Brain Health Service pilot: evaluation - final report
This report presents detailed findings from Blake Stevenson’s independent evaluation of the Brain Health Service demonstrator site in Aberdeen,
delivered collaboratively by NHS Grampian, Alzheimer Scotland, and the Scottish Government.
3. Key findings: Brain Health Service effectiveness and outcomes
In this chapter and Chapter 4, the evaluation findings are presented and organised to align with the core evaluation questions and RE-AIM framework (Reach, Effectiveness, Adoption, Implementation, Maintenance).
The first section considers the visibility and access to the service before exploring effectiveness and service outcomes.In this chapter we provide details of the delivery model and impact of the PDS innovation site in East Edinburgh.
Reach
The Brain Health Service was officially launched on 4 December 2023 by Maree Todd MSP, attracting media attention from outlets including Aberdeen Live and STV News. To further enhance visibility, and promote the novel concept of brain health, from February – March 2024 a public awareness campaign ran across multiple media channels.
The objective of the campaign was to engage with people aged 18-65+ who might have concerns about brain health and want to find out more about reducing their risk of developing dementia in the future. The campaign incorporated bus advertising on the rear of 20 buses, a 40 second radio advert on Northsound 1 and Northsound 2 with a potential reach of 277,000 listeners as well as NHS Grampian marketing activities on hospital screens, webpages and radio interviews .
There was also targeted Facebook and Instagram adverts.The results of the paid social media campaign showed:
- significant campaign visibility with 939,369 impressions generated which identify a wide reach of the adverts in driving awareness;
- 6950 link clicks through to the landing page (click through rate – CTR of 0.74%) demonstrating audience interest and intention in learning more;
- 698 positive sentiment engagements with post reactions, comments, saves and post shares
To reinforce the public’s awareness a range of resources was developed and distributed across key locations. These posters and leaflets were placed in GP practices, libraries, pharmacies, and community centres, making the service more visible to the public. They provided details on the importance of brain health and how to access the Service, helping potential users understand its benefits and availability.
Community outreach efforts were a key component of the promotion strategy with more than 30 presentations and networking events held to introduce the Service to various community groups and healthcare professionals. This included:
- targeted work with community groups and professional organisations to deliver hands-on resources, fostering direct interaction with attendees;
- engagement with healthcare workers with presentations at rehabilitation units and occupational therapy teams to provide a platform to engage healthcare professionals who could act as referral points to the service;
- public events with a pop-up stall at events like Challenge Poverty Week at Aberdeen Music Hall and the Grampian Gathering at The Beach Ballroom;
- volunteer and support networks to reach the volunteers and social care professionals supporting vulnerable populations; and
- strategic partnerships facilitating discussions with key organisations like Sport Aberdeen and the Aberdeen City Council to explore opportunities for future collaboration.
The wide range of approaches to raising awareness of the Service reflected the need for varied forms of communication so that the public and stakeholders understood the unique nature of the Service and its existence.
Awareness of the service
When asked about how they became aware of the Service, users highlighted these multiple channels and promotional activities. Chart 3.1 summarises the key sources.
