Brain Health Service pilot: evaluation - final report
This report presents detailed findings from Blake Stevenson’s independent evaluation of the Brain Health Service demonstrator site in Aberdeen,
delivered collaboratively by NHS Grampian, Alzheimer Scotland, and the Scottish Government.
2. Context and methodology
Dementia in Scotland: Everyone’s Story
Scotland’s national dementia strategy, Dementia in Scotland: Everyone’s Story, was launched in May 2023 as a joint initiative between the Scottish Government and COSLA. This 10-year strategy sets out a vision in which people living with dementia have their strengths recognised, their rights upheld and can live free from stigma. The strategy reflects a commitment to ensuring that individuals, their families, and carers receive the support necessary to live independently.
A central pillar of this strategy is the commitment to evidence-informed delivery, ensuring that policy and services are developed based on high-quality research, data, and the lived experiences of people with dementia. This approach acknowledges the complexities of dementia care and the importance of integrating real-world perspectives to inform service design and implementation.
The strategy also emphasises establishing “building blocks” for future work. This includes fostering an environment in which people with dementia and their families are empowered to influence decisions that affect them, ensuring that their voices shape Scotland’s approach to dementia care.
To enact this vision, the Two-Year Delivery Plan (published in February 2024) identifies key priorities, including an independent evaluation of the Brain Health Service (BHS) demonstrator site in Aberdeen. This evaluation is overseen by a cross-governmental, cross-sector group and is intended to assess how well the service is achieving its objectives, inform potential service improvements, and provide evidence to guide future brain health policy and practice in Scotland. The evaluation will help determine the efficacy and sustainability of the Brain Health Service model, ensuring that lessons learned from the initial implementation can contribute to the long-term strategic vision for dementia care in Scotland. This aligns with the broader goal of enhancing Scotland’s public health approach to dementia prevention, early intervention, and support services.
Brain health
Dementia prevention has become an increasing focus of public health efforts, driven by emerging evidence that a significant proportion of dementia cases may be preventable through targeted interventions.
Building on previous research, the 2024 Lancet Commission on Dementia Prevention, Intervention, and Care highlights 14 modifiable risk factors associated with dementia. These risk factors include less education, hearing loss, hypertension, smoking, obesity, depression, physical inactivity, diabetes, excessive alcohol consumption, traumatic brain injury, air pollution, and social isolation. The 2024 report further adds untreated vision loss and high LDL (low-density lipoproteins) cholesterol as newly recognised risk factors. The report underlines that addressing these modifiable risk factors across the life course—from early childhood education to midlife and older adulthood—could potentially prevent or delay nearly half of dementia cases. This strengthens the case for early intervention strategies, including promoting cognitive and physical activity, reducing exposure to air pollution, encouraging the use of hearing aids, and implementing policies to reduce high-risk behaviours such as smoking and excessive alcohol consumption.
Scotland’s commitment to integrating this into policy and practice is reflected in the Brain Health Service model, which is designed to raise awareness of brain health, support individuals in reducing their risk factors, and provide structured clinical assessments and interventions.
Brain Health Scotland
Recognising the potential for prevention in dementia care, the Scottish Government in partnership with Alzheimer Scotland, established Brain Health Scotland in 2019. This initiative was designed to explore preventive approaches to brain health and translate emerging scientific evidence into practical public health interventions. Brain Health Scotland operates with a public health focus, aiming to educate the population on risk reduction while supporting healthcare integration. Its work includes developing new service models, such as the Brain Health Service, and fostering collaborations with NHS Scotland to implement innovative care pathways. A key milestone in this work has been the establishment of a demonstrator site in NHS Grampian, which aims to test the Brain Health Service model in a real-world setting. By integrating prevention into Scotland’s dementia strategy, the demonstrator Brain Health Service provides a proactive model—moving beyond reactive dementia care toward early engagement and intervention.
Brain Health Service model
The Brain Health Service model consists of two interconnected components – a service and a two-stage clinic. Across all three stages of the Brain Health Service (the Service) outcomes include:
- offering individuals concerned about their brain health a place to discuss their concerns in depth and with professional advice;
- raising awareness of people’s ability to influence their brain health;
- providing the individual with different levels of personalised action plans to guide them towards health behaviour change; and
- individuals are signposted to relevant research opportunities and, where necessary, referral to other specialist services.
