Ending HIV transmission in Scotland by 2030
The HIV transmission elimination proposal has been developed by Professor Rak Nandwani and an expert group made up of clinicians, academia and third sector partners. The proposal contains 22 recommendations to ensure progress is made to meet our goal of zero transmissions in Scotland by 2030.
Interim targets for 2025
In addition to (at least) meeting the previously stated UNAIDS 95:95:95 target by 2025, Scotland is cognisant of the WHO 2030 target of fewer than 0.025 people newly infected with HIV per 1,000 uninfected population per year (2.5 per 100,000) [Ref 26]. The ambition for Scotland is to not only achieve this WHO incidence target but exceed it five years in advance of 2030. This aligns with Public Health Scotland's strategic plan and timelines to lead and support work to prevent disease; specifically wanting to see fewer people losing health to infectious diseases, especially hepatitis C, HIV and tuberculosis, by March 2025.
In the context of HIV testing levels returning to at least equivalent of that pre-COVID-19, we propose an interim HIV elimination target of 100 or fewer first ever diagnoses per year by the end of 2025.
This represents a greater than 60% reduction since 2010 and at least a 40% reduction compared with the 2019 baseline by the end of 2025.
With a return to pre COVID-19 HIV testing levels, the 100 first ever HIV diagnoses per year by the end of 2025 will comprise a combination of people with incident HIV (acquired within the previous 12 months identified with the assistance of avidity and negative testing) and also detection of people with longer-established previously undiagnosed HIV. With potentially as many as 500 people living with established undiagnosed infection in Scotland [Ref 4] approximately 60-70 people with prevalent HIV need to be diagnosed each year in the years to 2030. The aim of this proposal is to "front-load" HIV detection strategies to locate people and to prevent mortality and morbidity related to late HIV diagnosis [Ref 27]. Therefore, it is desirable and expected that there are higher numbers of people found for the first time in the years from 2023 onwards (greater than 60 per year). It is anticipated that this will decline as 2030 is approached.
It is recognised that the estimate of people living with HIV in Scotland, including those undiagnosed, will need to be recalculated with adjustments made from the impact of the COVID-19 pandemic on behaviours, testing and service attendance. It would be desirable to reach a consensus approach on back-calculation and statistical models for consistent UK definitions [Ref 28].
Although incomplete, utilising recent infection testing algorithms (RITA) linked to HIV antibody avidity data, we estimate that around a quarter of the 167 first ever HIV diagnoses in 2019 were recently acquired. The remainder comprised infections that were probably acquired more than 3-4 months prior to the first positive HIV antibody test. Thus, the number of people with newly diagnosed recently acquired HIV reduced by approximately 40% (from 67 to 41) between 2015 and 2019. [Ref 4]
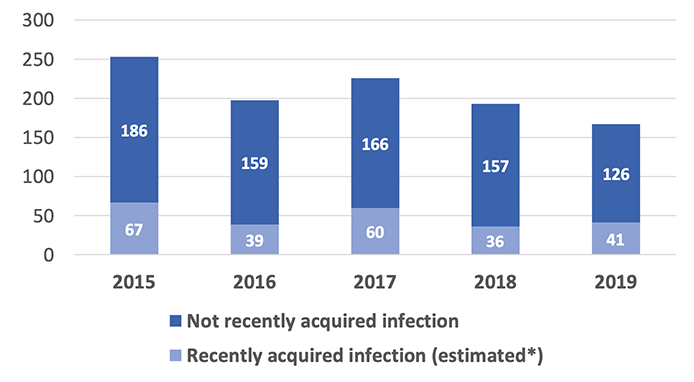
(Source: Public Health Scotland)
* New diagnoses are tested for recent acquired infection using the HIV avidity antibody test; estimates of recently acquired infection were derived for 114 samples (11%) without an avidity test result based on those with available data.
In the context of HIV testing levels returning to at least equivalent of that pre-COVID-19, HiTEOG proposes that the number of people diagnosed for the first time with recently acquired HIV infection (within the previous 3-4 months) in Scotland should be 20 per year or fewer by 2025.
If achieved, this would be consistent with an approximate halving of diagnosed recently acquired infection in Scotland between 2019 and 2025.
Given the low numerical target, it would be challenging to propose meaningful outcomes for specific demographic groups or sub-populations in Scotland, but as far as possible there should be equity of reduced HIV incidence in all regardless of age, sex, gender identity, sexual orientation, race, ethnicity, religion, deprivation or disability status. Analysis of the demographic characteristics of people who continue to present with a first ever HIV diagnosis (especially recently acquired infection) should be used to refine prevention and diagnosis interventions so that all communities benefit equally.
As first ever HIV diagnosis numbers decrease over time, there are two key considerations to bear in mind. The first is there may be greater challenge and possibly cost to reach individuals remaining at highest risk of HIV acquisition, owing to pre-existing inequalities and intersectionality. The second is the need to avoid stigmatising people who are newly diagnosed when HIV becomes a relatively rare event.
It is anticipated that there will be a "tipping point" between 2025 and 2030 when the proportion of recently acquired HIV begins to account for the majority of first ever diagnoses, rather than instances of established HIV. This will require review of the strategy to progress to a new phase with emphasis shifting from high testing coverage towards contact tracing, whilst maintaining primary prevention, treatment and care and public health surveillance.
Contact
Email: healthprotection@gov.scot