI response for young people aged 14 and 15 (as an expansion of their existing model of support for 16- to 25-year-olds in East Dunbartonshire; and 16 and over in Glasgow City). Referral routes into the CDRS include Mental Health Assessment Units, CAMHS, agreed contacts in secondary schools, further education and higher education institutions, Social Work Services staff and third sector organisations. The service provided by the CDRS differs from DBI. While both aim to offer a response within 24 hours, only CDRS offers a response within 1 hour if the referral takes place out of hours, and CDRS offers support for up to 1 month, compared to the 14 days offered by DBI. The CDRS is not considered to be an official part of the test of change but, as it is providing DBI support to under 16s, it is included within the scope of the evaluation.
The evaluation of the test of change work and of the CDRS will help the Scottish Government understand the effectiveness of DBI for this age group to support and inform future planning.
The 2022-2025 Action Plan for Creating Hope Together, Scotland’s Suicide Prevention Strategy, highlights the importance of learning from this evaluation in terms of what works for supporting children and young people. Additionally, the school referral pathway links to the Scottish Government’s ‘whole school approach’ to mental health and wellbeing Whole School Approach to Mental Health and Wellbeing by exploring options for specialist support options for pupils experiencing acute distress.
More broadly, to drive improvements forward for children and young people’s mental health, The Child and Family Mental Health Joint Strategic Board led by Scottish Government and COSLA, is taking a whole system approach to improving children and young people’s mental health. This includes focusing on four early priorities, which includes improving support for children and young people in distress and crisis.
A key early priority for the Board is the exploration of a “Scottish Approach to Supporting Children and Young People in Crisis”. This Framework will outline the principles of good crisis support at a local, regional and national level to support decision makers to ensure that they are providing the right support for their populations. This will cover a range of sectors such as the third sector, youth work, and statutory services. As part of the Framework’s development, a wide range of evidence is being assessed, with efforts to learn from current practice. The evaluation of DBI for under 18s will provide evidence to inform the Scottish Government’s next steps in improving support for children and young people in crisis and distress.
Aims
This evaluation is intended to produce evidence-based recommendations for the continued development of the DBI Under 18s programme and inform associated policy and practice decision making through providing a clear and robust account of:
- whether DBI can be an effective intervention for use with young adults aged under 18, and whether this varies among subgroups of young people, particularly those aged under 16 compared with 16- and 17-year-olds?
- what changes in the design and implementation of the DBI, if any, are needed compared with its use in adults?
- what mechanisms of delivery and contextual factors contribute to its successful implementation and impact?
A number of detailed research questions were explored through this evaluation. These are provided in appendix 1.
Key terms and scope of the evaluation
Distress Brief Intervention (DBI): DBI is a non-clinical intervention, consisting of two interrelated parts. Level 1 sees trained front-line staff such as health, police, ambulance and primary care staff help ease the person’s distress, provide a compassionate response and where appropriate, involves an offer of a seamless referral, with confidence and clarity to a DBI Level 2 service. Level 2 is provided by commissioned and trained third sector staff who contact the person within 24-hours of referral and provide community-based problem-solving support, wellness and distress management planning, supported connections and signposting.
Adult programme: This refers to the delivery of DBI to adults, considered as those aged 16 and over. DBI was originally piloted with those aged 18 and over, and the age range was extended to include those aged 16 and 17 in 2019.
Established pathway: The referral routes into DBI which are in place for the adult programme. This includes frontline services such as the police, Scottish Ambulance Service, primary care, and accident and emergency departments.
Distress Management Plan (D-MaP): A resource to help someone receiving DBI support to begin to explore and make sense of their distress. It is used with individuals with the aim of clarifying their aims and expectations for DBI, problem-solving key issues and identifying strategies to manage their distress now and in the longer term. The D-MaP is considered a mandatory component of DBI.
Stakeholder groups:
Level 1 referrer: school staff (usually guidance or pupil support teachers) and CAMHS staff who refer young people to DBI
Level 2 provider: the service which provides Level 2 support in each local area
Level 2 staff member: those working in Level 2 services, including staff who indirectly and directly provide support to young people aged under 18
Strategic stakeholders: those involved in the development and governance of DBI. This could include DBI Central staff and members of the CYP Advisory Group.
Test of change: A programme of controlled testing of the delivery of DBI to young people in a small number of local areas via a new referral pathway which involves schools and CAMHS services, as part of a tripartite pathway. This work initially focussed on 14- and 15-year-olds but was extended to include:
- 13 year olds when they were in S3 (to prevent the intervention excluding young people in that year group)
- 16, 17, and on occasion, 18 years
Tripartite pathway: The referral pathway which was developed for the under 16s test of change. This involves a three-way referral arrangement between schools, DBI providers and CAMHS services. Schools can refer young people to DBI and CAMHS, as appropriate for the young person’s needs, and DBI and CAMHS can refer into one another. Figure 1 below shows this referral pathway.