Stage 1 of the service functions as a walk-in to the Alzheimer Scotland Brain Health Resource Centre or a telephone call to NHS Grampian Healthpoint where individuals are offered access to brain health information, self-assessments, and guidance on modifiable risk factors. This stage prioritises early engagement and awareness-raising, equipping individuals with the knowledge to take proactive steps toward reducing their dementia risk. The discussions can explore personalised strategies and plans to support brain health and serve as a gateway to clinical services, with those (from Aberdeen) requiring further evaluation referred to the Brain Health Clinic.
The Brain Health Clinic forms stages 2 and 3 of the Service. Stage 2 involves the specialist Nurse Practitioner who undertakes clinical assessments with individuals undergoing risk profiling, cognitive and lifestyle assessments, and targeted interventions to support lifestyle changes and risk reduction.
If individuals are identified as being at higher risk of cognitive decline or requiring further evaluation, they are then referred to the third stage of the Service for a consultant-led assessment. This stage may involve diagnostic imaging to provide a detailed understanding of an individual’s brain health status and/or onward referral to psychiatry or specialist neurological services. The Consultant may also diagnose specific conditions.
Methodology
The remainder of the chapter describes the evaluation approach. Diagram 2.1 summarises the methodology and is followed by a more detailed description of the key elements.
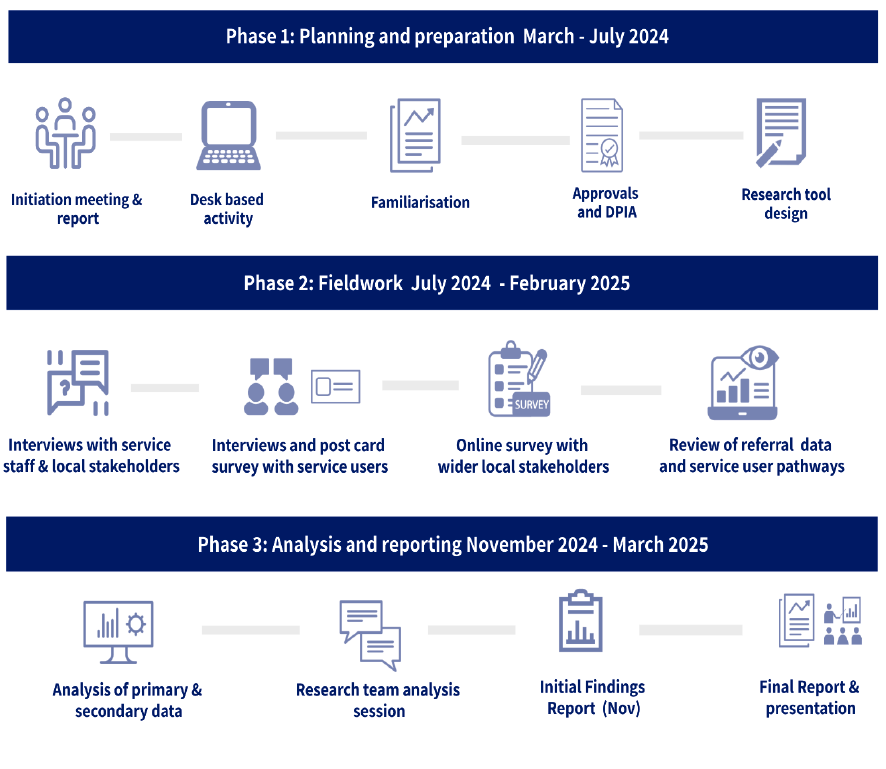
Data governance approvals
To ensure compliance with NHS Grampian information governance requirements, the Blake Stevenson team needed to obtain specific data protection approvals and by July 2024 the Data Protection Impact Assessment (DPIA) and Information Sharing Agreement and Cyber Essentials Plus accreditation were in place, allowing the fieldwork activities to begin.
Interviews with staff supporting the delivery and management of the service
The staff delivering the service were interviewed at three points during the evaluation to capture their experiences, learning and insights as the service became established. The discussions centred on their role, service operation, enablers and barriers to delivery and changes required in ways of working, processes and systems. The discussions also considered the impact of the service and the opportunities for learning and innovation. For those overseeing the service there was also discussion about their experiences of managing the stages and service fit within existing NHS Grampian systems. A total of ten staff in delivery and management roles were interviewed as part of the evaluation.