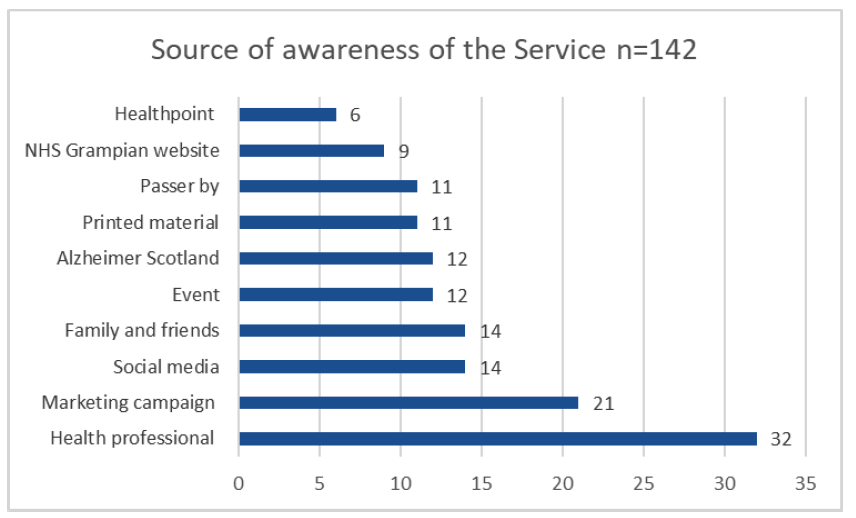
The most frequently cited source was a health professional which included GPs, and pharmacists within those roles. The marketing campaign, particularly the radio advertisements was the next most commonly cited source of information – following by social media adverts, all through Facebook. Information from family and friends was a source of information as was and the pop-up stalls at events that people attended. For many of the service users who were interviewed, word of mouth through colleagues, family and friends and local organisations was their main source of information about the Service.
Despite the wide range of promotional and engagement activities, there was still a call from various evaluation participants for increased awareness-raising both with potential service users and for wider stakeholders:
“I would say that it should maybe be publicised more, for more people to be more aware of it. I just thought it [Resource Centre] was for people who had Alzheimers.” Service user
Accessing the service
Stage 1 of the Service is open to all NHS Grampian residents, and between 11 December 2023 and 31 January 2025, 159 people were supported through the first stage of the Service.

Based on the available profile data, it shows that the Service predominantly supported older age groups, with the majority of users aged between 60-79 years (57%). Younger individuals, particularly those under 50, were less represented, with 18% of service users under the age of 50.
The gender distribution of users accessing the service showed a higher proportion of females (55%) compared to males (45%). Geographically, the Service primarily reached individuals residing in Aberdeen City (56%), compared to the broader NHS Grampian area (44%) and in terms of ethnicity, the vast majority of service users identified as White (91%), with only a small [1]proportion from Black and Minority Ethnic (BME) groups (6%). The data collected on service users did not enable analysis of the socioeconomic profile of Stage 1 users.
The Service was resourced to a level that meant Aberdeen City residents could access the clinic and so individuals from Aberdeenshire, despite demonstrating suitability, were not referred to Stage 2 of the Service but instead they were encouraged to make follow on appointments with their GPs. This did create some frustration for both users and a few staff and presented inequalities across areas of NHS Grampian.
"It can be frustrating because I know some [Aberdeenshire residents] would be perfect for Stage 2." Staff member
The majority (74%) of individuals accessed the Service by walking in to the Resource Centre, 15% phoned Healthpoint and were supported by the advisors and 11% were referred by GPs directly into Stage 2 of the Service.
Motivation for accessing the Service
Craig has a family history of dementia and was prompted to contact the Resource Centre after watching a TV documentary on brain health. After an initial conversation with the centre manager, Craig was referred to the nurse and then doctor but scored highly on the memory assessment.
Behaviour change
The conversations with the centre manager and nurse reassured him that the type of dementia his family member had experienced was unlikely to have a genetic link. He was also given advice on what he could do to reduce his risk of dementia, and it was suggested that he could improve his diet, increase his physical activity and do more to keep his brain active. Craig is now trying to walk more and keep “the brain ticking” by doing crosswords. While he already knew about the benefits of a more active and healthier lifestyle, the Brain Health Service was described as “hammering it home.”
Experience of the Service
Craig described his experience of the service positively and felt that he was put at ease by the team:
“It was very good, it was a relaxing atmosphere. I suppose I was a little bit apprehensive but [resource manager] put me at ease. I felt quite comfortable yapping away.”
Craig, 47-year-old male
Motivations for accessing the Service
Individuals accessed the Service for diverse reasons, ranging from health concerns to proactive health management. Individuals with a family history of dementia or who were experiencing memory issues or challenges with daily tasks and were therefore worried about cognitive decline were keen to access support. Physical health conditions were another common motivator, particularly among individuals with hypertension, diabetes, or a history of stroke or head injuries. Mental health and emotional wellbeing also influenced users, with anxiety, depression and stress prompting them to seek advice.