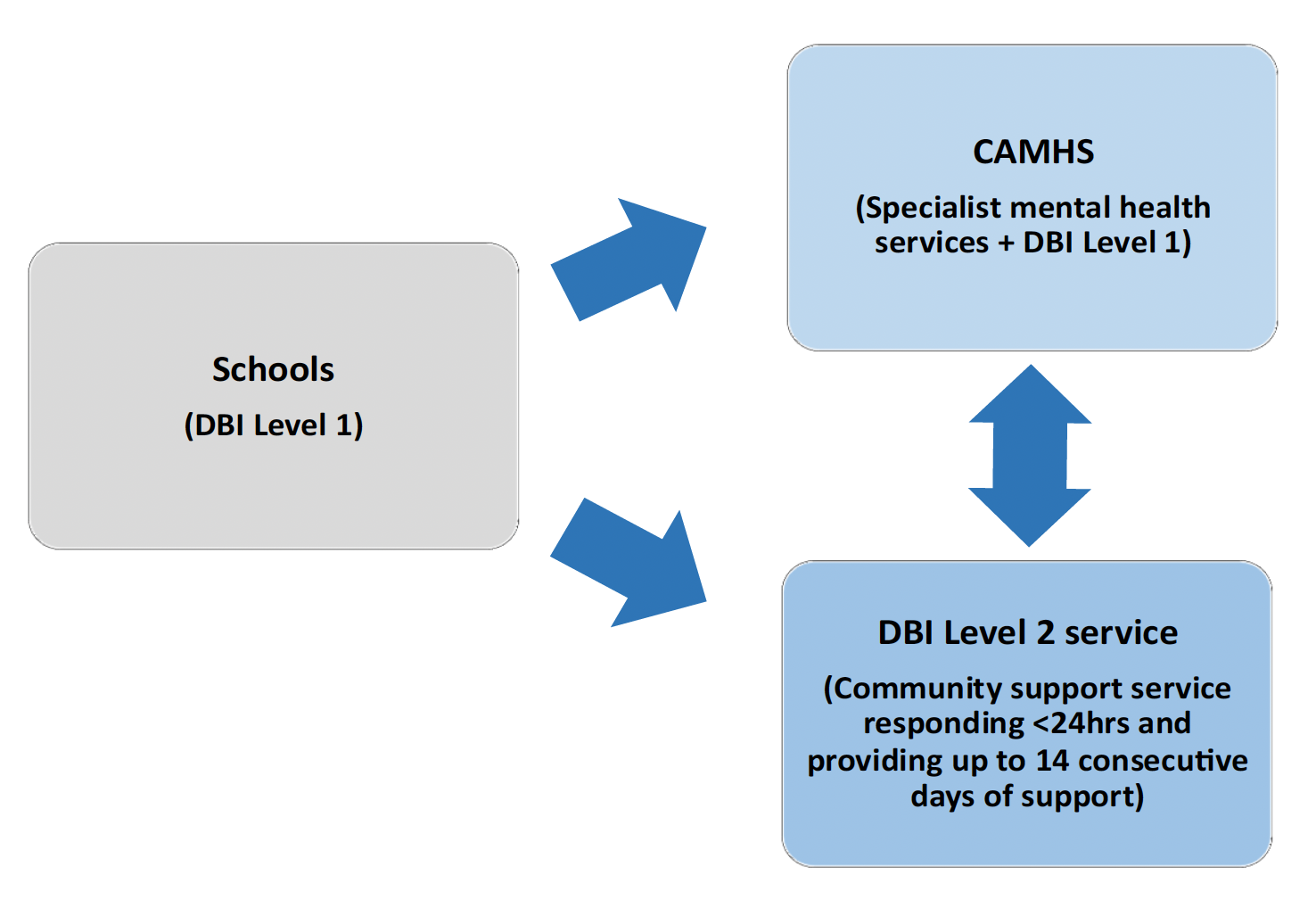
Scope of the evaluation
This evaluation considers all of the elements of DBI delivery which involve under 18s as in scope. That includes:
- Individuals aged 16 and 17 who were referred via the routes into DBI which were already in place for adults (referred to as the adult pathway), including frontline services such as the police, Scottish Ambulance Service, primary care, and accident and emergency departments.
- Young people aged 13 to 18 who have accessed DBI as part of a programme of controlled testing (referred to as the ‘test of change’) of the delivery of DBI to young people in S3 and up (age 14 to 18, later expanded to pupils aged 13 in S3 upwards) via a new tripartite referral pathway which involves schools and CAMHS services.
- Young people aged 14 to 18 who have accessed DBI via the Compassionate Distress Response Service (CDRS) in Glasgow City and East Dunbartonshire.
Contact
Email: socialresearch@gov.scot