Interviews and postcard survey with service users
People accessing the Brain Health Service engaged with the evaluation in two ways. A pre-paid postcard was handed to individuals after accessing any of the three stages of the service. This had three short questions about their experience, the support they received and their short-term plans to positively support their brain health. If these were completed by individuals, they were posted to the Blake Stevenson team and a total of 25 postcards were received.
Individuals could also volunteer to take part in an interview with one of the evaluation team. The prospective participants were provided with information and if they gave consent for their information to be shared with the evaluators, in-person or virtual interviews were offered. Between September 2024 and February 2025 24 individuals were interviewed as part of this evaluation. Of these, 11 interviewees accessed Stage 1 via the Resource Centre and 13 individuals accessed Stages 2 and 3 of the Brain Health Clinic.
Online survey with wider stakeholders
The online survey was aimed at those stakeholders who may refer into the Service and wider health, social care and third sector staff involved in delivering elements of care and support that service users might access. The survey was designed and administered using Snap Surveys and the questions explored a range of issues including awareness of the service, the experience of interacting with the Service, integration and coordination of the Service within existing healthcare system and perceived changes in brain health awareness.
The survey link was distributed by NHS Grampian, it was live for three months and 27 people responded. Most respondents (21) were NHS Grampian staff followed by staff from GP Practices (5), with one respondent from another NHS Board. The NHS Grampian staff represented a variety of services including Older Adults Mental Health, Clinical Support Services, Radiology, Genetics and Speech and Language Therapy.
Local stakeholder interviews
The final set of interviews were with local stakeholders, some who had been involved in the original design and implementation of service and others that were part of the wider NHS Grampian system. These interviews explored, in more depth, the expectations of the Service and its achievements, the fit with existing local system and referral pathways and further opportunities for collaboration and wider learning. Eight local stakeholders were interviewed from NHS Grampian and Brain Health Scotland.
Review of clinical data and service user information
The data collected as part of Stage 1 service was reviewed. The clinical audit data contained information on 117 individuals who had accessed stages 2 and 3 of the service (for the period 4 January 2024 to 31 January 2025) was analysed.
Analysis and reporting
The content of the report is informed by the:
- 24 service user interviews and 25 service user postcards;
- 10 service staff and management interviews;
- eight local stakeholders;
- 27 survey responses from wider stakeholders; and
- analysis of the clinical audit data and service data from December 2023 – January 2025 and additional materials like the promotion activities and communication plans
The qualitative data gathered from the interviews, the survey responses and the service and clinical data were analysed in line with the evaluation aims and key questions. This involved a process of coding responses to identify key and recurring themes as well as any differences in viewpoints among different groups of participants. To further protect anonymity, all interview data were anonymised, and any identifying details were removed during analysis.
An internal team meeting to discuss the key emerging themes was held before producing the report outline. This was shared with the Evaluation Advisory Group for comment before the draft report was produced. The results of the analysis are presented in this report.
Advantages and limitations of the evaluation approach
The eight-month fieldwork period allowed for multiple discussions with staff and management teams, enabling real-time learning from service adaptations. This timeframe also provided an opportunity for a sufficient flow of service users, which helped in securing participants for the evaluation. The Service’s staff and management successfully integrated the evaluation activities into their day-to-day responsibilities, making it easier for the evaluation team to engage with staff despite their busy workloads.
There were some limitations to the evaluation which included:
- some service users were still progressing through the Service stages, making it difficult to observe and measure behaviour change. In particular, individuals awaiting clinical assessments or moving to the next phase of support had not yet shown measurable outcomes;
- stringent NHS Grampian data protection protocols prevented the straightforward tracking of individuals from Stage 1 through the clinic stages. This limited the ability to chart each person’s journey or develop deprivation profiles of those accessing the service;
- a survey was used to gather wider stakeholder feedback; however, a higher response rate would have yielded a broader, more diverse sample. This increase in participation would also have strengthened the reliability and generalisability of the stakeholders’ views; and
- the final phase of evaluation activities took place during a period of funding uncertainty for the Service. As a result, the focus of discussion with some participants remained on delivering the existing service model rather than planning for long-term changes or enhancements.
Despite these constraints—and the short-term nature of this evaluation relative to a service with a long-term focus—this qualitative evaluation offers a better understanding of how a demonstrator brain health service can effectively operationalise dementia prevention.
Contact
Email: dementiapolicy@gov.scot