Service users with concerns about their lifestyle - smoking, alcohol consumption, poor sleep quality, and reduced physical activity were also motivated to seek help. Lastly, a proactive group engaged with the Service to actively monitor and maintain their brain health, particularly if approaching an age associated with increased dementia risk. These individuals sought reassurance and preventive guidance.
Effectiveness of the service
The Service was intended to provide people with concerns about their cognitive well-being within a dedicated space for in-depth, professional guidance; increase public awareness of how lifestyle factors can influence brain health; offer tailored action plans to support positive behaviour changes; and, where appropriate, undertake clinical assessments and refer them to additional specialist services.
Brain Health Service Stage 1
The data from the Stage 1 Service provides a wealth of information about the tailored support and advice given to individuals based on their reported symptoms, personal concerns, and identified risk factors.
Service users experiencing mental health or emotional challenges were signposted to support services and local groups as well as self-help resources on NHS Inform.
Lifestyle recommendations were comprehensive, with Healthpoint staff and the Centre Manager encouraging gentle physical activities, joining local sports clubs, attending organised health walks, or participating in exercise classes. Healthy eating advice emphasised increased fruit and vegetable consumption, reducing processed foods, balanced dietary intake, and portion control and was supported by resources like the Eatwell Guide, and staff also advised on alcohol moderation and better sleep management practices.
Cognitive engagement was encouraged through recommendations to participate in stimulating activities, including learning new skills, engaging in brain games or puzzles, and, in some cases, joining research studies. Practical memory aids such as diaries, calendars, or task lists were also suggested to improve organisation and daily functioning.
To reduce social isolation and enhance emotional wellbeing, service users were advised to join local community groups, increase social interactions, and engage openly with family members regarding their concerns, drawing on both emotional and practical support networks.
Motivation for accessing the Service
Mary is 54 years old and was referred to the Brain Health Service by her GP because of short term memory problems that were making work and driving difficult. Mary was assessed by the nurse and told that she had “nothing to worry about” but referred to the consultant to discuss her memory problems. The consultant identified medications and another health condition as the potential causes. After changing her medication, Mary still forgets things but is “now managing to function” and carry out everyday tasks again.
Experience of the Service
Mary described how, when she was first referred to the Service, she was “scared because I’d got into my head that I had dementia” but was “made to feel relaxed” by the nurse. She saw the consultant afterwards and said that:
“It was an amazing, smooth, easy process. I’m one of the lucky ones because it was so quick, from me initially realising that something was definitely wrong to seeing the doctor.”
Behaviour change
The actions Mary could take to reduce her risk of dementia were discussed during her appointment with the nurse and more exercise was recommended. In identifying medication as the potential source of her memory problems, Mary’s GP has also referred her back to the relevant hospital department for a review.
Mary, 54-year-old female
An essential aspect of Stage 1 interactions involved raising awareness about modifiable dementia risk factors. Informational leaflets reinforced the advice on maintaining brain-healthy behaviours further supporting their ongoing brain health journey.
Brian Health Service – stages 2 and 3
Aberdeen City residents could be referred to the second stage of the service by the Centre Manager, Healthpoint advisors or GPs. When a service user is referred to Stage 2 of the Service, they have a detailed assessment with the Nurse Practitioner that includes:
- a comprehensive review of the individual's personal concerns;
- lifestyle evaluations, including sleep quality, mental health questionnaires, and assessments of Activities of Daily Life (ADL);
- a physical health check; and
- administration of the Addenbrooke’s Cognitive Examination (ACE-III), an objective cognitive assessment tool.
The clinical audit data provided rich insights into outcomes from nurse assessments, highlighting the complex interplay of cognitive, mental, and physical health factors.
Memory and cognitive function
Assessments revealed diverse underlying factors influencing cognitive concerns. In instances where individuals displayed no clear evidence of Mild Cognitive Impairment (MCI), memory lapses were commonly attributed to lifestyle and physiological factors such as busy or stressful lifestyles, menopausal symptoms or alcohol consumption. In a smaller number of cases, objective evidence of MCI emerged clearly, frequently linked with factors such as anxiety, depression, chronic physical health conditions, or possible early dementia. ACE-III scores were valuable in indicating the need for further investigation. Even users with ACE scores within normal limits occasionally exhibited subjective cognitive concerns that warranted ongoing monitoring.
Mental health and emotional wellbeing
Mental health factors significantly impacted cognitive presentation. Numerous assessments uncovered underlying issues with depression and anxiety, which manifested as cognitive difficulties, low mood, and disrupted daily functioning. Contributing factors frequently identified included poor sleep hygiene, stress related to personal responsibilities such as caregiving, and other emotionally taxing lifestyle components. These findings highlighted the necessity of integrating mental health support into the clinical planning process.
Physical health influences
Physical health challenges were prevalent among users and significantly influenced cognitive health concerns. Conditions such as fibromyalgia, cardiovascular issues, previous chemotherapy or radiotherapy treatments, and peri-menopausal or menopausal symptoms were all noted as contributing to subjective memory concerns and cognitive decline. This recognition informed referrals to appropriate physical health services, ensuring a comprehensive approach to users' cognitive health management.
Following the initial nurse assessment and subsequent case discussions with the Consultant, tailored clinical plans were developed and according to the clinical audit data relating to 117 individuals:
- 56 were referred to the Consultant for further evaluation;
- 28 were directly discharged with advice like GP follow-ups, signposting to mental health support resources or community-based support groups or lifestyle guidance; and
- 17 had specialist referrals e.g. audiology, physiotherapy with Nurse follow-up.
The Consultant reviews played a crucial role in determining the ongoing care pathway for service users. Following these assessments, common outcomes included scheduling six-month reviews, referring service users to specialist services (for example, psychiatry, neurology, stroke clinics, or ADHD clinics), requesting further diagnostic investigations such as CT or MRI scans, and recommending ongoing clinical or nurse oversight to manage cognitive health or related conditions.
The data indicate that the highest proportion (27) individuals were recommended for a six-month review with the Nurse or the Consultant, some (14) were discharged directly after consultant assessments, suggesting that initial concerns had been sufficiently addressed and a smaller group (10) required additional diagnostic testing.
This approach ensures that all service users, regardless of their specific cognitive concerns or contributing factors, benefit from comprehensive, person-centred support. Tailored interventions help address both cognitive symptoms and underlying health factors, demonstrating a structured and responsive approach to clinical management within the service, and reflecting the original vision and model for the Service.
Service outcomes
The available data indicates that wide-ranging conversations about brain health took place in response to the concerns and risk factors presented by people accessing the Service.
Awareness and knowledge of brain health
Where people had a family history of dementia, the Service provided a space for them to learn and better understand their genetic risks. More often though, discussions focussed on the modifiable risk factors and the types of actions that could be taken to reduce risk. Informational leaflets about each of these had been prepared by the service and shared with people as appropriate but, amongst those people engaged in the evaluation interviews, information was commonly given verbally.
From the responses to the service user postcards, 21 out of 25 people reported that after receiving support they felt that they had increased awareness of brain health and had information about how to support their brain health.
In the interviews with service users, many explained that they already possessed a solid understanding of healthy living—such as eating well, moderating alcohol intake, and staying active—before engaging with the Service. Several had also learned about brain health risks through television programs, newspaper features, or presentations. This existing knowledge often prompted their initial interest in accessing the Service.
Owing to these differing levels of familiarity, the effect of the Service on users’ awareness varied. Some reported a notable increase in their overall understanding, while others found that the information simply reinforced what they already knew. Where people did describe an increase, it was typically described as a broader improvement in their awareness of brain health.
“I’m just more aware of things now, how I think, what I think. So it’s improved.” Service user interview
“I think it’s given me a little bit more awareness.” Service user
Others described how they were now more aware of the specific risk factors that they needed to reduce, with the importance of keeping the brain active, managing high blood pressure and cholesterol, and addressing hearing loss all being mentioned.
Motivation for accessing the Service
Theo, is 64 years old and first learned about the Brain Health Service through a pop-up promotional stand in the Shopping Centre. For some time, he had been feeling "out of sorts" and experiencing increasing forgetfulness in everyday tasks. His role at work required him to engage members of the public and direct them to designated seats, but often by the time he escorted them, he would forget which seat was their allocation. This ongoing forgetfulness caused him significant anxiety.
Experience of the Service
After speaking with staff at the promotional stand, Theo was encouraged to visit King Street, where he booked an appointment with the Centre Manager. His initial consultation was reassuring and non-judgmental, making him feel at ease. Following the Brain Health questionnaire assessment, it was decided that he should be referred to the Nurse, and this happened quickly. During his appointment, the Nurse identified that Theo had high blood pressure, requiring medical attention. Accessing his GP was challenging, and with his next appointment scheduled four weeks away, he was unable to secure an earlier slot. The Brain Health Service intervened, contacting his GP directly to ensure an urgent appointment. At this appointment, an ECG confirmed high blood pressure and angina, and he was prescribed medication.
Behaviour change
Beyond medical intervention, Theo received lifestyle advice, encouraging him to be more active and make healthier food choices. While he still enjoys some of his favourite foods, he now consumes them in moderation. He has also increased his physical activity, walking 20-25 miles per week, and is gradually losing weight.
Theo is booked to see the Consultant at the Brain Health Service but already, his memory has improved, and he feels more confident in both his everyday life and work. Reflecting on his experience, he shared:
"Memory loss makes you anxious and question yourself. Instead of waiting months to see my GP and worrying, I was able to access a service that not only helped me with my medical condition but also supported me in changing my habits. I’m not sure I would have gone to the GP with these concerns—getting past the receptionist to book an appointment is hard, and if I had said it was about my memory, I don’t think they would have taken me seriously. At the Brain Health Service, I was listened to, and my concerns were acted upon."
Theo, 64-year-old male
The tailored discussions that considered the modifiable risk factors also encompassed broader issues that were affecting cognitive function of individuals such as a lack of sleep, mental health concerns and in response to these issues, people were given advice and signposted or referred as appropriate. This holistic response was appreciated by users and for one individual, this broader conversation was particularly helpful to them:
“The initial conversation was around family background, lifestyle, potential indicators, info gathering. Potential strategies and plans that we could look at just to assess the potential of any future problem. That was very much the initial part of the conversation, but it quickly expanded beyond the whole dementia thing, and I found, well, I found myself opening up on other mental health issues. That’s where the major benefits have been, on that expanded service.”
Behaviour change
The Service’s approach to facilitating behaviour change evolved over time. The Recommendations for Clinical Practice provides the template for the Service and describes a key intervention as the personalised action plan prepared at Stage 1. Initially this was intended to be a written document but learning throughout the delivery period identified that what constituted an action plan varied according to individual need. For example, an action plan might simply be a recommendation to have a hearing test or for an onward referral to be made to a GP for the management of high blood pressure, cholesterol or diabetes. Other recommendations were made around lifestyle, cognitive stimulation and social engagement to address isolation.
There has then been an individual person-centred rather than a standardised approach to the preparation of action plans:
“An action plan can be verbal advice [rather than a physical thing]. It’s patient centred, it’s what the patient wants. If it’s one thing they want to change, we won’t send a massive thing out by post. The patient might be happy to look online, so we’ll email them links. That action planning, it’s about what the patient needs and is appropriate to them… We didn’t want to make it too structured, it won’t work for every person. I think it’s more about the personalised advice we can give.” Staff interview
Staff and stakeholders highlighted Healthpoint's involvement in Stage 1 of the Service as a significant strength. Given their established public health role, Healthpoint staff are particularly adept at identifying appropriate NHS services and support groups, collating relevant information effectively, and clearly communicating tailored behaviour change messages to service users.
“The Healthpoint always delivered those key messages, it’s what we do all the time.” Staff
However, because formal action plans were not consistently prepared, some interviewees were unable to clearly identify specific recommended behaviour changes. This limited the assessment of the service’s impact on behaviour change, resulting in mixed evidence. Some participants reported no changes, while others indicated they were already proactively taking steps to support their brain health. For these individuals, the service primarily reinforced the importance of existing behaviours rather than initiating new actions.
Amongst those who did report behaviour changes, a reduction in alcohol intake was common:
“I’ve cut down my use of alcohol. It was just making me think about the whole way I lived and when I did things, it made me reflect back.”
“I think I’m probably more aware of alcohol, I used to have a G&T every other night but I’ve reduced my intake. I know that alcohol is bad but [the Consultant] reinforced that. Made me more aware of everything.”
Other people were taking action to keep their brain active through doing daily crosswords, for example, and others were now more physically active.
The service user postcards echoed these findings from the service user interviews with 21 out of the 25 postcard respondents reporting a variety of planned or initiated behavioural changes to positively support their brain health. Like those interviewed, some intended to take specific health-related actions, including reducing alcohol consumption, improving diet, managing their weight, and increasing physical activity. Others highlighted plans for better sleep management using resources such as the Sleepio app or Alcohol Focus Scotland. Several users who completed the postcards emphasised the importance of maintaining social interactions and engaging in activities outside the home to improve overall wellbeing.
Some individuals were waiting for the next phase of support and had appointments, e.g. with their GP or follow-ups with the Nurse to address specific health concerns like diabetes management or blood pressure monitoring. What was clearly expressed from the postcard surveys was service users intentions to keep their brains active.
For those accessing the clinic, follow-up appointments with the Nurse or Consultant were scheduled when they were required. For individuals accessing Stage 1, the model was not designed for follow up under this stage but, within the Centre Manager, using Alzheimer Scotland, arranged for users to return to receive limited support in progressing their personalised actions.
It was suggested by both a service user and staff interviewee that further encouragement of lifestyle changes could be facilitated through follow up reviews (for example via a phone check-in). The experiences of one person who had benefitted from multiple follow up appointments with the Centre Manager provided support for these views. The review meetings were perceived to provide additional motivation for behaviour change and, in a follow up evaluation interview in January 2025, were reported to have been sustained over six months after the initial Stage 1 appointment:
“I think back regularly to the conversations [Centre Manager] and I had and what a positive impact it had on me. If I’m feeling a bit susceptible then I just replay some of the things and some of the self-help tools, we talked about. It works for me and I think knowing that the additional support is there almost on tap if required is a real support. Especially when not all services and support services are so readily available. So knowing that they’re there and accessible is helpful.” Service user interview
Discussions with service users across all service stages reveal that they are making plans and taking actions to support their brain health. The nurse and consultant assessments further reinforce these behaviour changes or help manage underlying conditions. Although the Nurse and Consultant have been conducting six-month follow-ups with some patients for this evaluation there was limited access to clinical data—such as changes in cholesterol levels—that would indicate improvements in relevant health markers.
In the survey responses, participants acknowledged the Service’s potential to foster meaningful behaviour change, while also recognising that sufficient time and a larger volume of service users would be required for these medium to longer-term benefits to fully emerge.
"Huge potential long-term benefits. Allowing patients to self-manage better but at this stage there are too few patients to understand that difference”. Survey respondent
Motivation for accessing the Service
Susan is a 47-year-old user of the Brain Health service. At the age of 43, Susan had begun to experience difficulties finding some words, not knowing where her keys were and a range of other memory issues. She had noticed that it was beginning to get worse and thought she may have a problem that required further investigation.
“At certain times I felt – am I stupid? I also felt like I was numb with tiredness.”
She had seen an advertisement on a bus about dementia, and, having read a lot about the importance of maintaining good brain health, she decided to visit the Brain Health Service with her husband.
Experience of the Service
Susan met the Centre Manager who worked through the Brain Health Questionnaire with her and then referred her into the Brain Health Clinic to meet the Nurse where she undertook a clinical assessment. The memory test results from the assessment were lower than would be expected for a person of Susan’s age but the Nurse attributed this to English being an additional language and potentially a symptom of peri-menopause.
The Nurse developed a personalised action plan with Susan which included setting up a meeting with her GP, making changes to her diet, including incorporating fish into her vegetarian diet weekly, eating meat once a month, and taking a daily dose of Kaffir, exercising more and undertaking therapy with a psychologist.
Behaviour change
Susan has found having an action plan really helpful. Susan reflected that the results provided by the nurse did not alarm her, and in fact motivated her to “fix things”.
Shortly following her visit to the GP, Susan began taking hormone replacement therapy (HRT) and many of her symptoms improved quickly.
“My mental health is better, and I am now undertaking training with the intention of changing jobs.”
She feels that her understanding of brain health has significantly increased and has made changes that will help which includes exercising four days a week – two days weight training and two days. The combination of these changes has had a knock-on effect on her husband and son because she is feeling so much better, and the dietary changes have also positively impacted on them.
Susan, 47-year old female
User satisfaction
As evidenced by both the service user postcards and interviews, experiences of all stages of the Service were positive. The interviews with service users described how accessing the service provided reassurance, reduced anxiety and prevented potential issues from going undiagnosed. The levels of user satisfaction highlighted through consistently low Did Not Attend (DNA) rates, indicating strong engagement and suggesting that the Service was effectively meeting user needs and expectations.
“Our DNA rate is extremely low, which reinforces the demand and engagement with the service." Staff
As a new service, many people arrived with few specific expectations. In some cases, however, their experiences surpassed what they had anticipated. For instance, one individual initially expected only to receive information on brain health, but their discussion with the Centre Manager encouraged them to think more broadly about their overall wellbeing.
"[The Service] can make a difference...they can have a 1-1 session about behaviour change and risk factors, not just been given a leaflet, so much more”. Stakeholder
The available evidence indicates that the following factors were particularly important in creating a positive service user experience:
Ease of access
The ability to self-refer via a phone call to Healthpoint or a walk-in to the Resource Centre was an important feature and meant that the service was easy to access. In recognising this, staff and stakeholder interviewees often highlighted the accessibility of the service as a key strength.
“I love that people can just self-refer and walk in. They don’t have to go through any clinical gateway first.” (staff interview)
A city centre location also meant that the service was visible to passers-by. While some stakeholders felt that King Street had relatively low footfall compared to other parts of the city centre and noted limited parking, evidence suggests that visibility nevertheless encouraged some people to explore the Service. For example, one individual found out about the Service after visiting a nearby shop and another walked past several times before deciding to go in.
Those accessing the Service via the Resource Centre described being seen by the Centre Manager soon after walking in – often the same day or, if necessary, with an appointment scheduled for the following day.
One person who had accessed the Service as a walk-in explained how this experience contrasted sharply with waiting for a GP appointment, which they reported took several weeks. Access was also reported to be quick and easy for another user who was referred to Stage 2 by their GP:
“It was an amazing, smooth, easy process. I’m one of the lucky ones because it was so quick, from me initially realising that something was wrong to seeing the Consultant. The process was very, very quick. It was amazing.”
Welcoming environment
"Trust, person-patient relationship...first impression, when you’re met with warmth, it can improve your connection with service." stakeholder
The Resource Centre was consistently described as welcoming and supportive, with staff immediately engaging users in conversation and offering refreshments to help them feel at ease. As one service user noted:
“Welcoming as you arrive, the receptionist arranged for us to have a cup of tea while we waited.”
Another user praised the simple but reassuring process:
“It was unbelievable, when you press the buzzer and go in, it’s amazing. The receptionist was out of this world…. I had to see a lady and didn’t have to wait long. They made an appointment for an assessment.”
Others highlighted the sense of safety the environment fostered:
“For the first time ever, I think I was in what I deemed a safe place and that enabled me to open up.” Service user
Although the clinical assessments by the Nurse are conducted in a dedicated consulting room within the same building, individuals generally remained at ease in the familiar setting. In many instances the Nurse contacted them beforehand to explain the assessment process, ensuring they knew what to expect.
Other users shared similar views, noting the absence of the stigma often linked to psychiatric settings. They also embraced Alzheimer Scotland's decision to rebrand some of the Centres as “brain health resource centres,” seeing this as a meaningful way to focus on overall well-being and encourage more open conversations about memory concerns. In doing so, brain health “is just like any other form of health.”
Compassionate staff
The evidence suggests that staff members were key in creating positive experiences, with interviewees frequently describing the team as personable and empathetic. Many noted that the Centre Manager, Nurse, and Consultant provided ample time and space to discuss their concerns and there were repeated examples from service users of that compassionate approach:
“It felt like I was talking to someone [Centre Manager] that cared and wanted to help.”
“The Nurse was brilliant. She went through all the tests with me and she was excellent.”
“When I first saw the doctor, I got emotional and apologised for taking up his time. I was never rushed, the doctor sat and explained everything.”
Users and staff also contrasted the lengthier sessions with shorter GP appointments, noting that the extended timeframe allowed them to share concerns they might otherwise withhold.
“We can spend time with people—an hour or so—so they feel they can open up, which is different from a 10-minute GP appointment.” Staff
Access to a clinical assessment
As previously noted, some individuals were referred to the clinic component of the Service, where they were assessed initially by the Nurse and subsequently by the Consultant. Service users highly valued these clinical assessments, including appropriate onward referrals to specialist services or departments. These assessments provided reassurance, alleviated anxiety related to memory concerns, and identified suitable actions to address their health conditions. One individual particularly appreciated the early access to the service and timely diagnosis, stating:.
“To be honest, I’m very grateful that the service was there. Otherwise this could have gone undiagnosed for long enough.”
Reflecting these positive experiences, few improvements were suggested and where they were, these most often related to a perceived need to better promote the Service and increase its availability across Scotland:
“I don’t think anything could have been done better, but the NHS should make it more available and publicise it more.” Service user
“I’d like to think other people could get that opportunity. I think it’s a great intervention to avoid much more serious and complex problems both mental and physical.” Service user
Motivation for accessing the Service
Sarah has been retired for six years; her husband was diagnosed with dementia in January 2023 and to reduce their social isolation she attended an unpaid carers’ support group at the Resource Centre with her husband.
The Centre Manager mentioned the Brain Health Service and Sarah decided to make an appointment and complete the brain health questionnaire.
Experience of the Service
Sarah was very positive about the Brain Health Service and thought that there were more opportunities to advertise it more widely – she only found out about it due to attending the carers’ group – but suggested that advertising the service on social media, like Facebook, in workplaces, as well as services that the wider population use, e.g. at vaccination centres could be beneficial. She noted the importance of the preventative message - emphasising to people that “It’s not just about your memory.” and also felt that a service in the Resource Centre could be seen to be a gentler route to a memory test for people who were reluctant to visit their GP.
“I feel like I know a lot more about brain health now. It has pushed me to get out, and to look after my own mental and physical health.”
Behaviour change
Sarah had anticipated that she would need to take a memory test but the need for that was not identified. Instead the outcome of the questionnaire showed that Sarah would benefit from lifestyle changes which included losing weight and increasing her exercise. These two actions were set out as goals in her Brain Health Action Plan and the discussion with the Centre Manager explored how she could achieve these goals. Two targets were set for her – to go walking three times a week, and to attend local yoga classes.
Sarah explained that the support she received had encouraged her to get out and walk, it had raised her awareness of brain health generally, and in particular has helped her understand the importance of doing something for herself to improve her own mental and physical health alongside caring for her husband.
The support she has received has had the additional benefit of encouraging her husband to take part in more activities too, and he has recently suggested activities like visiting art galleries or the supermarket as a means of staying mobile.
Sarah, retired female
Contact
Email: dementiapolicy@gov.scot